* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Estrogen
Gynecomastia wikipedia , lookup
Hormone replacement therapy (female-to-male) wikipedia , lookup
Progesterone wikipedia , lookup
Hypothalamus wikipedia , lookup
Hormonal breast enhancement wikipedia , lookup
Growth hormone therapy wikipedia , lookup
Bioidentical hormone replacement therapy wikipedia , lookup
Hyperandrogenism wikipedia , lookup
Polycystic ovary syndrome wikipedia , lookup
Hormone replacement therapy (menopause) wikipedia , lookup
Hormone replacement therapy (male-to-female) wikipedia , lookup
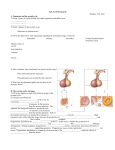
Estrogen: A female steroid hormone that is produced by the ovaries and, in lesser amounts, by the adrenal cortex, placenta, and male testes. Estrogen helps control and guide sexual development, including the physical changes associated with puberty. It also influences the course of ovulation in the monthly menstrual cycle, lactation after pregnancy, aspects of mood, and the aging process. Major estrogens (1) Estradiol-17β - most potent natural estrogen and major secretory product of ovary. (2) Estrone - also of ovarian/adrenal origin; exists in equilibrium with estradiol. (3) Estriol - not a product of the ovary, estriol is the predominant urinary end product of estrogen metabolism. In the pregnant woman, estriol, as estradiol and estrone, are secreted by the placenta. Displays minimal estrogenic activity. Estradiol (E2) is the predominant estrogen during reproductive years both in terms of absolute serum levels as well as in terms of estrogenic activity. During menopause, estrone (E1) is the predominant circulating estrogen and during pregnancy estriol (E3) is the predominant circulating estrogen in terms of serum levels. Biosynthesis Estrogens, in females, are produced primarily by the ovaries, and during pregnancy, the placenta. Follicle-stimulating hormone (FSH) stimulates the ovarian production of estrogens by the granulosa cells of the ovarian follicles and corpora lutea. Some estrogens are also produced in smaller amounts by other tissues such as the liver, adrenal glands, and the breasts. These secondary sources of estrogens are especially important in postmenopausal women. Fat cells produce estrogen as well. Function The actions of estrogen are mediated by the estrogen receptor (ER), a dimeric nuclear protein that binds to DNA and controls gene expression. Like other steroid hormones, estrogen enters passively into the cell where it binds to and activates the estrogen receptor. Since estrogen enters all cells, its actions are dependent on the presence of the ER in the cell. The ER is expressed in specific tissues including the ovary, uterus and breast. They also act by activating G protein-coupled receptor, GPR30. Physiological effects of estrogens (1) Promotion of tissue growth associated with puberty--vagina, uterus, Fallopian tubes, mammary glands (stromal and ductal growth). (2) Proliferation of uterine endometrium. (3) Increase in myometrial and Fallopian tube peristalsis to promote ovum transport. (4) Decrease in viscosity of cervical mucus. (5) Biphasic inhibition on pituitary gonadotropin secretion. (6) Promotion of epiphyseal closure. (7) Ovum implantation facilitated via endometrial "conditioning". (8) Promotion of salt and water retention via decrease in plasma volume. (9) Lipid metabolism (↑HDL, ↓LDL; ↓LDL/HDL ratio). (10) Enhancement of blood coagulability. (11) Inhibition of PTH-induced bone resorption. (12) Reduction of intestinal motility. Pharmacology Oestradiol is broken down in the stomach, but an ethinyl group at the 17 position confers oral activity. Ethinyloestradiol is the most widely used oestrogen in oral contraceptives. The other estrogen sometimes used is the 3methyl ester of ethinyloestradiol, mestranol, which has half the potency of ethinyloestradiol. Other orally active oestrogens are sometimes used therapeutically (e.g. for menaupausal symptoms): Premarin: conjucated oestrone from the urine of pregnant mares Oestradiol valerate: converted to oestrone during absorption. Oestradiol: on a micronized solid phase, also converted to oestrone during absorption. Therapeutic uses of estrogens: (1) Oral contraceptives. (2) Relief of menopausal symptoms. (3) Dysmenorrhea. (4) Failure of pituitary function/ovarian development- estrogens will not result in normal reproductive functioning but will promote growth of reproductive organs and appearance of secondary sexual characteristics. (5) Osteoporosis. Hormone replacement therapy Estrogen and other hormones are given to postmenopausal women in order to prevent osteoporosis as well as treat the symptoms of menopause such as hot flushes, vaginal dryness, urinary stress incontinence, chilly sensations, dizziness, fatigue, irritability, and sweating. For many years, estrogen therapy and estrogenprogestin therapy were prescribed to treat menopausal symptoms, to prevent osteoporosis and to improve women's overall health. However, after publication of results from the Women's Health Initiative (WHI) in 2002 and March 2004, the U.S. Food and Drug Administration (FDA) now advises health care professionals to prescribe menopausal hormone therapies at the lowest possible dose and for the shortest possible length of time to achieve treatment goals. Treatment is generally reserved for management of menopausal symptoms rather than prevention of chronic disease. Premarin: Premarin is the commercial name for a medication consisting primarily of conjugated estrogens. Isolated from mares' urine (pregnant mares' urine). It is available in oral (0.3/0.45/0.625/0.9/1.25 mg), IV, and topical (vaginal) form. Premarin is a form of hormone replacement therapy. Premarin pills are used most commonly in post menopausal women who have had a hysterectomy to treat hot flashes, and burning, itching, and dryness of the vagina and surrounding areas. It can also be used in conjunction with a progestin pill in women who have not had a hysterectomy. For women already taking the drug it can be used to treat osteoporosis, although it is not recommended solely for this use. The most common side effects associated with Premarin use are vaginal yeast infections, vaginal spotting or bleeding, painful menses, and cramping of the legs. PROGESTERONE Site of synthesis: ovaries, adrenal and placenta (testes and adrenal in male). Terminology: Progestin: any of a group of steroid hormones, including synthetic forms, that have the effect of progesterone Progestogen: any of a group of steroid hormones that have the effect of progesterone Progesterone: the naturally occurring hormone, produced in the corpus luteum of the ovary Physiological effects (1) Development of secretory endometrium. (2) Decrease in myometrial contractility (3) Decrease in fallopian tube peristalsis (4) Increase in viscosity of cervical mucus (5) Mammary gland development - promotion of development of lobules and alveoli (6) Feedback inhibition on pituitary gonadotropins - not as potent as the estrogens. (7) Thermogenic effects-appears to be a direct effect on thermoregulatory centers in the hypothalamus. (8) Increase in basal insulin levels and insulin response to glucose. (9) Respiratory effects - increased response to CO2. (10) Lipid metabolism (↓ HDL, ↑ LDL; ↑ LDL/HDL ratio). (11) ↑ Na+ and H2O elimination (12) Weight gain Pharmacology: Progesterone itself is destroyed by stomach acid but can be administered as suppository. There are three forms of progesterone which are absorbed after oral preparation: Dydrogesterone: which is a very weak progestogen. 17 α-hydroxyprogesterone derivatives, the best known of which is medroxyprogesterone acetate. Other 17-OH derivatives are megestrol acetate and chlormadinone acetate. 19-nor-Progesterone: the commonest progestogen in oral contraceptives. Removal of the CH3 group from the 19 position of testosterone protect the steroid from acid breakdown. The 19-norprogesterones are related to this compound and all have some residual androgenic activity. It includes norethisterone, norgestrel (is the most potent and widely used), & levonorgestrel. Three newer progestogens, norgestimate, desogestrel and gestodene are all chemically related to levonorgestrel. Cycle control is improved with lower incidence of intermenstrual bleeding and less adverse effect on blood lipid. The progestogens used in currently available combined contraceptive pills fall broadly into three groups: 1st generation progestins--------norethindrone. 2nd generation --------levonorgestrel. 3rd generation-------gestodene, desogestrel and norgestimate. The newest COCP (Yasmin)contains a progestogen with both antiandrogenic and antimineralocorticoid activity (drospirenone). Therapeutic uses of progestins 1) 2) 3) 4) 5) 6) 7) 8) Contraceptives (COCP, POP, injectable progesterone, progesterone releasing IUS). Dysmenorrhea. Endometriosis. Dysfunctional uterine bleeding. Prevention of habitual abortion, premature labor. Amenorrhea due to unopposed estrogen. Infertility due to shortened luteal phase. Endometrial cancer. SIDE EFFECTS: Nausea, bloating, breast tenderness, headache, change in vaginal discharge, mood swings, blurred vision, dizziness, or drowsiness may occur. PRIMOLUT -N Norethisterone 5 mg tablets Norethisterone is a strong progestogen with negligible androgenic effects Indications Dysfunctional bleeding, premenstrual syndrome, cyclical mastopathy, timing of menstruation, endometriosis, menorrhagia. Dysfunctional uterine bleeding: The administration of one tablet PRIMOLUT N three times daily over 10 days, in the majority of cases, leads to the arrest of uterine bleeding that is not associated with organic lesions within 1 to 3 days. Nevertheless, to ensure treatment success, PRIMOLUT N must be taken for the full 10 days. About 2 to 4 days after completion of the treatment, withdrawal bleeding will occur with the intensity and duration of normal menstruation. To prevent recurrence of dysfunctional bleeding in patients with anovulatory cycles, it is recommended to administer PRIMOLUT N prophylactically. One tablet 1 to 2 times daily from the 16th to the 25th day of the cycle. Withdrawal bleeding occurs a few days after administration of the last tablet. Menorrhagia: Treatment with PRIMOLUT N one tablet 3 times daily from day 5 - 25 of the cycle has been shown to be effective in reducing menstrual blood loss. ANDROGENS Androgens in Females Sites of synthesis--ovaries, adrenals, placenta Physiological significance - apparently not necessary for normal menstrual cycling, but may be involved in pubertal growth spurt, libido Danazol It is an isoxazole of testosterone with isolated weak androgenic activity and no estrogenic or progestagenic effects. Danazol inhibits ovarian steroidogenesis resulting in decreased secretion of estradiol and may increase androgens. Pituitary hormones are largely unaffected, although luteinizing hormone may be slightly elevated. It was approved by the US Food and Drug Administration (FDA) as the first drug to specifically treat endometriosis in the early 1970s. Although effective for endometriosis, its use is limited by its masculinizing side-effects. Its role as a treatment for endometriosis has been largely replaced by the GnRH agonists. Danazol has been used for other indications, namely in the management of menorrhagia, fibrocystic breast disease, immune thrombocytopenic purpura, breast pain (mastodynia) and hereditary angioedema. Although not currently a standard treatment for menorrhagia, danazol has resulted in significant relief in young women with menorrhagia in a study, and, because of a lack of significant adverse effects, it was proposed as an alternative Side effects: Androgenic side effects are of concern, it includes hirsutism. On rare occasion, it can deepen the voice. Other possible side effects include acne and oily skin. Because danazol is metabolized by the liver, it cannot be used by patients with liver disease, and in patients receiving long-term therapy, liver function must be monitored on a periodic basis. Some patients who use danazol experience weight gain and fluid retention. Danazol, like most other androgenic agents, has been linked with an increased risk of liver tumors. These are generally benign. Antiprogesterones: These either inhibit progesterone formation or block the receptor (mifepristone, RU486). They are abortifacient and contraceptive. Anti-androgens: Anti-androgens include: cyproterone acetate, spironolactone, stillbestrol, flutamide and cimetidine. Cyproterone acetate commonly used to treat hirsutism in female. Other commonly used hormons therapy in gynecology: gonadotrophins Human menopausal gonadotrophin (hMG) was used initially for ovulation induction in anovulatory women until the introduction of IVF led to its use to induce multiple ovulation so that a large number of follicles and oocytes could be obtained. E.g. of these drugs: Pergonal (menotrophins): human menopausal gonadotrophin; hMG, contains both FSH and LH. Metrodin: purified human urinary FSH preparation. Gonal-F: recombinant FSH. Gonadotrophin-releasing hormone analogues: GnRH [LH_RH] is naturally secreted in intermittent pulses. For induction of ovulation is given intravenously or subcutaneously by special pump which deliver the hormone in pulses. If it is given continuously it cause pituitary desensitization which result in inhibition of ovarian steroidogenesis & amenorrhoea. The administration of a GnRH agonist result in an initial agonist effect, leading to the production of both FSH and LH, the so-called ‘flare-up’ effect followed by a sustained decline in both pituitary response and gonadotrophins production, a process known as pituitary down regulation. A number of synthetic ,long-acting analogues of GnRH have been synthesized, they are administered as intranasal sprays or as subcutaneous depot preparations E.g.: Goserelin (zoladex). Uses: GnRH agonists are used with controlled ovarian stimulation (COS) to improve the outcome of ovarian stimulation by allowing synchoronous folliculogenesis and later to prevent premature luteinization by supressing the endogenous LH surge. In the management of hormon dependent conditions as endometriosis. Gonadotrophin-releasing hormone antagonists They competitively bind (block) gonadotrophic receptors. They are capable of immediate inhibition of pituitary gonadotrophin secretion and are unlikely to offer advantages over the currently available agonists due to the absence of flare-up effect. E.g.: Ganirelex. Human chorionic gonadotrophin (hCG) Mimics LH surge to induce ovulation. E.g.: pregnyl