* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Skeletal System
Survey
Document related concepts
Transcript
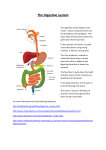
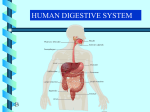
The Digestive System Chapter 22 The Digestive System The digestive system – Takes in food – Breaks it down into nutrient molecules – Absorbs the nutrient molecules into the bloodstream – Rids the body of indigestible remains The Digestive System The organs of the digestive system can be separated into two main groups; those of the alimentary canal and the accessory organs The Digestive System The alimentary canal or gastrointestinal (GI) tract is the continuous muscular digestive tube that winds through the body The Digestive System The organs of the alimentary canal are – Mouth, pharynx, esophagus, stomach, small intestine and large intestine – Food in this canal is technically out of the body The accessory digestive organs are – Teeth, tongue, gallbladder, salivary glands, liver and pancreas – The accessory organs produce saliva, bile and digestive enzymes that contribute to the breakdown of foodstuffs Digestive Processes The digestive tract can be viewed as a process by which food becomes less complex at each step of processing and nutrients become available to the body Ingestion Ingestion is simply the process of taking food into the digestive tract via the mouth Propulsion Propulsion is the process that moves food through the alimentary canal It includes swallowing (voluntary process) and peristalsis (involuntary process) Propulsion Peristalsis involves alternate waves of contraction and relaxation of muscles in the organ walls Its main effect is to squeeze food from one organ to the next Some mixing occurs as well Mechanical Digestion Mechanical digestion physically prepares food for chemical digestion by enzymes Mechanical Digestion Mechanical processes include chewing, mixing of food with saliva by the tongue, churning of food by the stomach, and segmentation Segmentation mixes food with digestive juices and increases the rate of absorption by moving food over the intestinal wall Chemical Digestion Chemical digestion is a series of catabolic steps in which complex food molecules are broken down to their chemical building blocks Chemical Digestion Chemical digestion is accomplished by enzymes secreted by various glands into the lumen of the alimentary canal The enzymatic breakdown of foodstuffs begins in the mouth and is essentially complete in the small intestine Absorption Absorption is the passage of digested end products (plus vitamins, mineral and water) from the lumen of the GI tract into the blood or lymph capillaries located in the wall of the canal Absorption For absorption to occur these substances must first enter the mucosal cells by active or passive transport processes The small intestine is the main absorption site Defecation Defecation is the elimination of indigestible substances from the body as feces Basic Functional Concepts Most organ systems respond to changes in the internal environment either by attempting to restore some plasma variable or by changing their own function The digestive system creates an optimal environment for its functioning in the lumen of the GI tract Essentially all digestive tract regulatory mechanisms act to control luminal conditions so that digestion and absorption can occur there as effectively as possible Basic Functional Concepts Digestive activity is provoked by a range of mechanical and chemical stimuli – Receptors are located in the walls of the tract organs – These receptors respond to several stimuli – The most important being the stretching of the organ by food in the lumen, osmolarity (solute concentration) and pH of the contents and the presence of substrates and end products of digestion Basic Functional Concepts When appropriately stimulated, these receptors initiate reflexes that – Activate or inhibit glands that secrete digestive juices into the lumen or hormones into the blood – Mix lumen contents along the length of the tract by stimulating the smooth muscle of the GI tract walls Basic Functional Concepts Controls of digestive activity are both extrinsic and intrinsic – Another novel trait of the digestive tract is that many of its controlling systems are intrinsic - a product of in-house nerve plexuses or local hormone-producing cells – The walls of the alimentary canal contain nerve plexuses – These plexuses extend essentially the entire length of the GI tract and influence each other both in the same and in different organs Digestive Processes Two kinds of reflex activity occur Short reflexes are mediated entirely by the local enteric plexuses in response to GI tract stimuli Long reflexes are initiated by stimuli arising from within or outside of the GI tract and involve CNS centers and ANS Digestive Processes The stomach and small intestine also contain hormone-producing cells that, when stimulated by chemicals, nerve fibers, or local stretch, release their products to the extracellular space These hormones circulate in the blood and are distributed to their target cells within the same or different tract organs, which they prod into secretory or contractile activity Digestive System Organs Most of the digestive organs reside in the abdominal-pelvic cavity All ventral body cavities contain serous membranes The peritoneum of the abdominal cavity is the most extensive serous membrane of the body Digestive System Organs The visceral peritoneum covers the external surface of most digestive organs and is continuous with the parietal peritoneum that lines the walls of the abdomino-pelvic cavity Between the two layers is the peritoneal cavity, a slitlike potential space containing fluid secreted by the serous membranes Digestive System Organs The serous fluid lubricates the mobile digestive organs, allowing them to glide easily across one another as they carry out their digestive activities Digestive System Organs A mesentery is a double layer of peritoneum - a sheet of two serous membranes fused back to back - that extends to the digestive organ from the body wall Digestive System Organs Mesenteries provide routes for blood vessels, lymphatics and nerves to reach the digestive viscera Digestive System Organs Mesenteries also suspend the visceral organs in place as well as serving as a site for fat storage Digestive Processes Not all alimentary canal organs are suspended with the peritoneal cavity by a mesentery Some parts of the small intestine originate the cavity but then adhere to the dorsal abdominal wall (Figure 22.5) above Digestive Processes Organs that adhere to the dorsal abdominal wall lose their mesentery and lie posterior to the peritoneum These organs, which also include most of the pancreas and parts of the large intestine are called retroperitoneal organs Digestive Processes Digestive organs like the stomach that keep their mesentery and remain in the peritoneal cavity are called interperitoneal or peritoneal organs It is not known why some digestive organs end up in the retroperitoneal position Blood Supply The splanchnic circulation includes those arteries that branch off the abdominal aorta to serve the digestive organs and the hepatic portal circulation The hepatic, splenic and left gastric branches of the celiac trunk serve the spleen, liver, and stomach The mesenteric arteries (superior and inferior) serve the small and large intestine Blood Supply The arterial supply to the abdominal organs is approximately one quarter of the cardiac output The hepatic portal circulation collects nutrient-rich venous blood draining from the digestive viscera and delivers it to the liver The liver collects the absorbed nutrients for metabolic processing or for storage before releasing them back to the bloodstream for general cellular use Histology of the Alimentary Canal From the esophagus to the anal canal, the walls of every organ of the alimentary canal are made up of the same four basic layers or tunics – – – – Mucosa Submucosa Muscularis externa Serosa Each tunic contains a predominant tissue type that plays a specific role in food breakdown Histology of the Alimentary Canal From internal to external the four layers of the alimentary canal are – Mucosa – Submucosa – Muscularis Externa – Serosa Histology: Mucosa The mucosa is the moist epithelial membrane that lines the length of the lumen of the alimentary canal Major functions are – Secretion of mucus, digestive enzymes and hormones – Absorption – Protection Histology: Mucosa The mucosa is the moist epithelial membrane that lines the length of the lumen of the alimentary canal Major functions are – Secretion of mucus, digestive enzymes and hormones – Absorption – Protection Histology: Mucosa More complex than most other mucosae the typical digestive mucosa consists of three sublayers – A surface epithelium – A lamina propria – A deep muscularis mucosae Histology: Mucosa The epithelium of the mucosa is a simple columnar epithelium that is rich in mucus secreting goblet cells Histology: Mucosa The slippery mucus it produces protects certain digestive organs from digesting themselves by enzymes working within their cavities and eases food passage In the stomach and small intestine the mucosa contain both enzyme-secreting and hormone-secreting cells Thus, in such sites, the mucosa is a diffuse kind of endocrine organ as well as part of the digestive organ Histology: Mucosa The lamina propria which underlies the epithelium is loose areolar connective Note lymph nodule Histology: Mucosa Its capillaries nourish the epithelium and absorb digested nutrients Its isolated lymph nodules are part of the mucosa associated lymphatic tissue (MALT) which collectively act as a defense against bacteria and other pathogens Large collections of lymph nodules occur at strategic locations such as within the pharynx (tonsils) and appendix Histology: Mucosa The muscularis mucosae is a scant layer of smooth muscle cells that produces local movements of the mucosa Histology: Mucosa The twitching of this muscle layer dislodges food particles that have adhered to the mucosa In the small intestine, it throws the mucosa into a series of small folds that immensely increase its surface area Histology: Submucosa The submocosa is a moderately dense connective tissue containing blood and lymphatic vessels, lymph nodules, and nerve fibers Its rich supply of elastic fibers enables the stomach to regain its normal shape after storing a large meal Histology: Submucosa The submocosa is a moderately dense connective tissue containing blood and lymphatic vessels, lymph nodules, and nerve fibers Its rich supply of elastic fibers enables the stomach to regain its normal shape after storing a large meal Histology: Muscularis Externa The muscularis externa is responsible for segmentation and peristalsis It mixes and propels foodstuffs along the digestive tract This thick muscular layer has an inner circular and an outer longitudinal layer Histology: Muscularis Externa In several places along the GI tract, the circular layer thickens to form sphincters Sphincters act as valves to prevent backflow and control food passage from one organ to the next Histology: Serosa The serosa is the protective outermost layer of interperitoneal organ This visceral peritoneum is formed of areolar connective tissue covered with mesothelium, a single layer of squamous epithelial cells Histology: Serosa In the esophagus, which is located in the thoracic instead of the abdominopelvic cavity, the serosa is replaced by an adventitia The adventitia is an ordinary fibrous connective tissue that binds the esophagus to surrounding structures Retroperitoneal organs have both a serosa (on the side facing the peritoneal cavity) and an adventitia (on the side abutting the dorsal body wall) Enteric Nervous System The alimentary canal has its own inhouse nerve supply Enteric neurons communicate widely with each other to regulate digestive system activity Intrinsic Nerve Plexes Enteric Nervous System These enteric neurons constitute the bulk of the two major intrinsic nerve plexuses found within the walls of the alimentary canal – Submucosal nerve plexus – Myenteric nerve plexus Myenteric plexus Submucosal plexus Enteric Nervous System A smaller third plexus is found within the serosa layer – Subsersora nerve plexus Subserosa nerve plexus Enteric Nervous System The submucosal nerve plexus chiefly regulates the activity of glands and smooth muscle in the mucosa tunic The myenteric nerve plexus lies between the circular and longitudinal layers of smooth muscle of the muscularis externa Myenteric plexus Submucosal plexus Enteric Nervous System Via their communication with each other, with smooth muscle layers, and with submucosal plexus, the enteric neurons of the myenteric plexus provide the major nerve supply to the GI tract This plexus controls GI tract mobility by controlling the patterns of segmentation and peristalsis Control comes from local reflex arcs between enteric neurons in the same or different plexus or organs Enteric Nervous System The enteric nervous system is also linked to the CNS by afferent visceral fibers and sympathetic and parasympathetic branches of the ANS Digestive activity is subject to extrinsic control exerted by ANS which can speed up or slow secretory activity and mobility Digestive System Mouth, Pharynx, and Esophagus The mouth is the only part of the digestive system that is involved in the ingestion of food Most digestive function of the mouth reflect the activity of accessory organs chewing the food and mixing it with salvia to begin the process of chemical digestion The mouth also begin the propulsive process by which food is carried through the pharynx and esophagus to the stomach The Mouth The oral cavity is a lined with mucosa It bounded by the lips anteriorly, and the tongue inferiorly and the cheeks laterally Its anterior opening is the oral orifice Posteriorly the oral cavity is continuous with the oropharynx The Mouth The walls of the mouth are lined with stratified squamous epithelium The epithelium is highly ketatinized for extra protection against abrasion during eating The mucosa also produces defensins to fight microbes in the mouth The Lips and Cheeks The labia and the cheeks have a core of skeletal muscle covered by skin The orbicularis oris muscle forms the bulk of the lips The cheeks are formed largely by the buccinators The area between the teeth and gums is the vestibule The Lips and Cheeks The lips extend from the inferior margin of the nose to the superior boundary of the chin The reddened area is called red margin The labial frenulum is a median fold that joins the internal aspect of each lip to the gum The Palate The palate which forms the roof of the mouth has two distinct parts – Hard palate – Soft palate The Palate The hard palate is underlain by bone and is a rigid surface against which the tongue forces food during chewing There exists a centerline ridge called a raphe The mucosa is corrugated for friction The Palate The soft palate is a mobile fold formed by skeletal muscle Projecting down from its free edge is the uvula The soft palate rises reflexively to close off the nasopharynx when swallowing The Palate The soft palate is anchored to the tongue by the palantoglossal arches and to the wall of oropharynx by the palantopharyngeal arches These arches form the boundary of the facuces The Tongue The tongue occupies the floor of the mouth and fills most of the oral cavity when closed The tongue is composed of interlacing masses of skeletal muscle fibers The tongue grips the food and constantly repositions it between the teeth The tongue also mixes the food with salvia and form it into a mass called a bolus and then initiates swallowing by moving the mass into the pharynx The Tongue The tongue has both intrinsic and extrinsic skeletal muscles The intrinsic muscles are confined within the tongue and are not attached bone The fibers allow the tongue to change its shape for speech and swallowing but not its position The Tongue The extrinsic muscles extend the tongue from their points of origin The extrinsic muscles allow the tongue to be protruded, retracted and moved side to side The tongue is divided by a median septum of connective tissue The Tongue A fold of mucosa called the lingual frenulum secures the tongue to the floor of the mouth This frenulum limits the posterior movement of the tongue You cannot swallow your tongue The Tongue The conical filaform papillae give the tongue surface a roughness that aids in manipulating foods in the mouth They align in parallel rows on the dorsum They contain keratin which stiffens them House taste buds The Tongue The mushroom shaped fungiform palillae are scattered over the surface Each has a vascular core that gives it a reddish hue Houses taste buds The Tongue The circumvallate are located in a Vshaped row at the back of the tongue Appear similar to the fungiform papillae but with an additional surrounding furrow The Salivary Glands A number of glands both inside and outside the oral cavity produce and secrete saliva Saliva functions to – Cleanses the mouth – Dissolves food chemical so that they can be tasted – Moistens food and aids in compacting it into a bolus – Contains enzymes that begin the chemical breakdown of starches The Salivary Glands Most saliva is produced by three pairs of extrinsic salivary glands – Parotid – Submandibular – Sublingual These glands lie outside the oral cavity and empty their secretions into it The Salivary Glands The intrinsic salivary glands are small and are scattered throughout the oral cavity The Salivary Glands The salivary glands are composed of two types of secretory cells; mucus and serous The serous cells produce a watery secretion containing enzymes and the ions of saliva The mucus cells produce mucus a stringy viscous solution The Teeth The teeth lie in sockets in the gum covered margins of the mandible and maxilla Teeth function to tear and grind food and begin the mechanical process of digestion Dentition Ordinarily we have two sets of teeth the primary and permanent dentitions The primary dentition consists of deciduous teeth The first teeth appear at six months and additional teeth continue to erupt until about 24 months when all 20 teeth have emerged Dentition As the deeper permanent teeth enlarge and develop, the root of the milk teeth are resorbed from below causing them to loosen and fall out between the ages of 6 and 12 years Generally, all the teeth of the permanent dentition have erupted by adolescence The Teeth Teeth are classified according to their shape and function – – – – Incisors / cutting Canines / tear Premolars / grind Molars / crush There are 20 milk teeth and 32 permanent teeth Tooth Structure Each tooth has two major regions; the crown and the root The crown represents the visible portion of the tooth exposed above the gum The root is the portion of the tooth that is imbedded in the jawbone The Pharynx From the mouth, the food passes posteriorly into the oropharnyx The mucosa consists of stratified squamous epithelium The epithelium is supplied with mucus producing glands for lubrication The Pharynx The external muscle layer consists of two skeletal muscle layers The cells of the inner layer run longitudinally The outer layer of muscles pharyngeal constrictor muscles, encircle the wall Sequential contractions propel food into esophagus The Esophagus The esophagus takes a fairly straight course through the mediastinum of the thorax, pierces the diaphragm at the esophageal hiatus to enter the abdomen The Esophagus The esophagus joins the stomach at the cardiac orifice The cardica orifice is surrounded by the cardiac esophogeal sphincter The Pharynx The esophageal mucosa contains a nonketatinized stratified squamous epithelium which changes abruptly simple columnar epithelium upon reaching the stomach When empty the esophagus is empty with its mucosa drawn into folds which flatten out when food is in passage The mucosa contains mucus secreting esophageal glands which are compressed by a passing bolus of food resulting in the glands secreting a lubricant The Pharynx The muscularis externa changes from skeletal muscle to a mix of skeletal and smooth to finally all smooth as it approaches the stomach Instead of a serosa, the esophagus has a fibrous adventitia composed entirely of connective tissue, which blends with surrounding structures along its route Digestive Processes The mouth and its accessory digestive organs are involved in most digestive processes – – – – The mouth ingests food Begins mechanical digestion by chewing Initiates propulsion by swallowing Starts the process of chemical digestion – The pharynx and the esophagus serve as conduits to pass food from the mouth to the stomach Digestive Processes: Mastication Mastication is the mechanical process of breaking down food The cheeks and closed lips hold the food between the teeth The tongue mixes the food with saliva to soften it The teeth cut and grind food into smaller pieces Digestive Processes: Deglutition In deglutition, food is first compacted by the tongue into a bolus and swallowed Swallowing is a process that requires the coordination of tongue soft palate, pharynx, esophagus and 22 separate muscles Digestive Processes: Deglutition In deglutition, food is first compacted by the tongue into a bolus and swallowed Swallowing is a process that requires the coordination of tongue soft palate, pharynx, esophagus and 22 separate muscles Digestive Processes: Deglutition Food passage into respiratory passageways by rising of the uvula and larynx Relaxation of the upper esophageal sphincter allows food entry into the esophagus Digestive Processes: Deglutition The constrictor muscles of the pharynx contract, forcing food into the esophagus inferiorly The upper esophageal sphincter contracts after entry Digestive Processes: Deglutition Food is conducted along the length of the esophagus to the stomach by peristaltic waves Digestive Processes The gastroesophageal sphincter enters opens and food enters the stomach The Stomach The stomach functions as a temporary storage tank where the chemical breakdown of protein begins and food is converted to a creamy paste called chyme The stomach lies in the upper left quadrant of the abdominal cavity Though relatively fixed at both ends, it is free to move in between The Stomach: Gross Anatomy The stomach varies from 6 to 10 inches in length, but its diameter and volume depend on how much food it contains Empty it may contain on 50 ml but can expand to hold about 4 liters of food The Stomach: Gross Anatomy When empty, the stomach collapses inward, throwing its mucosa into large, longitudinal folds called rugae The Stomach: Gross Anatomy The major region of the stomach are the cardia region, the fundus, body, pyloric region, and the greater and lesser curvatures The Stomach: Gross Anatomy The lesser omentum runs from the liver to the lesser curvature where it becomes continuous with the visceral peritoneum of the stomach The Stomach: Gross Anatomy The greater omentum drapes inferior from the greater curvature of the stomach to cover the coils of the small intestine Stomach: Microscopic Anatomy The stomach wall exhibits the four tunics of most of the alimentary canal but its muscularis and mucosa are modified for the special roles of stomach The muscularis externa has an extra oblique layer of muscle that enables it to mix, churn and pummel food The epithelium lining the stomach mucosa is simple columnar epithelium composed entirely of goblet cells, which produce a protective coating of mucus Microscopic Anatomy The four tunics typical of the alimentary canal – – – – Mucosa Submucosa Muscularis Externia Serosa Microscopic Anatomy The otherwise smooth lining is dotted with millions of gastric pits which lead to gastric glands that produce gastric juice The glands of the stomach body are substantially larger and produce the majority of the stomach secretions Microscopic Anatomy Mucus neck cells produce a different type of mucus from that secreted by the mucus secreting cells of the surface epithelium The special function of this unique mucus is not yet understood Microscopic Anatomy Parietal cells scattered among the chief cells secrete hydrochloric acid (HCl) and intrinsic factor The parietal cells have a large surface area adapted for secreting HCl in the stomach Intrinsic factor is required for absorption of B12 in the small intestine Microscopic Anatomy Chief cells produce pepsinogen, the inactive form of the proteindigesting enzyme pepsin The cells occur mainly in the basal regions of the gastric glands Pepsinogen is activated by HCl Microscopic Anatomy Parietal cells scattered among the chief cells secrete hydrochloric acid (HCL) and intrinsic factor The parietal cells have a large surface area adapted for secreting HCL in the stomach Intrinsic factor is required for absorption of B12 in the small intestine Microscopic Anatomy Enteroendocrine release a variety of hormones directly into the lamina propria These products diffuse into capillaries and ultimately influence several digestive system target organs which regulate stomach secretion and mobility Mucosal Barrier Gastric juice is 100,000 more concentrated than that found in the blood Under such harsh conditions the stomach must protect itself from self digestion with a mucosal barrier – – – – Bicarbonate rich mucus is on the stomach wall Epithelial cells are joined by tight junctions Glandular cells are impermeable to HCl Surface epithelium is replace every 3 to 6 days Digestive Processes: Stomach The stomach is involved in the whole range of digestive activities – It serves as a holding area for ingested food – Breaks down food further chemically and mechanically – It delivers chyme to the small intestine at a controlled rate Digestive Processes: Stomach Protein digestion is initiated in the stomach and is essentially the only type of enyzmatic digestion that occurs there The most important protein digesting enzyme produced by the gastric mucosa is pepsin In children, the stomach glands also secrete rennin, an enzyme that acts on milk protein converting it to a curdy substance appearing like sour milk Digestive Processes: Stomach Despite its many functions in the digestive system the only one that is essential for life is secretion of intrinsic factor Intrinsic factor is required for intestinal absorption of vitamin B12, needed to produce mature erythrocytes Without B12 the individual will develop prenicious anemia unless administered by injection Regulation of Gastric Secretion Gastric secretion is controlled by both neural and hormonal mechanisms Under normal conditions the gastric mucosa creates as much as 3 liters of gastric juice every day Gastric juice is an acid solution that has the potential to dissolve nails Regulation of Gastric Secretion Nervous control is regulated by long (vagus nerve mediated) and short (local enteric) nerve reflexes When the vagus nerves actively stimulate the stomach, secretory activity of virtually all of its glands increase The sympathetic nerves depress secretory activity Regulation of Gastric Secretion Hormonal control of gastric secretion is largely from the presence of gastrin Gastrin stimulates the secretion of both enzymes and HCL in the stomach Hormones produced by the small intestine are largely gastrin antagonists Regulation of Gastric Secretion Stimuli acting at three distinct sites, the head, stomach, and small intestine, provoke or inhibit gastric secretory activity Accordingly the three phases are called cephalic, gastric, and intestinal phases However, the effector site is the stomach in all cases and once initiated, one or all threephases may be occurring at the same time Phase 1: Cephalic reflex The cephalic reflex phase of gastric secretion occurs before food enters the stomach It is triggered by the aroma, taste, sight, or though of food During this phase the brain gets the stomach ready for food Phase 1: Cephalic reflex Inputs from activated olfactory receptors and taste buds are relayed to the hypothalamus which in turn stimulates the vagal nuclei of the medulla oblongata, causing motor impulses to be transmitted via the vagus nerves to the parasympathetic nerve ganglia Eneteric ganglionic neurons in turn stimulate the stomach glands Phase 1: Cephalic reflex The enhanced secretory activity that results when we see or think of food is a conditioned reflex and occurs only when we like or want the food If we are depressed or have no appetite, this part of the cephalic reflex is suppressed Phase 2: Gastric reflex Once food reaches the stomach, local neural and hormonal mechanisms initiate the gastric phase This phase provides about two-thirds of the gastric juice released The most important stimuli are distension, peptids, and low acidity Phase 2: Gastric reflex Stomach distension activates stretch receptors and initiates both local (myentertic) reflexes and the long vagovagal reflexes In vagovagal reflex, impulses travel to the medulla and then back to the stomach via vagal fibers Both types of reflexes lead to acetylcholine (ACH) release, which in turn stimulates the output of more gastric juice by cells Phase 2: Gastric reflex Though neural influences initiated by stomach distension are important, the hormone gastrin probably plays a greater role in stimulating stomach gland secretion during the gastric phase Chemical stimuli provided by partially digested proteins (peptids)caffine (colas, coffee) and rising pH directly active gastrin secreting entoendocrine cells called G cells Phase 2: Gastric reflex Although gastrin also stimulates the release of enzymes, its main target is the HCL secreting parietal cells, which it prods to spew out even more HCL Highly acidic (pH below 2) gastric contents inhibit gastrin secretion Phase 2: Gastric reflex When protein foods are in the stomach, the pH of the gastric contents generally rises because proteins act as buffers to tie up H+ The rise in pH stimulates gastrin and subsequently HCL release, which in turn provides the acidic conditions needed for protein digestion Phase 2: Gastric reflex The more protein in the meal, the greater the amount of gastrin and HCL released As proteins are digested, the gastric contents gradually become more acidic, which again inhibits the gastrin secreting cells This negative feedback mechanism helps maintain optimal pH and working conditions for the gastric enzymes Phase 2: Gastric reflex G cells are also activated by the neural reflexes already described Emotional upsets, fear, anxiety, or anything that triggers the fight-or-flight response inhibits gastric secretion because (during such times) the sympathetic division overrides parasympathetic controls of digestion Phase 2: Gastric reflex The control of the HCL secreting parietal cells is unique and multifaceted Basically, HCL secretion is stimulated by three chemicals, all of which work through second-messenger systems Ach released by parasympathetic nerve fibers and gastrin secreted by G cells Phase 2: Gastric reflex Ach released by parasympathetic nerve fibers and gastrin secreted by G cells bring about their effects by increasing intercellular Ca++ levels Phase 2: Gastric reflex Histamine released by mucosal cells called histaminocytes acts through cyclic AMP (cAMP) Phase 2: Gastric reflex When only one of the three chemicals binds to the parietal cells, HCL secretions are minimul When all three of the chemicals bind to the parietal cells volumes of HCL pour forth as if pushed out under pressure Phase 2: Gastric reflex The process of HCL formation within the parietal cells is complicated and poorly understood The consensus is that H+ is actively pumped into the stomach lumen against a tremendous concentration gradient Phase 2: Gastric reflex As hydrogen ions are secreted, chloride ions (Cl-) are also pumped into the lumen to maintain an electrical balance in the stomach The Cl- is obtained from blood plasma, while the H+ appears to come from a breakdown of carbonic acid formed by the combination of carbon dioxide and water and within the parietal cells Phase 2: Gastric reflex CO2 + H2O H2CO3 H+ + HCO3As H+ is pumped from the cell and HCO3- is ejected through the basal cell membrane into the capillary blood Phase 2: Gastric reflex The result of ejection of the bicarbonate ion into the capillary blood is that blood draining from the stomach is more alkaline than the blood serving it The phenomenon is called the alkaline tide Phase 3: Intestinal The intestinal phase of gastric secretion has two components – One excitatory – One inhibitory Phase 3: Intestinal The excitatory aspect is set into motion as partially digested food begins to fill the initial part (duodenum) of the small intestine This stimulates intestinal mucosal cells to release a hormone that encourages the gastric glands to continue their secretory activity Phase 3: Intestinal The effects of this hormone imitate those of gastrin, so it has been named intestinal (enteric) gastrin However, intestinal mechanisms stimulate gastrin secretion only briefly As the intestine distends with chyme containing large amounts of H+, fats, partially digested proteins, and irritating substances, the inhibitatory component is triggered in the form of the enterogastric reflex Phase 3: Intestinal The enterogastric reflex is actually a trio of reflexes that – Inhibit the vagal nuclei in the medulla – Inhibit local reflexes – Activate sympathetic fibers that cause the pyloric sphincter to tighten and prevent further food entry into the small intestine As a result, gastric secretory activity declines Phase 3: Intestinal These inhibitions on gastric activity product the small intestine to harm due to excessive acidity and match the small intestine’s processing abilities to the amount of chyme entering it at a given time Phase 3: Intestinal In addition, the factors just named trigger the release of several intestinal hormones collectively called enterogastrones which include – – – – Secretin Cholecystokinin (CCK) Vasoactive intestinal peptide (VIP) Gastric inhibitory peptide (GIP) All of these hormones inhibit gastric secretion when the stomach is very active Gastric Motility and Emptying Stomach contractions, accomplished by the tri-layered muscularis, not only cause its emptying but also compress, knead, twist, and continually mix the food with gastric juice to produce chyme Because the mixing movements are accomplished by a unique type of peristalis (bidirectional) the process of mechanical digestion and propulsion are inseparable in the stomach Gastric Motility: Stomach Filling Although the stomach stretches to accommodate incoming food, internal stomach pressure remains constant until about 1 liter of food has been ingested The relatively unchanging pressure in the filling stomach is due to 1) reflex mediated relaxation of the stomach muscle and 2) plasticity of visceral smooth muscle Gastric Motility: Stomach Filling Reflexive relaxation of stomach muscle in the fundus and body occurs both in anticipation of and in response to food entry into the stomach As food travels through the esophagus, the stomach muscles relax This receptive relaxation is coordinated by the swallowing center in the brain stem and mediated by the vagus nerves Gastric Motility:Stomach Filling The stomach also actively dilates in response to gastric filling, which activates stretch receptors in the wall The phenomenon called adaptive relaxation appears to depend on local reflexes involving nitric oxide (NO) releasing hormones Gastric Motility: Stomach Filling Plasticity is the intrinsic ability of visceral smooth muscle to exhibit the stressrelaxation response, that is, to be stretched without greatly increasing its tension and contractile strength Gastric Motility and Emptying After a meal peristalsis begins near the cardiac sphincter, where it produces only gentle rippling movements of the stomach wall Gastric Motility and Emptying As contractions approach the pylorus, where the stomach musculature is thicker, the contractions become more powerful Gastric Motility and Emptying Consequently, the contents of the fundus remain relatively undisturbed, while the foodstuffs close to the pylorus receive a very active mixing Gastric Motility and Emptying The pyloric region of the stomach, which holds about 30 ml of chyme, acts as a “dynamic filter” that allows only liquids and small particles of food to pass Gastric Motility and Emptying Normally, each peristaltic wave reaching the pyloric muscle squirts 3 ml or less of chyme into the small intestine Gastric Motility and Emptying While the stomach delivers small amounts of chyme into the doudenum it also simultaneously forces most of the contained material backward into the stomach for further mixing Gastric Motility and Emptying Although the intensity of the stomach’s peristaltic waves can be modified, the rate is always constant at around 3 per minute The contractile rhythm is set by the spontaneous activity of pacemaker cells located at the margins of the longitudinal smooth muscle layer Gastric Motility and Emptying The pacemaker cells, are believed to be muscle-like noncontractile cells called interstitial cells of Cajal which depolarize the repolarize spontaneously three times each minute This depolarization and repolarization establish the so-called cyclic slow waves of the stomach or its basic electrical rhythm (BER) Gastric Motility and Emptying Since the pacemakers are electrically coupled to the rest of the smooth muscle sheet by gap junctions, their “beat” is transmitted efficiently and quickly to the entire muscularis The pacemakers set the maximum rate of contraction, but they do not initiate the contractions or regulate their force They generate subthreshold depolarization waves, which are then enhance by neural and hormonal factors Gastric Motility and Emptying Factors that increase the strength of stomach contractions are the same factors that enhance gastric secetory activity Distension of the stomach wall by food activates stretch receptors and gastric secreting cells, which both ultimately gastric smooth muscle and so increase gastric motility Gastric Motility and Emptying Thus, the more food there is in the stomach, the more vigorous the stomach mixing and emptying movements will be evident The stomach usually empties completely within four hours after a meal However, the larger the meal (greater distension) and the more liquid the meal, the faster the stomach empties Gastric Motility and Emptying Fluids pass quickly through the stomach Solids linger, remaining until they are well mixed with gastric juice and converted to a liquid state Gastric Motility and Emptying The rate of emptying depends as much on the contents of the duodenum as on whats happening in the stomach The stomach and duodenum act in tandem As chyme enters the duodenum, receptors in its wall respond to chemical signals and to stretch, initiating the enterogastric reflex and hormonal mechanisms described earlier These factors inhibit gastric secretory activity and prevent further duodenal filling by reducing the force of pyloric contractions Gastric Motility and Emptying A carbohydrate-rich meal moves through the duodenum rapidly, but fats form an oily layer at the top of the chyme and are digested more slowly by enzymes acting in the intestines Thus, when chyme entering the duodenum is fatty, food may remain in the stomach six hours or more The Small Intestine and Associated Structures In the small intestine, usable food is finally prepared for its journey into the cells of the body However, this vital function cannot be accomplished without the aid of secretions from the liver (bile) and pancreas (digestive enzymes) Thus the accessory organ are discussed in this section Small Intestine The small intestine is a convoluted tube extending from the pyloric sphincter in the epigastric region to the iliocecal valve where it joins the large intestine Small Intestine It is the longest part of the alimentary tube, but its diameter is only about 2.5 cm In the cadaver, the small intestine is 6 - 7 meters long because of loss of muscle tone, while it is only 2 - 4 meters long in the living individual The small intestine has three subdivisions – Duodenum – Jejunum – Ileum Gross Anatomy The relatively immovable duodenum which curves about the head of the pancreas Small Intestine The duodenum is about 10 inches long Although it is the shortest subdivision, the duodenum has the most features of interest – – – – The bile duct Main pancreatic duct Hepatopancreatic ampulla Major duodenal papilla Gross Anatomy The bile duct, delivering bile from the liver The main pancreatic duct, carries pancreatic juice from the pancreas Gross Anatomy The hepatopancreatic ampulla is where these two ducts unite in the wall of the duodenum The papilla is where this sphincter enters the duodenum Small Intestine The jejunum is about 8 ft long and extends from the duodenum to the ileum This central section twists back and forth within the abdominal cavity Small Intestine The ileum is approximately 12 ft. in length It joins the large intestine at the ileocecal valve Small Intestine The jejunum and ileum hang in coils in the central and lower part of the abdominal cavity Small Intestine The jejunum and ileum are suspended from the posterior abdominal wall by the fan shaped mesentery Small Intestine Nerve fibers serving the small intestine include the parasympathetics from the vagus nerves and sympathetics from the long splanchic nerves These are relayed through the superior mesenteric and celiac plexus Small Intestine The arterial supply is primarily from the superior and mesenteric artery The veins run parallel to the arteries and typically drain into the superior mesenteric vein From the mesenteric vein, the nutrient rich venous blood from the small intestine drains into the hepatic portal vein which carries it to the liver Microscopic Anatomy The small intestine is highly adapted for nutrient absorption Its length provides a huge surface area for absorption There are three structural modifications which increase the surface area for absorption – Plicae circulares – Villi – Microvilli Microscopic Anatomy Digestive System Organs In this view you can see the plicae circulares and the villi of the small intestine Microscopic Anatomy Structural modifications increase the intestinal surface area tremendously It is estimated that the surface area of the small intestine is equal to 200 square meters or roughly equivalent to the floor space of a two story house Most absorption occurs in the proximal part of the small intestine, with these structural modifications decreasing toward the distal end Microscopic Anatomy The circular folds or plicae circularis are deep permanent folds of the mucosa and submucosa These folds are nearly 1 cm tall Microscopic Anatomy The folds force chyme to spiral through the lumen, slowing its movement and allowing time for full nutrient absorption Microscopic Anatomy Villi are finger like projections of the mucosa Over 1 mm tall they give a velvety texture to the mucosa Microscopic Anatomy The epithelial cells of the villi are chiefly absorptive columnar cells called enterocytes Microscopic Anatomy In each villus is a capillary bed and a wide lymphatic capillary called a lacteal Digested food is absorbed through the epithelial cells into both the capillary blood and the lacteal Villi become gradually narrower and shorter along the length of the sm. intestine Enterocyte Microscopic Anatomy Microvilli are tiny projections of the plasma membrane of the absorptive cells of the mucosa It gives the mucosal surface a fuzzy appearance sometimes called a brush border Microscopic Anatomy Beside increasing the absorptive surface, the plasma membrane of the microvilli bear enzymes referred to as the brush border enzymes These enzymes complete the final stages of digestion of carbohydrates and proteins in the small intestine Histology of the Wall The four tunics of the digestive tract are modified in the small intestine by variations in mucosa and submucosa Histology of the Wall The epithelium of the mucosa is largely simple columnar epithelium serving as absorptive cells The cells are bound by tight junctions and richly endowed with microvilli Also present are many mucus-secreting goblet cells Histology of the Wall Scattered among the epithelial cells of the wall are T cells called intraepithelial lymphocytes These T cells provide an immunological component Finally, there scattered enteroendocrine cells which are the source of secretin and cholecystokinin Histology of the Wall Between villi the mucosa is studded with pits that lead into tubular intestinal glands called intestinal crypts or crypts of Lieberkuhn Histology of the Wall The epithelial cells that line these crypts secrete intestinal juice Intestinal juice is a watery mixture containing mucus that serves as a carrier fluid for absorption of nutrients from chyme Histology of the Wall Located deep on the crypts are specialized secretory cells called Paneth cells Paneth cells fortify the small intestine by releasing lysozyme an antibacterial enzyme The number of crypts decreases along the length of the wall of the small intestine, but the number of goblet cells becomes more abundant Histology of the Wall The various epithelial cells arise from rapidly dividing stem cells at the base of the crypts The daughter cells gradually migrate up the villi where they are shed from the villis tips In this way the villus of the epithelium is renewed every three to six days Histology of the Wall The rapid replacement of the intestinal (and gastric) epithelial cells has clinical as well as physiological implications Treatments for cancer, such as radiation therapy and chemotherapy preferentially target the cells in the body that divide most quickly This kills cancer cells, but it also nearly obliterates the GI epithelium causing nausea, vomiting, and diarrhea after each treatment Histology of the Wall The submucosa is typical areolar connective tissue, and it contains both individual and aggregated lymphoid follicles (Peyer’s patches) Peyer’s patches increase in abundance toward the end of the small intestine, reflecting the fact that the large intestine contains huge numbers of bacteria that must be prevented from entering the bloodstream Histology of the Wall A set of elaborated mucus-secreting duodenal glands (Brunner’s) is found in the submucosa of the duodenum only Histology of the Wall These glands produce an alkaline (bicarbonate-rich) mucus that helps neutralize the acidic chyme moving in from the stomach When this protective mucus barrier is inadequate, the intestinal wall is eroded and duodenal ulcers results Histology of the Wall The muscularis is typical and bilayered Except for the bulk of the duodenum, which is retroperitoneal and has an adventitia, the external intestinal surface is covered by visceral peritoneum (serosa) Intestinal Juice The intestinal glands normally secrete between 1 and 2 liters of intestional juice daily The major stimulus for its production is distension or irritation of the intestinal mucosa by hypertonic or acidic chyme Intestinal Juice Normally, the pH range of intestinal juice is slightly alkaline (7.4-7.8), and it is isotonic with blood plasma Intestinal juice is largely water but it also contains some mucus, which is secreted both by the duodenal glands and by goblet cells of the mucosa Intestinal juice is relatively enzyme poor because intestinal enzymes are largely limited to the bound enzymes of the brush border The Liver and Gallbladder The liver and gallbladder are accessory organs associated with the small intestine The liver has many metabolic and regulatory roles Its digestive function is to produce bile for export to the duodenum Bile is a fat emulsifier which breaks up fat into tiny particles so that they are more accessible to digestive enzymes The gallbladder is a storage site for bile The Liver The ruddy, blood rich liver is the largest gland in the body weighing about 1.4 kg in the average adult The Liver Shaped like a wedge, it occupies most of the right hypochondriac and epigastric regions extending farther to the right of the body midline than the left The Liver Located under the diaphragm, the liver lies almost entirely within the rib cage The location of the liver within the rib cage offers this organ some degree of protection The Liver The liver has four primary lobes; right, left, caudate and quadrate The Liver A mesentery, the falciform ligament, separates the right and left lobes anteriorly and suspends the liver from the diaphragm The Liver Running along the free inferior edge of the falciform ligament is the ligamentum teres a remnant of the fetal umbilical vein The Liver Except for the superiormost liver area, which is fused to the diaphragm, the entire liver is enclosed by a serosa (visceral peritoneum) The Liver A dorsal mesentery, the lesser omentum, anchors the liver to the lesser curvature of the stomach The Liver The hepatic artery and hepatic portal vein, enter the liver at the porta hepatis The Liver The common bile duct, which runs inferiorly from the liver, travels through the lesser omentum The Liver The gallbladder rests in a recess of the inferior surface of the right lobe of the liver The Liver Bile leaves the liver through several bile ducts that ultimately fuse to form the large common hepatic duct which travels to the duodenum The Liver The common hepatic duct and the cystic duct fuse to form the bile duct Microscopic Anatomy of Liver The liver is composed of seed sized structural & functional units called liver lobules Each lobule is roughly hexagonal Microscopic Anatomy of Liver Hepatocytes or live cells are organized to radiate out from a central vein running the length of the longitudinal axis of the lobule Microscopic Anatomy of Liver To make a rough “model” of a liver lobule, open a paperback book until the two covers meet The pages represent the plates of hepatocytes and the hollow cylinder formed by the rolled spine represents the central vein Microscopic Anatomy of Liver The liver’s main function is to filter and process the nutrient rich blood delivered to it At each of the six corners of a lobule is a portal triad so named because three basic structures are always present there: – A branch of the hepatic artery – A branch of the hepatic portal vein – A bile duct Microscopic Anatomy of Liver The hepatic artery supplies oxygen rich arterial blood to the liver Microscopic Anatomy of Liver The hepatic vein carries blood laden with nutrients from the digestive viscera Microscopic Anatomy of Liver A bile duct to carry secreted bile toward the common bile duct and ultimately to the duodenum Microscopic Anatomy of Liver Between the hepatocyte plates are enlarged, very leaky capillaries, the liver sinusoids Microscopic Anatomy of Liver Blood from both the hepatic portal vein and the hepatic artery percolates from the triad regions through these sinusoids and empties into the central vein Microscopic Anatomy of Liver From the central vein blood eventually enters the hepatic veins, which drain the liver, and empty into the inferior vena cava Microscopic Anatomy of Liver Inside the sinusoids are star shaped hepatic macrophages, also called Kupffer cells, which remove debris such as bacteria and worn-out blood cells Microscopic Anatomy of Liver The hepatocytes (liver cells) are virtual organelle storehouses with large amounts of both rough and smooth endoplasmic reticulum, Golgi apparatuses, peroxisomes, and mitochondria Thus equipped, the hepatocytes produce not only bile but also – Process blood borne nutrients – Store Fat-soluble vitamins – Detoxify the blood Microscopic Anatomy of Liver In processing nutrients the hepatocytes store glycogen and make plasma proteins Fat soluble vitamins are stored until such time as they are needed for metabolism Detoxification occurs are the hepatocytes rid the blood of ammonia by converting it to urea The net result is that the blood leaving the liver contains fewer nutrients and waste materials than the blood that entered Microscopic Anatomy of Liver Secreted bile flows through tiny canals, called bile canaliculi that run between adjacent hepato cytes toward the bile branch ducts in the portal triad Microscopic Anatomy of Liver Note that the bile and the blood flow in opposite directions in the liver lobule Bile entering the bile ducts eventually leaves the liver via the common hepatic duct Microscopic Anatomy of Liver Bile is a yellow-green, alkaline solution containing – – – – – – Bile salts Bile pigments Cholesterol Neutral fats Phospholipids (lecithin and others) Electrolytes Only bile salts and phospholipids aid the digestive process Microscopic Anatomy of Liver Bile salts, primarily cholic acid and chenodeoxycholic acids are cholesterol derivatives Their role is to emulsify fats which distributes them throughout the watery intestinal contents As a result, large fat globules entering the small intestine are physically separated into millions of small fatty droplets Microscopic Anatomy of Liver Millions of tiny fat droplets vastly increase the surface area for the fat digesting enzymes to work on Bile salts also facilitate fat and cholesterol absorption and help solubilize cholesterol, both that contained in bile and that entering the small intestine for food Microscopic Anatomy of Liver Although many substances secreted in bile leave the body in feces, bile salts are not among them Bile salts are conserved by a means of a recycling mechanism called enterohepatic circulation In this process bile salts are – Reabsorbed into the small intestine – Returned to the liver via the hepatic portal vein – Resecreted in newly formed bile Microscopic Anatomy of Liver The chief bile pigment is bilirubin, a waste product of hemoglobin (heme) during the breakdown of worn-out erythrocytes The globin and iron parts of hemoglobin are saved and recycled, but bilirubin is absorbed from the blood by the liver cells and actively excreted into the bile Microscopic Anatomy of Liver Most of the bilirubin in bile is metabolized in the small intestine by resident bacteria A breakdown by-product is urobilirubin which give feces its brown color In the absence of bile, feces are grey-white in color and have fatty streaks because essentially no fats are digested or absorbed Microscopic Anatomy of Liver The liver produces 500 to 1000 ml of bile daily, and bile production is stepped up when the GI tract contains fatty chyme Bile salts themselves are a major stimulus for enhance bile secretion Microscopic Anatomy of Liver The single most important stimulus of bile secretion is an increased level of bile salts in the enterohepatic circulation The Gallbladder The gallbladder is a thin-walled, green muscular sac, rouhgly the size of a kiwi fruit It snuggles in a shallow fossa on the ventral surface of the liver The Gallbladder The gallbladder stores bile that is not immediately needed for digestions The Gallbladder Bile that is not needed is concentrated by absorbing some of its water and ions When empty, its mucosa adopts the ridge like folds or rugae of the stomach Its muscular walls can contract to expell its contents into the cystic duct which then flows into the bile duct Like most of the liver it is covered by visceral peritoneum The Gallbladder When digestion is not occurring, the hepatopancreatic sphincter is tightly closed The Gallbladder Bile then backs up the cystic duct into the gallbladder where it is stored until needed The Gallbladder Although the liver makes bile continuously bile does not usually enter the small intestine until the gallbladder contract The major stimulus for gallbladder contraction is the intestinal hormone cholecystokinin (CCK) CCK is released to the blood when acidic, fatty chyme enters the duodenum The Gallbladder Besides causing the gallbladder to contract, CCk has two other important effects – It stimulates secreation of pancreatic juice – It relaxes the hepatppancreatic sphincter so that bile and pancreatic juice can enter the duodenum Parasympathetic impulses delivered by the vagus nerves have a minor impact on stimulating gallbladder contraction The Pancreas The pancreas is a soft, tadpole-shaped gland that extends across the abdomen The Pancreas Most the pancreas is retroperitoneal and lies deep to the greater curvature of stomach The Pancreas An accessory organ, the pancreas is important to the digestive process because it produces a broad spectrum of enzymes These enzymes break down all categories of foodstuffs, which the pancreas then delivers to the duodenum This exocrine product is called pancreatic juice The Pancreas Pancreatic juice drains from the pancreas via the centrally located main pancreatic duct The Pancreas The pancreatic duct generally fuses with the bile duct just as it enters the duodenum The Pancreas A smaller accessory pancreatic duct empties directly into the main duct The Pancreas Within the pancreas are the acini, clusters of secretory cells surrounding ducts The Pancreas The acini cells are full of rough endoplasmic reticulum and exhibit deeply staining zymogen granules containing digestive enzymes The Pancreas The pancreas also has an endocrine function Scattered amidst the acini are the more lightly staining pancreatic islets The Pancreas These Islets of Langerhans release insulin and glucagon, hormones that regulate carbohydrate metabolism Pancreatic Juice Approximately 1200 to 1500 ml of clear pancreatic juice is produced daily It consists mainly of water and contains enzymes and electrolytes The acinar cells produce the enzyme rich pancreatic juice The epithelial cells lining the smallest pancreatic ducts release the bicarbonate ions that make it alkaline (pH 8) The Pancreas The high pH enables pancreatic fluid to neutralize the acid chyme entering the duodenum It also provides the optimal environment for activity of intestinal and pancreatic enzymes Like pepsin of the stomach, pancreatic protein digesting enzymes are produced and released in active forms, which are then activated in the duodenum The Pancreas Within the duodenum trypsinogen is activated to trypsin by enterokinase an intestinal brush border enzyme Trypsin in turn activates two other pancreatic enzymes – Procarboxypeptidase > carboxypeptidase – Chymotrypsinogen > chymotrypsin Other pancreatic enzymes (amylase, lipase, and nucleases) are secreted in active form but require ions in the bile for activity Regulation of Pancreatic Secretion Secretion of pancreatic juice is regulated both by local hormones and by the parasympathetic nervous system Regulation of Pancreatic Secretion Secretin is released in response to the presence of HCL in the intestine Cholecystokinin is released in response to the entry of proteins and fats Regulation of Pancreas Secretion Both hormones act on the pancreas, but secretin targets the duct cells, prompting their release of watery bicarbonate-rich pancreatic juice, Whereas CCK stimulates the acini to release enzyme-rich pancreatic juice Vagal stimulation causes release of pancreatic juice primarily during the cephalic and gastric phases of gastric secretion Regulation of Pancreatic Secretion Normally, the amount of HCL produced in the stomach is exactly balanced by the amount of bicarbonate (HCO3) actively secreted by the pancreas HCO3 is secreted into the pancreatic juice, and H+ enters the blood Regulation of Pancreatic Secretion Consequently, the pH of venous blood returning to the heart remains relatively unchanged because alkaline blood draining from the stomach is neutralized by the acidic blood draining the pancreas Digestion: Small Intestine Although food reaching the small intestine is unrecognizable, it is far from being digested chemically Carbohydrates and proteins are partially degraded, but virtually no fat digestion has occurred to this point The process of food digestion is accelerated during the chyme’s journey of 3 to 6 hours through the small intestine, it is here that virtually all nutrient absorption occurs Optimal Intestinal Activity Although the primary functions of the small intestine are digestion and absorption, intestinal juice provides little of what is needed to perform these functions Most substances required for chemical digestion - bile, digestive enzymes (except for brush border enzymes) and bicarbonate ions (to provide the proper pH for enzymatic catalysis) are imported from the liver and pancreas Optimal Intestinal Activity Anything that impairs liver or pancreatic function or delivery of their juices to the small intestine severely hinders the individual’s ability to digest food and absorb nutrients Optimal Intestinal Activity Optimal digestive activity in the small intestine also depends on a slow, measured delivery of chyme from the stomach The small intestine can process only small amounts of chyme at one time Chyme enter the small intestine is usually hypertonic Optimal Intestinal Activity If large amounts of chyme were rushed into the small intestine, the osmotic water loss from the blood into the intestinal lumen would result in dangerously low blood volume Additionally, the low pH of entering chyme must be adjusted upward and the chyme must be well mixed with bile and pancreatic juice for digestion to continue These adjustments take time Optimal Intestinal Activity Food movement into the small intestine is carefully controlled by the pumping action of the stomach pylorus which prevents the duodenum from being overwhelmed Motility of the Small Intestine Intestinal smooth muscle mixes chyme thoroughly with bile and pancreatic and intestinal juices and moves food residues through the ileocecal valve and into the large intestine In contrast to the peristaltic waves of the stomach, which both mix and propel food, segmentation is the most common motion of the small intestine Motility of the Small Intestine In segmentation, chyme is moved backward and forward a few centimeters at a time by alternating contraction and relaxation of rings of smooth muscles Motility of the Small Intestine These segmenting movements of the intestine are initiated by intrinsic pacemaker cells (interstitial cells of Cajal) in the longitudinal smooth muscle layer Motility of the Small Intestine Unlike the somach pacemakers, which have only one rhythm, the pacemakers in the duodenum depolarizes more frequently (12-14 contractions per minute) than those of the ileum (8-9 contractions per minute) As a result, segmentation moves intestinal contents slowly and steadily toward the ileocecal valve at a rate that allows ample time to complete digestion and absorption Motility of the Small Intestine The intensity of the segmentation is altered by hormones and long and short reflexes – Parasympathetic enhances segmentation – Sympathetic decreases segmentation The more intense the contractions, the greater the mixing effect, however the basic contractile rhythms of the various intestinal regions remain unchanged Motility of the Small Intestine True peristalsis occurs only after most nutrients have been absorbed Segmentation movements wane, and peristaltic waves begin Motility of the Small Intestine Peristaltic waves initiated in the duodenum begin to sweep slowly along the intestine, moving 10 - 70 cm before dying out Each successive wave is initiated a bit more distally, and this pattern of peristaltic activity is called the migrating mobility complex A complete migration from the duodenum to the ileum takes about two hours and then repeats itself Motility of the Small Intestine Peristalsis serves to sweep out the last remnants of the meal plus bacteria, sloughed-off mucosal cells, and other debris into the large intestine This “housekeeping” function is critical for preventing the overgrowth of bacteria that migrate from the large intestine to the small intestine As food enters the stomach with the next meal segmentation replaces peristalsis Motility of the Small Intestine The local enteric neurons of the GI tract wall coordinate intestinal mobility patterns The physiological diversity of the enteric neurons allows a variety of effects to occur depending on which neurons are activated or inhibited Motility of the Small Intestine A given ACh-releasing (cholinergic) sensory neuron in the small intestine, once activated, may simultaneously send messages to several different interneurons in the myenteric plexus that regulate peristalsis: – Impulses sent proximally by cholingeric neurons cause contraction and shortening of the circular muscular layer Motility of the Small Intestine …interneurons in the myenteric plexus that regulate peristalsis: – Impulses sent distally to certain interneurons cause shortening of the longitudinal muscle layers and distension of the intestine, in response to Ach-releasing neurons – Other impulses sent distally by activated VIP or NO-releasing enteric neurons cause relaxation of the circular muscle Motility of the Small Intestine As a result, as the proximal area constricts and forces chyme along the tract, the lumen of the distal part of the intestine enlarges to receive it Motility of the Small Intestine Most of the time, the ileocecal sphincter is constricted and closed Two mechanisms, one neural and one hormonal , cause it to relax when ileal mobility increases and allow food residues to entry the cecum Enhance activity of the stomach initiates the gastroileal reflex, a long reflex than enhances the force of segmentation in the ileum Motility of the Small Intestine In addition, gastrin released by the stomach increases the motility of the ileum and relaxes the ileocecal sphincter Once the chyme has passes through, it exerts backward pressure that closes the valve’s flaps, preventing regurgitation into the ileum Large Intestine The large intestine frames the small intestine on three sides and extends from the ileocecal valve to the anus Large Intestine Its diameter is greater than that of the small intestine, but is less than half as long 1.5 meters Its major function is to absorb water from indigestible food residues (delivered to it in fluid state) and eliminate them from the body as semisolid feces Large Intestine Over most of its length, the large intestine exhibits three features not seen elsewhere; teniae coli, haustra, epiploic appendages Large Intestine Teniae coli are three bands of smooth muscle which are the remnants of the smooth muscle layer Large Intestine The muscle tone of the teniae coli cause the wall of the large intestine to form pocketlike sacs called haustra Large Intestine Epiplocic appendages are small fat-filled pouches of visceral peritoneum that hang from its surface. Significance is not known Large Intestine The large intestine has the following subdivisions; cecum, appendix, colon, rectum, and anal canal Large Intestine The saclike cecum, or blind pouch, lies below the ileocecal valve is the first part of the large intestine Large Intestine Attached to the cecum is the blind, wormlike, vermiform appendix Large Intestine The appendix contains masses of lymphoid tissue, and as part of the MALT it plays an important role in body immunity It has a significant structural problem in that its twisted tissue provides an ideal location for enteric bacteria to accumulate and multiply Large Intestine The colon has several distinct regions; ascending, transverse, and descending colon segments connected by flexures Large Intestine The ascending colon travels up the right side of the abdominal cavity to the level of the right kidney Large Intestine At the level of the kidney the colon makes a right-angle turn, the right colic, or hepatic flexure Large Intestine The transverse colon travels across the top of the abdominal cavity Large Intestine Directly anterior to the spleen, it bends downward to form the left colic or splenic flexure Large Intestine The descending colon descends down the left side of the abdominal cavity Large Intestine As the descending colon enters the pelvis it forms the S-shaped sigmoid colon Large Intestine The transverse and sigmoid portions of the colon are anchored to the posterior abdominal wall by mesentary sheets called mesocolons Large Intestine In the pelvis, at the level of the third sacral vertebra, the sigmoid colon joins the rectum, which is positioned anterior to the sacrum Large Intestine The natural orientation of the rectum allows for a number of pelvic organs to be examined digitally during a rectal exam Large Intestine The rectum has three lateral curves or bends represented internally are transverse folds called rectal valves Large Intestine Rectal valves separate feces from flatus, thus allowing gas to passed Large Intestine The anal canal lies entirely external to the abdominopelvic cavity About 3 cm long the canal begins where the rectum penetrates the muscles of the pelvic floor Large Intestine The anal canal has two sphincters – External anal sphincter – Internal anal sphincter Large Intestine The involuntary internal anal sphincter is composed of smooth muscle The voluntary external anal sphincter is composed of voluntary muscle These sphincters which act rather like purse strings to open and close the anus, are ordinarily closed excepts during defecation Large Intestine: Microscopic The wall of the large intestine differs in several ways from that of the small intestine The colon mucosa is simple columnar epithelium except in the anal canal Because most food is absorbed before reaching the large intestine, there are no circular folds, no villi, and no cells that secrete digestive enzymes Large Intestine: Microscopic Its mucosa is thicker, its abundant crypts are deeper, and there are tremendous numbers of goblet cells in the crypts Lubricating mucus produced by goblet cells eases the passage of feces and protects the intestinal wall from irritating acids and gases released by resident bacteria in the colon Large Intestine: Microscopic The mucosa of the anal canal is different from the rest of the colon, reflecting the greater abrasion that this region receives Large Intestine: Microscopic The mucosa hangs in long ridges or folds called anal columns and contains stratified squamous epithelium Large Intestine The anal sinuses are recesses between the anal columns which exude mucus when compressed by feces This aids in the emptying of the canal Large Intestine The horizontal lines that parallels the inferior margin of the anal sinuses is called the pectinate line The line separates areas of visceral and somatic sensory innervation Pectinate line Large Intestine: Microscopic The mucosa superior to the line is innervated by visceral sensory fibers and so are relatively insensitive to pain The are inferior to the pectinate line is innervated by somatic sensory fibers and is very sensitive to pain Large Intestine: Microscopic Two superficial venous plexuses are associated with the anal canal, one with the anal columns and the other with the anus itself Where these veins (hemorhoidal) are inflamed, itchy varicosities called hemorrhoids result Large Intestine: Microscopic In contrast to the more proximal regions of the large intestine, teniae coli and haustra are absent in the rectum and anal canal Consistent with its need to generate strong contractions to perform its expulsive role, the rectum’s muscularis muscle layers are complete and well developed Bacterial Flora Although most bacteria entering the cecum from the small intestine are dead having been killed by the action of lysozyme, defensins, HCL, and protein digesting enzymes The bacteria that survive, together with the bacteria that enter the GI tract via the anus, constitute the bacterial flora of the large intestine Bacterial Flora The bacterial flora colonize the colon and ferment some of the indigestible carbohydrates (cellulose and others) releasing irritating acids and a mixture of gases – Dimethyl sulfide, H2, N2, CH4, and CO2 About 500 ml of gas is produced each day with much more when certain carbohydrate rich foods are eaten The bacterial flora also synthesize B complex vitamins and most of vitamin K Processes: Large Intestine What is finally delivered to the large intestine contains few nutrients, but still has 12 to 24 hours more digestive system Except for the small amount of digestion of residue by the enteric bacteria, no further food breakdown takes place in the large intestine Processes: Large Intestine Although the large intestine harvests vitamins made by the bacterial flora and reclaims most of the remaining water and some of the electrolytes (particularly sodium and chloride) absorption is not a major function of this organ The primary concern of the large intestine are propulsive activities that force the fecal material toward the anus and then eliminate it from the body Processes: Large Intestine While the large intestine is undeniably essential for our comfort, it is not essential for life Several different surgical procedures remove a part or all of the large intestine in order to save life Motility: Large Intestine The large intestine musculature is inactive much of the time, and when it is mobile, its contractions are sluggish and of short duration The most frequent movements seen in the colon are haustral contractions, which are slow segmenting movements that occurs every 30 minutes or so Motility: Large Intestine Haustral contractions reflect local controls of smooth muscle within the walls of individual haustra As a haustrum fills with food residue, the distension stimulates its muscle to contract, which propels the luminal contents into the next haustrum These movements also mix the residue which aids in water absorption Motility: Large Intestine Mass movements (mass peristalsis) are long, slow-moving, but powerful contractile waves that move over large areas of the colon three or four times daily and force the contents toward the rectum Typically these movements occur during or just after eating when the presence of food in the stomach activates the gastroileal reflex in the small intestine and the propulsive gastrocolic reflex in the colon Motility: Large Intestine Bulk, or fiber, in the diet increases the strength of colon contractions and softens the stool, allowing the colon to act more efficiently Defecation The rectum is usually empty, but when feces are forced into it by mass movements, stretching of the rectal walls initiates the defecation reflex Defecation This is a spinal cord mediated reflex that causes the walls of the sigmoid colon and the rectum to contract and the anal sphincters to relax Defecation Distension or stretch of the rectal walls triggers a depolarization of sensory (afferent) fibers which synapse with the spinal cord Defecation Parasympathetic motor (efferent) fibers, in turn, stimulate contraction of the rectal walls and relaxation of the internal anal sphincter Defecation If it is convenient to defecate, voluntary signals stimulate the relaxation of the external anal sphincter Defecation As feces are forced into the anal canal, impulses reach the brain allowing us to decide whether the external(voluntary) anal sphincter should remain open or closed If defection is delayed, the reflex contractions end within a few seconds and the walls relax With the next mass movement, the reflex is initiated again and again until one chooses to defecate