* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Lecture 03. General characterization of monogenic pathology
Gene therapy wikipedia , lookup
Microevolution wikipedia , lookup
Neuronal ceroid lipofuscinosis wikipedia , lookup
Genome (book) wikipedia , lookup
Medical genetics wikipedia , lookup
Gene therapy of the human retina wikipedia , lookup
Designer baby wikipedia , lookup
Epigenetics of diabetes Type 2 wikipedia , lookup
Polydactyly wikipedia , lookup
DiGeorge syndrome wikipedia , lookup
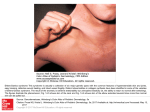
General characterization of monogenic pathology. Clinical symptoms and genetics of the main forms of monogenic diseases Ass. prof. Furdela V.B. Causes Molecular Basis of Ehlers-Danlos Syndrome Type Old Nomenclature Protein Abnormality Gene Abnormality Chromosome Locus Type I/II Type V collagen COL5A1, COL5A2 9q34.2-34.3 2q31 Type III Unknown Unknown Unknown Type IV Type III collagen COL3A1 2q31 Kyphoscoliosis Type VI Lysyl hydroxylase PLOD1 deficiency (some) Arthrochalasia Type VII A/B Type I collagen COL1A1 COL1A2 17q31-22.5 7q22.1 N-proteinase ADAMST2 5q23-24 Classic Hypermobility Vascular DermatoType VIIC sparaxis 1p36.3-36.2 Ehlers-Danlos syndrome. Skin hyperextensibility Ehlers-Danlos syndrome. Dorsiflexion of all the fingers is easy and absolutely painless. Ehlers-Danlos syndrome. Joint hypermobility is less intense than with other conditions. Ehlers-Danlos syndrome. Note the abnormal ability to elevate the right toe. Types of Ehlers-Danlos Syndromes • Classic (Types I and II) – Autosomal dominant • Major Diagnostic Criteria – Skin hyperextensibility, wide atrophic scars, joint hypermobility • Minor Diagnostic Criteria – Smooth, velvety skin; easy bruising; molluscoid pseudotumors; joint hypermobility; muscle hypotonia; postoperative complication (eg, hernia); positive family history; manifestations of connective tissue lesions (eg, hernia, prolapse) Treatment • In the event of injuries, take extreme care with the use of sutures, adhesive strips and wound glues. • avoid excessive activities on hypermobile joints. • In the presence of mitral valve prolapse, subacute bacterial endocarditis (SBE) prevention. • High-dose (1-4 g/d) ascorbic acid therapy • desmopressin in the prevention and treatment of bleeding Neurofibromatosis • Neurofibromatosis (NF) is a multisystem genetic disorder commonly associated with cutaneous, neurologic, and orthopedic manifestations. Frequency. Rase. Sex • Incidence of neurofibromatosis type 1 is 1 case in 3 000 persons • Half of affected individuals represent first cases in their families as the result of a new genetic event or mutation • All races and ethnic backgrounds are equally affected • While males and females are equally affected , scoliosis may be especially severe in young girls Causes. Pathophysiology • Manifestations of neurofibromatosis type 1 are caused by a mutation in, or a deletion of, the NF1 gene. The gene product, neurofibromin, serves as a tumor suppressor. Decreased production of this protein causes various clinical features. • The NF1 gene is located within the long arm of chromosome 17. Clinical criteria for diagnosis (presence of at least 2 of 7 criteria ) • At least 6 café au lait spots or hyperpigmented macules • Axillary or inguinal freckles • Two or more typical neurofibromas or 1 plexiform neurofibroma • Optic nerve glioma • Two or more iris hamartomas (also known as Lisch nodules), • Sphenoid dysplasia or typical long-bone abnormalities • First-degree relative with neurofibromatosis type 1 Café au lait spots Neurofibromas • Subcutaneous or cutaneous neurofibromas appear over time in older children, adolescents, and adults. Puberty and pregnancy may be associated with increased numbers and more rapid growth of preexisting lesions. • Plexiform neurofibromas are more diffuse growths. They may be associated with bony erosion and pain, accompanied by overlying hyperpigmentation or hypertrichosis. • Neurofibromas rarely grow rapidly. Multiple neurofibromas Plexiform neurofibroma of the eyelid A right thigh plexiform neurofibroma Ophthalmologic examination – Optic nerve tumors in children younger than 5 years – Optic nerve gliomas in older children or even adults with spontaneous regression. – Subtle peripheral field defects, color discrimination difficulties, optic nerve pallor, proptosis may occur in association with an optic glioma. – Lisch nodules can occasionally be seen with an ophthalmoscope – Patchy choroidal abnormalities and corkscrew retinal vascular changes Neurofibromatosis. Lisch nodules Orthopedic examination • Sphenoid dysplasia in patients with plexiform neurofibroma of the eyelid or temporal region • Congenital pseudarthrosis. Bowing of the tibia. Thinning and angulation of long. Bowing of the forearm is less common. • Thoracic cage asymmetry with flaring or prominence of the inferior ribs. • Scoliosis, with or without kyphosis. Radiograph showing radial bowing, ulnar bowing, and obliteration of the intramedullary spaces MRI showing a left optic nerve glioma with thickening of the nerve and proptosis. Neurofibromatosis. MRI scan depicting an unidentified bright object (UBO) within the brain parenchyma. Treatment • Biannual examinations for children younger than 5 years, and annual examinations thereafter • Annual eye examinations • cutaneous examination to search for new neurofibromas and progression of preexisting lesions. • a careful search for skeletal involvement • Check blood pressure at every visit • Ask parents about the child's neurodevelopmental progress Prognosis • neurofibromatosis type 1 may reduce overall life expectancy as much as 15 years Marfan syndrome • Marfan syndrome is an inherited connectivetissue disorder (the most common single-gene malformation syndromes) transmitted as an autosomal dominant trait. • Marfan syndrome is named after Antoine Marfan, the French pediatrician who first described the condition in 1896. Frequency. Mortality. Rase. Age • Marfan syndrome affects about 1 in 10,000 individuals3 and perhaps as many as 1 in 30005000. • Cardiovascular disease (aortic dilatation and dissection) is the major cause of morbidity and mortality. • Marfan syndrome is panethnic. • Marfan syndrome may be diagnosed prenatally, at birth, or well into adulthood. Type of inheritance Skeletal findings • taller and thinner than their family members. • limbs are disproportionately long compared with the trunk • Arachnodactyly – For the skeletal system to be involved, at least 2 major criteria or 1 major criterion plus 2 minor criteria must be present. Adult with Marfan syndrome. Note tall and thin build, disproportionately long arms and legs, and kyphoscoliosis. Arachnodactyly – Major criteria • Pectus excavatum that requires surgery or pectus carinatum • Positive wrist (Walker) and thumb (Steinberg) signs • Scoliosis greater than 20˚ • Reduced extension of the elbows (<170°) • Pes planus • Protrusio acetabuli Pectus excavatum of moderate severity Positive thumb (Steinberg) sign Positive wrist (Walker) sign Minor criteria • • • • • • • Pectus excavatum of moderate severity Scoliosis less than 20° Thoracic lordosis Joint hypermobility Highly arched palate Dental crowding Typical facies (dolichocephaly, malar hypoplasia, enophthalmos, retrognathia, down-slanting palpebral fissures) Hypermobility of finger joints Ocular findings • The major criterion is ectopia lentis • Minor criteria: – – – – – Flat cornea Increased axial length of the globe Cataract in patients younger than 50 years Hypoplastic iris or hypoplastic ciliary muscle The most common refraction error is myopia due to elongated globe and amblyopia. – Glaucoma (patients younger than 50 years) – Retinal detachment • At least 2 minor criteria must be present. Cardiovascular findings • Major criteria – Aortic root dilatation in 70-80%. – Aortic dissections involving the ascending aorta • Minor criteria: – – – – Mitral valve prolapse (55-69%). Dilatation of proximal pulmonary artery Calcification of mitral annulus (patients < 40 yrs) Dilatation of abdominal or descending thoracic aorta (patients < 50 yrs) • For the cardiovascular system to be involved, a minor criterion must be present. Pulmonary findings a minor criterion: – Spontaneous pneumothorax – Apical blebs on chest radiography • Skin and integumentary findings • Minor criteria: – Striae atrophicae in the absence of marked weight changes on the shoulder, mid back, and thighs. – Recurrent or incisional hernia Stretch marks (striae atrophicae) in the lower back Workup • • • • • • • • • Genetic testing - screening the entire FBN1 gene Molecular studies of the fibrillin gene Radiography: Chest, Pelvis Echocardiography CT and MRI of the lumbosacral spine Aortography ECG Measure blood pressure Ophthalmoscopy Treatment • • • • • • • • Moderate restriction of physical activity Endocarditis prophylaxis (Intravenous antibiotic) Echocardiography at annual intervals Beta-blocking treatment Anticoagulant medications Conservative treatment of protrusio acetabuli Myopia is treatable with refraction. Patients with flat feet may wear shoes with adequate arch support.