* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Document
Munchausen by Internet wikipedia , lookup
Death anxiety (psychology) wikipedia , lookup
Causes of mental disorders wikipedia , lookup
Wernicke–Korsakoff syndrome wikipedia , lookup
Down syndrome wikipedia , lookup
Generalized anxiety disorder wikipedia , lookup
Child psychopathology wikipedia , lookup
Dissociative identity disorder wikipedia , lookup
Rumination syndrome wikipedia , lookup
Externalizing disorders wikipedia , lookup
Combat stress reaction wikipedia , lookup
Asperger syndrome wikipedia , lookup
Diagnosis of Asperger syndrome wikipedia , lookup
Diagnostic and Statistical Manual of Mental Disorders wikipedia , lookup
Depression in childhood and adolescence wikipedia , lookup
Post-concussion syndrome wikipedia , lookup
Conversion disorder wikipedia , lookup
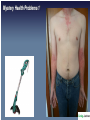
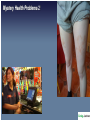
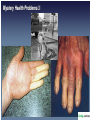
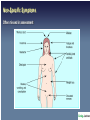
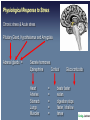
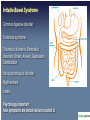
The following lecture has been approved for University Undergraduate Students It is not intended for the content or delivery to cause offence Any issues raised in the lecture may require the viewer to engage in further thought, insight, reflection or critical evaluation This lecture may contain information, ideas, concepts and discursive anecdotes that may be thought provoking and challenging BioPsychSocial Factors in Ill-Health Prof. Craig Jackson Prof of Workplace Health Psychology Division of Psychology BCU www.health.bcu.ac.uk/craigjackson Mystery Health Problems 1 Mystery Health Problems 2 Mystery Health Problems 3 Linking Emotions with Physical Symptoms “The good physician treats the disease, but the great physician treats the person.” William Osler Non-Specific Symptoms Often missed in assessment Dualism “If you are distressed by anything external, the pain is not due to the thing itself, but to your estimate of it; this you have the power to revoke at any moment” Marcus Aurelius 180BC Dualism Mind / Body Divide Rene Descartes' Biopsychosocial Unification popular in last 10-15 years Traditional model of Disease Development Pathogen Modifiers Lifestyle Individual susceptibility Disease (pathology) Dominance of the biopsychosocial model Mainstream in last 15 years Hazard Illness (well-being) Psychosocial Factors Attitudes Behaviour Quality of Life Rise of the patient as a “psychological entity” Mental States & Physical Well-being “Triggering” Hypothesis Chinese # 4 Phillips et al. 2001 World cup 1998 Carroll et al. 2002 Stressful Events and Breast Cancer Chen et al. 1995 Scottish Heart Attack Deaths Evans et al. 2002 The “Baskerville” Effect Is disease real or is it in the mind? Linking Emotions with Physical Symptoms Which causes which? Prevalence of Non-Specific Symptoms Symptom Prevalence % Stuffy nose Headaches Tiredness Cough Itchy eyes Sore throat Skin rash Wheezing Respiratory Nausea Diarrhoea Vomiting Heyworth & McCaul, 2001 46.2 33.0 29.8 25.9 24.7 22.4 12.0 10.1 10.0 9.0 5.7 4.0 Modern day complaints Multiple Chemical Sensitivity Chronic Fatigue Syndrome Sick Building Syndrome Gulf War Syndrome Low-level Chemical Exposure Electrical Sensitivity Historical complaints Railway Spine Neurasthenia Combat Syndrome Physiological Response to Stress Chronic stress & Acute stress Pituitary Gland, Hypothalamus and Amygdala Adrenal glands = Secrete hormones Epinephrine Cortisol Heart Arteries Stomach Lungs Muscles = = = = = Glucocorticoids beats faster widen digestion stops faster / shallow tense Damage from Stress Arterial damage Increased glucocorticosteroids weaken immune system reduce bone mass reproductive suppression memory problems Anxiety Depression Tension Sleeping problems Apathy Apprehension Alienation Resentment Confidence Aggression Withdrawal Restlessness Indecision Worry Concentration Tired Common Chronic Ill-Health Complaints • Low Back Pain • Carpal Tunnel Syndrome • Cumulative Trauma Disorders • Tendonytis • Repetitive Strain Injury • Fibromyalgia • Irritable Bowel Syndrome • Chronic Fatigue FORMS OF CHRONIC PAIN & FATIGUE Those with heightened symptoms choose attributions to match concepts of what is currently acceptable in medicine External cause for illness preferred - patient becomes a helpless victim Chronic Patient’s Attributions of Ill-Health • Work • Environment Chemicals Stress Toxins Virus Allergies • Traumatic injury • Anatomy / Ergonomic “Exploit someone new today” Allergies – the role of psychology Allergies Somatization and Fashionable Diagnoses Somatoform Disorders (DSM IV category) “Somatization disorder” Psychiatric diagnosis Somatization 1. Rationalisation for psychosocial problems 2. Coping mechanism 3. Becomes a way of life Fibromyalgia Multiple Chemical Sensitivity Dysautonomia Reactive Hypoglycemia Irritable Bowel Syndrome Chronic Fatigue Syndrome 1. 2. 3. 4. Vague subjective multisystem complaints Lack of objective lab findings e.g no organic cause Semi-scientific explanations e.g “post-viral syndrome” Symptoms consistent with Depression, Anxiety or general unhappiness Case Summary of a Chronic Patient #1 Date Symptoms Referral Investigation Outcome 1980 (18) Abdominal pain GP --> surgical OP Appendicectomy Normal 1983 (21) Pregnancy (boyfriend in prison) GP --> obs and gynae OP 1985-7 (23-25) Bloating, abdominal blackouts (divorce) GP --> Gastro and neurology OP 1989 (27) Pelvic pain (wants sterilisation) GP --> obs and gynae Sterilised OP Pain persists for 2 years 1991 (29) Fatigue GP --> infectious diseases unit Diagnosis of ME by patient and self help group 1993 (31) Aching muscles GP --> rheumatology Mild cervical clinic spondylosis 1995 (34) Chest pain, breathless A&E --> chest clinic (child truanting) Termination All tests normal Nothing abnormal IBS diagnosis unexplained syncope Pain clinic - Tryptizol Nothing abnormal Refer to psychiatric services poss hyperventilation Psychological / Perceptual Process of Illness Internal Processes “Do I notice internal changes?” “Should I interpret them negatively?” “Should I think they are important?” External processes “Do I notice external sources?” “What should I believe about it?” “What should I do about it?” MENTAL SCHEMA Internal representation of the world (knowledge, attitudes, beliefs) What do we believe about health? What do we believe affects health? Factors Influencing Symptom Development Selective Internal Attention Tedious & un-stimulating environment Little communication Stressful environment Learned behaviours “Negative Affectivity” OVER FOCUS ON SYMPTOMS Comparisons Attributions Responses Blame Pessimism Factors Influencing Symptom Development Selective External Attention Heightened concern about risk involuntary uncontrolled lack of information dreaded consequences Mistrust of government / industry Attitudes about medicine Political agenda Legal agenda Social and political climate Media and pressure group activity OVER FOCUS ON SYMPTOMS Comparisons Attributions Responses Blame Pessimism Personality Hey. Hi H. On Are way you home. Left around lecture and earlydo you a cos fancy feel like crap. Next time! brew? A good sign or a bad sign? Personality type Optimism vs Pessimism Negative Affectivity Hardiness Irritable Bowel Syndrome Common digestive disorder Functional syndrome Traumatic life events, Personality disorders, Stress, Anxiety, Depression Somatization Not a psychological disorder Night-workers Loners Psychology important : how symptoms are perceived and reacted to Chronic Fatigue Syndrome • Non-specific subjective symptom • Overlap with psychiatric diagnoses (66%) • Chronic long-term inability and tiredness • Both Physical and Psychological fatigue • Most prevalent in white, middle class thirtysomething females • Fatigue dominates activities and life Mind over Matter A.A. Mason Congenital Ichthyosis Hypnosis Cured severe case of 16yr old male Mistaken C.I. for Acne Vulgaris Could not repeat successful treatment Bennedetti & the Turin Study Behavioural Responses to Diagnoses Hedonism Put life in order Premature grieving ADAPTIVE COPING Talk about it Planning Changes Sick Role Illness Behaviour Over-sensitivity to symptoms Premature death MALADAPTIVE COPING Drink Eat Substance use Four Pathways of Psychological Factors in Ill-Health 1) Part of Cause of Health Condition e.g. Influencing factors (personality) Risky behaviours 2) Part of Health Condition e.g. Stroke, Metastases 3) Effects of Health Condition e.g. Chronic ill-health, depression, anxiety, withdrawal 4) Psychological Interventions e.g. Therapeutic benefits Increased compliance Compensation Neurosis Pending litigation Treatment results often poor Some overt malingering Exaggerated illness due to: suggestion + somatization rationalization + distorted sense of justice victim status + entitlement Adverse legal / admin. systems Harden patient’s convictions With time, care-eliciting behaviour may remain permanent Bellamy, 1997 Compensation Neurosis Improvement in health..... ...may result in loss of status Patient compelled to guard against getting better Financial reward for illness is a powerful nocebo Exacerbates illness In a litigious society, will compensation neurosis become more widespread? Accident Neurosis • Failure to improve with treatment until compensation issue settled • Accident must occur in circumstances with potential for compensation payment • Inverse relationship to severity of injury - Accident neurosis rare in cases of severe injury • Low socio-economic status favors accident neurosis • Complete recovery common following settlement of compensation issue ??? Miller, 1961 Abnormal Illness Behaviour after Compensable Injury Accident neurosis Aftermath neurosis Attitudinal pathosis Compensatory hysteria Compensation neurosis Functional overlay Greenback neurosis Justice neurosis Post accident anxiety syndrome Postaccident fibromyalgia Profit neurosis Railway spine Traumatic hysteria Traumatic neurasthenia Triggered neurosis Vertebral neurosis Whiplash neurosis Accident victim syndrome American disease Barristogenic illness Compensationitis Fright neurosis Greek disease Invalid syndrome Perceptual augmenter Pensionitis Post-traumatic syndrome Psychogenic invalidism Secondary gain neurosis Symptom magnification syndrome Traumatic neurosis Unconscious malingering Wharfie’s back Mendelson, 1984 Secondary Gain Pre-disposition What is the Motivation? • Desire for attention • Punish spouse / others • Solve life’s problems • Cry for help • Diversion from work • Socially approved task avoidance sex with spouse work military duty Secondary Gain Pre-disposition Non-economic motivation? • Loneliness • Difficulty expressing emotional pain • Previous history of attention seeking when ill • Depression • Anxiety Secondary Gain Pre-disposition Who are the Potential Claimants? • Military patients nearing severance • Workers under retirement age • Low job satisfaction • Workers soon to be made redundant • Members of support groups Abnormal Illness Behaviour (Care Eliciting Behaviour) • Disability disproportionate to detectable illness • Constant search for disease validation • Relentless pursuit of “enlightened doctors” • Appeals to doctor’s responsibility • Attitude of personal vulnerability and entitlement to care by others • Avoidance of health roles due to lack of skills and fear of failure • Adoption of sick role due to rewards from family, friends, physicians • Behaviours which sustain the sick role - complaints, demands, threats Blackwell, 1987 Psychological Consequences of Chronic Illness Back Pain • Distress Money worries - Disablement • Reduced Quality of Life • Delay in seeking help Fear Denial • Depressed / Anxious • Increased somatic complaints Pain Fatigue Breathlessness Begins bad habit of seeking help too readily Adjustment Disorder – commonest psychiatric diagnosis Increased risk of suicide in early stages (of some conditions) Behavioural Yellow Flags of Chronic Ill-Health Indicative of long term chronicity and disability Back Pain • Negative attitude – back pain is harmful and disabling • Fear avoidance – stops trying things – disability mindset • Reduced activity • Expects passive treatment to be better than active treatment • Tendency to low morale, depression and social withdrawal • Social / Financial problems Somatization & Sick Role The process by which psychological needs are expressed in physical symptoms: e.g., the expression or conversion into physical symptoms of anxiety, or a wish for material gain associated with a legal action. 1. Auxiliary social support 2. Rationalisation for failure 3. Gratification of nurturance 4. Manipulate interpersonal relations 5. Articulate distress: cry for help 6. Misinterpretation of anxiety / depression symptoms 7. Over-vigilance for significant symptoms 8. Avoids stigma with a physical cause 9. Over-attention reflects learned behaviour 10. Amplification and Negative Affectivity 11. Primary, Secondary and Tertiary gains 12. Unexplained physical symptoms in trauma victims (e.g. abuse) Conclusion • Somatization influenced by numerous factors • Sick role resolves intrapsychic, interpersonal or social problems • Fashionable diagnoses have considerable overlap • Occupational and Environmental syndromes • Non specific and subjective complaints • Underlying depression, anxiety, and history of unexplained complaints • Mass communication + support groups = fashionable way to solve distress • Behavioural aspects of chronic patients – blame, refusal, over-reporting etc. 21st Century Satanic Mills Modern-Day Patients Patients more involved in their own care than even before The term “consultation” is disappearing Mistrust of Medicine e.g. Shipman, Allit, Meadows cases Less Mysterious and Powerful Change in what is expected from practitioners… …Has changed how practitioners view patients Emphasis on (1) risk reduction (2) public health (3) preventative behaviour “Do you know about statistics?” Some (older patients) still prefer to be told what the treatment will be Skill is in achieving the correct balance for each patient The benefits of support groups? The benefits of support groups?