* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Cardiac CT and MRI Findings of Structural Heart Diseases
Remote ischemic conditioning wikipedia , lookup
Saturated fat and cardiovascular disease wikipedia , lookup
Electrocardiography wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Cardiovascular disease wikipedia , lookup
Marfan syndrome wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Aortic stenosis wikipedia , lookup
Drug-eluting stent wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Cardiac surgery wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
History of invasive and interventional cardiology wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
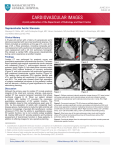
Cardiac CT and MRI Findings of Structural Heart Diseases causing Sudden Cardiac Death in Adults 1Department Sung-Min Ko1, Jeong-Geun Yi1,Woo-Chul Kwon2 of Radiology, Konkuk University Hospital, Seoul, Korea Introduction Coronary y artery y disease with angina g or MI Ischemic Heart Disease CAD with MI or angina Coronary artery embolism Nonatherogenic CAD Coronary artery spasm C D E No structural Heart Disease Primary electrical disease Prolonged QT syndrome Preexcitation syndrome Complete heart block Chest wall trauma Nonischemic heart disease CAD without MI or angina Cardiomyopathy – hypertrophic, dilated, restictive Valvular heart disease Congenital heart disease Myocarditis Acute pericardial tamponade Acute myocardial rupture Acute aortic dissection Arrhythmogenic RV dysplasia - 80% of patients who experience SCD at all ages have atherosclerotic coronary artery disease - At post mortem acute occlusive coronary thrombus was found in 15% to 64% due to plaque fissuring, hemorrhage or thrombosis - No difference in artery involved. - More risk of SCD with abrupt proximal obstruction rather than progressive diffuse disease when collateral can form - Patient prognosis with AMI depends on the extent of myocardial necrosis, the presence of microvascular obstruction, and the degree of contractile dysfunction A of Radiology, Wonju Christian Hospital Causes of SCD Sudden cardiac death (SCD) is defined as an unexpected sudden death due to cardiac cause and occurring within 1 hour of symptoms and is a major public health problem. SCD accounts for 30% of sudden deaths between 14 and 21 years of age. There is an increased risk of SCD in athletic young adults. There are a number of underlying cardiac conditions that increase the risk of SCD even though acute myocardial infarction as a correlate of coronary artery disease is mostly common. Different underlying causes can be diagnosed and differentiated by contrast-enhanced CT and MRI non-invasively. B 2Department Fig. 2. 72-year-old man with reperfused AMI. (A) CT angiography of RCA – Massive thrombotic occlusion of m-dRCA (B-E) Two-phase perfusion images with CT (B, C) and MR ((D,E) , ) - Early y subendocardial perfusion defect (B&D, arrows) and subendocardial residual PD with transmural late enhancement (C&E, arrows) in the mid inferior myocardium of LV wall. A A Noncardiac Disease Drowning Pickwickian syndrome Pulmonary embolism Drug-induced Airway obstruction B C Fig. 1. 62-year-old man who presented with anterior chest pain for 10 days. (A, B) CT angiography -Significant stenoses (arrows) with noncalcified plaques in the proximal segment of LAD (C) Conventional angiography – 85% stenosis in the same segment (arrow). Fig. 3. 68-yearold man with AMI. (A, B) Multiplanar reformations in 4-chamber 4 chamber (A) and short-axis (B) views – Rupture of interventricular septum A B B Fig. 6. 58-year-old woman who presented with dyspnea on exertion. (A) Inverse angiographic emulsion image- Left anterior descending coronary artery (arrow) originating right coronary artery (arrowhead, single coronary artery without left circumflex artery). (B) Oblique coronary thick slap MIP image – Interarterial and intramyocardial course of LAD (arrow) originating from the right coronary (arrowhead) Myocardial bridging A Coronary artery fistula - An anomalous communication between a coronary artery and either a cardiac chamber, coronary sinus or pulmonary artery - More commonly involving the RCA (60% of cases) than the LCA (40%) - The commonest sites of drainage are the right ventricle (45%), right atrium (25%) or pulmonary artery (15%), producing left to-right shunt. - If fistula flow is high, the distal perfusion of the originating coronary artery may be compromised. B A Hypertrophic cardiomyopathy A B Fig. 4. 59-year-old man who presented with chest pain after blunt trauma. (A, B) Multiplanar reformations in 4-chamber (A) and short-axis (B) views – Intramural hematoma (arrows) extending from the left main bifurcation to the proximal LAD. (C) Volume Volume-rendered rendered image – Excellent depiction of luminal narrowing of pLAD. pLAD B A - The most common of cardiomyopathy with an incidence of 1 in 500 - The commonest cause of SCD in the US (70% of patient suddenly die) - Most common inherited cardiac disease (autosomal dominant) - Basal anterior and anterior septal are most commonly affected - Wall thickness > 30 mm infers an increased risk of SCD - Systolic anterior motion (SAM) of the mitral leaflet with associated mitral regurgitation is frequent finding. finding - With increasing wall thickness, there is increased percentage of fibrosis. As fibrosis increases, wall function decreases. B C Fig. 8. 66-year-old woman who presented with chest pain on exercise. (A, B) Curved MPR image (A) and short-axis MIP image of LAD (B) - Intramyocardial course of mLAD (arrows) and asymmetric wall thickening of LV myocardium (B), corresponding to hypertrophic cardiomyopathy. C A B C D H F C B E A A B Fig. 7. 50-year-old man who presented with angina. (A) Short-axis MPR image – Deep type of myocardial bridging (arrow) (B, C) Conventional angiography – Systolic compression of the tunneled segment (B, arrow) but recovery its normal diameter on di t l (C, diastole (C arrow). ) Fig. 9. Two cases of coronary artery-pulmonary artery fistula. (A, B) Volume-rendered images – Anomalous connection (arrows) arising from right and left coronary arteries and draining into the pulmonary trunk. The fistulas contain aneurysms (arrowheads). Anomalous coronary artery from the opposite sinus - Risk of adverse events is highest in anomalous arteries with interarterial course : RCA from left coronary sinus - >90% : LCA from right coronary sinus – 60% : LAD from right coronary sinus – 50% - The cause of 5-35% of SCD in young athletes - Mechanism not entirely clear : Abberant artery arises at an acute angle, often from a slitlike hypoplastic ostium, traverses the aortic wall obliquely, emerges between the aorta and the right ventricular outflow tract, and then proceeds to its usual area of distribution. : With exertion, proximal angulation or compression obstructs the blood flow , leading to distal ischemia, ventricular tachycardia, and fibrillation. A - Coronary artery dives into the substance of the myocardium di (i (intramyocardial t di l course)) - Commonly middle segment of LAD - Clinically silent in most cases. Rarely, myocardial ischemia and infarction, arrhythmia, SCD - Incidence: angiography 0.5-4.5%, CTA 3.5-30.5% - Atherosclerotic plaque proximal to tunneled segment - Angiography: milking effect and step down-step up phenomena induced by systolic compression of MB segment - MDCT: superficial and deep type, systolic compression Æ Alternative noninvasive imaging tool that allows for easy and accurate evaluation of myocardial bridging. Coronary artery dissection after blunt trauma - Coronary artery injuries after blunt chest trauma : Lacerations, L ti s thrombosis, th mb sis intimal i tim l dissection, diss ti arteriovenous fistula, pseudoaneurysm formation - Coronary dissection consists of about 16% of traumatic coronary injuries. - MDCT : Ideal imaging technique to delineate intramural hematoma, assess luminal narrowing and follow up the appearance : Useful to decide to do coronary angiography or not in patients with borderline probability of coronary injury. B Fig. 5. 54-year-old man who presented with chest pain during exercise. (A) Volume-rendered image – Left coronary artery (arrow) originating from the right sinus of Valsalva and traveling between the aorta and pulmonary artery (B) Curved multiplanar reformation image of LAD - Intramyocardial course of proximal segment of LAD (arrow) D Fig. 5. 29-year-old man who presented with chest pain during exercise. (A) Volume-rendered image – Right coronary artery (RCA) originating from the left sinus of Valsalva and traveling between the aorta and pulmonary artery (B, C) Oblique axial thick slap maximum intensity projection images of a RCA - Slit-like narrowing of RCA ostium on end-systole (B) compared with enddiastole (C). (D) Volume-rendered image obtained after coronary artery bypass graft surgery – Patent right internal mammary artery graft to pRCA B D G I J Fig. 10. 64-year-old woman who presented with severe chest discomfort on exertion. (A, B) 2- (A) and 4-chamber (B) SSFP cine images of MR – Concentric hypertrophy of LV wall. (C, D) First pass myocardial perfusion cardiac MR images at stress (C) and rest (D) – Partially reversible myocardial perfusion defect in anterior, septal and inferior LV wall. (E-G) Delayed contrast-enhanced cardiac MR images – Diffuse enhancement except lateral wall (H, I) Dual-energy CT iodine map images – Myocardial perfusion deficit in anterior LV wall (J) Myocardial perfusion SPECT – No myocardial perfusion defect at stress and rest. Fig. 11. 62-year-old man who presented with chest pain for more than 10 year. (A, B) LV outflow tract SSFP cine images of cardiac MR - Hypertrophied LV septum (arrows) – Narrow LVOT (arrowheads) on diastole (A) and systole (B) - SAM with associated subvalvular stenosis and stenotic jet flow (B, arrowhead) on systole and mitral regurgitation (C) Short-axis SSFP cine image of cardiac MR – Asymmetric hypertrophy of LV septum and anterior myocardium. (D) Delayed contrast-enhanced cardiac MR image - Extensive delayed hyperenhancement (arrows) of LV wall. Non-ischemic dilated cardiomyopathy (NIDCM) - Dilatation of all four chambers of the heart, but primarily the left ventricle, with associated systolic dysfunction. - 18% of symptomatic patients with ejection fraction less than 30% were diagnosed with NIDCM. - Patients with NIDCM suffer from heart failure mortality and SCD in near equal numbers. - SCD may well be the first manifestation of NIDCM, NIDCM and idiopathic NIDCM is responsible for 10% of all SCDs in adults - It is often preceded by infectious myocarditis but 2030% is familial. Other causes include autoimmune, toxic and metabolic diseases. - A mid-myocardial stripe on delayed contrast-enhanced cardiac MR imaging is the “classic” imaging pattern seen in about 30% of patients. 60% of patients will have no enhancement Aortic stenosis (AS) B A - Most common valve disease resulting in valve replacement - Causes: Congenital (bicuspid aortic valve), degenerative, rheumatic heart disease - Pathophysiologic effects of AS : LV hypertrophy, LV systolic dysfunction, myocardial fibrosis, abnormal coronary blood flow, pulmonary hypertension - Incidence of SCD in asymptomatic severe AS : 0-4.1% - Mechanism of SCD: Unclear, and both malignant ventricular arrhythmia and bradyarrhythmia have been documented. -Timing of surgery for AS : Symptomatic moderate to severe AS : Asymptomatic severe AS - Progressive increase in AV velocity and decrease in AVA grad > 65 mmHg, g, AVA 0.7 cm2) - Critical AS ((mean g - LV systolic dysfunction - Marked LVH - Associated severe coronary artery disease C Fig. 12. 62-year-old man with congestive heart failure (A,B) 4-chamber SSFP cine images of cardiac MR – Severely dilated LV without thinned myocardium (A, diastole). Global severe hypokinesia of LV wall and mild MR (B, systole) (C,D) Delayed contrast-enhanced cardiac MR images – A mid-wall stripe of delayed hyperenhancement in the myocardium of anterior and septal LV wall (arrows). D Amyloidosis cardiomyopathy - Almost all cases of primary amyloidosis and approximately ¼ of familial amyloidosis - Amyloid deposition occurs with the myocardium of the ventricle and atria, valve leaflets and within the coronary arteries. ymp m occur from f m disruption p in contractile function, f , - Symptoms conduction and influences coronary artery flow. - Left ventricular wall thickness - prognostic importance (median survival of only 6 months) - Cardiac MR imaging: diffuse hyperenhancement pattern on delayed-enhancement MRI, typically more prominent in the subendocardium and the basal segments. A B C Fig. 13. 56-year-old woman who presented with dyspnea on exertion. (A) Short-axis MPR image of cardiac CT – Concentric hypertrophy of LV myocardial wall. (B) First pass myocardial perfusion cardiac MR images at rest – Concentric perfusion defect (arrows) of LV myocardial wall (C) Delayed contrast-enhanced cardiac MR images – Diffuse myocardial enhancement involving both ventricles (arrows). A B C Fig. 14. 67-year-old man with heart failure. (A) Axial double inversion recovery T1WI – High signal intensity of thick p layer y ( )and ) iso-signal g intensity y of thin compacted p layer y ( )of ) noncompacted LV myocardium. Ratio noncompacted/compated layer = 4.8 (B, C) Short-axis (B) and 2-chamber (C) end-diastolic SSFP cine image of cardiac MR – Excessive trabeculations of the LV wall, particularly severe in apex and apical wall. LV dilatation and severe, global hypokinesia in the LV wall. LV ejection fraction 15% Fig. 15. 47-year-old woman with arrhythmia. (A, B) Axial SSFP cine image of cardiac MR – Prominent epicardial fat (A, (A arrow). arrow) - Aneurysm formation in RV wall (B, arrows) on end-systole. Arrhythmogenic right ventricular dysplasia - Myocardial y cell loss with partial p or total replacement p of right ventricular muscle by adipose and fibrous tissue - A familial disorder in 30% of cases, with autosomal dominant inheritance. - The most commonest cause of SCD in an Italian screening program. - Unexplained syncope or SCD is the first clinical manifestation of the ARVD. - Onset in adolescence or early childhood. - CT: Abundant epicardial adipose tissue, prominent t b trabeculations l ti s with ith low l attenuation, tt ti scalloped s ll d appearance of f RV free wall, intramyocardial fat deposits - MRI : Intramyocardial fat, RV wall thinning or hypertrophy, trabecular disarray of RV, enlargement of RVOT, global and regional RV dysfunction, myocardial fibrosis with delayed contrast enhancement - “billowing” or prolapse of one or both of the mitral leaflets into the left atrium prevalent condition more associated with non- MVP is a p lethal arrhythmias. - Whether simple MVP causes SCD in unclear as it is such a prevalent condition that it may be coincidental finding and not causally related to SCD. - Patients who also have mitral regurgitation and LV dysfunction or myxomatous degeneration of the valve are at higher risk of SCD. - M/C cause of severe non-ischemic MR in the USA - Overall prognosis – excellent, but serious complications i f ti endocarditis, infective d diti SCD SCD, severe MR - Pathophysiological basis : Leaflet thickening and redundancy (myxomatous degeneration) - Echocardiography : single or bileaflet prolapse at least 2 mm - Association with heritable connective tissue disorders : Marfan syndrome, Ehlers-Danlos syndrome, osteogenesis imperfecta, and pseudoxanthoma elasticum Marfan’s syndrome - Autosomal dominant inherited connective disorder occurring in about 1 in 10000 people - Defects in fibrillin-1 gene (FBN1) on chromosome 15 - Involves CV, skeletal, ocular systems - Cystic medial necrosis in the wall of the aorta which weakens it g dilatation of f aortic root and sinus of f Valsalva - Progressive and may lead to aortic regurgitation and complete dissection or rupture of the aorta with subsequent death, pericardial tamponade or coronary artery dissection C A B A Fig. 16. 29-year-old woman with arrhythmia (A, B) Axial (A) and oblique coronal MIP images – RV wall thinning (A, arrow) and scalloped appearance of RV free wall (B, arrows) B A B Fig. 17. 27-year-old woman who presented with acute atypical chest pain (A) Delayed contrast-enhanced cardiac MR – Mainly subepicardial enhancement involving the mid anteroseptal and inferior LV wall (arrows). (B) Short-axis triple inversion recovery T2WI – Ill defined high signal intensity in the same areas (arrows). Courtesy of Chun EJ (BSNU) - Longitudinal cleavage of the aortic media by dissecting column of blood - Almost always accompanied by a transverse intimal and medial tear - Intimal tear sites :Type I and II: 1 ~ 2 cm above the sino-tubular junction involving right lateral wall :Type III: Distal to the origin of the left subclavian artery -False lumen in classic dissection : Within the media : Intimomedial flap = inner 2/3 of media + intima - Complication : rupture, rupture leakage, leakage side branch involvement, aortic occlusion, dissection aneurysm Conclusion C D Fig. 19. 57-year-old woman with known aortic stenosis. (A, B) CT images with thick slab 4D reconstruction with blood pool inversion technique – Pure bicuspid aortic valve with thickened, calcified cusps (A, arrow) and reduced systolic opening (B (B, arrow) (C) CT planimetry of bicuspid AV – Moderate to severe degree of AS (D) Oblique sagittal MPR image of cardiac CT – Aneurysmal dilatation of aorta A B C D E Fig. 20. 49-year-old F ld man with h known k mitrall regurgitation (A-C) CT images with thick slab 4D reconstruction with blood pool inversion technique – Prolapsed posterior mitral leaflet (P1 portion, arrows) during systole (D, E) Short axis (D) and 3-chamber (E) SSFP cine images of cardiac MR - Eccentric regurgitant jet flow across mitral valve into LA in systole (arrows) Aortic dissection B D Fig. 18. 81-year-old man who presented with chest pain. (A, B) Double oblique axial MPR images of cardiac CT images – Degenerative aortic valve disease with severely reduced systolic opening of aortic valve (CT planimetry 0.72 mm2), corresponding to severe AS (C) Oblique sagittal SSFP cine image of cardiac MR – Stenotic jet flow across aortic valve into ascending aorta in systole (peak velocity 4.2 m/sec) (D) Short-axis MPR image of cardiac CT – Old MI in the mid inferolateral wall A A Myocarditis - Most M t cases are subclinical. b li i l - Most common cause: group B Coxsackie virus - SCD is a recognized complication and is often associated with exercise due to poor contraction of a dilated LV or an arrhythmogenic focus from acutely inflamed or healed myocardium. - DE-MRI : Multiple patchy enhancement predominantly in subepicardial, inferolateral portion. : follow-up Æ decreased extent of enhancement B Mitral valve prolapse (MVP) Non-compaction cardiomyopathy - Rare cardiomyopathy which is believed to be a result of an arrest in development of the myocardium. - Gross anatomical appearance: numerous, excessively prominent trabeculations and deep intertrabecular recesses in communication with the ventricular cavity. - Predominantly (>80%) found in the apical and midventricular areas of both the inferior and the lateral wall. - Natural history: LV systolic dysfunction and heart failure (most common), arrhythmias, thromboembolism, SCD - Non-compacted to compacted ration > 2.3 in end-diastole is considered diagnostic by MRI criteria. - Differential diagnosis: prominent normal ventricular trabeculations, ARVD, apical HCMP, thrombus, endomyocardial fibrosis A B C Fig. 21. 33-year-old man with Marfan’s syndrome. (A, B) Oblique sagittal (A) and axial MPR (B) images of cardiac CT - Dilatation of aortic root and redundant non-coronary cusp (arrows) with coaptation defect in diastole. (C) Cine echocardiographic image - Severe eccentric aortic regurgitation (arrow) due to prolapse of noncoronary cusp. A B C Fig. 22. 35-year-old man with Marfan’s syndrome. (A C) Oblique (A-C) Obli sagittal itt l (A) (A), axial i l (B) (B), and d oblique bli coronall MPR (C) iimages of f cardiac CT - Aortic dissection (arrows) involving aortic root, particularly right sinus of Valsalva with RCA ostial mild stenosis. - Dilatation of aortic root and redundant non-coronary cusp (arrowhead) with coaptation failure. 1. SCD is not common in the general population. However, the incidence is significantly higher in the cohort of patients who has congenital cardiac disease. The causes of SCD in adults vary with age. 2. It is very important for the radiologists to be familiar with radiological findings of the predisposing underlying cardiac abnormalities may allow preventive management.