* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download IschemicaHy Mediated Sustained Monomorphic Ventricular
Survey
Document related concepts
Remote ischemic conditioning wikipedia , lookup
Drug-eluting stent wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Electrocardiography wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Cardiac surgery wikipedia , lookup
History of invasive and interventional cardiology wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Coronary artery disease wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Ventricular fibrillation wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Transcript
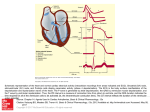
IschemicaHy Mediated Sustained Monomorphic Ventricular Tachycardia* Resolution With Antiischemic Therapy Robert W Thters; Gregory M.D.; A. Buser, HyunJoseph M.D.; Kim, and Michael CASE A 51-year-old was admission, he He began receiving developed M.D., underwent resistant to sinus Ph.D. a patient with ischemically mediated sustained ventricular tachycardia occurring at rest and to treatment with intravenously administered procainamide. plasty was transluminal Percutaneous successful, initially coronary but rest angina ular tachycardia, curred 2 weeks resistant later and isehemic medication ventricular therapy. We suggest be of benefit in patients cardial M medical may arrhythmias rhythm tained (Chest is an important of ventricular death. with by precipitated ischemia genesis diac responded However, ventricular nonfatal tachycardia myo- 1993; 104:1613-14) factor in the and sudden car- ischemically mediated unusual. susSeveral studies have examined the effects of myocardial revascularand anti-ischemic pharmacologic therapy upon exercise-induced ventricular arrhythmias.’ Relatively litfie is known, however, about the effects of these interventions upon ischemically mediated ventricular arrhythmias unassociated with exercise. ization *Fmm the Division of Cardiology, Department of Medicine, Administration Medical Center, School of Medicine, Baltimore. Baltimore Veterans versity ofMaryland the and the Uni- .1’- FIGURE beats and a patent anterior descending left circumflex marginal was left internal coronary coronary branches coronary artery 1. An ECC showing the six limb leads during per minute. The paper speed is 100 mm/s. artery graft poor distal was occluded, diseased. The occluded, and there and then intravenously. Coronary with artery had to the 1). He converted administered mammary diffusely was discomfort to surgery. and admission (Fig begun. artery were dinitrate After disease prior bypass artery tachycardia then artery months isosorbide procainamidewas infusion arteriography to the left runoff. The and the obtuse graft to the distal was a filling defect, presumably thrombus, occluding the origin of the large posterior descending artery Left ventriculography revealed overall normal left ventricular function. Subsequently, the patient experienced intermittent chest discomfort followed by long runs of seif-terminating ventricular tachycardia. There was no clear relationship between resting of flow. The rate heart and artery artery coronary arrhythmia the onset gradually of the at the angioplasty resulted subsided, arrhythmia. origin of the in some resolution and procainamide therapy was discontinued. Electrophysiologic study, in the drugfree state, revealed no inducible arrhythmias during programmed stimulation using up to three extrastimuli at two right ventricular sites and two paced cycle lengths. Thallium exercise stress test showed small fixed defects inferiorly and apically, but no reversible defects. Ten days later, the patient’s rest angina recurred, followed by sustained ventricular tachycardia with morphologic findings iden- to the original tachycardia. Therapy with intravenously adminprocainamide was reinstituted, and because he was a poor interventional candidate, the dosage of metoprolol was increased to 150 mg twice a day and therapy with diltiazem to 360 mg daily, was added. After resolution of the arrhythmia, treatment was switched to the oral form of procainamide, and a repeat electrotical istered I . Five coronary ventricular Percutaneous coronary posterior descending trigger arrhythmias is relatively malignant spontaneous 2-vessel when revealed right ventric- therapy, reto aggressive antithat anti-isehemic to procainamide isehemia. yocardial angio- and coronary angina. metoprolol sustained A maintenance We describe monomorphic atherosclerotic with for crescendo hospitalized done well until 3 weeks prior to admission. coronary care unit, he experienced chest M.D.; R. Gold, man REPORT -t-1SS---- an episode : ,14 ofventricular tachycardia CHEST Downloaded From: http://publications.chestnet.org/pdfaccess.ashx?url=/data/journals/chest/21677/ on 05/12/2017 at a rate V of 180 I 104 I 5 I NOVEMBER, 1993 1613 physiologic study exercise from stress again showed no test was unchanged, inducible arrhythmias. and the patient The was discharged the hospital. The patient was readmitted 6 weeks later because of presumed procainamide-induced lupus. Procainamide therapy was discontinued, but he developed a life-threatening lower gastrointestinal hemorrhage, necessitating emergency transverse colectomy. He experienced no anginal symptoms during this period, and no ventricular arrhythmias were observed. After uneventful recovery, he has remained asymptomatic with no further ventricular tachycardia over a 9-month period while receiving treatment with metoprolol, diltiazem, and isosorbide dinitrate. DISCusSIoN There tachycardia First, are several factors seen in our patient it was always suggesting that was ischemically preceded by typical ventricular mediated. anginal symptoms. Although ischemic symptoms were not preceded by obvious tachycardia, we cannot exclude minor fluctuations in heart rate and blood pressure as trigger factors. Alternatively, spontaneous alterations have been cardia in patients with while was relatively setting of life-threatening though ischemically curring at rest preserved favorable mic not. than is unusual, be left ventricular outcome. While re- has Al- with oc- onstrate are common that patient’s cardiac the beneficial role of beta It has become a common this death has has practice in not are DA, Levine bypass SR. exercise surgery Klein testing: and MD, Ryan TJ. Ventricular mechanism, prognostic response arrhyth- Am J Cardiol RJ Jr. Gettes LS. Reproducibility and treatment JR. Simpson of exercise-induced ventricular 5 The and CAST Investigators suppression tachycardia. Am J on after preliminary mortality report: Effect of encaimide in a randomized trial of arrhythmia myocardial infarction. N Engl J Med its efficacy present Heart of propranolol results. Attack in patients JAMA Trial Research with 1982; acute 247:1707-14 Group. A randomized myocardial 104:1614-16) infarction. refractory ablation effective of accessory in the treatment syndrome. in eliminating period Recent accessory pathways of patients series dem- pathways and two in cases which intravenous adenosine ‘concath- REPORTS 1 energy (55 disappearing V) was delivered the first for a total of 2 s. There after 27 was s no evidence for accessory pathway conduction during ventricular or atrial pacing after 30 mlii. Adenosine (12 mg) intravenously demonstrated transient ventricular preexcitation (Fig 1, top). Further radiofrequency energy was delivered to the site and again preexcitation disappeared. After 30 mm, adenosine was repeated, producbog transient complete atrioventricular (AV) block. The patient’s ECG remains free ofpreexcitation 5 months after the procedure. 2 A 41-year.old historyofatrial 6 B-Blocker 1993; revealed persistent accessory pathway duction following presumed successful radiofrequency eter ablation. CASE 1989; 321:406-12 Mortality highly with preexcitation 1984; flecainide im- ms 1984; 53:751-56 3 Lehrman KL, lilkian AG, Hultgren HN, Fowles RE. Effect of coronary arterial bypass surgery on exercise-induced ventricular arrhythmias. Am J Cardiol 1979; 44:1056-61 4 Josephson ME, Horowitz LN, Farhidi A, Kastor JA. Recurrent sustained ventricular tachycardia. Circulation 1978; 57:431-40 Cardiol catheter been Radiofrequency A, Foster may A 49-year.old man had atrial fibrillation and cardiac arrest. An ECG showed ventricular preexcitation. The pathway was mapped to the lateral mitral annulus. The anterograde effective refractory period (ERP) was 200 ms and the retrograde ERP was less than 220 to coronary significance. ERPeffective CASE 53:1553-57 2 Woolfel Adenosine administration CASE REFERENCES during M.D. (Chest WolflParlanson-White We to inducible in the electrophysiology laboratory. Our experience suggests that aggressive anti-ischemic therapy may be ofbenefit in some of these individuals. mias M.D.; thereby sparing patients the need for life-long drug therapy or cardiac surgery.’ Unfortunately, accessory pathway conduction may recur days to months after apparently successful ablation. Many of these failures may be due to modification ofaccessory pathway conduction that leaves the tissue viable but transiently unable to conduct.’ well- blockers automatic implantable cardioverter-defibrillators with sustained ventricular arrhythmias that 1 Weiner Jack Krvn, of radiofrequency catheter by manifesting latent acces- conduction. adiofrequency tachycardia our of sudden therapy. efficacy pathways I AVatrioventricular; in the function played a role in his the experience with antiarrhyth- prevention ablative long-term of accessory pathway hemorrhage. suggesting Perhaps M.D.; H. McAnulty, and Blair D. Halperin, of further the 5017 of but even symptoms death, fatal. John M.D.; Silka, ablation may M.D.; Radiofrequency catheter ablation is very effective in eliminating conduction over accessory pathways in patients with Wolff-Parkinson-White syndrome. However, accessory pathway conduction recurs in approximately 5 to 9 percent of patients in the weeks to months following ablation. We describe two cases in which intravenous adenosine revealed persistent accessory pathway conduction after apparently successful ablation, thus providing an indication for the prove arrhythmia drugs ventricular cardiac may in the the therapy, ischemic Michaelj delivery tachy- 90 percent Third, gastrointestinal mediated disappointing,’ well established.6 insert patients in greater W Walker, Kirk is inducible to anti-arrhythmic to sudden drugs been been disease to anti-ischemic frequently tone ventricular heart it was resistant dramatically entity ischemic patient sponded vasomotor sustained stimulation in our antecedents coronary Second, with programmed cases,4 in responsible. Unmasking Accessory Pathway Conduction wfth Adenosineinduced Atrioventricular Nodal Block After Radlofrequency Catheter Ablation* man fibrillation had WolflParhinson-White with rapid accessory syndrome and pathway conduction. a trial I. *From sity, the Division ofCar&ologc Oregon Health Sciences Univer- Portland. 1614 Downloaded From: http://publications.chestnet.org/pdfaccess.ashx?url=/data/journals/chest/21677/ on 05/12/2017 Adenosine-Iriduced AV Nodal Block (b%Wker et a!)