* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download PDF - Circulation: Arrhythmia and Electrophysiology
Survey
Document related concepts
History of invasive and interventional cardiology wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Heart failure wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Coronary artery disease wikipedia , lookup
Myocardial infarction wikipedia , lookup
Jatene procedure wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Electrocardiography wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Ventricular fibrillation wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Transcript
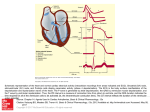
Images and Case Reports in Arrhythmia and Electrophysiology Left Ventricular Outflow Tract Tachycardia With Preferential Conduction and Multiple Exits Takumi Yamada, MD; Michael Platonov, MD; H. Thomas McElderry, MD; and G. Neal Kay, MD A Downloaded from http://circep.ahajournals.org/ by guest on May 14, 2017 RVOT, GCV, and right coronary cusp (RCC) (VT 2, Figure 1C; VT 3, Figure 1D; and VT 4, Figure 1E, respectively). Gradual transition between 2 of those VT morphologies (VT 3 and VT 4) was observed, and the local ventricular activation in the GCV preceded the QRS onset during both of those VTs (Figure 2). The local ventricular activation in the GCV relative to that in the His bundle region was 35 ms earlier during VT 3 than VT 4 (Figure 2). Because RF applications in the GCV were limited by high impedance, epicardial mapping via a subxiphoid access was performed. However, no epicardial ventricular activation as early as in the GCV could be recorded. Very detailed endocardial and epicardial activation mapping of both the RVOT and LVOT during the multiple morphologies of VT revealed a consistently early activation in the AMC but variable activation times at remote sites. Finally, RF applications delivered to the medial AMC with an irrigated ablation catheter eliminated all the ventricular arrhythmias (VAs) (Figure 3). In this case, a single intramural origin with a preferential conduction1 to multiple exit sites all over the RVOT and 50-year-old man with idiopathic premature ventricular contractions (PVCs; PVC 1, Figure 1A) and ventricular tachycardias (VTs) was referred for catheter ablation. Activation and pace mapping were performed at multiple sites in the right and left ventricular outflow tracts (RVOT and LVOT) (Figure 1). Nonirrigated radiofrequency (RF) applications delivered in the left coronary cusp where pacing reproduced a perfect pace map failed to suppress PVCs but gave a slight change in the QRS morphology of the PVCs characterized by S waves in lead V6 (PVC 2, Figure 1B). VT with this altered QRS morphology was induced by programmed stimulation (VT 1, Figure 1B). Pacing in the distal great cardiac vein (GCV) reproduced a different QRS morphology (Figure 1D). During PVC 2, the earliest ventricular activation was observed at the aorto-mitral continuity (AMC) where pacing reproduced a perfect pace map (Figure 1B). However, nonirrigated RF applications at this site did not prevent the induction of multiple morphologies of VT with programmed stimulation (Figure 1). Those VT morphologies exhibited a fair match to the pace maps from the Figure 1. Twelve-lead electrocardiograms of VTs, PVCs, and pace maps (PMs), and a 3-dimensional computed tomography image showing the presumed ventricular arrhythmia origin (star), preferential conduction (dotted arrows), and exits identified by pace mapping. Ao indicates aorta; GCV, great cardiac vein; LA, left atrium; LCC, left coronary cusp; LV, left ventricle; RCC, right coronary cusp; and RVOT, right ventricular outflow tract. From the Division of Cardiovascular Disease, University of Alabama at Birmingham, Birmingham, Ala. Correspondence to Takumi Yamada, MD, PhD, Division of Cardiovascular Disease, University of Alabama at Birmingham, VH B147, 1670 University Boulevard, 1530 3rd Ave S, Birmingham, AL 35294-0019. E-mail [email protected] (Circ Arrhythmia Electrophysiol. 2008;1:140 –142.) © 2008 American Heart Association, Inc. Circ Arrhythmia Electrophysiol is available at http://circep.ahajournals.org 140 DOI: 10.1161/CIRCEP.108.778563 Yamada et al LVOT VT With Preferential Conduction and Multiple Exits 141 Downloaded from http://circep.ahajournals.org/ by guest on May 14, 2017 Figure 2. Cardiac tracings showing the spontaneous gradual conversions between the 2 VTs exhibiting a fair match to the pace map in the GCV and RCC. The first and second beats are fusion beats and the third and fourth and fifth to ninth beats are VTs exhibiting a fair match to the pace map in the GCV and RCC, respectively. Note that the ventricular activation in the His bundle (HB) region preceded the QRS onset during only the VT exhibiting a fair match to the pace map in the RCC and fusion beats of the 2 VTs. Xd,p indicates the distal and proximal electrode pairs of the X catheter. The other abbreviations are as in the previous figures. LVOT might have exhibited multiple VAs. No anatomic specificities other than an intramural origin were suggested because the QRS morphologies of all the VAs and their relevant pace maps were consistent with those of previous reports.2– 4 Although all the exits were located in close proximity, the directions from the origin varied between rightward and leftward and between endocardial and epicardial. This case suggests that preferential conduction to multiple exits may occur anywhere in the LVOT. That property of preferential conduction in the LVOT may cause VAs with LVOT origins to exhibit variable ECG features and limit the accuracy of ECG algorithms to predict the site of a VA origin. Disclosures Dr Yamada is supported by a research grant from Boston Scientific and St. Jude Medical. Drs McElderry and Kay have participated in catheter research funded by Biosense-Webster and Irvine Biomedical. Dr Kay has received honoraria from Medtronic, Boston Scientific, and St. Jude Medical. The electrophysiology fellowship program at the University of Alabama at Birmingham receives funding support from Boston Scientific and Medtronic. Dr Platonov reports no conflicts. References 1. Yamada T, Murakami Y, Yoshida N, Okada T, Shimizu T, Toyama J, Yoshida Y, Tsuboi N, Muto M, Inden Y, Hirai M, Murohara T, McElderry HT, Epstein AE, Plumb VJ, Kay GN. Preferential conduction across the ventricular outflow septum in ventricular arrhythmias originating from the aortic sinus cusp. J Am Coll Cardiol. 2007; 50:884 – 891. 2. Ito S, Tada H, Naito S, Kurosaki K, Ueda M, Hoshizaki H, Miyamori I, Oshima S, Taniguchi K, Nogami A. Development and validation of an ECG algorithm for identifying the optimal ablation site for idiopathic ventricular outflow tract tachycardia. J Cardiovasc Electrophysiol. 2003; 14:1280 –1286. 3. Dixit S, Gerstenfeld EP, Lin D, Callans DJ, Hsia HH, Nayak HM, Zado E, Marchlinski FE. Identification of distinct electrocardiographic patterns from the basal left ventricle: distinguishing medial and lateral sites of origin in patients with idiopathic ventricular tachycardia. Heart Rhythm. 2005;2:485– 491. 4. Yamada T, McElderry HT, Doppalapudi H, Kay GN. Catheter ablation of ventricular arrhythmias originating from the vicinity of the His bundle: significance of mapping of the aortic sinus cusp. Heart Rhythm. 2008;5:37– 42. 142 Circ Arrhythmia Electrophysiol June 2008 Downloaded from http://circep.ahajournals.org/ by guest on May 14, 2017 Figure 3. Successful ablation site. ABL indicates ablation catheter; LAO, left anterior oblique view; RAO, right anterior oblique view; RV, right ventricular catheter; and V-QRS, the local ventricular activation time relative to the QRS onset. The other abbreviations are as in the previous figures. Left Ventricular Outflow Tract Tachycardia With Preferential Conduction and Multiple Exits Takumi Yamada, Michael Platonov, H. Thomas McElderry and G. Neal Kay Downloaded from http://circep.ahajournals.org/ by guest on May 14, 2017 Circ Arrhythm Electrophysiol. 2008;1:140-142 doi: 10.1161/CIRCEP.108.778563 Circulation: Arrhythmia and Electrophysiology is published by the American Heart Association, 7272 Greenville Avenue, Dallas, TX 75231 Copyright © 2008 American Heart Association, Inc. All rights reserved. Print ISSN: 1941-3149. Online ISSN: 1941-3084 The online version of this article, along with updated information and services, is located on the World Wide Web at: http://circep.ahajournals.org/content/1/2/140 Permissions: Requests for permissions to reproduce figures, tables, or portions of articles originally published in Circulation: Arrhythmia and Electrophysiology can be obtained via RightsLink, a service of the Copyright Clearance Center, not the Editorial Office. Once the online version of the published article for which permission is being requested is located, click Request Permissions in the middle column of the Web page under Services. Further information about this process is available in the Permissions and Rights Question and Answer document. Reprints: Information about reprints can be found online at: http://www.lww.com/reprints Subscriptions: Information about subscribing to Circulation: Arrhythmia and Electrophysiology is online at: http://circep.ahajournals.org//subscriptions/