* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Lecture #22 - Suraj @ LUMS
Survey
Document related concepts
Transcript
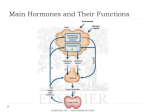
Lecture 22 Homeostasis Two Ways to Regulate • Negative Feedback - O2 and CO2 levels in blood Heart rate Blood pressure Metabolite levels Water and ions pH Body temperature • Positive Feedback - Depolarisation during action potential - Oxytocin Components of Regulatory System • To regulate the internal environment, the following basic process are common to all regulatory systems: • Some imbalance (deficit or excess occurs). • Some detector or detectors which sense deviations from stable levels. • Some central processing system -- hypothalamus. • Effectors capable of remedying the imbalance -involuntary or reflexive. • Complex learned behaviours - aid in maintaining a balance. • Planning external aids to deal with future imbalances. The Liver • Largest gland in the body (weighs about 1500 g). • Two lobes: left and right (lower than left). . • 1/3 of blood flows into the liver from the aorta and 2/3’s enter from the portal vein ( absorbed food material from gut). • Blood exits via left and right hepatic veins into inferior vena cava. • The cells of the liver are known as hepatocytes. Functions of the Liver • Carbohydrate, fat and protein metabolism. • Vitamin/mineral storage. • The liver of the fetus makes red blood cells, eventually taken over by cells in the bone marrow. • Breakdown of heamoglobin. • Bile production – bile acids, bile pigments (bilirubin), cholesterol, bile salts (cholesterol) for lipid breakdown. Blood Glucose Is Controlled Mainly by the Liver • Immediately after meals blood glucose comes from meal • Between meals blood glucose comes from the liver & kidneys • Only the liver and kidneys can release glucose into the blood (requires a special enzyme that converts glucose metabolites to glucose, which can be transported across the cell membrane) • Liver provides 80% of blood glucose supply between meals, the kidney 20% Glucose Synthesis in Liver • Liver makes glucose in 2 ways: - Breaks down liver glycogen (glycogenolysis). - Converts other types of small molecules into glucose (gluconeogenesis). • Many small molecules can be converted to glucose: - Lactate & pyruvate: mainly come from muscles. - Glycerol: supplied by adipose tissue when triglycerides are broken down. - Fatty acids cannot be converted into glucose, but: Fatty acid metabolism indirectly supports gluconeogenesis by producing AcetylCoA. AcetylCoA activates and inhibits key enzymes, promoting glucose formation. - Amino acids can be converted to glucose. Control of Blood Glucose • Respiratory substrate needed continuously by cells. • Normal level 90mg/100 cm3 blood, can be as low as 70mg during fasting or as high as 150mg following a meal. • Six hormones and two negative feedback pathways. Regulation of Blood Glucose Levels Liver-glycogen, cell respiration, insulin rise pancreas fat Muscle-glycogen, cell respiration Other cells-cell respiration Beta cells islets of Langerhans Normal glucose level 90mg/100 cm3 fall Alpha cells Islets of pancreas Langerhans - glucagon Adrenal medulla adrenaline Adrenal glands Pituitary Gland – adrenocorticotropic hormone hypothalamus stimulates adrenal cortex to produce cortisol Thyroid stimulating hormones stimulates thyroid gland to produce thyroxine Liver Glycogen - glucose Protein - glucose Alcohol • Alcohol, or ethyl alcohol (ethanol). • Alcohol is metabolized extremely quickly by the body. Unlike foods, which require time for digestion, alcohol needs no digestion and is quickly absorbed. • Once alcohol reaches the stomach, it begins to break down with the alcohol dehydrogenase enzyme. • This process reduces the amount of alcohol entering the blood by approximately 20%. (Women produce less of this enzyme, which may help to partially explain why women become more intoxicated on less alcohol than men.). • In addition, about 10% of the alcohol is expelled in the breath and urine. Liver and Alcohol • Though alcohol affects every organ of the body, it’s most dramatic impact is upon the liver. • The liver cells prefer fatty acids as fuel, and package excess fatty acids as triglycerides. • When alcohol is present, the liver cells are forced to first metabolize the alcohol, letting the fatty acids accumulate, sometimes in huge amounts. • Alcohol metabolism permanently changes liver cell structure, which impairs the liver’s ability to metabolize fats. • This explains why heavy drinkers tend to develop fatty livers. • The liver is able to metabolize about ½ ounce of ethanol per hour. How the Liver Breaks Down Alcohol • The alcohol dehydrogenase enzyme breaks down alcohol by removing hydrogen in two steps: 1. Alcohol dehydrogenase oxidizes alcohol to acetaldehyde. 2. Acetaldehyde dehydrogenase oxidizes the acetaldehyde to acetyl CoA. These reactions produce hydrogen ions (acid). The B vitamin (coenzyme NAD) picks up these hydrogen ions (becoming NADH). • During alcohol metabolism, NAD becomes unavailable for the many other vital body processes for which it is needed, including glycolysis, the TCA cycle and the electron transport chain. Alcoholism & Liver Disease • Fatty liver is the first stage of liver deterioration in heavy drinkers. • It interferes with the distribution of oxygen and nutrients to the liver’s cells. • If the condition persists long enough, the liver cells will die, forming fibrous scar tissue (the second stage of liver deterioration, or fibrosis). • Some liver cells can regenerate with good nutrition and abstinence. • In the last stage of deterioration, or cirrhosis, the damage to the liver cells is the least reversible. Alcoholic Hepatitis and Cirrhosis • Most common liver disease. • Characterized by hepatomegaly, increase in transaminase levels, and serum bilirubin concentration. • Inflammation due to accumulation of fat and the effect of acetaldehyde on liver cells. • Symptoms may include: abdominal pain, anorexia, vomiting, weakness, diarrhea, weight loss, fever. • Distorted liver structure inhibiting blood flood (portal hypertension) varices and accumulation of fluid in abdominal cavity (ascites), varices may cause acute bleeding in gastrointestinal tract. • Impairment of liver function causing high ammonia levels. • Malnutrition in the Alcoholic - alcohol replaces food thus displacing energy and nutrients. Breakdown of Haemoglobin • Phagocytic cells in liver, spleen and bone marrow breakdown red blood cells. • Heamoglobin released and dissolves in plasma. • Taken up by macrophages where broken down into haem and globin (amino acids). • Iron removed, green pigment biliverdin left. • This is converted into bilirubin, yellow pigmented molecule.