* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download 3 rd Lecture
Survey
Document related concepts
Transcript
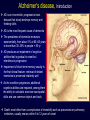
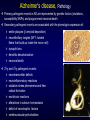
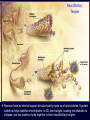
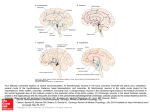
PHL 437/Pharmacogenomics Third Lecture (Alzheimer's disease) By Abdelkader Ashour, Ph.D. Phone: 4677212 Email: [email protected] Neurodegenerative diseases, Introduction Neurodegenerative disorders are characterized by progressive and irreversible loss of neurons from specific regions of the brain The most common neurodegenerative disorders include: Alzheimer's disease (AD), where the loss of hippocampal and cortical neurons leads to impairment of memory and cognitive ability Parkinson's disease (PD), in which extensive destruction of the dopaminergic neurons of the substantia nigra results in abnormalities in the control of movement The pharmacological therapy of neurodegenerative disorders is limited mostly to symptomatic treatments that do not alter the course of the underlying disease Symptomatic treatment for PD, where the neurochemical deficit produced by the disease is well defined, is, in general, relatively successful, and a number of effective agents are available The available treatments for AD are much more limited in effectiveness, and new strategies are urgently needed Alzheimer's disease, Introduction AD is an irreversible, progressive brain disease that slowly destroys memory and thinking skills AD is the most frequent cause of dementia The prevalence of dementia increases exponentially, from about 1% at 60–65 years to more than 30–35% in people > 80 yr AD produces an impairment of cognitive abilities that is gradual in onset but relentless in progression Impairment of short-term memory usually is the first clinical feature; retrieval of distant memories is preserved relatively well As the condition progresses, additional cognitive abilities are impaired, among them the ability to calculate, exercise visuospatial skills and use common objects and tools Death, most often from a complication of immobility such as pneumonia or pulmonary embolism, usually ensues within 6 to 12 years of onset Alzheimer's disease, Pathology Primary pathogenic events in AD are represented by genetic factors (mutations, susceptibility SNPs) and programmed neuronal death Secondary pathogenic events are associated with the phenotypic expression of: senile plaques (b-amyloid deposition) neurofibrillary tangles (NFT; twisted fibers that build up inside the nerve cell) synaptic loss dendritic desarborization neuronal death 3ory and 4ory pathogenic events: neurotransmitter deficits neuroinflammatory reactions oxidative stress phenomena and freeradical formation excitotoxic reactions alterations in calcium homeostasis deficit of neurotrophic factors cerebrovascular perturbations Beta-amyloid Plaques The presence of aggregates of b-amyloid (ABP; a short polypeptide of 42 to 43 aa) is a constant feature of AD Amyloid precursor protein (APP; expressed widely by neurons throughout the brain in normal individuals as well as in those with AD) is the precursor to amyloid plaque 1. 1. APP is a membrane glycoprotein (contains the ABP region (4 kDa) extending to 28 amino acids of the ectodomain 2. The production of b-amyloid from APP results from: Abnormal proteolytic cleavage of APP by the b-site APPcleaving enzyme BACE (b-secretase), generating a 99residue C-terminal fragment (C99) bound to the membrane α-Secretase cleaves APP at the ABP region to produce an 83-residue C-terminal fragment (C83) 2. γ-Secretase acts on the C99 and C83 substrates at the TM domain to produce C99-derived 4-kDa ABP Presenilin facilitates γ-secretase cleavage of APP 3. b-amyloid fragments come together in clumps to form plaques, disrupting the work of neurons. This affects the hippocampus and other areas of the cerebral cortex 3. Neurofibrillary Tangles Neurons have an internal support structure partly made up of microtubules. A protein called tau helps stabilize microtubules. In AD, tau changes, causing microtubules to collapse, and tau proteins clump together to form neurofibrillary tangles Alzheimer's disease, Neurochemistry Direct analysis of neurotransmitter content in the cerebral cortex shows a reduction of many transmitter substances mainly acetylcholine The anatomical basis of the cholinergic deficit is the atrophy and degeneration of subcortical cholinergic neurons that provide cholinergic innervation to the whole cerebral cortex The deficit in AD is complex, where it involves multiple neurotransmitter systems, including serotonin, glutamate and neuropeptides, and that in AD there is destruction of not only cholinergic neurons but also the cortical and hippocampal targets that receive cholinergic input Alzheimer's disease, Pharmacogenomics AD is a complex disorder associated with multiple genetic defects either mutational or of susceptibility origin Structural genomics studies demonstrated that more than 200 genes might be involved in AD pathogenesis regulating dysfunctional genetic networks leading to premature neuronal death Pharmacological treatment in AD accounts for 10–20% of direct costs, and fewer than 20% of AD patients are moderate responders to conventional drugs (donepezil, rivastigmine, galantamine, memantine), with doubtful cost-effectiveness The therapeutic response to drugs in AD has been shown to be genotype-specific Apolipoprotein E (Apo E) has been identified as the first of genetic risk factors for AD. Four distinct isoforms of this protein (which is well known to be involved in transport of cholesterol and lipids in blood) exist. Although all the isoforms carry out their primary role in lipid metabolism equally well, individuals who are homozygous for the Apo E 4 allele ("4/4") have a much higher lifetime risk of AD than do those homozygous for the Apo E 2 allele ("2/2") The mechanism by which the Apo E 4 protein increases the risk of AD is not known, but a secondary function of the protein in b-amyloid aggregation or processing of APP has been suggested Alzheimer's disease, Pharmacogenomics, contd. The accumulation of genetic defects in AD anticipates the onset of the disease and influence the therapeutic response of patients to conventional drugs Several missense mutations have been identified in APP that potentially result in early-onset AD The combination of 6 ApoE genotypes with 3 PS1 genotypes and 2 PS gene related variants generates the 36 most frequent genotypes in the AD population Amyloid production and deposition is increased in AD patients with PS mutations Patients with a defective PS2 gene exon 5 (PS2+) always show a worse therapeutic response than PS2- patients The therapeutic response in AD using cholinesterase inhibitors and/or noncholinergic compounds is genotype specific ApoE-3/4 patients are the best responders , whereas APOE-4/4 patients are the worst responders About 10–20% of Caucasians are carriers of defective cytochrome P450 2D6 polymorphic variants that alter the metabolism and effects of AD drugs