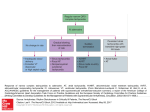
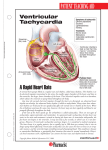
* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Rhythm disorders in neonates
Remote ischemic conditioning wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Heart failure wikipedia , lookup
Coronary artery disease wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Jatene procedure wikipedia , lookup
Cardiac surgery wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Myocardial infarction wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Atrial fibrillation wikipedia , lookup
Electrocardiography wikipedia , lookup
Ventricular fibrillation wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Review article Acta Pediátr Mex 2014;35:134-144. Rhythm disorders in neonates Luis Martín Garrido-García1 María de Guadalupe Delgado-Onofre2 1 Pediatric cardiologist. Head of Undergraduate and Postgraduate Department. 2 Third year resident. Instituto Nacional de Pediatría, México, D.F. ABSTRACT Arrhythmias are a variety of heart rhythm alterations which may occur in fetuses and neonates considered healthy. The majority are benign. The incidence reported varies from 1 to 10% in neonates in the first days of extrauterine life. Arrhythmias in the neonatal stage entail high morbidity and mortality, above all when they occur in patients with congenital heart disease or lack of response to medical treatment. Opportune pharmacological control of rhythm offers a good long-term prognosis. The natural history of arrhythmias in the neonatal period differs from arrhythmias in other pediatric age groups; they can be classified as: sinus arrhythmia, tachyarrhythmias, long QT syndrome, and bradyarrhythmias. It is important that doctors in charge of treating this group of patients recognize the causal factors of arrhythmias, and the diagnostic and therapeutic options available. Key words: arrhythmias, neonates, sinus dysrhythmia, tachyarrhythmias, long QT syndrome, treatment, prognosis. 134 Received: August, 2013 Accepted: January, 2014 Correspondence Dr. Luis Martín Garrido García Insurgentes Sur 3700, Letra C Col. Insurgentes Cuicuilco CP 04530, México D.F. Tel: 1084-0900 [email protected] This article must be quoted Garrido-García LM y Delgado-Onofre MG. Trastornos del ritmo en el recién nacido. Acta Pediat Mex 2014;35:148-158. www.actapediatricademexico.org Garrido-Garcia LM and Delgado-Onofre MG. Heart rhythm disorders in neonates The electrocardiogram (ECG) is the reference procedure to identify heart rhythm alterations in neonates; however, it is necessary to ascertain that an arrhythmia is not transitory. With the development of neonatal intensive care units and increased monitoring of patients, in both the prenatal and postnatal stages, various rhythm alterations have been identified in fetuses and neonates considered healthy.1,2 The majority of those arrhythmias are benign; however, detecting them requires a thorough evaluation of them and the risk factors for their genesis, such as maternal illnesses or infections, fetal distress, or congenital heart disease. An incidence of heart rhythm alterations of between 1 and 10% has been described in healthy neonates in the first days of extrauterine life; notwithstanding, this figure is higher in patients admitted to neonatal intensive care units.2-5 PATHOPHYSIOLOGY Arrhythmias may occur as a result of various mechanisms; the most important are: defects in impulse generation with increase or reduction of automaticity and defects in conduction of stimulus with a simple block or one-directional block and a reentry mechanism. However, for these alterations to manifest clinically there must be a pathophysiological substrate, in the neonate, that predisposes him/her to rhythm disorders. The most common are: 1) hydroelectrolytic alterations; 2) hypoxemia; 3) immaturity of the autonomic nervous system; 4) myocarditis; 5) congenital heart disease; or 6) endovenous catheters that irritate the endocardium.6 Evaluation of neonates with arrhythmias starts with the search for maternal factors, which may trigger rhythm alterations, in electrolyte intake and blood sugar. A surface electrocardiogram is sufficient to establish a diagnosis in most cases. An echocardiogram is indicated in symptomatic patients, in those with suspected congenital heart disease and with persistent arrhythmias. A 24hour (Holter) electrocardiogram can establish a diagnosis in patients with arrhythmias which cannot be documented with a surface electrocardiogram.4,6 SINUS DYSRHYTHMIA Sinus dysrhythmia is the most common form of change in heart rhythm in neonates and is considered a normal variant; the heart rate drops during expiration and rises during inspiration. This type of rhythm is more evident during episodes of fever.7 TACHYARRHYTHMIAS This term means an abnormal increase in heart rate. They are considered “benign” tachycardias when there is no clinical hemodynamic repercussion and no treatment is required. This type of phenomena do not require follow up because they do not affect health.4,5 Depending on the site where these arrhythmias are generated, they can be classified as: a) supraventricular tachyarrhythmias (when there is an ectopic focus above the bundle of His or it participates in the circuit of the arrhythmia) and b) ventricular tachyarrhythmias (when the abnormal stimulus is generated below the bundle of His). Finally, if the start and end of the abnormal rhythm are sudden or gradual, tachyarrhythmias are classified as paroxysmal or non-paroxysmal. The most common form of non-paroxysmal tachycardia is sinus tachycardia, in which case the various factors that triggered the tachycardia must be corrected: anemia, hydroelectrolytic alterations, sepsis, respiratory problems, etc.5-9 (Figure 1). 135 Volume 35, No. 2, March-April 2014 Acta Pediátrica de México Figure 1. 12-lead electrocardiogram of a neonate of 8 days of extrauterine life and neonatal sepsis, with fever of 39ºC and heart rate 200 bpm. We also observe dilation of right auricle and ventricle. Supraventricular tachyarrhythmias Supraventricular extrasystoles Are premature heartbeats originating in the atria. They have been reported to exist in 5 to 30% of neonates, a figure which is higher in preterm neonates.10 Electrocardiographically there is premature atrial depolarization with an abnormal morphology; if depolarization is conducted to the ventricles it usually does so with a normal ventricular complex. If the supraventricular extrasystole is capable of reactivating the sinus node it will have an incomplete compensatory pause. (Figure 2). In these heart rhythm disorders patients are usually asymptomatic and they are considered benign events in patients with structurally healthy hearts. Supraventricular extrasystoles can be triggered by several causes, among them: toxic concentrations of sympathomimetic amines such as isoproterenol or dopamine, or by central catheters which cause mechanical irritation. If supraventricular extrasystoles are frequent, a chest x-ray and an electrocardiogram are indicated to rule out congenital heart disease or cardiomyopathy. Such patients should be monitored for three or four days and a 24-hour electrocardiographic record is indicated. If there are no episodes of 136 Figure 2. Healthy neonate of 15 days of extrauterine life with extrasystoles detected by auscultation. The electrocardiogram shows supraventricular extrasystoles with incomplete compensatory pause. supraventricular tachycardia the patients do not require treatment; however, they are kept under observation for a month. Cases in which atrial extrasystoles trigger supraventricular tachycardia with alteration of ventricular function should receive treatment.6,7 Atrial ectopy This arrhythmia is very common in fetuses and neonates. It is produced by increased automaticity in a group of atrial cells which are not part of the normal conduction system. In the ECG they appear as tachycardias with a narrow QRS complex and an abnormal P wave with variable morphology (migratory pacemaker) or they may have a single ectopic focus. It tends to accelerate and decelerate (“heating” and “cooling” phenomenon). In most cases this arrhythmia disappears over time and does not cause further complications; however, when the ectopic atrial rhythm has a frequency above 200 bpm and accelerated ventricular conduction, it can cause heart failure and dilated cardiomyopathy.7,8 Atrioventricular reentry tachycardia Occurs in one of every 1,700 neonates and is the leading cause of supraventricular paroxysmal Garrido-Garcia LM and Delgado-Onofre MG. Heart rhythm disorders in neonates tachycardia in the neonatal period in up to 50% of cases.2-5 For this arrhythmia to occur there must be an accessory pathway that can allow anterograde or retrograde conduction (Wolff-Parkinson-White WPW syndrome) or a pathway with only retrograde conduction (occult pathway). In most cases the tachycardia starts with an extrasystole which may be atrial or ventricular; it causes a one-directional block, usually in the accessory pathway, although it may also occur in the atrioventricular node and the tachycardia is initiated by a reentry mechanism.6-9 (Figures 3 and 4) To distinguish an atrioventricular reentry tachycardia from other forms of supraventricular tachycardia, it is important to locate the P wave on the electrocardiogram during the tachycardia. In atrioventricular reentry tachycardia there is a retrograde P wave which is inscribed after the QRS complex. For these arrhythmias atrial and ventricular tissue is required to maintain the reentry circuit; therefore, there cannot be atrioventricular block or disassociation during the arrhythmia.7,8 These arrhythmias occur more commonly in patients with structurally healthy hearts; however, WPW syndrome may be associated with Ebstein disease, corrected transposition of the great vessels, or hypertrophic cardiomyopathy.3 It is well established that neonates with WPW syndrome have a high probability of resolution of supraventricular tachycardia in the first year of life. However, it has also been shown that up to one third of such patients with resolution of symptoms have a probability of a relapse of tachycardia at school age.3,6 Figure 3. 12-lead electrocardiogram of a patient of 1 month of age taken to the Emergency Service with hemodynamic deterioration. Physical exploration detected tachycardia with a narrow QRS complex; ventricular heart rate of 300 bpm; retrograde P wave. Lemler et al. conducted a study to identify risk factors for reincidence of symptoms in patients with WPW in subsequent stages of life. They analyzed the following factors: heart failure during the arrhythmia, recurrence of the arrhythmia during treatment in the first year of life, difficulty controlling the arrhythmia in the initial period, congenital heart disease and persistence of the delta wave on the electrocardiogram. They found that the only positive predictive factor for recurrence of the arrhythmia was persistence of the delta wave despite treatment.11 Atrial flutter Figure 4. 12-lead electrocardiogram of the same patient as Figure 3 after electric cardioversion. In sinus rhythm with a short PR interval (90 ms) and delta wave. Wolff-Parkinson-White Syndrome. Although it is a common rhythm disorder in fetuses (25% of tachycardias in fetuses) and in neonates, it is very rare in pediatric age and does not become common again until adult age. It is associated with congenital heart diseases: endocardial fibroelastosis or cardiomyopathies, 137 Acta Pediátrica de México chromosomal alterations, and other pathological states in up to 30% of cases. Electrocardiographically it is characterized by a “sawtooth” shaped pattern of P waves with frequencies ranging from 300 to 600 beats per minute; the ventricular response may be regular or irregular, but with lower frequency (Figure 5). This arrhythmia has high morbidity and mortality in the neonatal stage, especially if it is associated with congenital heart diseases or lack of response to medical treatment; however, if pharmacological control of the rhythm is achieved, the long-term prognosis is good.7-9,12 Treatment of supraventricular tachyarrhythmias Acute treatment. Depends on the patient’s general condition. In cases of tachycardia with narrow QRS complex, without hemodynamic compromise, the initial treatment is to attempt to suppress the arrhythmia with vagal maneuvers like applying a cold compress on the patient’s face for 10 to 20 seconds and even facial immersion in cold water for 5 seconds. Ocular compression or carotid massage are not recommended. These maneuvers trigger the “diving reflex,” which not only causes vagal stimulation but also a drop in sympathetic activity. During the procedure, the electrocardiographic record and blood pressure should be monitored, due to the possibility of asystole at the end of the Volume 35, No. 2, March-April 2014 supraventricular tachycardia.7-9,13 If treatment with vagal maneuvers is ineffective intravenous adenosine is recommended in both term and preterm neonates; initial dose 50 to 150 mg/ kg. The dose may be increased by 50 g/kg every minute to a maximum dose of 250 to 500 mg/ kg. Side effects of large doses of adenosine are bronchoconstriction, stridor, and low blood pressure secondary to peripheral vasodilation.13 If the tachycardia persists despite treatment, with hemodynamic instability of the patient, electric cardioversion is indicated. The application of current should be synchronized with the QRS complex, starting with a dose of 0.5 joules per kilogram of body weight. In the large majority of cases cardioversion is effective to stop the supraventricular tachycardia.7-9,11,13,14 Chronic treatment. In neonates with a history of supraventricular tachycardia, when the acute event is resolved, chronic treatment should be initiated to prevent recurrence of the tachycardia. Digoxin and b blockers are the first-line agents for treating reentry tachyarrhythmias. Class 1A (procainamide), IC (propafenone or flecainide) and class 3 (amiodarone) antiarrhythmic drugs have also been used successfully when digoxin and b blockers are ineffective. Use of calcium antagonists in neonates should be avoided as a sudden drop in cardiac flow following their administration has been reported13,14 (Table 1). Ablation with radiofrequency in the neonatal stage has been used in isolated cases where there is recurrence of arrhythmia with hemodynamic deterioration despite treatment which has also had the side effects of antiarrhythmic drugs.14,15 Ventricular tachyarrhythmias Figure 5. Rhythm strip from a neonate of 15 days with diagnosis of transposition of the great vessels, who underwent “arterial switch”. We can observe the “sawtooth waves” typical of atrial flutter with heart rate of 150 bpm and 2:1 conduction with mean ventricular heart rate of 75 bpm. 138 Ventricular extrasystoles Are defined as premature ventricular complexes. The following criteria are used in electrocardio- Garrido-Garcia LM and Delgado-Onofre MG. Heart rhythm disorders in neonates graphic diagnosis: 1) early start of QRS complex; 2) duration of QRS complex greater than 80 ms; 3) abnormal morphology of QRS complex with alteration in the ST segment and in the T wave; and 4) no preceding P wave.3 Ventricular extrasystoles are common in neonates with structurally healthy hearts; their occurrence has been reported in up to 18% of healthy neonates who have undergone a 24-hour Holter in the first day of extrauterine life.3,4 Premature ventricular contractions have also been observed in patients with hypoxia, hypoglycemia, myocarditis, ventricular hypertrophy, ventricular tumors, or ventricular catheters3-6,9 (Figure 6). Table 1. Antiarrhythmic drugs indicated in neonatology88 (continued on next page) Drug Oral Dose IV Dose Indications Side effects Remarks Adenosine 0.05 mg/kg. The dose Reentry SVT Dyspnea, arrhythmias, Administer rapidly may be increased Diagnosis of atrial AV block, palpitations, every 2 minutes by flutter bradycardia 0.05 mg/kg Amiodarone 10-20 mg/kg/day (Class 3) for 7 to 14 days and then 5 mg/ kg/day DI: 5 mg/kg in 1 h; Refractory SVT, VT, Proarrhythmia, brady- M o n i t o r p u l m o DM continuous in- and VF c a r d i a , AV b l o ck , nary and thyroid fusion 10-15 mg/kg/ hypothyroidism, in- functions day terstitial pneumonitis, pulmonary fibrosis, photosensitivity Digoxin DI: 15-20 μg/kg divi- SVT, atrial flutter ded in 3 doses. DM: 4-8 μg/kg/day divided in 2 doses/ day Maintenance 5-10 mg/kg/day divided in 2 doses F l e c a i n i d e 1-3 mg/kg/day in (Class 1c) 3 doses. May be increased to up to 3-6 mg/ kg/day Lidocaine Bradycardia, arrhythmias, delayed conduction, lethargy, vomiting, diarrhea Contraindication: VT, hypokalemia, AV block. Use with caution in WPW syndrome: may cause VF Refractory tachycar- Bradycardia, AV block, dias: SVT, VT a r r hy t h m i a s, h e a r t failure, blood dyscrasias, liver dysfunction, dyspnea Contraindication: retarded conduction, liver or myocardial dysfunction 1 mg/kg/dose in 1 to VT, VF 2 minutes. Infusion 20-50 μg/ kg/min Low blood pressure, Use after a cardiobradycardia, arrhyth- version mias, lethargy, vomiting, paresthesia, respiratory depression Procainami- 15-50 mg/kg/day DI. 3-6 mg/kg/dose SVT, WPW, VT de Divided in 4-8 in 5 minutes (Class 1a) doses/day DM. Continuous infusion 20-80 mg/ kg/min Low blood pressure, block, arrhythmias, vomiting, diarrhea, blood dyscrasias, hepatomegaly, increase in liver enzymes Contraindication: blockage in conduction, helical ventricular tachycardia Propranolol 0.25 mg/kg/dose (Class 2) every 6-8 h; increase to a maximum of 5 mg/ kg/day Low blood pressure, heart failure, arrhythmias, alterations in conduction, asystole, lethargy, hypoglycemia, hyperglycemia, bronchospasm, vomiting, diarrhea, agranulocytosis Contraindication: asthma, bradycardia, heart block, cardiogenic shock SVT, WPW, VT 139 Volume 35, No. 2, March-April 2014 Acta Pediátrica de México Table 1. Antiarrhythmic drugs indicated in neonatology8 (continuation) Drug Oral Dose Quinidine (Class 1a) IV Dose Indications Side effects Remarks 15-60 mg/kg/day divided in 4 doses/day SVT, VT Low blood pressure, heart block, ventricular fibrillation, fever, vomiting, diarrhea, blood dyscrasias, respiratory depression Contraindication: WPW heart block with propranolol Reduce the dose of digoxin in case of combined use Sotalol (Class 2/3) 2-4 mg/kg/day in 2 doses SVT, WPW, VT Low blood pressure, helical ventricular tachycardia, blockage in conduction, bradycardia, fatigue, hypoglycemia. Contraindication: structural heart disease, bronchospasm, heart block Verapamil (Class 4) 4-8 mg/kg/day in 3 doses Refractory tachycar- L ow b l o o d p r e s s u r e , Contraindication: dias: SVT, VT bradycardia, apnea Children < 1 year and WPW ST: sinus tachycardia; SVT: supraventricular tachycardia; VT: ventricular tachycardia; VF: ventricular fibrillation; WPW: WolffParkinson-White. Ventricular tachycardia Figure 6. 12-lead surface electrocardiogram of a neonate with diagnosis of double right ventricle outlet. Shows acuminate P wave and right ventricular hypertrophy. Bigeminal ventricular extrasystoles (normal heartbeat and abnormal heartbeat). In neonates with ventricular extrasystoles, a chest x-ray and an echocardiogram are indicated to rule out an underlying heart disease. Patients with structurally healthy hearts and isolated ventricular extrasystoles do not require treatment. In cases of underlying heart disease and frequent ventricular extrasystoles (more than ten per hour), of polymorphic ventricular extrasystoles or when there are pairs of them, the initiation of antiarrhythmic therapy is indicated.3-6,9 140 Is defined as the presence of three or more consecutive ventricular extrasystoles with a heart rate above 120 bpm. This tachycardia may be monomorphic, when the abnormal beats have a single morphology, or polymorphic: different morphologies in the extrasystoles, which means that there are multiple ectopic foci. It may be nonsustained (less than 30 seconds of arrhythmia) or sustained ventricular tachycardia. Incessant ventricular tachycardia is arrhythmia in more than 10% of a day.3-6,9,16 This type of arrhythmias are uncommon in the neonatal stage, and when they appear their causes should be investigated. Usually, antiarrhythmic therapy is required. Conditions to consider as possible causes of ventricular tachycardias include: myocarditis, ventricular tumors, myocardial infarction secondary to anomalies in the coronary arteries, electrolyte disorders, metabolic diseases, drug use, and long QT syndrome3-6,9,16 (Figure 7). Neonates with sustained ventricular tachycardia suffer hard-to-control heart failure and may Garrido-Garcia LM and Delgado-Onofre MG. Heart rhythm disorders in neonates long QT (corrected QT > 450 ms) on the surface electrocardiogram.6,17,18 (Figure 8). Figure 7. Male patient of two days’ extrauterine life with severe neonatal asphyxia and hypoxic cardiomyopathy who developed ventricular tachycardia. 12lead electrocardiogram: ventricular tachycardia with wide QRS complexes and mean ventricular heart rate of 300 bpm. develop cardiogenic shock; they have a poor prognosis given that, even with antiarrhythmic therapy, mortality near 50% has been observed.16 Treatment of ventricular tachycardias In patients with ventricular tachycardia and hemodynamic compromise, it is indicated, initially to perform electric cardioversion or defibrillation with a dose of 2 joules per kilogram of body weight. In patients with nonsustained ventricular tachycardia, without hemodynamic deterioration, antiarrhythmic therapy with lidocaine or amiodarone should be initiated. In cases of incessant and recurrent ventricular tachycardia, despite medical treatment, an electrophysiological study is indicated to locate the origin of the ventricular tachycardia and attempt ablation with radiofrequency6-9,13 (Table 1). LONG QT SYNDROME Long QT syndrome (LQT) is a hereditary disease and causes sudden death in the neonatal stage; it is associated with both bradycardia and helical ventricular tachycardia (torsade de pointes)6,17,18 The diagnosis is based on a family history of sudden death and the finding of a Figure 8. Rhythm strip from a patient with heart rate of 75 bpm. QT interval 460 ms. The QT interval corrected by heart rate (Bazett formula = measured QT interval (ms)/ÖR-R (ms) of 470 ms). Normal up to 450 ms. Recently long QT syndrome has been associated with three molecular abnormalities in transport of electrolytes across the cell membrane: LQT 1 and LQT 2, related to potassium channels, and LQT 3, which is accompanied by alterations in sodium channels. A higher incidence of cardiovascular symptoms has been found in LQT 1 and LQT 2; there is higher mortality in LQT 3.17,18 Treatment of long QT syndrome uses propranolol at high doses to lower the adrenergic discharges involved in the genesis of arrhythmias. If such treatment proves unsuccessful, placement of a permanent pacemaker or an implantable automatic defibrillator is indicated.13,17-19 BRADYARRHYTHMIAS In neonates a drop in cardiac rhythm may be due to alterations in impulse generation (function of the pacemaker) or in conduction of the stimulus. Sinus bradycardia Is defined as a heart rate below 90 beats per minute and has been described as the leading cause of rhythm disorders in the neonatal stage. This bradycardia may be primary, due to sinus 141 Acta Pediátrica de México node dysfunction; it is very rare in the neonatal period and is associated with immaturity of the central nervous system, and therefore is more common in preterm neonates.10 The most common causes of pathological sinus bradycardia are hypoxia and use of medications6,20 (Figure 9). Volume 35, No. 2, March-April 2014 prolongation of the PR interval with eventual failure of conduction and a blocked heartbeat. This block is associated with medications or with maternal connective tissue disease. In the Mobitz 2 block the alteration is located in the distal part of the conduction system. It is characterized by normal PR intervals interrupted by a blocked heartbeat. This block has a more serious prognosis and in some cases may require placement of a pacemaker.3,6,20 Congenital complete atrioventricular block Figure 9. Female patient of 15 days’ extrauterine life, asymptomatic. With sinus arrhythmia and sinus bradycardia with ventricular heart rate of 80 bpm during sleep. First degree atrioventricular block Is the presence of a PR interval above the normal limit for the patient’s age. The normal PR interval in the neonatal period varies from 0.06 to 0.14 s (0.17 seconds in the first day of extrauterine life). A prolonged PR interval may be due to alterations in atrial conduction, in the atrioventricular node, or in the His-Purkinje system. It is very commonly associated with congenital heart diseases or with inflammatory heart diseases. Medications that raise vagal tone can also prolong the PR interval. The majority of patients are asymptomatic and do not require treatment.3,6 Congenital complete atrioventricular block occurs in 15 000 to 20 000 live births. It is characterized by failure of conduction of cardiac stimulus from the atrium to the ventricles. The atrial rhythm is higher than the ventricular and the P waves have no relationship with the QRS complexes2,6,21 (Figure 10). Congenital complete atrioventricular block may occur in a structurally healthy heart or be associated with congenital heart diseases. Patients with congenital atrioventricular block and structurally healthy hearts are very commonly associated Second degree atrioventricular block Is characterized by intermittent failure of conduction of stimulus to the ventricles. There are two forms: Mobitz 1, with blockage in the atrioventricular node which produces the characteristic Wenckebach phenomenon, consisting of gradual 142 Figure 10. Male patient of 40 days’ extrauterine life with Holt-Oram syndrome. Interatrial communication with signs of heart failure. 12-lead electrocardiogram showing complete atrioventricular block, with atrioventricular disassociation. P waves with heart rate of 150 bpm and QRS complexes with heart rate of 75 bpm. Garrido-Garcia LM and Delgado-Onofre MG. Heart rhythm disorders in neonates with exposure to anti-Ro (SS-A) and anti-La (SS-B) antibodies. Such antibodies are common in women with connective tissue disease, especially systemic lupus erythematosus and Sjögren syndrome. These antibodies cause tissue damage and fibrous degeneration of conductive tissue.20,22 Congenital heart block in patients with heart disease is associated with complex congenital anomalies such as L-transposition of the great vessels, left isomerism, and also in patients with trisomy 18.6,20-22 Patients with congenital atrioventricular block may be asymptomatic or develop left ventricular dysfunction and heart failure in early stages of life and even in the prenatal stage. In such cases an unstable ventricular escape rhythm is observed, with heart rate below 50 bpm, and a permanent pacemaker is indicated. Eronen et al. studied 91 patients with congenital atrioventricular block. They observed that despite early placement of permanent pacemakers in symptomatic neonates, they developed heart failure and dilated cardiomyopathy: risk factors for this torpid evolution were hydrops, fetal and neonatal bradycardias, low birth weight, male patients with neonatal problems associated with “prematurity” or with neonatal lupus.23,24 CONCLUSIONS Arrhythmias in neonates are not common events. However, the natural history of arrhythmias in the neonatal period differs greatly from that of arrhythmias in other pediatric age groups. It is important for physicians who attend to this group of patients to know how to recognize rhythm disorders, the factors for development of arrhythmias, and the available diagnostic and therapeutic options. REFERENCES 1. Semizel E, Öztürk B, Bostan OM, Cil E, Ediz B. The Effect of Age and Gender on the Electrocardiogram in Children. Cardiol Young 2008;18:26-40. 2. Poddar B, Basu S, Parmar VR. Neonatal Arrhythmias. Ind J Pediatr 2006;73:131-134. 3. Dubin AM. Arrhythmias in the Newborn. NeoReviews 2000;1:146-151. 4. Badrawi N, Hegazi RA, Tokovic E, Lofty W, Mahmoud F, Aly H. Arrhythmia in Neonatal Intensive Care Unit. Pediatr Cardiol 2009;30:325-330. 5. Massin MM, Benatar A, Rondia G. Epidemiology and Outcome of Tachyarrhythmias in Tertiary Pediatric Cardiac Centers. Cardiology 2008,111:191-196. 6. Fish FA, Benson DW Jr. Disorders of Cardiac Rhythm and Conduction. En Allen HD, Gutgesell HP, Clark EB, Driscoll DJ. Heart Disease in Infants, Children and Adolescents. 6th Edition. Philadelphia: Lippincott, Williams & Wilkins, 2001. pp: 482-533. 7. Larmay HJ, Strasburger JF. Differential Diagnosis and Management of the Fetus and Newborn with an Irregular or Abnormal Heart Rate. Pediatr Clin N Am 2004;51:10331050 8. Kothari DS, Skinner JR. Neonatal Tachycardias: An Update. Arch Dis Child Fetal Neonatal 2006;91:F136-144. 9. Watson M. Neonatal Tachyarrhythmias. Neonatal Network 2000;19:45-51. 10. Scagliotti D, Deal BJ. Arrhythmias in the Tiny, Premature Infant. Clin Perinatol 1986;13:339-350. 11. Lemler MS, Schaffer MS. Neonatal Supraventricular Tachycardia: Predictors of Successful Treatment Withdrawal. Am Heart J 1997;133.130-131. 12. Lisowski LA, Verheijen PM, Benatar AA, Soyeur DJ, Stoutenbeek P, Brenner JI, Kleinman CS, Meijboom EJ. Atrial Flutter in the Perinatal Age Group: Diagnosis, Management and Outcome. J Am Coll Cardiol 2000;35:771-777. 13. Ward RM, Lugo RA. Cardiovascular Drugs for the Newborn. Clin Perinatol 2005;32979-997. 14. Gilljam T, Jaeggi E, Gow RM. Neonatal Supraventricular Tachycardia: Outcomes Over a 27-year period at a Single Institution. Acta Pediatrica 2008;97:1035-1039. 15. Iturralde-Torres P, Garrido-García LM. Ablación con Radiofrecuencia en el Tratamiento de las Arritmias Supraventriculares en Pediatría. Experiencia en 203 Pacientes Consecutivos. Arch Inst Cardiol Mex 1998;68:27-36. 16. Perry JC. Ventricular Tachycardia in Neonates. Pacing Clin Electrophysiol 1997;20:2061-4. 17. Crotti L, Celano G, Dagradi F, Schwartz PJ. Congenital Long QT Syndrome. Orphanet Journal of Rare Diseases 2008;3:318. 18. Schwartz PJ, Stramba-Badiales M, Crotti L, Pedrazzzini M, Besana A, Bosi G, et al. Prevalence of the Congenital LongQT Syndrome. Circulation 2009;120:1761-1767. 19. Stramba-Badiale M, Goulene K, Schwartz PJ, Effects of Beta-adrenergic Blockade on Dispersion of Ventricular Repolarization in Newborn Infants with Prolonged QT Interval. Am Heart J 1997;134:406-410. 143 Volume 35, No. 2, March-April 2014 Acta Pediátrica de México 20. O’Connor M, McDaniel N, Brady WJ. The Pediatric Electrocardiogram Part II: Dysrhythmias. Am J Emerg Med 2008;26:348-358. Smallest Successful Pacemaker Implantation. J Perinatol 2004;24:112-117. 21. Gillete PC, Fyfe DA, Ross BA. Atrioventricular Block. En: Walker A, Long MB. Fetal and Neonatal Cardiology. WB Saunders Co, 1990. pp: 519-524. 23. Eronen M, Siren MK, Ekblad H, Tikanoja T, Julkunen H, Paavilainen T. Short and Long Term Outcome of Children With Congenital Complete Heart Block Diagnosed in Utero or as a Newborn. Pediatrics 2000;106:86-91. 22. Donofrio MT, Gullquist SD, Mehta ID, Moskowitz WB. Congenital Complete Heart Block: Fetal Management Protocol, Review of the Literature, and Report of the 24. Eronen M. Long-Term Outcome of Children With Complete Heart Block Diagnosed After the Neonatal Period. Pediatr Cardiol 2001;22:133-137. Visit Acta Pediátrica de México on line: www.actapediatricademexico.org FB: actapediatricademexico Twitter: @ActaPedMex 144