* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Tobramycin
Pharmacogenomics wikipedia , lookup
Gastrointestinal tract wikipedia , lookup
Pharmaceutical industry wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
Prescription costs wikipedia , lookup
Neuropharmacology wikipedia , lookup
Drug interaction wikipedia , lookup
Drug design wikipedia , lookup
Drug discovery wikipedia , lookup
Levofloxacin wikipedia , lookup
Pharmacokinetics wikipedia , lookup
Ciprofloxacin wikipedia , lookup
Discovery and development of cephalosporins wikipedia , lookup
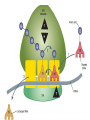
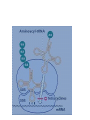
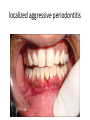
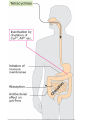
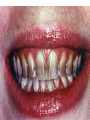
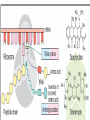
Tetracyclines (Doxycycline and Minocycline) Mechanism of Action • The site of action of TET is the bacterial ribosome and all TET function in the same manner. They are bacteriostatic compounds. • TET enter to susptible MO by Passive diffusion through hydrophilic pores in the outer cell membranes.or by Energy-dependent active transport system that pumps all TET through the inner cytoplasmic membrane. • TET inhibit protein synthesis by binding specifically to the 30S ribosome. This appears to prevent access of AA-tRNA to the acceptor site on the mRNA-ribosome complex; preventing the addition of AA to the growing peptide chain. Resistance • Resistance to the TET for gram-ve and gram+ve bacteria is mediated by inducible plasmid [the bacteria become resistant only after exposure to the drug]. Antibacterial spectrum(broad bacteriostatic ) • These compounds also impair protein synthesis in: mammalian cells at high concentration. For gram (-) bacteria, less understood for gram (+) bacteria. Uses: Treated Cholera , Chlamydia infection , Mycoplasma pneumonia - Pharmacokinetics Absorption: • All TET are adequately but incompletely absorbed from the G.I. tract. Most absorption takes place from the stomach and upper small intestine (greater in a fasting state). • Absorption of TET is impaired by • food in the stomach, • milk products, • aluminum OH gels, Na+ bicarbonate, Ca++ & Mg++, and Fe++ preparations. • . • They bind to tissue undergoing calcification ( teeth and bone) . • It enter CSF but level insufficient for therapeutic and it appear in tears and saliva • It cross placental barrier and concentrated in fetal bones and dentine • Doxycycline and minocycline are almost totally absorbed on oral administration. • doxycycline is the preferred tetracycline for parenteral administration • Minocycline enters the brain in the absence of inflammation and also appears in tears and saliva. • useful in eradicating the meningococcal carrier state • minocycline is not effective for central nervous system Therapeutic uses in dentistry • The use of tetracyclines in the management of acute orofacial infections is widely considered inappropriate because of their bacteriostatic activity and extensive microbial resistance. • . • Systemic tetracyclines in the management of chronic periodontitis must be carefully evaluated for risk/benefit ratio considering their limited efficacy • . • Tetracyclines are effective in the management of localized aggressive periodontitis and its associated organism, A. actinomycetemcomitans. • Tetracyclines may also be used subgingivally localized aggressive periodontitis Excretion • TET metabolized in liver • excreted in bile and reabsorbed by entero hepatic circulation all the TET are excreted in the urine and the feces. EXCEPT doxycycline , The drug is excreted by bile and feces, largely as an inactive conjugate. Thus one of the safest of the TET for the treatment of extrarenal infections. • TET also excreted in breast milk . Adverse Effects • TET can produce a variety of adverse effects ranging from minor inconvenience to life-threatening. • Wide safety margin, but many side effects Gastrointestinal TET produce GI irritation to a varying degree in some but not all individuals. Nausea, vomiting, burning, diarrhea (common) • Diarrhea must be promptly distinguished from that which results from pseudomembranous colitis - caused by overgrowth of clostridium difficile ( can be life-threatening) . • TET like other antimicrobial agents administered orally may lead to development super infections, usually due to strains of bacteria or yeast resistant to these agents. Hepatic Toxicity • In Pregnant women are particularly sensitive to TET -induced hepatic damage When received high dose of TET . Renal Toxicity • TET may aggregate uremia in patients with renal disease by Inhibition protein synthesis – Effects on TEETH • Children receiving long-or short term therapy with TET may develop brown discoloration of the teeth. The drug deposits in the teeth and bones probably due to its chelating property and the formation of a TET -calcium orthophosphate complex. This discoloration is permanent. Avoid giving to pregnant women and children under the age of 8 years . Other effects • Hypersensitivity : -Rash, hives with itching, itching anaphylactic ( decrease in BP, increase in HR, release of histamine, etc.) • Photoxicity : darkening of skin & sunburn when patient exposed to sunlight Contra indication • . • 1. TET should not be used in pregnant women and children under 8 years . • 2. Tetracycline during 1st trimester of pregnancy can cause birth defects • 3. Should not be given to patient with severe liver and renal disease. Glycylcyclines • Tigecycline is a derivative of minocycline, • similar to the tetracyclines and has a broadspectrum activity against multidrug-resistant gram-positive pathogens, • some gram-negative organisms, • anaerobic organisms. • Tigecycline is indicated for treatment of complicated skin and soft tissue infections as well as complicated intra-abdominal infections. • Giving as intravenous infusion every 12 hours Drug interactions • tigecycline inhibit the clearance of warfarin.. • tigecycline decrease the effects of oral contraceptives. Aminoglycosides & Spectinomycin • Aminoglycosides Streptomycin Amikacin ,gentamicin,Tobramycin Tobramycin,Neomycin, Netilmicin • Use to in restricted to treat serious infection due to aerobic gram negative bacilli because of serious toxicities so replace by more safe drug . 1. Gram (-) Aerobic Bacilli 2. Beta-lactamase Staph. aureus N. gonorrhea 3. Mycobacteria 4. Pseudomonas aeruginosa All aminoglycosides are bactericidal I. AMINOGLYCOSIDES Older Aminoglycosides: Streptomycin Kanamycin Newer Aminoglycosides: Gentamicin Tobramycin Neomycin Amikacin Netilmicin Sisomicin MECHANISMS OF ACTION OF ANTIBACTERIAL DRUGS • Aminoglycosides – Irreversibly binds to 30S ribosomal subunit • Causes distortion and malfunction of ribosome • Blocks translation –Causes misreading of mRNA – Not effective against anaerobes, enterococci and streptococci Aminoglycosides • irreversible inhibitors of protein synthesis, but the precise mechanism for bactericidal activity is not known. • The initial event is passive diffusion via porin channels across the outer membrane • Drug is then actively transported across the cell membrane into the cytoplasm by an oxygen-dependent process. • Low extra cellular pH and anaerobic conditions inhibit transport by reducing the gradient. . Mechanism of action • aminoglycosides bind to specific 30S-subunit ribosomal proteins Protein synthesis is inhibited by aminoglycosides through • (1) interference with the initiation complex of peptide formation • (2) misreading of mRNA, which causes incorporation of incorrect amino acids into the peptide and results in a nonfunctional or toxic protein and Therapeutic uses • 1- infection due to enterococci which is resistant to most antibiotic classes and require two synergistic antibiotic for effective therapy eg : Gentamycin or streptomycin + Vancomycin or B- lactam (P group ) • 2- infected due to Pseudomonas aeruginosa which rarely attack healthy individual like immunocompromised treated include Tobramycin + anti Pseudomonal pencillin (ticarcillin ) Resistance to aminoglycosides • due to: 1-failure of drug to penetrate intracellular 2-low affinity of drug for bacterial ribosome 3-drug inactivation PHARMACOKINETICS • Aminoglycosides are absorbed very poorly from the intact gastrointestinal tract; almost the entire oral dose is excreted in feces after oral administration • . intramuscular injection, are well absorbed, giving peak concentrations in blood within 30– 90 minutes. • Aminoglycosides are usually administered intravenously as a 30- to 60-minute infusion. • . • once-daily aminoglycoside dosing may be preferred in certain clinical situations. Aminoglycosides have concentration-dependent killing; that is, increasing concentrations kill an increasing proportion of bacteria and at a more rapid rate. They also have a significant postantibiotic effect, such that the antibacterial activity persists beyond the time during which measurable drug is present. Side effect of Aminoglycosides 1- Ototoxicity(Vestibular and Cochlear ) related to high peak plasma level and duration of treatment : deafness may be irreversible . 2- Nephrotoxicity :mild , reversible 3- neuromuscular paralysis : after direct intraperitoneal or intrapleural application of high doses, aminoglycosides can produce a curare-like effect with neuromuscular blockade that results in respiratory paralysis. This paralysis is usually reversible by calcium gluconate (given promptly) or neostigmine. 4- Allergic reaction : contact dermatitis when neomycin applied topically . streptomycin • Used for Rx of certain unusual infections in combination with others • Given by deep i.m or i.v • Indicated for Rx of; 1- bacterial endocarditis 2-Brucellosis 3-second choise in TB. Gentamicin(garamycin) • For gm –ve bacillary infection • Given parentally , topical(solutions,ointment) indications: *Urinary tract infection(uTI) *pneumonia *meningitis *bacterial endocarditis *sepsis *Meningitis caused by gram-negative bacteria has been treated by the intrathecal injection of gentamicin *Ocular infection NEOMYCIN & KANAMYCIN . • Neomycin and kanamycin are closely related. are active against gram-negative bacteria and some mycobacteria. • Pseudomonas and streptococci are generally resistant. • Given oral, topical • Uses: topical for skin and mucous membrane infections e.g.burns,wound,ulcer • Poorly absorbed from GIT • Excreted by kidney neomycin • Side effects -hypersensitivity -renal damage -deafness -orally can cause intestinal malabsorption and superinfection Tobramycin • has almost the same antibacterial spectrum as gentamicin with a few exceptions. tobramycin is slightly more active against pseudomonas; Enterococcus faecalis • Like other aminoglycosides, tobramycin is ototoxic and nephrotoxic. Nephrotoxicity of tobramycin may be slightly less than that of gentamicin • Tobramycin is also formulated in solution (300 mg in 5 mL) for inhalation for treatment of Pseudomonas aeruginosa lower respiratory tract infections . Amikacin • a semisynthetic derivative of kanamycin; it is less toxic than the parent molecule • Act on Many gram-negative enteric bacteria, including many strains of proteus, pseudomonas, enterobacter, strains, are usually susceptible to amikacin • . Like all aminoglycosides, amikacin is nephrotoxic and ototoxic (particularly for the auditory portion of the eighth nerve). SPECTINOMYCIN • Spectinomycin is an aminocyclitol antibiotic that is structurally related to aminoglycosides. It lacks amino sugars and glycosidic bonds. General notes on aminoglycosides • Combined with Penicillin or cephalosporin for serious gm-ve infections • Should not be used more than few days. • Never mix with P in same solution (inactivation) • Contra indicated in pregnancy.