* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Major Basic Science Discoveries in HIV
Survey
Document related concepts
Transcript
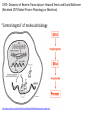
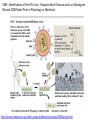
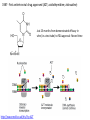
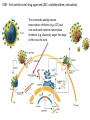
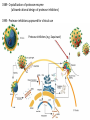
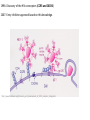
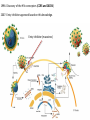
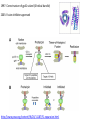
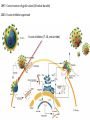
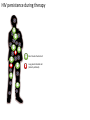
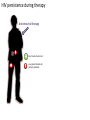
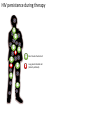
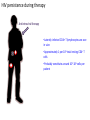
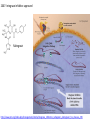
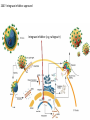
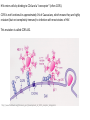
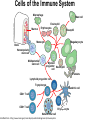
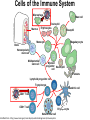
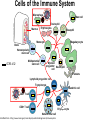
Major basic science discoveries in HIV Dr. Matthew Marsden, Ph.D. UCLA School of Medicine A new disease… On http://aids.gov/hiv-aids-basics/hiv-aids-101/aids-timeline/ A new disease… • By the end of 1981, there was a cumulative total of 270 reported cases of severe immune deficiency among gay men, and 121 of those individuals had died. • In 1983, Luc Montagnier and Françoise Barré-Sinoussi reported the discovery of a new virus (later called HIV) that is the cause of AIDS. • The first commercial blood test for HIV was licensed in 1985, allowing screening of the U.S. blood supply. • In 1987 the first anti-HIV drug (AZT) was approved by the U.S. Food and Drug Administration. • The first potent combination of anti-HIV drugs became available in 1995. On http://aids.gov/hiv-aids-basics/hiv-aids-101/aids-timeline/ Some Significant Historical Discoveries in the field of Retrovirology 1908- Discovery of Retroviruses in chickens (Ellermann and Bang). 1911- Cell free transmission of a sarcoma in chickens (Rous) named “Rous sarcoma virus”. Some Significant Historical Discoveries in the field of Retrovirology 1908- Discovery of Retroviruses in chickens (Ellermann and Bang). 1911- Cell free transmission of a sarcoma in chickens (Rous) named “Rous sarcoma virus”. Many additional retroviruses were subsequently identified in different animals, including important model systems: 1936- Mammary carcinoma in mice caused by milktransmitted, filterable agent (Bittner) termed “Mouse Mammary Tumor virus”. 1957- Potent leukemia virus isolated from mice (Gross) named “Gross murine leukemia virus”. Some Significant Historical Discoveries in the field of Retrovirology 1908- Discovery of Retroviruses in chickens (Ellermann and Bang). 1911- Cell free transmission of a sarcoma in chickens (Rous) named “Rous sarcoma virus”. Many additional retroviruses were subsequently identified in different animals, including important model systems: 1936- Mammary carcinoma in mice caused by milktransmitted, filterable agent (Bittner) termed “Mouse Mammary Tumor virus”. 1957- Potent leukemia virus isolated from mice (Gross) named “Gross murine leukemia virus”. 1957- Visna, a neurological disease in sheep caused by a lentivirus was described, giving rise to the concept of slow infections by these viruses (Latin: lentus, slow). 1980- 1st human retrovirus “Human T-cell leukemia virus 1” (HTLV-1) isolated. For more information see “Retroviruses” textbook chapter here: http://www.ncbi.nlm.nih.gov/books/NBK19403/ Timeline of discoveries 1970s: Discovery of retroviruses and retroviral enzymes 1970- Discovery of Reverse Transcriptase- Howard Temin and David Baltimore (Received 1975 Nobel Prize in Physiology or Medicine) “Central dogma” of molecular biology http://www.ncbi.nlm.nih.gov/Class/MLACourse/Modules/MolBioReview/central_dogma.html 1970- Discovery of Reverse Transcriptase- Howard Temin and David Baltimore (Received 1975 Nobel Prize in Physiology or Medicine) “Central dogma” of molecular biology However….. Reverse transcriptase catalyzes formation of DNA using an RNA template http://www.ncbi.nlm.nih.gov/Class/MLACourse/Modules/MolBioReview/central_dogma.html Timeline of discoveries 1970s: Discovery of retroviruses and retroviral enzymes 1981: Epidemic first identified 1983: Identification of the HIV virus 1983- Identification of the HIV virus- Françoise Barré-Sinoussi and Luc Montagnier (Shared 2008 Nobel Prize in Physiology or Medicine) http://www.nobelprize.org/nobel_prizes/medicine/laureates/2008/press.html Timeline of discoveries 1970s: Discovery of retroviruses and retroviral enzymes 1981: Epidemic first identified 1983: Identification of the HIV virus 1985: First commercial test to detect HIV 1987: First antiretroviral drug approved 1987- First antiretroviral drug approved (AZT; azidothymidine; zidovudine) Just 25 months from demonstrated efficacy in vitro (in a test tube) to FDA approval- Record time http://www.mcld.co.uk/hiv/?q=AZT 1987- First antiretroviral drug approved (AZT; azidothymidine; zidovudine) The nucleoside analog reverse transcriptase inhibitors (e.g. AZT) and non-nucleoside reverse transcriptase inhibitors (e.g. efavirenz) target this stage of the virus life cycle. Timeline of discoveries 1970s: Discovery of retroviruses and retroviral enzymes 1981: Epidemic first identified 1983: Identification of the HIV virus 1985: First commercial test to detect HIV 1987: First antiretroviral drug approved 1989: Crystallization of protease 1991: 2nd and 3rd anti-retrovirals approved 1995: Discovery of RANTES and MIP as suppressive factors 1995: Protease inhibitors approved 1989- Crystallization of protease enzyme (allowed rational design of protease inhibitors) 1995- Protease inhibitors approved for clinical use http://people.mbi.ucla.edu/yeates/153AH_2009_project/sriphanlop.html http://physiologyonline.physiology.org/content /26/4/236/F2.expansion.html 1989- Crystallization of protease enzyme (allowed rational design of protease inhibitors) 1995- Protease inhibitors approved for clinical use Protease inhibitors (e.g. Saquinavir) Timeline of discoveries 1970s: Discovery of retroviruses and retroviral enzymes 1981: Epidemic first identified 1983: Identification of the HIV virus 1985: First commercial test to detect HIV 1987: First antiretroviral drug approved 1989: Crystallization of protease 1991: 2nd and 3rd anti-retrovirals approved 1995: Discovery of RANTES and MIP as suppressive factors 1995: Protease inhibitors approved 1996: Discovery of CXCR4 and CCR5 co-receptors 1996- Discovery of the HIV coreceptors (CCR5 and CXCR4) 2007- Entry inhibitor approved based on this knowledge. http://www.thefullwiki.org/Discovery_and_development_of_CCR5_receptor_antagonists 1996- Discovery of the HIV coreceptors (CCR5 and CXCR4) 2007- Entry inhibitor approved based on this knowledge. Entry inhibitor (maraviroc) Timeline of discoveries 1970s: Discovery of retroviruses and retroviral enzymes 1981: Epidemic first identified 1983: Identification of the HIV virus 1985: First commercial test to detect HIV 1987: First antiretroviral drug approved 1989: Crystallization of protease 1991: 2nd and 3rd anti-retrovirals approved 1995: Discovery of RANTES and MIP as suppressive factors 1995: Protease inhibitors approved 1996: Discovery of CXCR4 and CCR5 co-receptors 1996: Discovery of protective effect of Δ32 CCR5 deletion 1997: Three-drug therapy (HAART) shown to delay progression 1997: Core structure of gp41 solved (6-helix bundle) 1997- Core structure of gp41 solved (6-helical bundle) 2003- Fusion inhibitor approved http://www.pnas.org/content/98/20/11187/F1.expansion.html 1997- Core structure of gp41 solved (6-helical bundle) 2003- Fusion inhibitor approved Fusion inhibitor (T-20, enfuvirtide) Timeline of discoveries 1970s: Discovery of retroviruses and retroviral enzymes 1981: Epidemic first identified 1983: Identification of the HIV virus 1985: First commercial test to detect HIV 1987: First antiretroviral drug approved 1989: Crystallization of protease 1991: 2nd and 3rd anti-retrovirals approved 1995: Discovery of RANTES and MIP as suppressive factors 1995: Protease inhibitors approved 1996: Discovery of CXCR4 and CCR5 co-receptors 1996: Discovery of protective effect of Δ32 CCR5 deletion 1997: Three-drug therapy (HAART) shown to delay progression 1997: Core structure of gp41 solved (6-helix bundle) 1997: Virus shown to persist in treated patients HIV persistence during therapy Short-lived infected cell Long-lived infected cell (latently infected) HIV persistence during therapy Antiretroviral therapy Short-lived infected cell Long-lived infected cell (latently infected) HIV persistence during therapy Short-lived infected cell Long-lived infected cell (latently infected) HIV persistence during therapy Antiretroviral therapy •Latently infected CD4+ T lymphocytes are rare in vivo: •Approximately 1 per 106 total resting CD4+ T cells •Probably constitute around 105-106 cells per patient Approximately 1 per million resting CD4+ T cells harbor a latent provirus. Rose Bowl Capacity = 92,542 Approximately 1 per million resting CD4+ T cells harbor a latent provirus. Rose Bowl Capacity = 92,542 Like finding one person in 11 football stadiums. To cure the infection we need to do this with 1,000,000 (one million) cells hidden in this way. Activation/elimination strategy for clearing latently-infected cells: Marsden and Zack (2010) Future Virol. 5(1): 97–109. Prostratin is a phorbol ester isolated from the Samoan medicinal plant Homalanthus nutans (and previously from Pimelea prostrata) Pimelea prostrata © 1991 Kennedy Harris Homalanthus nutans (Mamala Tree) http://members.ozemail.com.au/~pete rrjones/plants/f.html Traditionally used in treatment of jaundice and hepatitis http://www.berkeley.edu/news/ media/releases/2004/09/29_sa moa.shtml U1 cell latency assay: Add PKC agonist Assay p24 concentration in supernatant 2 days Bugula neritina Bryostatin 1: •First isolated from Bugula neritina. •Modulates PKC activity. •Shows potential as an anti-cancer therapeutic •Has been shown to inhibit tumor invasion, tumor growth in vitro and in vivo, and angiogenesis. http://www.marine.csiro.au •In various phase 1 and phase 2 clinical trials for treatment of cancer. •Previously was very difficult to obtain and hard to modify to alter activity. Bryostatin 1 -Publication involves 7 bryostatin analogs (bryologs). -These can be synthesized for several thousand dollars/gram (rather than 1 million). -Can be modified according to need. -Activate latent HIV expression more efficiently in vitro (cell lines). J-Lat 10.6 latency assay: Add latency activating agent 48 hours Timeline of discoveries 1970s: Discovery of retroviruses and retroviral enzymes 1981: Epidemic first identified 1983: Identification of the HIV virus 1985: First commercial test to detect HIV 1987: First antiretroviral drug approved 1989: Crystallization of protease 1991: 2nd and 3rd anti-retrovirals approved 1995: Discovery of RANTES and MIP as suppressive factors 1995: Protease inhibitors approved 1996: Discovery of CXCR4 and CCR5 co-receptors 1996: Discovery of protective effect of Δ32 CCR5 deletion 1997: Three-drug therapy (HAART) shown to delay progression 1997: Core structure of gp41 solved (6-helix bundle) 1997: Virus shown to persist in treated patients 1998: First non-nucleoside RT inhibitor approved 2003: Fusion inhibitor approved 2003: Restriction factors, TRIM5α and APOBEC3G, identified 2007: Integrase inhibitor approved 2007- Integrase inhibitor approved Raltegravir http://www.prn.org/index.php/management/article/integrase_inhibitors_raltegravir_elvitegravir_hiv_disease_478 2007- Integrase inhibitor approved Integrase inhibitor (e.g. raltegravir) Movie of the HIV Life Cycle http://www.youtube.com/watch?v=9leO28ydyfU Timeline of discoveries 1970s: Discovery of retroviruses and retroviral enzymes 1981: Epidemic first identified 1983: Identification of the HIV virus 1985: First commercial test to detect HIV 1987: First antiretroviral drug approved 1989: Crystallization of protease 1991: 2nd and 3rd anti-retrovirals approved 1995: Discovery of RANTES and MIP as suppressive factors 1995: Protease inhibitors approved 1996: Discovery of CXCR4 and CCR5 co-receptors 1996: Discovery of protective effect of Δ32 CCR5 deletion 1997: Three-drug therapy (HAART) shown to delay progression 1997: Core structure of gp41 solved (6-helix bundle) 1997: Virus shown to persist in treated patients 1998: First non-nucleoside RT inhibitor approved 2003: Fusion inhibitor approved 2003: Restriction factors, TRIM5α and APOBEC3G, identified 2007: Integrase inhibitor approved 2007: Entry inhibitor approved (Maraviroc) 2008: Discovery of Tetherin 2008: Transplant of infected subject with Δ32 donor stem cells http://www.nytimes.com/2011/11/29/health/new-hope-of-a-cure-for-hiv.html?pagewanted=all HIV enters cells by binding to CD4 and a “corecepter” (often CCR5). CCR5 is not functional in approximately 1% of Caucasians, which means they are highly resistant (but not completely immune) to infection with most strains of HIV. This mutation is called CCR532. http://www.thefullwiki.org/Discovery_and_development_of_CCR5_receptor_antagonists • The “Berlin Patient” was HIV positive and also developed leukemia. • He underwent aggressive chemotherapy to clear the leukemia, and in the process almost all the HIV+ cells in his body were also killed. • This patient then received two bone marrow transplants from a CCR5-32 individual. • The new immune cells were not susceptible HIV, and the virus in currently undetectable more than four years post-transplant. Cells of the Immune System Macrophage Marrow Mast cell Eosinophil Erythrocytes Basophil Monocyte Bone Megakaryocyte Hematopoietic stem cell Multipotential stem cell Myeloid progenitor Neutrophil cell Platelets Lymphoid progenitor cell T lymphocyte Dendritic cell CD4+ T cell CD8+ T cell B lymphocyte Natural killer cell Modified from : http://www.cancer.gov/cancertopics/understandingcancer/immunesystem Cells of the Immune System Macrophage Marrow Mast cell Eosinophil Erythrocytes Basophil Monocyte Bone Megakaryocyte Hematopoietic stem cell Multipotential stem cell Myeloid progenitor Neutrophil cell Platelets Lymphoid progenitor cell T lymphocyte Dendritic cell CD4+ T cell CD8+ T cell B lymphocyte Natural killer cell Modified from : http://www.cancer.gov/cancertopics/understandingcancer/immunesystem Cells of the Immune System Macrophage Marrow Mast cell Eosinophil Erythrocytes Basophil Monocyte Bone Megakaryocyte Hematopoietic stem cell Multipotential stem cell Myeloid progenitor Neutrophil cell Platelets Lymphoid progenitor cell T lymphocyte Dendritic cell CD4+ T cell CD8+ T cell B lymphocyte Natural killer cell Modified from : http://www.cancer.gov/cancertopics/understandingcancer/immunesystem Cells of the Immune System Macrophage Marrow Mast cell Eosinophil Erythrocytes Basophil Monocyte Bone Megakaryocyte Hematopoietic stem cell Multipotential stem cell Myeloid progenitor Neutrophil cell Platelets Lymphoid progenitor cell T lymphocyte Dendritic cell CD4+ T cell CD8+ T cell B lymphocyte Natural killer cell Modified from : http://www.cancer.gov/cancertopics/understandingcancer/immunesystem Cells of the Immune System Macrophage Marrow Mast cell Eosinophil Erythrocytes Basophil Monocyte Bone Megakaryocyte Hematopoietic stem cell CCR5-32 Multipotential stem cell Myeloid progenitor Neutrophil cell Platelets Lymphoid progenitor cell T lymphocyte Dendritic cell CD4+ T cell CD8+ T cell B lymphocyte Natural killer cell Modified from : http://www.cancer.gov/cancertopics/understandingcancer/immunesystem Why can’t we use this approach for everybody? • The chemotherapy and bone marrow transplant procedure was very risky (the patient nearly died). • Matching donors that are also CCR5-32 are very hard to find. • The procedure is very expensive, time consuming, and requires excellent medical facilities (not feasible in many parts of the world) . • The patient will have to take immunosuppressive drugs for the rest of their life to avoid problems with the transplant (this may be worse than just taking the anti-HIV drugs). Timeline of discoveries 1970s: Discovery of retroviruses and retroviral enzymes 1981: Epidemic first identified 1983: Identification of the HIV virus 1985: First commercial test to detect HIV 1987: First antiretroviral drug approved 1989: Crystallization of protease 1991: 2nd and 3rd anti-retrovirals approved 1995: Discovery of RANTES and MIP as suppressive factors 1995: Protease inhibitors approved 1996: Discovery of CXCR4 and CCR5 co-receptors 1996: Discovery of protective effect of Δ32 CCR5 deletion 1997: Three-drug therapy (HAART) shown to delay progression 1997: Core structure of gp41 solved (6-helix bundle) 1997: Virus shown to persist in treated patients 1998: First non-nucleoside RT inhibitor approved 2003: Fusion inhibitor approved 2003: Restriction factors, TRIM5α and APOBEC3G, identified 2007: Integrase inhibitor approved 2007: Entry inhibitor approved (Maraviroc) 2008: Discovery of Tetherin 2008: Transplant of infected subject with Δ32 donor stem cells Thank you for your attention! Questions?