* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Slide 1
Childhood immunizations in the United States wikipedia , lookup
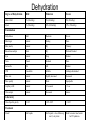
Marburg virus disease wikipedia , lookup
Rheumatic fever wikipedia , lookup
Hepatitis B wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Infection control wikipedia , lookup
Traveler's diarrhea wikipedia , lookup
Schistosomiasis wikipedia , lookup
Urinary tract infection wikipedia , lookup
Common cold wikipedia , lookup
Coccidioidomycosis wikipedia , lookup
Neonatal infection wikipedia , lookup
Gastroenteritis wikipedia , lookup
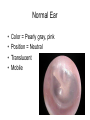
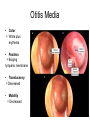
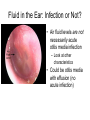
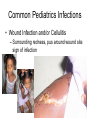
PEDIATRIC ISSUES IN ILAC Stephen F. Darrow, MD Chief Resident Internal Medicine-Pediatrics June 3, 2008 Pearls for the Campo • Most babies born in the DR are born in a hospital • There is a national vaccination program, so most kids have received their vaccines. • Parents want to make sure that their child is growing well and is healthy. Pearls for the Campo • Make sure you know (or have a chart with normal vital signs by age) • Every child should have a weight recorded (including kilograms) and percentile – Necessary for medication dosing and to assess growth • Be aware of whether your patient is able to swallow pills (your liquid medication options will be limited) Pediatric Fever • Fever is defined as temperature above 100.4 F or 38 C • You will have to rely on oral or axillary temperatures in the campo, which are frequently lower than the patient’s core body temperature. Pediatric Fever • Any febrile infant less than one month old should be transported to the nearest medical facility. – This child will require further evaluation including blood and urine cultures, lumbar puncture, and IV antibiotics Pediatric Fever • In children older than one month age, use your history and physical to assess for localizing signs. • Remember to look in the ears. • Examine the skin for abscess/ cellulitis. • If the child is toilet trained, collect urine for urinalysis. Pediatric Fever • Assess the child for signs of toxicity: – Lethargy – Signs of shock: • tachycardia, poor perfusion – Severe dehydration – Nuchal rigidity • Any infant who appears toxic should be transported to the nearest medical facility for further workup and IV antibiotics. Common Pediatrics Infections • Otitis media – – – – – Strep pneumonia, H. influenzae, M. catarrhalis Amoxicillin 80-90 mg/kg/day div bid or tid Cefuroxime 30 mg/kg/day div bid Azithromycin 10 mg/kg x 1 then 5 mg/kg/day x 4 days Treat for 10 days • Pharyngitis – Same as for otitis media. Treat for 10-14 days. • Thrush – Gentian violet/ nystatin (okay in infants) Normal Ear • • • • Color = Pearly gray, pink Position = Neutral Translucent Mobile Otitis Media • Color = White plus erythema • Position = Bulging tympanic membrane • Translucency = Decreased • Mobility = Decreased Fluid in the Ear: Infection or Not? • Air fluid levels are not necessarily acute otitis media infection – Look at other characteristics • Could be otitis media with effusion (no acute infection) Common Pediatrics Infections • Wound Infection and/or Cellulitis – Surrounding redness, pus around wound site sign of infection Common Pediatrics Infections • Cellulitis – Group A Strep, Staph aureus • Cephalexin 50-75 mg/kg/day div tid • Cloxacillin 50 mg/kg/day div qid • Clindamycin 10-30 mg/kg/day div tid or qid (side effect diarrhea) • TMP/SMX 8 mg/kg/day (TMP component) div bid (Stevens-Johnson side effect – consider using this if running low on above meds) Common Pediatrics Infections: Urinary Tract Infections • Organisms: E. Coli, Proteus • Lab + Nitrites, + leukocytes on urine analysis • Treatment: – TMP/SMX 8 mg/kg/day (TMP component) div bid – Cefixime 8 mg/kg q day – Treat for 7-10 days “Parasites” • Most GI complaints are attributed to parasites. • Parents are almost always concerned that their children do not eat enough and that this may be due to a parasite. • If you treat everyone who thinks they have a parasite, you will run out of medicine! “Parasites” • Evaluate for any signs of infection: – Abdominal pain – Chronic diarrhea – Poor Growth • If you treat one patient, treat the whole family. “Grippe” • “Grippe” encompasses all upper respiratory symptoms • Differential diagnosis includes – Allergies – Upper respiratory infection – Sinusitis • Cold medications are generally not recommended in children due to poor efficacy. “Grippe” • Treat for allergies if associated with itching, sneezing, or atopic sequelae on exam (pale mucosa, allergic shiners) • Treat for sinusitis if associated with headache or sinus pain, fever, or prolonged course • Remember to look for foreign body! Cough • Cough may be a symptom of a mild URI or may indicate a more serious problem. • Think asthma if associated with wheezing or shortness of breath or if it is worse at night. – There is often a history of eczema or allergies in the patient, or a family history of asthma or allergies. Cough • Think pneumonia if associated with fever or with signs of consolidation on exam (dullness to percussion) • Think TB if cough is chronic and if other family members have a chronic cough. Dehydration Degree of Dehydration Mild Moderate Severe Older Child 3% (30 ml/kg) 6% (60 ml/kg) 9% (90 ml/kg) Infant 5% (50 ml/kg) 10% (100 ml/kg) 15% (150 ml/kg) Dehydration Mild Moderate Severe Skin turgor Normal Tenting None Skin (touch) Normal Dry Clammy Buccal mucosa/lips Moist Dry Parched/Cracked Eyes Normal Deep Sunken Tears Present Reduced None Fontanelle Flat Soft Sunken CNS Consolable Irritable Lethargic/obutunded Pulse rate Normal Slightly increased Increased Pulse quality Normal Weak Impalpable Capillary refill Normal 2-3 seconds > 3 sec Urine output Normal Decreased Anuric <1.015 1.015-1.025 > 1.025 Oral liquids Oral liquids + close follow up next ½ day clinic Refer to nearest med center for IV hydration. Examination Laboratory Urine Specific gravity Treatment Fluids! Dehydration • Mild- Moderate Dehydration can be treated with oral rehydration therapy • Pedialyte or WHO oral rehydration solution • Administer small volumes (5-10 ml at a time) • Replace deficit over 4 hours • Replace ongoing losses Infestations • Scabies – Linear burrows around: • wrists, ankles, finger and toe webs, groin, waist – In infants and toddlers: head, neck, trunk, palms and soles are affected – Very pruritic Infestations • Scabies – Permethrin 5% cream or lindane lotion – Apply to entire body below neck and leave on overnight; bathe in am – Treat entire household – Wash all clothing and linen Infestations • Head Lice – Pediculosis humanus capitis – Acquired by close physical contact, sharing hats/ brushes – Nits are oval, white 0.5 mm dots stuck on hair shafts 1-3 cm from scalp. Found especially above and behind ears. – Lice are six legged insects visible to the unaided eye. Infestations • Head Lice – Pruritis is the principle symptom – Occipital adenopathy is common – Lindane shampoo; leave on scalp for five minutes before rinsing, then comb hair with a fine-tooth comb. Repeat in 7 days. • Use Permethrin 5% cream in infants – Treat entire household – Wash all bedding, clothing, hats Asthma: Emergency Treatment • • • • • Assess ABC’s Oxygen as needed Inhaled beta-agonist Ipratropium bromide Corticosteroids, po or IM (2 mg/kg load, then 1 mg/kg bid) • Epinephrine SC, 0.01 ml/kg • Terbutaline SC, 0.01 ml/kg Asthma Attack • Retractions (indentation of chest) • Accessory muscle use (neck muscles to breathe) • Nasal flaring High Blood Pressure • Coarctation of the aorta can lead to high blood pressure • Avoid ACE inhibitors in pubescent teenagers Take Home Points • Common Things Are Common – Colds – Stomach Pain • Parasites • Constipation – Ear infections – Skin infections – Scabies/ Lice