* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Cardiac Monitoring
Survey
Document related concepts
Coronary artery disease wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Heart failure wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Cardiac surgery wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Jatene procedure wikipedia , lookup
Myocardial infarction wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Ventricular fibrillation wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
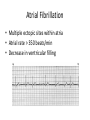
Atrial fibrillation wikipedia , lookup
Transcript
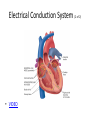
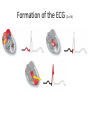
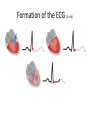
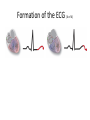
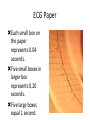
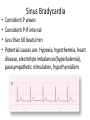
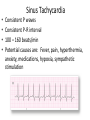
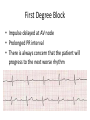
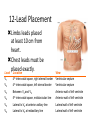
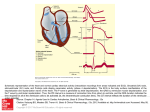
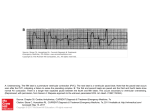
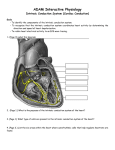
Cardiac monitoring Egan’s Ch. 17, CARC Ch. 11 Objectives (1 of 2) 1. To gain an understanding of basic terminology and techniques of cardiac monitoring. 2. To give you the knowledge and tools you need to assist the advanced provider with the use and implementation of an ECG. 3. To better understand the basic anatomy and physiology of the heart. Objectives (2 of 2) 4. Identify the components of basic cardiac arrhythmias (because many times the RTs are with the patient during the onset of the initial event). 5. Evaluate the rate and rhythm of a patient’s cardiovascular system, and become familiar with the normal ECG. 6. Familiarize yourself with and apply 4-lead electrodes and identify placements for the 12lead systems. Cardiac Monitoring • Use of 12-lead ECGs in the hospital is essential for cardiac patients. • Early identification of AMIs allows hospitals to be prepared. • The RT should know how to place electrodes and leads. Electrical Conduction System (1 of 2) • A network of specialized cells in the heart • Conducts electrical current throughout the heart • The flow of electrical current causes contractions that produce pumping of blood. VIDEO The Process of Electrical Conduction • Electrical conduction occurs through a pathway of special cells. • Automaticity – Ability of heart cells to generate a spontaneous electrical impulse • Sinoatrial (SA) node: the heart’s main pacemaker – Paces at a ventricular rate of 60–100 beats/min **Any beat that originates outside the SA node is called “ectopic”** The Process of Electrical conduction • Atrioventricular Junction- electrical bridge between atria and ventricles, comprised of: – (AV) node – Bundle of His • AV node – Acts as secondary (backup) pacemaker – Paces at a ventricular rate of 40-60 beats/min – Impulse is temporarily delayed here to allow better filling of the ventricles – Protects ventricles from excessively fast rates The Process of Electrical conduction • Bundle branches • Purkinje fibers – Fingerlike projections that pass electrical impulses throughout myocardium to create a coordinated contraction of the ventricles Electrical Conduction System (2 of 2) • VIDEO Formation of the ECG (1 of 4) Formation of the ECG (2 of 4) Formation of the ECG (3 of 4) Formation of the ECG (4 of 4) Electrodes and Waves Electrodes pick up electrical activity of the heart. The ECG Complex One complex represents one beat in the heart. Complex consists of P, QRS, and T waves. ECG Paper Each small box on the paper represents 0.04 seconds. Five small boxes in larger box represents 0.20 seconds. Five large boxes equal 1 second. Normal Sinus Rhythm Consistent P waves Consistent P-R interval (0.12-0.20 seconds) 60–100 beats/min QRS < 0.12 seconds • • • • Sinus Bradycardia Consistent P waves Consistent P-R interval Less than 60 beats/min Potential causes are: Hypoxia, hypothermia, heart disease, electrolyte imbalances(hyperkalemia), parasympathetic stimulation, hypothyroidism • • • • Sinus Tachycardia Consistent P waves Consistent P-R interval 100 – 160 beats/min Potential causes are: Fever, pain, hyperthermia, anxiety, medications, hypoxia, sympathetic stimulation First Degree Block • Impulse delayed at AV node • Prolonged PR interval • There is always concern that the patient will progress to the next worse rhythm 2nd Degree Type I (Wenckebach) • PR progressively longer until a QRS is dropped. 2nd Degree Type II (Mobitz) • Nonconducted P waves followed by conducted P waves. 3rd Degree Heart Block • Ventricles and atria beat independently of one another. • There is no relationship between the P waves and QRS complexes • The patient will need a pacemaker – Usually a temporary pacer (TCP) until a permanent one can be inserted Atrial Flutter • • • • • Rapidly firing ectopic site in atria Characteristic “sawtooth” pattern At risk for thrombi Rate: 180-400 beats/min May progress to atrial fibrillation Atrial Fibrillation • Multiple ectopic sites within atria • Atrial rate > 350 beats/min • Decrease in ventricular filling PVC’s • Wide and bizarre QRS complex is the most distinguishing feature • No P wave prior to PVC • Bigeminyand trigeminy • Unifocal and Multifocal – Multifocal is more concerning because there are multiple irritated areas in the ventricles • Occasional PVC is ok but > 6/min is a sign of irritability • May progress to ventricular tachycardia • Treatment PVC’s Supraventricular Tachycardia (SVT) • Impulse moves from atria – ventricles – atria (circular) • Rate: 160-220 beats/min • P waves may be unidentifiable, normal QRS • Treatment – If stable and narrow complex can try adenosine or vagal maneuvers – If unstable, then immediate cardioversion Ventricular Tachycardia Three or more PVC’s in a row Rate: 100-250 beats/min No distinguishable P waves Precedes or follows V-fib Treatment If stable, treat with amiodarone If unstable with a pulse, then cardioversion Pulseless VT is treated with CPR and defibrillation just like VF Ventricular Fibrillation Rapid, completely disorganized rhythm Deadly arrhythmia that requires immediate treatment A new onset is coarse and will progress to fine VF which is harder to defibrillate Fine VF can be confused with asystole Treatment is CPR and immediate defibrillation Pulseless Electrical Activity (PEA) • Pattern does not generate a pulse. • May show normal QRS complexes • Can be any kind of a pattern from NSR to one or two complexes • Treatment is CPR and identify the cause (H’s and T’s) Asystole • Complete absence of electrical cardiac activity • Patient is clinically dead. • Decision to terminate resuscitation efforts depends on local protocol. Cardiac Monitors • May be 3-, 4-, or 12-lead system • Compact, light, portable • Many monitors now combine functions beyond ECG. 4-Lead Placement Four leads are called limb leads. Leads must be placed at least 10 cm from heart. 12-Lead ECG • Used to identify possible myocardial ischemia • Studies show 12-lead acquisition takes little extra time. • Early identification of acute ischemia and accurate identification of arrhythmias 12-Lead Placement Limbs leads placed at least 10 cm from heart. Chest leads must be placed exactly. Lead Location View V1 4th intercostal space, right sternal border Ventricular septum V2 4th intercostal space, left sternal border Ventricular septum V3 Between V2 and V4 Anterior wall of left ventricle V4 5th intercostal space, midclavicular line Anterior wall of left ventricle V5 Lateral to V4 at anterior axillary line Lateral wall of left ventricle V6 Lateral to V5 at midaxillary line Lateral wall of left ventricle Holter monitoring • Portable, battery powered recording device • Done over 24 hours • Useful in patients experiencing irregular heart beats on an inconsistent basis. Troubleshooting • Clean skin. • Use benzoin. • Shave hair.