* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Slide 1
Cardiovascular disease wikipedia , lookup
Heart failure wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Cardiac surgery wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Coronary artery disease wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Jatene procedure wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Myocardial infarction wikipedia , lookup
Ventricular fibrillation wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Atrial fibrillation wikipedia , lookup
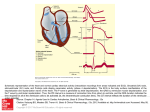
I- Electrophysiology of the heart Normal heart rate: 60-90 beats minute Abnormal: 60 beats min Bradycardia 90 beats min Tachycardia 2 Conducting System of the Heart: SA node, AV node, Purkinj fibers Contractile tissue of the heart Atrial & Ventricular muscles Impulse Propagation: SA node AV-node Bundle of His Purkinje fibers ventricle. SA node is the initial pacemaker. 3 P wave = atrial depolarization The PR interval corresponds to the time lag from the onset of atrial depolarization to the onset of ventricular depolarization. 4 In resting state: Myocytes are permeable to K+ only. RMP determined by K+ conc. (Ko & Ki). Ki is 150 mmol/L and Ko 4 mmol/L. Resting membrane potential ranges: From – 80 to -90 mv in contractile cells From -60 to -70 mv in pacemaker cells (SA node, AV node and His-Purkinj fibers) . Phase 4 of AP represents RMP. 5/24/2017 2:33:26 AM 5 The ECG is recorded at a speed of 25 mm/sec, and the voltages are calibrated so that 1 mV = 10 mm in the vertical direction. Therefore, each small 1-mm square represents 0.04 sec (40 msec) in time and 0.1 mV in voltage. Because the recording speed is standardized, one can calculate the heart rate from the intervals between different waves. 6 P Wave • P duration < 0.12 sec • P amplitude < 2.5 mm • The normal deflection of the P wave is upright (positive) in leads I, II, and aVf. PR Interval: 0.12 - 0.20 sec QRS Complex • QRS Duration: 0.06 - 0.10 sec • QRS duration < 0.10 sec T wave is always upright in leads I, II, V3-6, and always inverted in lead aVR. 7 Ca++ Na+ K+ K+ Na+ 5/24/2017 2:33:26 AM 8 Phase O: Na+ enter the cells (fastly). Phase 1: Na+ levels equalize & transient efflux of K+. Phase 2: Ca++ enter the cells. Phase 3: K+ efflux from the cells. Phase 4: Spontaneous depolarization in SA node, AV node and His-Purkinj system) Na and Ca influx. 5/24/2017 2:33:26 AM 9 1. Refractory Period (RP): Phases 1,2 & 3. ERP (absolute refractory period): Phases 1 & 2 represent ERP (no response to any stimuli). RRP (Relative Refractory Period): Phase 3 represents RRP (respone only to strong stimuli. 2. Action Potential Duration: Phases 1,2 & 3: - During APD, the heart in refractory state and no impulse propagation. 5/24/2017 2:33:26 AM 10 Arrhythmias or dysrhythmias: Disturbances in cardiac rhythm (rate and/or regularity) due to abnormality in impulse origination (ectopic beats) or abnormality in conductivity (reentry) or both. Antidysrhythmic drugs: Drugs which suppress abnormalities of automaticity and/or conductivity by blocking specific ion channels (Na+, Ca++ and K+) or by altering autonomic functions. 11 Electrolyte disturbances: hypokalemia, hyperkalemia). Cardiac ischemia & MI: e.g., hypoxia O2 supply. Structural damage: changing the conduction pathway. Drug toxicity:: e.g., digitalis toxicity. Autonomic changes: sympathetic or vagal tone. 12 Abnormal automaticity: Altered normal automaticity. Ectopic beats Triggered automaticity. Abnormal conductivity Re-entry 5/24/2017 2:33:26 AM 13 In pacemaker cells (SA, AV & H-P fibers. Precipitated by: Autonomic disturbance: Sympathetic activity sinus & nodal tachycardia. vagal tone sinus bradycardia. Hypokalemia sinus tachycardia. 14 A) Supraventricular arrhythmias: • • • • • • • Sinus tachycardia 90 beats min. Sinus bradycardia 60 beats min. Premature atrial contractions (PACs) Atrial tachycardia (regular pulse; up to 200 beats min). Atrial flutter (regular pulse; 200-300 beats min). Atrial fibrillation (irregular pulse; 300 beats min). Nodal tachycardia (AV nodal reentry; a common type of [SVT]). B) Ventricular Arrhythmias: • • • • • Premature ventricular contractions (PVCs), Ventricular tachycardia (VT), Ventricular fibrillation (VF), Bundle branch block, Torsade de pointes. N.B. Ventricular arrhythmias are life-threatening arrhythmias. 15 1- first degree 2- second degree - mobitz 1 ( wenckebach ) -Mobitz 2 3- third degree or complete A. Heart block Impaired myocardial conduction that occurs when electrical impulses encounter tissue that is electronically inexcitable, resulting in an arrhythmia First degree Caused by increased vagal tone or functional conduction impairment H/P = asymptomatic ECG = PR >0.2 sec , regular PR prolongation without skipped QRS Treatment = none necessary 1- first degree 2- second degree - mobitz 1 ( wenckebach ) -Mobitz 2 3- third degree or complete A. Heart block Impaired myocardial conduction that occurs when electrical impulses encounter tissue that is electronically inexcitable, resulting in an arrhythmia First degree Caused by increased vagal tone or functional conduction impairment H/P = asymptomatic ECG = PR >0.2 sec , regular PR prolongation without skipped QRS Treatment = none necessary Second degree—Mobitz I (Wenckebach) Caused by intranodal or His bundle conduction defect, drug effects (βblockers, digoxin, calcium channel blockers), or increased vagal tone H/P = asymptomatic ECG = progressive PR lengthening until skipped QRS; PR progression, then resets and begins again Treatment = adjust doses of medications associated with heart block; treatment usually not necessary unless symptomatic bradycardia is present (pacemaker indicated) Second degree—Mobitz II Caused by an infranodal conduction problem (bundle of His, Purkinje fibers) H/P = usually asymptomatic ECG = randomly skipped QRS without changes in PR interval Treatment = ventricular pacemaker Complications = can progress to third-degree heart block Complete or third-degree heart block Cause is absence of conduction between atria and ventricles H/P = syncope, dizziness, hypotension ECG = no relationship between P waves and QRS Treatment = avoid medications affecting atrioventricular (AV) conduction; ventricular pacemaker Mechanism of atrioventricular nodal reentry tachycardia. (A) Action potential reaches division in conduction pathway with both fast and slow fibers. (B) Conduction proceeds quickly down fast pathway to reach distal fibers and also proceeds up slow pathway in retrograde fashion. (C) Impulse returns to original division point after fibers have repolarized, allowing a reentry conduction loop and resultant tachycardia. AV, atrioventricular. Mechanism of atrioventricular reentry tachycardia as seen for Wolff-Parkinson-White syndrome. (A) Action potential passes through AV node and encounters accessory pathway during conduction to ventricles. (B) Accessory pathway conducts action potential back to AV node. (C) Return of secondary action potential to AV node completes reentry loop and results in tachycardia. AV, atrioventricular node; AP, accessory pathway. B. Paroxysmal supraventricular tachycardia (PSVT) Tachycardia (HR >100 bpm) arising in atria or AV junction Occurs mostly in young patients with healthy hearts Cause frequently is reentry anomaly AV nodal reentry— - presence of both slow and fast conduction pathways in AV node; - conduction proceeds quickly through fast pathway and progresses up slow pathway in retrograde fashion; - conduction loop is created, resulting in reentrant tachycardia AV reentry as found in Wolff-Parkinson-White (WPW) syndrome— similar to AV nodal reentry, but instead of fast and slow pathways existing in the AV node, a separate accessory conduction pathway exists between the atria and ventricles that returns a conduction impulse to the AV node to set up a reentry loop; ECG shows a delta wave (i.e., slurred upstroke of the QRS) and shortened PR H/P = sudden tachycardia; possible chest pain, shortness of breath, palpitations, syncope ECG = P waves hidden in T waves; 150–250 bpm HR; normal QRS Treatment = carotid massage or Valsalva maneuver may halt an acute arrhythmia, but cardioversion or calcium channel blocker is required in cases of hemodynamic instability; pharmacologic therapy (e.g., β-blocker or calcium channel blocker for AV nodal reentrant tachycardia and type IA or IC antiarrhythmic for WPW syndrome) or catheter ablation of accessory conduction pathways is frequently used for long-term control in symptomatic patients Antiarrhythmics, other than class IA or IC, are contraindicated for WPW syndrome because they can speed up conduction through the accessory pathway. C. Multifocal atrial tachycardia (MAT) Caused by several ectopic foci in the atria that discharge automatic impulses (multiple pacemakers), resulting in tachycardia H/P = usually asymptomatic ECG = variable morphology of P waves; HR >100 bpm and PR intervals and the irregular ventricular rate Treatment = calcium channel blockers or β-blockers acutely; catheter ablation or surgery to eliminate abnormal pacemakers D. Bradycardia HR <50 bpm Caused by increased vagal tone or nodal disease Risk factors = elderly, history of CAD H/P = frequently asymptomatic; possible weakness, syncope Predisposition to development of ectopic beats Treatment = stop precipitating medications; pacemaker if severe E. Atrial fibrillation (Afib) Lack of coordinated atrial contractions with independent sporadic ventricular contractions Caused by rapid, disorderly firing from a second atrial focus Risk factors = pulmonary disease, CAD, HTN, anemia, valvular disease, pericarditis, hyperthyroidism, rheumatic heart disease (RHD), sepsis, alcohol use H/P = possibly asymptomatic; shortness of breath, chest pain, palpitations, irregularly irregular pulse ECG = no discernible P waves, irregular QRS rate Treatment = anticoagulation; rate control via calcium channel blockers, βblockers, or digoxin; electric or chemical (i.e., class IA, IC, or III antiarrhythmics) cardioversion if presenting within initial 2 days; cardioversion can be performed in delayed presentation if absence of thrombi is confirmed by transesophageal echocardiogram; if presenting after 2 days or if thrombus is seen on ECG, then anticoagulate and wait 3–4 weeks before cardioversion; AV nodal ablation can be considered for recurrent cases Complications = increased risk of MI, heart failure; poor atrial contraction causes blood stasis, which leads to mural thrombi formation and a risk of embolization F. Atrial flutter (Aflutter) Caused by rapid firing of an ectopic focus in the atria Risk factors = CAD, congestive heart failure (CHF), chronic obstructive pulmonary disease (COPD), valvular disease, pericarditis H/P = possibly asymptomatic; palpitations, syncope ECG = regular tachycardia >150 bpm with occasionally set ratio of P waves-toQRS; sawtooth pattern of P waves , preceding QRS. Treatment = rate control with calcium channel blockers, β-blockers; electrical or chemical (class IA, IC, or III antiarrhythmics) cardioversion if unable to be controlled with medication; catheter ablation to remove ectopic focus may be possible in some cases Complications = may degenerate into Afib G. Premature ventricular contraction (PVC) Caused by ectopic beats from a ventricular origin Common, frequently benign; can also be caused by hypoxia, abnormal serum electrolyte levels, hyperthyroidism, caffeine use H/P = usually asymptomatic; possible palpitations, syncope ECG = early , and wide QRS without preceding P wave followed by brief pause in conduction , Treatment = none if patient is healthy; β-blockers in patients with CAD Complications = associated with increased risk of sudden death in patients with CAD , PVCs become concerning for the development of other ventricular arrhythmias if there are >3 PVCs/min H. Ventricular tachycardia (Vtach) Series of 3+ PVCs with HR 160–240 bpm Risk factors = CAD, history of MI H/P = possibly asymptomatic if brief; palpitations, syncope, hypotension ECG = series of regular, wide QRS complexes independent of P waves Treatment = electrical cardioversion followed by antiarrhythmic medications (class IA, IB, II, or III); for recurrent Vtach, internal defibrillator may be necessary (senses ventricular arrhythmia and automatically releases electric pulse to restore normal rhythm) Complications = sustained Vtach can quickly deteriorate into Vfib if not corrected I. Ventricular fibrillation (Vfib) Lack of ordered ventricular contraction leads to no CO and is rapidly fatal Frequently occurs after severe MI, post-Vtach Risk factors = CAD, MI H/P = syncope, hypotension, pulselessness ECG = totally erratic tracing; no P waves or QRS Treatment = CPR, immediate electric (± chemical) cardioversion Amiodarone also functions as an Na channel blocker.