* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Respiratory System Infections
Survey
Document related concepts
Transmission (medicine) wikipedia , lookup
Neglected tropical diseases wikipedia , lookup
Human microbiota wikipedia , lookup
Globalization and disease wikipedia , lookup
Staphylococcus aureus wikipedia , lookup
Typhoid fever wikipedia , lookup
Gastroenteritis wikipedia , lookup
Anaerobic infection wikipedia , lookup
Triclocarban wikipedia , lookup
Traveler's diarrhea wikipedia , lookup
Clostridium difficile infection wikipedia , lookup
Schistosomiasis wikipedia , lookup
Marburg virus disease wikipedia , lookup
Urinary tract infection wikipedia , lookup
Infection control wikipedia , lookup
Neonatal infection wikipedia , lookup
Transcript
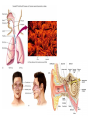
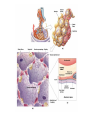
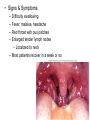
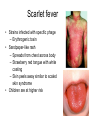
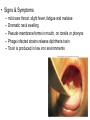
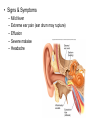
Respiratory System Infections Chapter 22 Respiratory System • Most common entry point for infections • Upper tract – Mouth, nasal cavity, sinuses, pharynx • Lower tract – epiglottis, larynx, trachea, bronchi, bronchioles and lung tissue Protection • • • • • Nasal hair Tonsils (adenoids) Mucus Ciliated mucus membrane Involuntary responses (coughing, etc.) • Alveolar macrophages Normal flora • Limited to the upper tract • Mostly Gram positive – S. aureus, alpha and non-hemolytic streptococci, diptheriods, Haemophilus influenzae and Moraxella catarrhalis Streptococcal Pharyngitis • Strep throat • Causative agent – Streptococcus pyogenes • Β-hemolytic group A streptococcus • Signs & Symptoms – – – – Difficulty swallowing Fever, malaise, headache Red throat with pus patches Enlarged tender lymph nodes • Localized to neck – Most patients recover in a week or so • Complications of infection can occur during acute illness • Laryngitis • Bronchitis • Scarlet fever (Scarlatina) Scarlet fever • Strains infected with specific phage – Erythrogenic toxin • Sandpaper-like rash – Spreads from chest across body – Strawberry red tongue with white coating – Skin peels away similar to scaled skin syndrome • Children are at higher risk • Complications that can develop later • Rheumatic fever • Glomerulonephritis • Necrotizing fasciitis Rheumatic fever • M protein in cell wall allows pathogen to persist • Autoimmune response – Antibodies cross react with heart cell antigens • Damage heart valves (endocarditis) and muscle • Arthritis, nodules over bony surfaces under skin Glomerulonephritis • Body fails to remove antigen-antibody complexes – Accumulate in glomeruli of the kidneys – Triggers inflammation obstructing blood flow – High blood pressure and low urine output • Irreversible kidney damage possible • Epidemiology (of Strep throat) – – – – Humans only host Spread by respiratory droplets Sore throats (with fever) should be cultured Beta hemolysis and serotype determination should be made for streptococci – Peak incidence occurs in winter or spring • Highest in grade school children • Prevention – No vaccine available – Adequate ventilation – Avoid crowds • Treatment – Penicillin, erythromycin or cephalosporin Diphtheria • Causative agent – Corynebacterium diphtheria – Gram variable – Pleomorphic – Non-spore forming – Metachromatic granules • Signs & Symptoms – – – – – mild sore throat, slight fever, fatigue and malaise Dramatic neck swelling Pseudo-membrane forms in mouth, on tonsils or pharynx Phage infected strains release diphtheria toxin Toxin is produced in low iron environments • Not very invasive bacteria • Exotoxin released into bloodstream – Results in damage to heart, nerves and kidneys • Very potent toxin – Small amount inactivates large population of cells which explains potency – Even with treatment 1 in 10 patents die • Epidemiology – Humans primary reservoir – Spread through direct/droplet contact transmission – Reservoir of infection include • Recovered and asymptomatic carriers • People with active disease – Diagnosed by immunoassay to detect circulating toxins • Prevention – Immunization • DTaP – Immunity not lifelong • Booster should be given every 10 years • Treatment – Open blocked airways – Antitoxin must be given early • No effect on absorbed toxin – Penicillin and erythromycin to eliminate bacteria Sinusitis and Otitis Media • Bacterial infection – Streptococcus pneumoniae; Haemophilus influenza; Moraxella catarrhalis; Staphylococcus aureus • Viral infections • Non-infectious allergies are the cause of many sinus infections • Signs & Symptoms – – – – – Mild fever Extreme ear pain (ear drum may rupture) Effusion Severe malaise Headache • Epidemiology – Begins with infection of nasopharynx – Spreads upward to sinuses or up Eustachian tubes • Sinusitis occurs in more in adults • Otitis Media occurs more often in children – Predisposing factors • damage to the ciliated mucus membrane • Prevention and treatment • No proven prevention for sinusitis • Prevention of otitis media involves influenza and pneumococcal vaccines • Tubes installed to avoid recurrent infections • Antibiotics for established bacterial cause – Penicillin like Amoxicillin Common Cold • Rhinitis • Causative agent – 30% to 50% caused by rhinovirus • More than 100 types of rhinovirus • Member of picornavirus family • Signs & Symptoms – Malaise, scratchy mild sore throat, runny nose – Cough and hoarsness (laryngitis) – Nasal secretion • Initially profuse and watery • Later, thick and purulent • No fever – Injured cells produce inflammation which stimulates profuse nasal secretion, sneezing and tissue swelling – Infection halted by inflammation, interferon release and immune response • Increased risk for secondary bacterial infections! • Epidemiology – Humans are only reservoir – Aerosols, fomites, direct contact transmission • Close contact with infected person or secretions necessary – No proven relationship between exposure to cold temperature and disease • Prevention – – – – No vaccine Hand washing Keep hands away from face Avoid crowds during times when colds are prevalent • Treatment – Certain antiviral medications showing promise • Pleconaril • Must be taken at first onset of symptoms