* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Type 2 DM
Survey
Document related concepts
Transcript
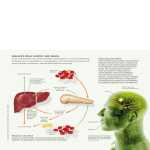
ANTIDIABETIC DRUGS (Abstract) © Assoc. Prof. Iv. Lambev, PhD E-mail: [email protected] Glucose occupies a central position in metabolism as the predominant substrate for energy production. NORMOGLYCEMIA 2.8-6.1 mmol/l Suspected diabetes mellitus 75 g glucose p.o.: 2 h later random blood glucose less than 8 mmol/l 8 to 11 mmol/l greater than 11 mmol/l Normal Impaired glucose tolerance Diabetes 1/3 become normal 1/3 remain IGT 1/3 become diabetic Worldwide prevalence of diabetes mellitus Diabetes mellitus (DM) Type 1 DM (beta-cell destruction) – about 10% of all patients. a) Autoimmune DM (so called insulin-dependent DM – IDDM or juvenile-onset diabetes). It results from autoimmune mediated destruction of the beta cells of the pancreas. The rate of destruction is quite variable (and may reach 80% of beta- cells of Langerhans islets), being rapid in some individuals and slow in others. The rapidly progressive form is commonly observed in children, but also may occur in adults. The slowly progressive form generally occurs in adults and is sometimes referred to as latent autoimmune DM in adults (LADA). b) Idiopathic type 1 DM, which have no known etiology (have no evidence of autoimmunity). This form is more common among individuals of African and Asian origin. Patients periodically develops ketoacidosis. Type 2 DM (predominantly insulin resistance with relative insulin deficiency or predominantly an insulin secretory defect with/without insulin resistance). DM of this type previously encompassed noninsulin-dependent diabetes (NIDDM), or adult-onset diabetes. It is a term used for individuals who have relative (rather than absolute) insulin deficiency. People with this type of diabetes (> 80% of patients with DM) frequently are resistant to the action of insulin. Other specific types of DM •Genetic defects of beta-cell function (mutations on chromosome 12 in a hepatic nuclear transcription factor referred to as HNF13. A second form is associated with mutations in the glucokinase gene on chromosome 7p. •Genetic defects in insulin action (e.g. Leprechaunism and Rabson–Mendenhall syndrome are pediatric syndromes that have mutations in the insulin receptor gene with subsequent alterations in insulin receptor function and extreme insulin resistance). •Diseases of the exocrine pancreas (pancreatitis, trauma, cancer) •Endocrinopathies (acromegaly, Cushing’s syndrome, glucagonoma and pheochromocytoma). •Drug- or chemical-induced (pentamidine, glucocorticoids etc.). •Viral infections may cause beta-cell destruction (e.g. mumps, adenovirus, cytomegalovirus, Coxsackie B, congenital rubella). •Other genetic syndromes sometimes associated with DM (Down’s, Klinefelter’s and Turner’s syndromes etc. Gestational diabetes (Includes the former categories of gestational impaired glucose tolerance and gestational DM). >400 000 patients with DM DM – complications: large blood vessel atherosclerosis •coronary heart disease (CHD) •limb ischaemia (diabetic foot!) •stroke small blood vessel atherosclerosis •retinopathy •neuropathy •nephropathy •skin ulceration infection (mycoses etc.) Diabetic retinopathy results in scattered haemorrhages, yellow exudates, and neovascularization Management goals •Normoglycemia - avoiding hypoglycemia or ketosis - HBA1C < 6.5% •Reduce - nephropathy - neuropathy - retinopathy - infections •Control blood pressure •Avoid smoking •Diet – weight control BMI 18.5–24.9 – low fat intake – normal protein intake – carbohydrates ~ 50% of total energy •Motor activity t1/2 5–6 min Insulin is a protein, secreted from the b-cells of the islets of Langerhans in the pancreas in response to a rise in blood glucose, and inhibited by a fall. glucagon cortisol adrenaline somatropin (GH) hyperglycemia insulin hypoglycemia Mechanism of action •Insulin acts via receptors that are transmembrane glycoproteins. •Each receptors has two insulin binding sites. Receptor occupancy results in: 1. Activation of insulin-dependent glucose transport processes in adipose tissue and muscle. 2. Inhibition of adenylyl cyclasedependent processes (lipolysis, proteolysis, glycogenolysis). 4. Intracellular accumulation of potassium and phosphate (which are linked to glucose transport in some tissue). 5. Increased cellular amino acid uptake, DNA and RNA synthesis. 6. Increased oxidative phosphorylation. Insulin (-) AC cAMP PD ATP 3’,5’-AMP (+) Lipolysis in adipose tissue (hypercholesterolemia) Insulin is extracted either from cattle or pig pancreas. Bovine (B) insulin differs from human insulin in three amino acid residues, and porcine (S) insulin in one, but their action is very similar to human. More recently, recombinant DNA technology has allowed in vitro manufacture of insulin with the same structure as human (H) insulin. All current insulin preparations have a low content of impurities. Insulin is initially purified by protein extraction to form a crystalline product. It may then undergo either gel filtration to produce a single peak (SP) insulin or gel filtration and ion exchange chromatography which generates: •monocomponent (MC), •single component (SC) and •rarely immunogenic (RI) insulin. Other abbreviations which use for insulins are: •Hum- and -man (for human ...), •PP (purified preparation) MAIN TYPES INSULIN PREPARATIONS •Short-acting •Intermediate-acting (they contain protamin or Zn) •Long-acting (they contain protamin & Zn) Injectors (with cartridge): OptiPen, OptiSet, Penfill etc ... Comparisons among insulins Type Onset of Peak Duration action activity Shortacting 10–20 min Intermediate-act. 1–2 h Long-act. 2–4 h 1–2 h 5–7 h 5–7 h 8–14 h 13–18 h 18–36 h Insulins use mainly in type 1 DM. Patients with type 2 DM use insulins in the follow cases too: •acute infections •pregnancy •surgical operations •burn •myocardial infarction •ketoacidosis Therapy of DM with insulin is a replacement therapy. 1. Short-acting insulins and analogues a) Insulins: Actrapid, Humulin R b) Analogues: Insulin aspart, Insulin lispro s.c. 15 min before meal 4 times daily chronobiologically (4:3:2:1) c) Per inhalation: Exubera Ketoacidosis Short-acting insulin (i.v. or i.v. infusion) with physiological saline and potassium chloride 2. Intermediate-acting insulins and analogues M •Humulin •Humulin N •Insulatard •Mixtard (s.c. 20 min before meal 2 times daily chronobiologically) 3. Long-acting insulins •Insulin detemir (Levemir) •Insulin glargine (Lantus) (s.c. 20 min before meal once daily) Adverse effects of insulins •hypoglycemia/coma •allergic reactions •insulin resistance •lipodystrophia of subcutaneous fat at or near injection •local fibrosis Oral hypoglycemic drugs •Used in type 2 DM 1. Biguanides metformin: •usually first line drug for type 2 DM •reduces intestinal glucose absorbtion •stimulates anaerobic glycolysis •stimulates glucose uptake •enhances insulin receptor binding Metformin •excreted exclusively by the kidney •does not increase weight and preferable in the obese •GI side effects •rarely lactic acidosis 2. Sulfonylureas I generation: •Chlorpropamide and Tolbutamide (Out...) II generation: •Glibenclamide (Maninil: tab. 5 mg) •Gliclazide (Diaprel : tabl. 80 mg) •Glipizide •Gliquidone Mechanism of action •promote enhanced insulin release from the pancreas •leads to a reduction in hepatic glucose production Unwanted effects •hypoglycemia weight gain •facial flushing following alcohol ingestion Sulfonylureas – important drug interactions: •displacement from protein binding sites – salicylates and sulphonamides •interference with hepatic metabolism – inducers: rifampicin, phenytoin – inhibitors: cimetidine •reduction of renal elimination – allopurinol, salicylates 3. Glucosidase inhibitors Acarbose (Gluco Bay): p.o. Zuccarin: p.o. •Inhibits intestinal alpha-glucosidase •Decreases intestinal absorption of the mono- and polysacharides. •Produces flatulence and diarrhoea. 4. Thiazolidinediones (TZDs) – increase tissue insulin sensitivity Rosiglitazone (Avandia): p.o. 3.5. Incretinomimetics Exenatide (analogue of GLP-1) 3.6. Inhibitors of Dipeptidil peptidase-4 (DPP-4) Sitagliptin Vildagliptin