* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Cardiovascular System
Cardiac contractility modulation wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Heart failure wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Coronary artery disease wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Electrocardiography wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Artificial heart valve wikipedia , lookup
Cardiac surgery wikipedia , lookup
Myocardial infarction wikipedia , lookup
Jatene procedure wikipedia , lookup
Atrial septal defect wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Atrial fibrillation wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
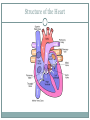
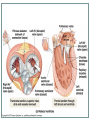
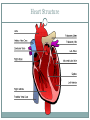
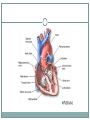
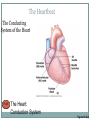
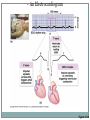
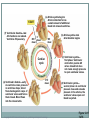
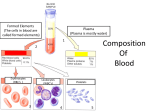
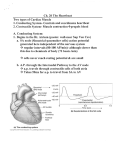
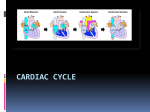
Cardiovascular System THE HEART The Heart Size: “fist size” 250 grams in females 350 grams in males Location: Medial cavity of the thorax 2/3 lies to the left of the sternum The Heart Base: widest part posterior Superior surface- 9 cm wide, directed toward the right shoulder Apex- directed inferiorly toward left hip Rests on diaphragm Point of Maximum Intensity: PMI Site where the apex is against the chest wall, between 5th and 6th rib. Pericardium Pericardium: double-walled fibersernous sac membrane which: 1. encloses the heart 2. anchors the heart Pericardium Fibrous Pericardium Serous Pericardium Tough dense Thin slippery connective tissue. Protects and anchors heart to sternum, diaphragm, and major vessels the enter and exit Prevents over distension of heart membrane Parietal layer: Lines fibrous pericardium Pericardial Cavity: space filled with pericardial fluid (prevents friction) Visceral Pericardium Lines surface of heart, connective tissue Wall of Heart Epicardium- composed of serous tissue and mesothelium outer thin layer 2. Myocardium- composed of cardiac muscle tissue1. 1. 2. Bulk of heart- layer that contracts (involuntary) Cells are tethered together by a layer of fiberous tissue that crosses 3. Endocardium- a glistening white sheet of endothelium resting on a layer of connective tissue. 1. 2. Lines heart chambers Continuous over valves and throughout vascular system. Heart Chambers Atria Ventricles 2 Atria (atrium) receive blood from veins 2 ventricles – pumping organs Auricle: an appendage that increases the atria’s volume capacity. – Pectinate muscles: muscle bundles that run parallel to one another and allow atrium to expand and contract. – Interatrial Septum: divides right and left atrium Foramen ovalis- opening between atria before birth- closes at birth and forms the fossa ovale (a dent) – Right Ventricle: pumps to the lungs Left Ventricle: pumps to the systemic circulation Interventricular Septum: Divides the left and right ventricles Structure of the Heart Grooves on the Surface Atrialventricular groove Coronary Sulcus Encircles juncitino of atria and ventricles Anterior Interventricle Sulcus: Marks the anterior portion of the interventricular septum Sulci: contains coronary blood vessels and fat Heart Valves Atrioventricular Valves (AV) Prevent back flow into the atria during ventricular contraction Right Atrioventricular Valve (tricuspid) Left Atrioventricular Valve (bicuspid, mitrovalve) Semilunar Valves Prevent back flow into the ventricles Aortic Semilunar- left side Pulmonary Semilunarright side Heart Structure Blood Flow Path of Nerve Impulse Through Heart 1. Sinoatrial node (SA Node) (Pacemaker) Mass of nerve tissue in right atrial wall near opening of superior vena cava- connected to medulla oblongata 2. Down the atria 3. Atrioventricular node collects 4. Passed to bundle of HIS in interventricular septum 5. Down Perkengie Network to Apex 6. Up across Ventricle – out of artery The Heartbeat The Conducting System of the Heart PLAY The Heart: Conduction System Figure 12-9(a) SA node activity and atrial activation begin. SA node Time = 0 Stimulus spreads across the atrial surfaces and reaches the AV node. AV node Elapsed time = 50 msec There is a 100-msec delay at the AV node. Atrial contraction begins. AV bundle Bundle branches Elapsed time = 150 msec The impulse travels along the interventricular septum within the AV bundle and the bundle branches to the Purkinje fibers. Elapsed time = 175 msec The impulse is distributed by Purkinje fibers and relayed throughout the ventricular myocardium. Atrial contraction is completed, and ventricular contraction begins. Elapsed time = 225 msec Purkinje fibers Copyright © 2007 Pearson Education, Inc., publishing as Benjamin Cummings Figure 12-9(b) 1 of 6 An Electrocardiogram Figure 12-10 Nervous Control of Heart Rate 1. Cardiac Acceleratory Centerincreased heart rate- connected to S.A. node by cervical sympathetic ganglion 2. Cardiac Inhibitory CenterVagus Nerve- decreases 3. Bainbridge Reflexincreases HR due to an increased flow of blood back to heart because of exercise 4. Aortic Arch Reflexdecreased HR due to increase of blood pressure in aorta 5. Carotid Sinuscan increase HR when Blood Pressure drops or decrease HR when blood pressure rises Chemical Controls Epinephrine: speeds up Noradrenaline: speeds up Thoroxyine: speeds up Sodium: speeds up, Potassium: slows down Calcium: speeds up Nicotine: speeds up initially, then slows down Cardiac Cycle 2 atria contract (ventricles relax) 2. 2 ventricles contract (atria relax) 1. Systole- contraction (chamber empties) Diastole- chamber filling (relaxation) Normal 120/80 Average cardiac cycle takes .8 seconds (a) Atriole systole begins: Atrial contraction forces a small amount of additional blood into relaxed ventricles. START (f) Ventricular diastole—late: All chambers are relaxed. Ventricles fill passively. 800 msec 0 msec 100 msec Cardiac cycle (e) Ventricular diastole—early: As ventricles relax, pressure in ventricles drops; blood flows back against cusps of semilunar valves and forces them closed. Blood flows into the relaxed atria. 370 msec Copyright © 2007 Pearson Education, Inc., publishing as Benjamin Cummings (b) Atriole systole ends atrial diastole begins (c) Ventricular systole— first phase: Ventricular contraction pushes AV valves closed but does not create enough pressure to open semilunar valves. (d) Ventricular systole— second phase: As ventricular pressure rises and exceeds pressure in the arteries, the semilunar valves open and blood is ejected. Figure 12-11 1 of 6 Stroke Volume: Amount of blood ejected from one ventricle in one contraction (80 ml) Cardiac Output: Amount of blood leaving heart in one minute CO = (HR) (SV)