* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Cardiovascular System Powerpoint
Cardiac contractility modulation wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Heart failure wikipedia , lookup
Artificial heart valve wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Electrocardiography wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Coronary artery disease wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Myocardial infarction wikipedia , lookup
Cardiac surgery wikipedia , lookup
Atrial septal defect wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
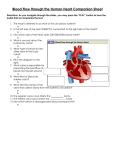
Basic Definitions • • • • • Arteries carry blood away from the heart Veins carry blood back to the heart Arterioles = small arteries Venules = small veins Capillaries: smallest vessels where nutrient, waste and gas exchange take place. So narrow that blood cells proceed through single file. Walls are a single layer of epithelium. Summary Concepts • The human heart has four chambers left and right atria, left and right ventricles • The human heart has four valves two atrioventricular valves (tricuspid and mitral) two semilunar valves (aortic semilunar and pulmonary semilunar) • Pulmonary circulation: starts as blood leaves the right ventricle and enters the pulmonary trunk -> lungs -> pulmonary veins -> left atrium • Systemic circulation: starts as blood leaves the left ventricles -> aorta -> head, arms, legs, body -> vena cava -> right atrium Coronary circulation: provides blood to the heart muscle (myocardium). Aorta -> coronary arteries -> heart muscle -> cardiac veins -> vena cava. The Heart and the Pulmonary Circulation Subclavian artery Superior vena cava Left carotid artery Brachiocephalic artery Aortic arch Pulmonary trunk Pulmonary arteries Pulmonary veins left atrium Right Atrium Coronary arteries Cardiac veins Left Ventricle Right ventricle Inferior vena cava Valves and Conduction Fibers of the Heart Atria: receive blood from principle veins and assist in filling the ventricles Ventricles: pump blood under high pressure into pulmonary trunk and the aorta. Left Atrium Aortic Semilunar Right Atrium Pulmonary Semilunar Bicuspid (mitral) Left Ventricle Tricuspid Right Ventricle Tissues of the Heart • • • • • Pericardium: serous membrane sack surrounding the heart Epicardium: serous membrane on outer surface of the heart Myocardium: muscle of the heart Endocardium: membrane lining the interior of the heart Chordae tendonae: “heart strings” that guide the atrioventricular valves. • Papillary muscle: small muscles that anchor the chordae tendonae to the ventricular walls. Heart Valves are passive and move According to pressure gradients (like a loose screen door in a breeze) Atrioventricular Semilunar Aorta Superior Vena Cava 7 8 Pulmonary trunk Pulmonary Vein 4 3 5 1 6 2 video Inferior Vena Cava The Cardiac Cycle Diastole: period of relaxation And ventricular filling Atrial Systole: atria contract force additional blood into the ventricles. Ventricular Systole: ventricles contract and force blood into pulmonary trunk and aorta. Purkinje Fibers Conduction System Video Electrical Recovery of Myocardium R P T Q S Electrocardiogram Cardiac Output Stroke Volume (mL/beat) X Heart Rate (beats/min) = Cardiac Output (mL/min) 75 mL/beat X 72 beats/min. = 5400 mL/min. Questions 1. Do athletes have greater or lesser demands for oxygen than non-athletes? 2. Do athletes have greater or lesser resting heart rates than non-athletes? 3. How do you reconcile this observation? Affects of Athletic Training - Stroke volume increases, heart rate decreases 95 mL/beat X 60 beats/min. = 5700 mL/min. Even though the athlete has a lower resting heart rate, s/he has a greater Cardiac Output than the untrained person. Cardiac Center in the Medulla Controls two nerves that lead to the heart 1. accelerator nerve (sympathetic) *acts on the sinoatrial node and ventricles *increases heart rate using norepinephrine 2. vagus nerve (parasympathetic) *acts on the sinoatrial node *decreases heart rate using acetylcholine Regulation of Heart Rate Cardiac Center (medulla) Vagus nerve Accelerator nerve Sensory nerves Proprioceptors Baroreceptors and Chemoreceptors in the carotid and aortic arteries Sensory Inputs 1. Proprioceptors (Am I moving more?) 2. Baroreceptors (Is my blood pressure low?) 3. Chemoreceptors (Is my CO2 high or O2 low?) Motor Output 1. Accelerator nerve (sympathetic) (releases norpepinephrine) increase rate and force 2. Vagus nerve (parasympathetic) decrease rate Arteries = elastic elements Veins = capacitance elements compliant valves skeletal muscles = Resistance Vessels Large arteries are elastic absorb kinetic energy store potential energy Arterioles and pre-capillary Sphincters are muscular constrict add resistance dilate reduce resistance Each organ has its own set of Arterioles, and capillary beds Which may be dilated or constricted The microcirculation 1. Capillary exchange by diffusion nutrients Vitamins CO2 O2 wastes 2. Capillary exchange by bulk flow Starling hypothesis - capillaries have low permeability to protein (osmotic effect) - hydrostatic pressure decreases as blood passes through Net outward pressure = 11 mmHg Net inward pressure = -9 mmHg Formation of Lymph • Edema • Alcoholism • Elephantiasis