* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Slide 1
Ebola virus disease wikipedia , lookup
West Nile fever wikipedia , lookup
Trichinosis wikipedia , lookup
Schistosomiasis wikipedia , lookup
Human cytomegalovirus wikipedia , lookup
Leptospirosis wikipedia , lookup
Staphylococcus aureus wikipedia , lookup
Marburg virus disease wikipedia , lookup
Diagnosis of HIV/AIDS wikipedia , lookup
Epidemiology of HIV/AIDS wikipedia , lookup
Neonatal infection wikipedia , lookup
Microbicides for sexually transmitted diseases wikipedia , lookup
Methicillin-resistant Staphylococcus aureus wikipedia , lookup
Lymphocytic choriomeningitis wikipedia , lookup
Hepatitis B wikipedia , lookup
Hepatitis C wikipedia , lookup
Montessori School of Anderson
KNOWING THE
FACTS ABOUT
BLOODBORNE
PATHOGENS
1
The procedures established in Montessori School of Anderson Bloodborne
Pathogens Exposure Control Plan and OSHA Bloodborne Pathogens Standard
29 CFR 1910.1030 are crucial to the health and safety of our employees.
FAILURE TO FOLLOW THESE PROCEDURES
IS SUBJECT TO FINES BY OSHA.
Therefore, the following procedures are enforced:
Refusal or failure to wear or use the required personal safety equipment as directed by the
supervisor or as required by conditions at the work site as specified by these procedures
may result in disciplinary action.
Refusal or failure of supervisors to require that employees under their direction or
supervision wear or use safety equipment, or observe safety guidelines as required by
conditions at the work site, may result in disciplinary action.
2
UNIVERSAL PRECAUTIONS
• In any situation wherever we go, we must remember
to handle all blood and body fluids as if they are
infectious.
In doing this, we are protecting our self not only
from HIV, HBV, or HCV, but also from more
common germs such as staph, strep, E. coli, etc. We
must not become a victim ourselves! We must stop
and think before we react, taking time to prepare
ourselves in order to safely assist the victim.
3
PERSONAL PROTECTIVE EQUIPMENT
• A barrier used to separate you from exposure to other’s blood
or body fluid. The most used barrier is disposable gloves.
Latex gloves are permitted but due to so many latex allergies
being reported today, only VINYL or latex free gloves will be
used by the staff. UNLESS there is a documented allergy to
vinyl from the Nurse or patient. Gloves are supplied by each
department to their staff. If an employee has a latex allergy,
please notify the School Nurse for a latex-free glove. Other
items of personal protective equipment can be face shields,
goggles, disposable gowns, lab jackets, shoe covers, and any
item deemed necessary to protect the employees.
4
HANDWASHING
Cleansing of the hands often and thoroughly is one of the best
ways to prevent contamination or infection through contact with
blood or other germs carried in body fluids.
Hand washing with soap and water is the preferred
way to cleanse your hands as germs are removed
when we briskly rub fingers, palm and back of hand,
and around nails for about two minutes. Sing “The
Birthday Song” through twice and your hands should
be clean and germ-free! Rinsing and drying well
helps to make hand washing one of the best ways to
prevent infection. Cover with band-aids any cuts,
open sores, etc, and apply lotion often to chapped, dry
hands. If you are away from a water source, one of
the hand sanitizers, alcohol gels, baby wipes, etc., are
excellent ways to cleanse hands away from water
source. Remember to always rewash with soap and
water as soon as possible.
Adults: Remember to monitor when allowing young children to use hand sanitizers or alcohol
gel as the ethyl alcohol content is 60-70%. There have been reported cases of children licking
the gel off their hands and developing alcohol poisoning. A MSDS (Material Safety Data Sheet)
must be obtained and on file in the Health Room and Office if hand gels or sanitizers are used in
classrooms or during any school activities. Any child suspected of ingesting the sanitizer should
be immediately transported by EMS to the nearest Emergency Room.
5
WASTE DISPOSAL
DHEC governs waste disposal guidelines in South Carolina. Companies that produce 50+
pounds of infectious waste per month must adhere to SC DHEC Infectious Waste
Management Regulation R-61-105. Since Montessori School of Anderson does not
produce this amount at any site per month, the waste is simply handled as household waste.
It is double-bagged to prevent leakage/breakage and disposed of in the dumpster on site.
Teachers are responsible for letting the Custodial Staff know if there is liquid waste in their
trash can such as vomitus or blood so these bags can be emptied promptly and safely.
Sharps Containers are available in the Health Rooms for needles, broken glass chards, or
other forms of sharp or piercing objects. Containers are also placed in the Science Labs for
disposal of slides, blood smears, etc.
Sharps Containers are available through Nursing Services (226-5344 ext. 201) and should
be replaced when 2/3 full. The Sharps Containers will be picked up by Nursing Services
and carried to the health room to await pick-up by the vendor. SHARPS CONTAINERS
ARE NOT TO BE PLACED IN THE DUMPSTERS ON SITE. WASTE
MANAGEMENTS WILL FINE THE SCHOOL SITE FOR ANY BIOHAZARD
BAGS OR CONTAINERS FOUND AS THIS IS A VIOLATION OF DHEC LAW.
6
EXPOSURES
An exposure occurs when an individual’s blood or body fluid comes in contact
with another individual through at least one of several ways:
a splatter into the mouth, nose, or eye (s);
through intact skin such as by a bite or scratching;
a contaminated needle or sharp object that has been used by another
individual;
or through an area already open on the skin such as a sore, an unhealed
cut, or even a torn cuticle or fingernail.
Two things are very important if you feel an exposure has occurred. The two
things are:
(1) Immediately wash or flush the area with water and if not the mouth,
nose, or eye, use soap to cleanse area well. Alcohol can also be applied to
areas (other than mouth, nose, or eyes) to see if any burning or stinging
occurs from the alcohol contact.
(2) Go immediately to the Nurse (Nurse will report incident to Principal,
Assistant, or his/her designee.) Be certain you know the name of the 7
source individual (the person whose blood/body fluid you contacted).
EXPOSURES CONTINUED
IT IS VITALLY IMPORTANT TO REPORT AN EXPOSURE AS
SOON AS IT OCCURS. Delays in reporting the incident can result in
questions regarding the validity of your lab tests. This medical care is offered
to protect you as an employee.
•
The Nurse will also contact the parent of the source individual, the individual
whose blood or body fluid you contacted, and seek permission for him/her to
be tested for the same tests you have if you desire medical evaluation.
8
EXPOSURES CONTINUED
The Nurse will begin the follow-up procedure for you and will assist
you in documentation of the incident.
•
***Remember: An exposure is defined as “specific” eye, mouth,
other mucous membrane, non-intact skin , or parenteral (“piercing”)
contact with blood or other potentially infectious materials that
results from the performance of an employee’s duties.” However, if
there is some question as to whether this would be classified as an
exposure it is much better to document the incident and have it on
file.
•
If medical care is needed, it will be offered to you at no cost.
•
If you have an exposure and have not had the Hepatitis B vaccine
series and wish to have these, it will be provided to you at no cost.
•
If, for some reason, the School Nurse is not available, complete #1
above, then contact the administration at 226-5344 at Montessori
School of Anderson. Tell them you need to contact Nurse Merriman
regarding an exposure that has just occurred.
9
FACTS ABOUT HEPATITIS
• Inflammation of the liver. There are seven known types of viral hepatitis (A-G).
• Types A, spread mainly through food contaminated with feces, and B,
transmitted sexually or by injection, cause jaundice and flulike symptoms. The
hepatitis C virus spreads mostly by shared needles in intravenous drug use and
can cause liver cirrhosis and cancer after a long latent period. Until recently
there was no test to detect it in blood, and many people were exposed through
blood transfusions. Hepatitis D becomes active only in the presence of type B;
it causes severe chronic liver disease. Type E, like Type A, is transmitted by
contaminated food or water; its symptoms are more severe than Type A's and
can result in death. The hepatitis F virus (HFV), which was first reported in
1994, is spread like Type A and E. The hepatitis G virus (HGV), isolated in
1996, is believed to be responsible for many sexually transmitted and
bloodborne cases of hepatitis.
• Vaccines exist for types A and B (the second also prevents type D). Drug
treatment for B and C is not always effective. The other types may not need
drug treatment. Chronic active hepatitis causes spidery and striated skin
markings, acne, and abnormal hair growth. It results in liver tissue death
(necrosis) progressing to cirrhosis. Alcoholic hepatitis, from long-term
overconsumption of alcohol, can be reversed and cirrhosis prevented by early
treatment including quitting or sharply reducing drinking. Other drugs can also
cause noninfectious hepatitis. An autoimmune hepatitis affects mainly young
women and is treated with corticosteroids to relieve symptoms.
• More facts about Hepatitis http://www.cdc.gov/hepatitis/
10
FACTS ABOUT HIV
•
HIV is a virus. Viruses infect the cells that make up the human body and replicate
(make new copies of themselves) within those cells. A virus can also damage
human cells, which is one of the things that can make a person ill.
•
HIV can be passed from one person to another. Someone can become infected
with HIV through contact with the bodily fluids of someone who already has
HIV.
•
HIV stands for the 'Human Immunodeficiency Virus'. Someone who is diagnosed
as infected with HIV is said to be 'HIV+' or 'HIV positive'.
HIV lives in blood and other body fluids that contain blood or white blood cells.
People have gotten HIV through:
unprotected sexual intercourse with an HIV-infected person. This includes vaginal or
anal intercourse, and oral sex on a man or woman without a condom or other barrier.
Intercourse while a woman is having her period, or during outbreaks of genital sores or
lesions (caused by herpes and other sexually transmitted diseases) can increase the risk
of HIV transmission.
pregnancy, childbirth, and/or breastfeeding, where the virus is passed from mother to
child.
11
FACTS ABOUT HIV CONTINUED
•
sharing drug injection equipment (needles and/or works); or being
accidentally stuck by needles or sharp objects contaminated with
infected blood.
•
infected blood used in transfusions, and infected blood products used in
the treatment of certain diseases and disorders (like hemophilia), before
March, 1985. (Since 1985, federally mandated screening of the blood
supply has reduced the risk of transmission through this route to 1 in
255,000.)
•
transplanted organs from infected donors. (Routine screening of
organ donors also began in 1985.)
•
HIV and AIDS are not transmitted through casual contact (that
is, where no blood or body fluids are involved). HIV is what
gets passed from person to person. People don't "catch AIDS";
they "become infected with HIV."
For more facts visit http://www.cdc.gov/hiv/
12
FACTS ABOUT MRSA
(Methicillin-resistant Staphylococcus aureus )
http://www.cdc.gov/ncidod/dhqp/ar_mrsa_in_schools.html
MRSA and the Workplace
Staphylococcus aureus, often referred to simply as "staph," is a type of bacteria
commonly carried on the skin or in the nose of healthy people. Sometimes, staph can
cause an infection. Staph bacteria are one of the most common causes of skin infections
in the United States. Most of these skin infections are minor (such as pustules and boils)
and can be treated without antibiotics. However, staph bacteria also can cause serious
infections (such as surgical wound infections, bloodstream infections, and pneumonia).
Methicillin-resistant Staphylococcus aureus (MRSA) refers to types of staph that are
resistant to a type of antibiotic methicillin. MRSA is often resistant to other antibiotics,
as well. While 25% to 30% of the population is colonized with staph (meaning that
bacteria are present, but not causing an infection with staph), approximately 1% is
colonized with MRSA.
13
ADDITIONAL FACTS ABOUT MRSA
(Methicillin-resistant Staphylococcus aureus )
Can I get MRSA from someone at work?
MRSA is transmitted most frequently by direct skin-to-skin contact or contact with shared items or
surfaces that have come into contact with someone else's infection (e.g., towels, used bandages).
MRSA skin infections can occur anywhere. However, some settings have factors that make it easier for
MRSA to be transmitted. These factors, referred to as the 5 C's, are as follows: Crowding, frequent
skin-to-skin Contact, Compromised skin (i.e., cuts or abrasions), Contaminated items and surfaces, and
lack of Cleanliness. Locations where the 5 C's are common include schools, dormitories, military
barracks, households, correctional facilities, and daycare centers.
If I have MRSA, can I go to work?
Unless directed by a healthcare provider, workers with MRSA infections should not be routinely
excluded from going to work.
Exclusion from work should be reserved for those with wound drainage ("pus") that cannot be covered
and contained with a clean, dry bandage and for those who cannot maintain good hygiene practices.
Workers with active infections should be excluded from activities where skin-to-skin contact with the
affected skin area is likely to occur until their infections are healed.
What should I do if I think I have a staph or MRSA infection?
See your healthcare provider and follow your healthcare provider's advice about returning to work.
14
ADDITIONAL FACTS ABOUT MRSA
(Methicillin-resistant Staphylococcus aureus )
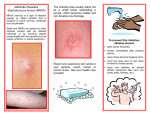
If I have staph, or a MRSA skin infection, what can I do to prevent the spread of MRSA at work
and at home?
You can prevent spreading staph or MRSA skin infections to others by following these steps:
Cover your wound. Keep areas of the skin affected by MRSA covered. Keep wounds that are draining
or have pus covered with clean, dry bandages. Follow your healthcare provider's instructions on proper
care of the wound. Pus from infected wounds can contain staph and MRSA, so keeping the infection
covered will help prevent the spread to others. Bandages or tape can be discarded with the regular trash.
Clean your hands. You, your family, and others in close contact should wash their hands frequently
with soap and warm water or use an alcohol-based hand sanitizer, especially after changing the bandage
or touching the infected wound.
Do not share personal items. Avoid sharing personal items such as uniforms, personal protective
equipment, clothing, towels, washcloths or razors that may have had contact with the infected wound or
bandage.
Talk to your doctor. Tell any healthcare providers who treat you that you have or had a staph or MRSA
skin infection.
What can my boss (employers) do to prevent the spread of staph or MRSA at the workplace?
Place importance on worker safety and health protection in the workplace
Ensure the availability of adequate facilities and supplies that encourage workers to practice good
hygiene
Ensure that routine housekeeping in the workplace is followed
Ensure that contaminated equipment and surfaces are cleaned with detergent-based cleaners or 15
Environmental Protection Agency (EPA)-registered disinfectants
Please view the mandatory Blood
Borne Pathogens video
http://www.schooltube.com/video/6f3f7609c9a947f0ac46/Blood-Borne-Pathogen-Video
16
You have completed your 2012 – 2013
Blood Borne Pathogens In-Service
Please complete the BBP quiz and place
in School Nurse’s mailbox. Once
competency is met, a certificate of
completion will be placed in your
employment file.
A
17