* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Respiratory System (Power Point Document)
Survey
Document related concepts
Pre-Bötzinger complex wikipedia , lookup
Cushing reflex wikipedia , lookup
Freediving blackout wikipedia , lookup
Intracranial pressure wikipedia , lookup
Cardiac output wikipedia , lookup
Hemodynamics wikipedia , lookup
High-altitude adaptation in humans wikipedia , lookup
Homeostasis wikipedia , lookup
Acute respiratory distress syndrome wikipedia , lookup
Biofluid dynamics wikipedia , lookup
Haemodynamic response wikipedia , lookup
Alveolar macrophage wikipedia , lookup
Organisms at high altitude wikipedia , lookup
Circulatory system wikipedia , lookup
Transcript
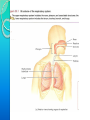
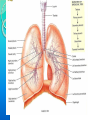
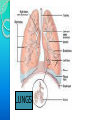
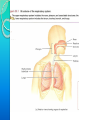
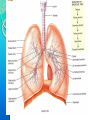
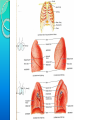
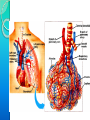
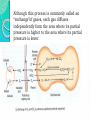
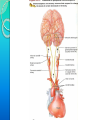
RESPIRATORY SYSTEM RESPIRATORY SYSTEM LUNGS CONTENTS:Introduction,general organisation Structures of respiratory system Mechanics of respiration, compliance Lung volumes and capacities Pulmonary and alveolar ventilation Physical principles of gaseous exchange Transport of respiratory gases Control of respiration Pulmonary function tests. INTRODUCTION Respiratory system constitutes one of the important system as it contributes the vital provision of supply of oxygen to the body, where cells continuously use oxygen for metabolic reactions which in turn releases energy. This energy is from the nutrient molecules which provide ATP. DEFINITION:- Respiration is the process by which oxygen from the lungs is carried by the blood to the tissues and carbon dioxide formed in the tissues by metabolic activity is carried by the blood to the lungs and is expired out The PROCESS OF RESPIRATION involves four stages:VENTILATION:-Ventilation means the passage of air in and out of lungs during Inspiration and expiration respectively . INTRAPULMONARY GAS MIXING:Intrapulmonary gas mixing or distribution of oxygen rich inspired air with the air already present in the lungs. DIFFUSION:- Diffusion which means gas transfer across the alveolar capillary membrane due to tension gradient. PERFUSION:- Perfusion means flow of adequate quantity of blood through the lungs so that the diffused gases are carried away. FUNCTIONS OF RESPIRATION •GAS TRANSFER: Transfer of O2 from the alveoli to the venous blood and CO2 in the opposite direction. •REGULATION OF pCO2 OF BLOOD: The most important function of respiration is to keep the arterial pCO2 at 40 mmHg which is essential for many vital functions of the body. •REGULATION OF PH OF BLOOD: By the reversible reaction, it maintains the pH of blood H2CO3 H+ + HCO3- •EXCRETION OF CERTAIN VOLATILE GASES: For example- chloroform, ether, ammonia, etc. •PUMPING ACTION: The rhythmic movement of the diaphragm and the chest wall causes rhythmic alteration of pressure in the abdomen and chest cavity. This assists in drawing blood from the lower part of the body to the abdomen and then to chest and thus helps in maintaining venous inflow to the heart. RESPIRATORY TRACT The whole respiratory tract is divided in two parts :•UPPER RESPIRATORY TRACTIt extends from the nasal cavity to the vocal cords i.e. (nose, pharynx and associated structures) •LOWER RESPIRATORY TRACTIt extends from the vocal cord to the alveoli i.e (larynx, trachea, bronchi, lungs.) STRUCTURES OF THE RESPIRATORY TRACT CONTENTS•Nose • Pharynx • Larynx • Trachea • Bronchi •Lungs CONTENTS •POSITION AND STRUCTURE •LINING OF THE NOSE •FUNCTIONS OF THE NOSE(A) RESPIRATORY FUNCTIONS OF THE NOSE (B) OLFACTORY FUNCTIONS OF THE NOSE I. POSITION AND STRUCTURE :The nasal cavity is the main route of air entry , and consists of a large irregular cavity divided in to two equal passages by a septum . The posterior bony part of the septum is formed by the perpendicular plate of the ethmoid bone and vomer. Anteriorly, it consists of hyaline cartilage . II. LINING OF THE NOSE :The nose is lined with very vascular ciliated columnar epithelium which contains mucus secreting goblet cells. At the anterior nares this blends with the skin and posterioly it extends in to the nasal part of the pharynx. •FUNCTIONS OF THE NOSE (A) RESPIRATORY FUNCTONS OF THE NOSE:1) WARMING:- This is due to the immense vascularity of the mucosa. This explains the large blood loss when a nosebleed occurs . 2) FILTERING AND CLEANING :- This occurs as hairs at the anterior nares trap large particles. Smaller particales such as dust and microbes settle and adhere to the mucus. Mucus protects the underlying epithelium from irritation and prevents drying. Synchronous beating of the cilia wafts the mucus towards the throat where it is swallowed or coughed up. 3) HUMIDIFICATION:- As air travels over the moist mucosa , it becomes saturated with water vapour . irritation of the nasal mucosa results in sneezing, a reflex action that forcibly expels an irritant. IV) OLFACTORY FUNCTIONS OF THE NOSE :The nose is the organ of the sense of smell . Nerve endings that detect smell are located in the roof of the nose in the area of the cribriform plate of the ethmoid bones and the superior conchae. These nerve endings are stimulated by airborne odours. The resultant nerve impulses are conveyed by the olfactory nerves to the brain where the sensation of smell is perceived. CONTENTS:•POSITION OF PHARYNX •DIVISION OF PHARYNX •BLOOD AND NERVE SUPPLY •FUNCTIONS OF PHARYNX 1. POSITION OF PHARYNX:The pharynx is a tube 12 to14 cm long that extends from the base of the skull to the level of the 6th cervical vertebra.it lies behind the nose mouth and larynx and is wider at its upper end 2. DIVISION OF PHARYNX:(A)THE NASOPHARYNX :The nasal part of the pharynx lies behind the Nose Above the level of the soft palate (B) THE OROPHARYNX :The oral part of the pharynx lies behind the Mouth extending from below the level of the soft palate to the level of the upper part of the body of the third cervical vertebra (C) THE LARYNGOPHARYNX :The laryngeal part of the pharynx extends From the oropharynx above the continues as the oesophagus below from the level of the 3rd to the 6th cervical vertebrae . 3. BLOOD AND NERVE SUPPLY :Blood supply is by the facial artery . Nerve supply is by the PARASYMPATHETIC by the :- Vagus nerve and glosso pharyngeal nerve. SYMPATHETIC by the :- Superior cervical ganglia. 4. FUNCTIONS OF THE PHARYNX:I) WARMING AND HUMIDIFYING :- By the same methods as in the nose the air is further warmed and moistened as it passes through the pharynx. II) PASSAGE WAY FOR AIR AND FOOD:Air passes through the nasal And oral section and food Through the oral and laryngeal section. POSITION :- The larynx or voice box extends from the root of the tongue and the hyoid bone to the trachea. It lies infront of the laryngo pharynx at the Level of the 3rd,4th,5th and 6th cervical vertebra BLOOD AND NERVE SUPPLY :- BLOOD SUPPLY:- By the superior and inferior laryngeal arteries. NERVE SUPPLY :a) PARASYMPATHETICS :- By the superior laryngeal And recurrent Laryngeal nerves. b) SYMPATHETICS:-Superior cervical ganglia, FUNCTIONS : SPEECH:- This occurs during expiration when the sounds produced by the vocal cords are manipulated by the tongue,cheek and lips. PROTECTION OF THE LOWER RESPIRATORY TRACT:- During Deglutition the larynx move upwards occulding the opening in to it from the pharynx and the hinged epiglottis closes over the larynx this ensure that food passes in to the oesophagus and not into the lower respiratory tract. PASSAGEWAY FOR AIR:- This is between the pharynx and trachea HUMIDIFYING FILTERING AND WARMING :- This processes continue As inspired air travel Through the larynx. TRACHEA CONTENTS:POSITION STRUCTURE BLOOD AND NERVE SUPPLY FUNCTION POSITION:The trachea or wind pipe is a continuation of the larynx and Extends downwards to about the level of the 5th thoracic Vertebra. STRUCTURE :The trachea is a cartilaginous membranous tube about 10 or 11cm. long it is not quite cylindrical being flattened posteriorly. Its external diameter from side to side is about 2cm in the adult male and 1.5 in the adult female it is kept patent by incomplete C-shaped rings of cartilage on its anterio lateral wall which keeps air tubes open. BLOOD AND NERVE SUPPLY :BLOOD SUPPLY :-By the inferior thyroid and bronchial arteries. NERVE SUPPLY:a)PARASYMPATHETICS:-By the recurrent laryngeal nerve b)SYMPATHETICS:- By the ganglia FUNCTIONS: SUPPORT AND PATENCY :-trachea is kept patent by incomplete C-shaped ring Of cartilage on its antero tateral wall which keeps Air tube open. COUGH REFLEX :-Cough is protective reflex by means of which respiratory Passage are kept free form foreign matter. WARMING,HUMIDIFYING AND FILTERING :This continues as the nose, Although air is normally Saturated and at body temperature when it reaches the trachea. APPLIED PHYSIOLOGY:TRACHEOSTOMY AND INTUBATION Several condition may Block air flow by Obstructing the trachea FOR EXAMPLE :-The rings of cartilage that support the trachea may collapse due to a crushing injury to the chest inflammation of the mucous membrane may cause it to Swell so much that the airway closes or vomit or a foreign object may be aspirated. Methods are used to reestablish air flow past a tracheal obstruction if the obstruction is superior to the level of the larynx tracheostomy an operation to make an opening in to the trachea may be performed. BRONCHI CONTENTS:STRUCTURE BLOOD AND NERVE SUPPLY FUNCTIONS STRUCTURE :The bronchi is progressively subdivided in to bronchioles, Terminal bronchioles, respiratory bronchioles, albeolar ducts and finally alveoli. Situated from the superior border of the 5th thorasic vertebra divided in to a right primary bronchus which goes in to the right lungs and a left primary bronchus which goes in to the left lungs. BLOOD AND NERVE SUPPLY:BLOOD SUPPLY :- By the right & left Bronchial arteries NERVE SUPPLY :-PARASYMPATHETICS & SYMPATHETIC NERVE 3) FUNCTIONS :CONTROL OF AIR ENTRY :- The diameter of the respiratory passages is Altered by contraction and relaxation of the Involuntary muscles in their walls, thus regulating the volume of entering the Lungs. These changes are controlled by the autonomic nerve supply parasympathetics causes constriction and sympathetics stimulation dilatation . WARMING AND HUMIDIFYING SUPPORT AND PATENCY REMOVAL 0F PARTICULATE MATTER COUGH REFLEX. LUNGS CONTENTS: INTRODUCTION POSITION AND STRUCTURE COVERING OF LUNGS LOBES, FISSURES AND LOBULES ALVEOLI SURFACTANT RESPIRATORY MEMBRANE BLOOD SUPPLY NERVE SUPPLY APPLIED PHYSIOLOGY INTRODUCTION :- The lungs (=lightweights, because they float), are paired cone- shaped organs in the thoracic cavity. They are separated from each other by the heart and other structures in the mediastinum while thoracic Cavity & mediastinum form two different chambers for two lungs. POSITION AND STRUCTURE The lungs extend from the diaphragm to just slightly superior to the clavicles and lie against the ribs anteriorly and posteriorly. The broad inferior portion of the lung, the base, is concave and fits over the convex area of the diaphragm. The narrow superior portion of the lungs is the apex. The surface of the lungs lying against the ribs, called the costal surface, matches the rounded curvature of the ribs. Medially, the left lung also contains a concavity, the cardiac notch, in which the heart lies The mediastinal (medial) surface of each lung contains the region, the hilus, through which bronchi, pulmonary blood vessels, lymphatic vessels, and nerves enter and exit. These structures are held together by pleura and connective tissue and constitute the root of lung. Due to the space occupied by the heart, the left lung is about 10% smaller than the right lung. COVERING OF LUNGSTwo layers of serous membrane collectively called the pleural membrane, enclose and protect each lung. The superficial layer lines the wall of the thoracic cavity and is called the parietal pleura, the deep layer, the visceral pleura, covers the lungs themselves . Between the visceral and parietal pleurae is a small space, the pleural cavity. Pleural cavity contains a small amount of lubricating fluid secreted by the membranes. This fluid reduces friction between the membranes, allowing them to slide easily over one another during breathing. Pleural fluid also causes the two membranes to adhere to one another just as a film of water causes two slides to stick together , a phenomenon called surface tension. LOBES, FISSURES AND LOBULES:The right lung is divided into three lobes-superior, middle and inferior. The left lung is smaller and is divided into two lobes-superior and inferior. Each lung is divided into lobes by one or more fissures .Both the lungs have oblique fissures . Right lung also has horizontal fissure. The oblique fissure in the left lung separates the superior lobe from the inferior lobe Each lobe receives its own secondary (lobar)bronchus .Thus, the right primary bronchus gives rise to three secondary bronchi called the superior, middle and inferior secondary bronchi, whereas the left primary bronchus gives rise to superior and inferior secondary bronchi. Within the substance of lung, the secondary bronchi give rise to the tertiary bronchi. The segment of lung tissue that each tertiary bronchus supplies is called a “Broncho pulmonary segment” . ALVEOLI Around the circumference of the alveolar ducts are numerous alveoli and alveolar sacs. An alveolus is a cup-shaped outpouching lined by simple squamous epithelium and supported by a thin elastic basement membrane. An alveolar sac consists of two or more alveoli that share a common opening. The walls of alveoli contains two types of alveolar epithelial cells1.)Type I alveolar cells. 2.)Type II alveolar cells. The Type I alveolar cells, the predominant cells, are simple squamous epithelial cells that form a nearly continuous lining of the alveolar wall. The Type II alveolar cells, also called septal cells, are fewer in number and are found in between type I alveolar cells. FUNCTIONS OF ALVEOLAR CELLS:Type I alveolar cells are main sites of gaseous exchange. Type II alveolar cells, which are rounded or cuboidal epithelial cells whose free surfaces contain microvilli, secrete alveolar fluid, which keeps the surface between cells and air moist. Included in the alveolar fluid is SURFACTANT. Asssociated with alveolar walls are alveolar macrophages (dust cells), wandering phagocytes that remove the fine dust particles and other debris in the alveolar spaces. SURFACTANTDEFINATION- Any surface acting material or agent that is responsible for lowering surface tension of fluid is called surfactant. The surfactant present in the alveoli of lungs is called as pulmonary surfactant. It is a complex detergent like mixture of phospholipids and lipoproteins. It is secreted by Type II alveolar epithelial cells. FUNCTIONS OF SURFACTANTThey reduces surface tension in alveoli of lungs & prevents collapsing tendency of lungs. Surfactant is responsible for stabilization of alveoli which have tendency to deflate. It plays an important role in inflation of lungs during birth. RESPIRATORY MEMBRANEThe exchange of oxygen & carbon dioxide between the air spaces in the lungs and the blood capillaries takes place by diffusion across the alveolar and capillary walls, which together form the respiratory membrane. Extending from the alveolar airspace to blood plasma, the respiratory membrane consists of four layers:- 1) A Layer of Type I and Type II alveolar cells and associated alveolar macrophages that constitutes the alveolar wall. 2) An epithelial basement membrane underlying the alveolar wall. 3) A capillary basement membrane that is often fused to the epithelial basement membrane. 4) The endothelial cells of the capillary. BLOOD SUPPLY Blood is provided to the lungs by two sets of arteries. Deoxygenated blood passes through pulmonary trunk which divides into Left And Right pulmonary artery which enters the left & right lung respectively. Return of oxygenated blood to the heart occurs by way of the four pulmonary veins, which drain into the left atrium. Bronchial arteries, which branch from the aorta, delivers oxygenated blood to the lungs. APPLIED PHYSIOLOGY PLEURISY or PLEURITISInflammation of the pleural membrane is called pleurisy or pleuritis. In its early stages it may cause pain due to friction between the parietal and visceral layers of the pleura. If the inflammation persists, excess fluid accumulates in the pleural space, a condition known as PLEURAL EFFUSION. RESPIRATORY MOVEMENT INTRODUCTION During normal quiet breathing, inspiration is the active process and expiration is the passive process. During inspiration, thoracic cage enlarges and lungs expands. During expiration, the thoracic cage and lungs decrease in size and attain the preinspiratory position. MUSCLES OF RESPIRATION Respiratory muscles involved in inspiration are know as inspiratory muscles. And the muscle and the muscle involved in expiration are called expiratory muscles. However, the respiratory muscles are generally classified into primary (responsible for change in size of thoracic cage during normal quiet breathing) and accessory (are put into action during forced breathing) muscles. PRIMARY INSPIRATORY MUSCLES :Primary inspiratory muscles are diaphragm,which is supplied by phrenic nerve and external intercostal muscles, supplied by intercostal nerves. ACCESSORY INSPIRATORY MUSCLES :Sternomastoid, scaleni, anterior serrati, elevators of scapulae and pectorals are the accessory inspiration muscle. PRIMARY EXPIRATORY MUSCLES :Primary expiratory muscles are the internal intercostal muscles, which are innervated by intercostal nerves. ACCESSORY EXPIRATORY MUSCLES:Accessory expiratory muscles are the abdominal muscles. MOVEMENT OF THORACIC CAGE :Inspiration causes enlargement of thoracic cage. The size of the thoracic cage is increased in all diameters. Increase in anterioposterior and transverse diameters occurs due to elevation of ribs. The vertical diameter of thoracic cage is increased by the descent of diaphragm. In general the change in size of thoracic cavity occurs because of the movement of four units of structures. 1. Thracic lid 2. Upper costal series 3. Lower costal series 4. Diaphragm RESPIRATORY PRESSURES Two types of pressures are exerted in the thoracic cavity and the lungs during the process of respiration. 1. Intrapleural pressure Or intrathoracic pressure. 2. Intraalveolar pressure Or intrapulmonary pressure. INTRAPLEURAL PRESSURE or INTRATHORACIC PRESSURE DEFINITIONThe intrapleural pressure is the pressure existing in pleural cavity, that is in between the visceral and parietal layers of pleura. It is exerted by the suction of the fluid that lines the pleural cavity. NORMAL VALUES The respiratory pressures are always expressed in relation to atmospheric pressure which is 760 mm Hg. Intrapleural pressure is always negative. The normal values of the intrapleural pressure in quiet breathing are:During inspiration :-6 mm Hg. (760-6=754 mm Hg). During expiration :-2 mm Hg. (760-2=758 mm Hg). SIGNIFICANCE OF INTRAPLEURAL PRESSURE The intrapleural pressure has two important functions :A. Since the intrapleural pressure is always negative, it prevents the collapsing tendency of lungs, which is caused by elastic recoiling of lungs tissue . B. Because of the negative pressure in thoracic region, the larger veins and vena cava are enlarged, i.e. dilated. This acts like suction pump to pull venous blood from lower part of the body towards heart against gravity. Thus,the intrapleural pressure is responsible for venous return. So, it is called the respiratory pump for venous return. INTRAALVEOLAR PRESSURE OR INTRAPULMONARY PRESSURE DEFINATION :The pressure existing in the alveoli of the lungs is called the intraalveoloar pressure or intrapulmonary pressure. NORMAL VALUES Normally, intraalveolar pressure is equal to the atmospheric pressure, which is 760 mm Hg. During inspiration, it becomes negative. The value is -4 mm Hg (760-4= 756 mm Hg). During expiration, it becomes positive. The value is +4 mm Hg (760+4=764 mm Hg). SIGNIFICANCE OF INTRAALVEOLAR PRESSURE The significance of the intraalveolar pressure is: A. The pressure in alveoli causes flow of air in and out of alveoli. During inspiration, since the pressure in the alveoli is negative, the atmospheric air enters the alveoli, and as the intrathoracic pressure becomes positive during expiration, the air is expelled out of alveoli. B. The intraalveolar pressure also helps in the exchange of gases between the alveolar air and the blood. COMPLIANCE DEFINITION The ability of the lungs and thorax to expand or the expansibility of lungs and thorax is called the compliance. It is defined as the change in volume per unit change in the pressure. The compliance can be expressed in relation to intraalveolar pressure or intrapleural pressure. NORMAL VALUES Compliance is the volume increase in lungs per unit increase in the intraalveolar pressure. Compliance of lungs and thorax together =130 ml/1 cm H2O pressure. Compliance of lungs alone =220 ml/1 cm H2O Pressure. FACTOR AFFECTING COMPLIANCE The expansibility of thorax and the total compliance is reduced in the following condition: 1. Deformities of thorax like kyphosis and scoliosis. 2. Fibrotic pleurisy 3. Paralysis of respiratory muscles 4. Pleural effusion 5. Abnormal thorax MOTION OF THE RIBS: The ribs are almost semicircular bones which articulate with the vertebrae at one end with the sternum or costal cartilages at the other . 1. During inspiration, the sternum is elevated and pushed forwards due to the elevation of the shaft of the ribs, of which the sternal ends are lower than the vertebral end during expiration. This is caused due to the contraction of intercostal muscles and results in an increase in the anterioposterior diameter of the chest. 2. The rotation of the ribs around the two points of attachment on sternum & vertebra causes an increase in transverse diameter of the thorax. During expiration both intercostal muscles which are responsible for movement of the ribs and sternum relaxes, the size of the thorax decreases in anterio-posterior and in transverse diameter , the lungs volume consequently decreases. Lung volume are of four types: 1.Tidal volume. 2. Inspiratory reserve volume. 3. Expiratory reserve volume. 4. Residual volume. 1.TIDAL VOLUME (TV): It is the amount of air which passes into and out of the lungs during each cycle of quiet breathing. It is about 500 ml= 0.5 litres. 2.INSPIRATORY RESERVE VOLUME (IRV) : It is the maximum volume of air that can be inhaled into the lungs after normal tidal inspiration It is about 3300 ml= 3.3 litres. 3.EXPIRTORY RESRVE VOLUME (ERV): It is the largest volume of air which can be expelled from the lungs after normal expiration. It is about 1000 ml = 1 litre. 4.RESIDUAL VOLUME(RV): It cannot be directly measured but is the volume of air remaining in the lungs after forced expiration. It is about 1200 ml =1.2 litres. Two or more lung volumes are together called lung capacities . There are four lung capacities:1.Inspiratory capacities 2.Vital capacity 3.Functional residual capacity 4.Total lung capacity 1. INSPIRATORY CAPACITIES: It is the maximum volume of air that can be inspired from end expiratory position. Inspiratory capacity includes TV and IRV. IC = TV +IRV 2. VITAL CAPACITY(VC): It is the maximum amount of air that can be expelled out forcefully after a maximal inspiration. vital capacity includes IRV and TV and ERV VC =IRV +TV +ERV 3. FUNCTIONAL RESIDUAL CAPACITY (FRC): It is the volume of air remaining in the lungs after normal expiration . Functional residual capacity includes ERV and RV. FRC = ERV +RV 4. TOTAL LUNG CAPACITY(TLC): It Is the amount of air present in the lungs after a maximal inspiration .This includes all the volumes. TLC =IRV+ TV+ ERV +RV RESPIRATORY DEAD SPACE DEFINITION:The air which remains confined in the upper respiratory tract with each inspiration and is not available for gaseous interchange constitutes what is known as ‘DEAD SPACE’. Dead space is of two types:1. Anatomical dead space 2. Physiological dead space PULMONARY VENTILATION DEFINATION:Pulmonary ventilation is a cyclic process by which fresh air enters the lungs and an equal volume of air leaves the lungs. It is the volume of air moving in and out of lungs per minute in quiet breathing. It is also called respiratory minute volume. NORMAL VALUE AND CALCULATION NORMAL VALUE:Normal value of pulmonary ventilation is 6000 ml (6 litres/min) CALCULATION:Pulmonary ventilation is the product of the Tidal volume and rate of respiration. It is calculated by formula:PULMONARY VENTILATION =Tidal volume x respiratory rate =500 ml x12/min. =6000ml/min. ALVEOLAR VENTILATION DEFINITION:The alveolar ventilation is defined as the amount of air utilize for gaseous exchange every minute. The alveolar ventilation is different from pulmonary ventilation. It indicates only the volume of air that is utilized for gaseous exchange. Some amount of air trapped in dead space is not utilised for gaseous exchange. NORMAL VALUE AND CALCULATION:- NORMAL VALUE:-Normal value of alveolar ventilation is 4200ml/min. CALCULATION:- It is calculated by the formula given below:Alveolar ventilation =(Tidal volume-dead space volume) x Respiratory rate =(500-150)x12 =4200ml(4.2lit.)/min. DIFFUSION OF GASES Diffusion means movement of a substance from an area of high concentration to an area of low concentration. In the present context the diffusion of O2 from alveoli to pulmonary capillaries and of CO2 in the reverse direction is to be considered. The following points are to be noted in this connection: Gases in the alveoli are dissolved in small quantity of alvoelar fluid and are in equilibrium with partial pressure of the respective gases in alveolar air. Gases in the blood of pulmonary capillaries are also dissolved in water of the plasma where these exert a tension. EXTERNAL RESPIRATION:External respiration or pulmonary gas exchange is the diffusion of O2 from air in the alveoli of the lunga to blood in pulmonary capillaries and the diffusion of CO2 in the opposite direction. External respiration in the lungs converts deoxygenated blood (depleted of some O2) coming from the right side of the heart into oxygenated blood that returns to the left side of the heart. As blood flows through the pulmonary capillaries, it picks up O2 from alveolar air and unloads CO2 into alveolar air. Although this process is commonly called an “exchange”of gases, each gas diffuses independently form the area where its partial pressure is higher to the area where its partial pressure is lower. INTERNAL RESPIRATION : The left ventricle pumps oxygenated blood into the aorta and through the systemic arteries to systemic capillaries. The exchange of O2 and CO2 between systemic capillaries and tissue cells is called internal respiration or systemic gas exchange. As O2 leaves the blood stream, oxygenated blood is converted into deoxygenated blood. Unlike external respiration, which occurs only in the lungs, internal respiration occurs in tissues throughout the body. The rate of pulmonary and systemic gas exchange depends on several factors:1. Partial pressure difference of the gasesAlveolar Po2 mustbe higher than blood Po2, for oxygen to diffuse from alveolar into the blood. The rate of diffusion is faster when the difference between Po2 in alveolar air and pulmonary capillary blood is larger. 2.Surface area available for gas exchange- the surface area of alveoli is very huge. Any pulmonary disorder that decreases the functional surface area of the respiratory membrane decreases the rate of external respiration. 3.Diffusion distance- the respiratory membrane is very thin, so diffusion occurs very quickly. Also, the capillaries are so narrow that the red blood cells must pass through them in single file, which minimize the diffusion distance from an alveolar space to haemoglobin inside red blood cells. 4.Molecular weight and solubility of gasesbecause O2 has a lower molecular weight than CO2,it could be expected to diffuse across the respiratory membrane about 1.2 times faster. TRANSPORT OF OXYGEN Oxygen is transported by the blood from alveoli to the tissues. The volume of oxygen in arterial blood is 19 ml% and ,the partial pressure of oxygen is 95mm of Hg. In venous blood the volume of oxygen is 14ml% and partial pressure is 40mm of Hg. Oxygen is transported in blood in two forms:As simple physical solution. In combination with haemoglobin. Oxygen is dissloves in water of plasma and is transported in this physical form.The amount of oxygen transported in this way is very negligible.It is only 0.3ml per 100ml of plasma.It is about 3% of total oxygen in blood. Hb + O2 HbO2 Oxygen combines with haemoglobin in blood and is transported as oxyhaemoglobin.The transport of oxygen in this form is important because maximum amount(97%) of oxygen is transported by this method.Oxygen combines the iron in heme part of haemoglobin.Each molecules of haemoglobin contains 4 atoms of iron One gram of haemoglobin carries 1.34ml of oxygen.The normal haemoglobin content in blood is 15 gm%.So the blood with 15 gm% of Hb must carry 20.1 ml% of oxygen i.e 20.1ml of oxygen in 100 ml of blood. OXYGEN HAEMOGLOBIN DISSOCIATION CURVE INTRODUCTION:The relationship between the the partial pressure of oxygen and the % saturation Hb with oxygen can be explained graphically and the graph is called “OXYGEN Hb DISSOCIATION CURVE Normally in blood ,Hb is saturated with oxygen only upto by 95%. The saturation of Hb with oxygen depends upon partial pressure of oxygen. When the partial pressure of oxygen is less, Hb accepts oxygen and when the partial pressure of oxygen is less, Hb releases oxygen. Under normal conditions ,the oxygen Hb dissociation curve is “S” shaped or sigmoid shaped. The lower part indicates dissociation of oxygen from Hb. The upper part of curve indicates the acceptance of oxygen by Hb depending upon the partial pressure of oxygen. FACTORS AFFECTING OXYGEN DISSOCIATION CURVE The oxygen Hb dissociation curve is shifted to right by left by various factors:Shift to left indicates acceptance of oxygen by Hb. Shift to right indicates dissociation oxygen from haemoglobin. Shift to right:The oxygen Hb dissociation curve is shifted to right in following conditions:Decrease in partial pressure of oxygen Increase in partial pressure of co2 Increase in hydrogen ion concentration and decrease in pH Increased in body temp. Excess of DPG(2,3-Di phospho glycerate) Shift to left:- Shift of oxygen Hb dissociation curve to left occurs in following conditions:In fetal blood :because fetal Hb has got more affinity for oxygen than adult Hb Decrease in hydrogen ion concentration and increase in PH. In the tissues due to continous metabolic activities, partial pressure of CO2 is very high and partial pressure of oxygen is low. Due to pressure gradient CO2 enters the blood and oxygen is release from blood to the tissues. The presence of CO2 decreases the affinity of Hb for oxygen .It enhances further Release of oxygen to tissues and oxygen dissociation curve is shifted to right. It is known as BOHR’S EFFECT. All the factors which shift the oxygen dissociation curve to right enhance bohr’s effect. CO2 is transported by blood from tissues to alveoli. In the arteriole blood the volume of CO2 IS 48ml% and partial pressure of CO2 is 40mm Hg.In venous blood volume of CO2 52ml% and partial pressure is 46 mm of Hg. CO2 is transported in 4 ways:•As dissloved form-7% •As carbonic acid-negligible •As bicarbonates-63% •As carbamino compounds-30% CO2 diffuses into blood into and dissolves in fluid of plasma forming a simple solution. Only about 3ml per 100ml of plasma of CO2 is transported as dissolved state. It is about 7% of total CO2 in blood. Part of dissolved CO2 in plasma combines with water to form carbonic acid. Though CO2 is transported in this form, this reaction is very slow and it is negligible. About 63% of CO2 is transported as bicarbonate from plasma,the CO2 enters the RBCs. In the RBCs ,CO2 combines with water to form carbonic acid.The reaction inside RBCs very rapid,Due to presence of carbonic anhydrase enzyme.Carbonic anhydrase is present only inside the RBC not in plasma. i.e why the carbonic acid formation is atleast 200-300 times more in RBCs than in plasma. The carbonic acid is very unstable.Almost all carbonic acid formed in RBCs dissociates into bicarbonate and hydrogen ions .The increased concentration of bicarbonate inside the RBCs causes diffusion of bicarbonate ions through cell CHLORIDE SHIFT/HAMBURGER PHENOMENON In plasma plenty of NaCl is present.It dissociates into Na+ and ClWhen negatively charged bicarbonate ions moved out of RBCs into plasma, to maintain the electrolyte equlibrium the negatively charged ions Cl- ions moved into RBC and it is called chloride shift or hamberger’s phenomenon. About 30% of CO2 is transported as carbamino compounds CO2 is transported as blood in combination with Hb and plasma proteins. CO2 Combines with Hb to form carbamino Hb, and it combines with plasma proteins . CO2 DISSOCIATION CURVE CO2.The relationship between the partial pressure of CO2 and the quantity of CO2 that combines with blood is demonstrated by a graph called CO2 dissociation curve. NORMAL CO2 DISSOCIATION CURVE:The normal CO2 dissociation curve shows that the CO2 content in the blood is 48% when partial pressure of CO2 is 40mm of Hg and it is 52ml% when partial pressure of CO2 is 48 mm Hg .The CO2 content becomes 70ml%.When partial pressure is about 100mm Hg. FACTORS AFFECTING CO2 DISSOCIATION CURVE Combination of more amount of oxygen with Hb displaces CO2 from Hb. This effect is called haldane’s effect. So the excess of oxygen content in blood causes shift of CO2 dissociation curve to right. CAUSES OF HALDANE’S EFFECT:Due to combination with oxygen, the Hb becomes strongly acidic. It causes displacement of CO2 from Hb in two ways:The highly acidic Hb has low tendency to combine with CO2 So CO2 is displaced from blood. Because of acidity, hydrogen ions are released in excess. The hydrogen ions bind with bicarbonate ions to form carbonic acid. Carbonic acid in turn dissociates into water and CO2. The CO2 is released from blood and alveoli. SIGNIFICANCE OF HALDANE’S EFFECT:- The release of co2 from blood into alveoli lungs. Uptake of oxygen by blood. INTRODUCTION Respiration is a reflex process. Voluntary control of respiration is possible but only for a short period of about 40 seconds. The pattern of respiration is regulated by 2 mechanism:NERVOUS MECHANISM CHEMICAL MECHANISM A}.NERVOUS MECHANISM :- It regulates respiration by reflex process . It includes: respiratory centres, afferent nerves and efferent nerves. Respiratory centres:- These are group of neurons, which control the rate rhythm and force of respiration. These centers situated in reticular formation of brainstem on either side. Depending upon situation in the brainstem the respiratory Centres are classified into 2 groups:•Medullary centres •Pontine centres Medullary centres:-1}.Inspiratory centre 2}.Expiratory centre Pontine centres:- 3}.Pneumotaxic centre 4}.Apneustic centre 1}.Inspiratory centre:-It situated in upper part of medulla oblongata. It is formed by inspiratory neurons which are otherwise called dorsal group of respiratory organs. Function:-Inspiratory centre concerned with inspiration. Effect of stimulation:- Electric stimulation of inspiratory centre in animals by using needle electrode causes contraction of inspiratory muscles and prolonged inspiration. 2}.Expiratory centre:-It situated in medulla oblongata and lateral to the inspiratory centre. It is formed by expiratory neurons; which are otherwise called ventral group of respiratory neurons. Function:-Normally expiratory centre is inactive during quiet breathing and it becomes active during forced breathing or when inspiratory centre is inhibited. During quiet breathing expiration is a passive process due to recoiling property of thoracic cage. 3}.Pneumotaxic centre:-It situated in dorsoventral part of reticular formation in upper pons. The neurons of this centre form nucleus parabrachialis. Function:-The primary function of pneumotaxic centre is to control medullary respiratory centres,particularly the inspiratory centre through apneustic centre. It always controls activity of inspiratory centre so that duration of inspiration is controlled. Indirectly the pneumotaxic centre increases respiratory rate by reducing duration of inspiration. 4}.APNEUSTIC CENTRE:-It is situated in reticular formation of lower pons. Function:-The centre increases depth of inspiration by acting directly on inspiratory centre. Effect of stimulation:-The stimulation increases the duration of inspiration with short expiratory gasp.so respiration is called gasping type of respiration. Impulses from higher centres Impulses from stretch receptors of lungs Impulses from ‘j’ receptors of lungs Impulses from irritant receptors of lungs Impulses from baroreceptors Impulses from chemoreceptors Impulses from proprioreceptors Impulses from thermoreceptors Impulses from pain receptors cough reflex Sneezing reflex Deglutition reflex. B}.CHEMICAL MECHANISM :Certain chemical stimuli modulate how quickly and how deeply we breathe. Sensory neurons that are responsive to chemicals are termed CHEMORECEPTORS. There are two types of chemoreceptors:- CENTRAL CHEMORECEPTORS These are located in the medulla oblongata in the central nervous system. They respond to changes in H+ concentration or pCO2, or both, in cerebrospinal fluid. CO2 + H2O H2CO3 H+ + HCO3- PERIPHERAL CHEMORECEPTORS These are located in the aortic bodies, clusters of chemoreceptors located in the walls of the arch of the aorta, and in the carotid bodies, which are oval nodules in the wall of the left and right common carotid arteries where they divide into the internal and external carotid arteries. Pulmonary function tests provide a quantitative and objective assessment of the physiological derangement associated with pulmonary diseases. While these tests do not give a specific etiological or pathological diagnosis, the reasons for pulmonary function testing are:- a) Identification of cause of respiratory symptoms. b) Diagnosis of functional abnormalities. c) Diagnosis of severity of dysfunction, including subclinical abnormalities. d) Identification of and screening of unsuspected diseases. e) Assessment of reversibility of airway obstruction. f) Assessment of airway sensitivity. g) Evaluation of effectiveness of shortterm and long-term therapy. h) Long-term follow up. On the basis of these requirements the various pulmonary function test can be broadly classified into three groups:Tests to assess ventilatory functions of lungs; Tests to assess gaseous exchange across the lungs; Tests to assess transport of gases in the body; TESTS TO ASSESS VENTILATORY FUNCTIONS OF LUNGS:- (A) Assessment of the expansion of lungs and chest wall:1.Measurement of pressure changes during ventilation. For example: Intra pulmonary (intra alveolar) pressure. Intra pleural (intra thoracic ) pressure. 2.Measurement of compliance Compliance of lungs and chest wall Compliance of lungs alone. (B)Assessment of restrictive and obstructive ventilatory defects 1.)Measurement of static and dynamic lung volumes and capacities by ‘ spirometry ’ . 2.)Measurement of airways resistance. These provide a fairly good idea of the physical fitness in normal and the type and the extent of derangement of lung functions in lung patients. TEST TO ASSESS GASEOUS EXCHANGE ACROSS THE LUNGS:- 1. Measurement of ‘functional residual capacity’- FRC. 2. Measurement of ‘dead space’ and uniformity of ‘alveolar ventilation’. 3. Measurement of diffusion capacity of lungs. TEST TO ASSESS TRANSPORT OF GASES IN THE BODY 1. Measurement of gas tension, for example, pO2 and pCO2 in inspired, expired and alveolar air. 2. Measurement of gas tension and acid-base status of the blood. HYPOXIA DEFINITION:Hypoxia is a condition characterised by inadequate or decreased supply of oxygen to the lungs because of extrinsic reasons. The term anoxia is used synonymously with the hypoxia. Based on the cause, we can classify hypoxia into following types:1. HYPOXIC HYPOXIA OR ARTERIAL HYPOXIAIt is caused by a low Po2 in arterial blood as a result of high altitude, airway obstruction, or fluid in the lungs. 2. ANEMIC HYPOXIA- IN this type, too little functioning hemoglobin is present in blood, which reduces o2 transport in tissue cells. Among the causes are haemorrhage, anemia, and failure of hemoglobin to carry its normal complement of o2, as in carbon monoxide poisoning. 3.ISCHEMIC HYPOXIAin this the blood flow to a tissue is so reduced that too little o2 is delivered to it, even though po2 and oxyhaemoglobin level are normal. 4. HISTOTOXIC HYPOXIAIn this the blood delivers adequate o2 to tissues, but the tissues are unable to use it properly because of the action of some toxic agent. One cause is cyanide poisoning, in which cyanide blocks an enzyme needed for o2 utilization during ATP synthesis. 5.STAGNANT HYPOXIAthis type is characterised by decreased rate of flow of blood through the tissues. the oxygenncontent and tension of the arterial blood is normal but that of the venous is abnormally low due to sluggish circulation. ACCLIMATISATION ( Compenstory changes at moderately high altitude or low atmospheric pressure) DEFINITION :The term acclimatisation means the adjustment of the human body to suit the climate at a higher altitude. It includes various physiological readjustments and compensatory mechanisms that reduces the effects of hypoxia in permanent residents at high altitude. Some of the changes are immediate while others are a little delayed. CHANGES IN ACCLIMATISATION ON RESPIRATION:- a) Vital capacity of lungs increases in those people . b) Diffusing capacity for O2 through the alveolo capillary membrane increases. The factor responsible for these changes are :1. Expansion and dilatation of pulmonary capillaries 2. Increased blood volume 3. Increased lung volume 4. Elevated pulmonary arterial pressure 5. The apical part of the lungs which is normally under perfused is adequately perfused during anoxic acclimatisation . ON CIRCULATION:The right heart hypertrophies so that blood can be effectively pumped through the expanded capillary bed of the lung. There occurs temporary increase in cardiac output. blood flow through the heart, brain, muscles and other organs isincreased at the expense of blood flow through the skin and kidneys. The blood capillaries exposed to anoxia for long time get dilated to accommodate the extra blood. CYANOSIS:DEFINITION: Cyanosis is the bluish discolouration of the skin and /or mucus membrane due to the presence of at least 5 gm of reduced haemoglobin per 100 ml of blood in the capillaries. SITESCyanosis is commonly seen at the sites where the skin is thin. for eg: 1. Mucus membrane of under surface of tongue. 2. lips 3. Ear lobes 4. Nail beds 5. Tip of nose DYSPNOEA DEFINITION:- Dyspnoea means difficulty in breathing associated with a sense of distress. It is to be differentiated from hypernoea which simply means hyperventilation, as occurs in muscular exercise, and is usually not associated with sense of distress, unless, of course, the exercise very severe. ASPHYXIA DEFINITION: Improper aeration of blood, if continued for some time in an intact animal, produces a series of pathological manifestations and ultimately death. these manifestations are collectively called asphyxia. CLASSIFICATION:Asphyxia may be classified as 1.GENERAL 2.LOCAL