* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Assessment and Management of Patients with Endocrine Disorders Dr Ibraheem Bashayreh 29/11/2010
Survey
Document related concepts
Cardiac physiology wikipedia , lookup
Breast development wikipedia , lookup
Mammary gland wikipedia , lookup
Glycemic index wikipedia , lookup
Endocrine disruptor wikipedia , lookup
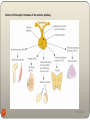
Hormone replacement therapy (male-to-female) wikipedia , lookup
Hyperandrogenism wikipedia , lookup
Adrenal gland wikipedia , lookup
Growth hormone therapy wikipedia , lookup
Hypothalamus wikipedia , lookup
Hypothyroidism wikipedia , lookup
Transcript
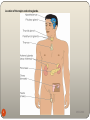
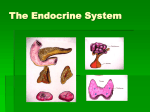
Assessment and Management of Patients with Endocrine Disorders Dr Ibraheem Bashayreh 1 29/11/2010 Location of the major endocrine glands. 2 29/11/2010 Definition of Hormones Chemical messengers of the body Act on specific target cells Regulated by negative feedback Too much hormone, then hormone release reduced Too little hormone, then hormone release increased 3 29/11/2010 Glands of the Endocrine System Hypothalamus Posterior Pituitary Anterior Pituitary Thyroid Parathyroids Adrenals Pancreatic islets Ovaries and testes 4 29/11/2010 Hypothalamus Sits between the cerebrum and brainstem Houses the pituitary gland and hypothalamus Regulates: Temperature Fluid volume Growth Pain and pleasure response Hunger and thirst 5 29/11/2010 Hypothalamus Hormones Releasing and inhibiting hormones Corticotropin-releasing hormone Thyrotropin-releasing hormone Growth hormone-releasing hormone Gonadotropin-releasing hormone Somatostatin-=-inhibits GH and TSH 6 29/11/2010 Pituitary Gland Sits beneath the hypothalamus Termed the “master gland” Divided into: Anterior Pituitary Gland Posterior Pituitary Gland 7 29/11/2010 Anterior Pituitary Gland Promotes growth Stimulates the secretion of six hormones Controls pigmentation of the skin 8 29/11/2010 Anterior Pituitary Gland Hormones Growth Hormone- Adrenocorticotropic hormone Thyroid stimulating hormone Follicle stimulating hormone—ovary in female, sperm in males Luteinizing hormone—corpus luteum in females, secretion of testosterone in males Prolactin—prepares female breasts for lactation 9 29/11/2010 Actions of the major hormones of the anterior pituitary. 10 29/11/2010 Posterior Pituitary Gland Stimulates the secretion of two hormones Promotes water retention 11 29/11/2010 Posterior Pituitary Hormones Antidiuretic Hormone Oxytocin—contraction of uterus, milk ejection from breasts 12 29/11/2010 Adrenal Cortex Mineralocorticoid—aldosterone. Affects sodium absorption, loss of potassium by kidney Glucocorticoids—cortisol. Affects metabolism, regulates blood sugar levels, affects growth, antiinflammatory action, decreases effects of stress Adrenal androgens—dehydroepiandrosterone and androstenedione. Converted to testosterone in the periphery. 13 29/11/2010 Adrenal Medulla Epinephrine and norepinephrine serve as neurotransmitters for sympathetic system 14 29/11/2010 Thyroid Gland Butterfly shaped Sits on either side of the trachea Has two lobes connected with an isthmus Functions in the presence of iodine Stimulates the secretion of three hormones Involved with metabolic rate management and serum calcium levels 15 29/11/2010 Thyroid Follicular cells—excretion of triiodothyronine (T3) and thyroxine (T4)—Increase BMR, increase bone and calcium turnover, increase response to catecholamines, need for fetal G&D Thyroid C cells—calcitonin. Lowers blood calcium and phosphate levels BMR: Basal Metabolic Rate 16 29/11/2010 Parathyroid Glands Embedded within the posterior lobes of the thyroid gland Secretion of one hormone Maintenance of serum calcium levels 17 29/11/2010 Parathyroid Parathyroid hormone—regulates serum calcium 18 29/11/2010 Pancreas Located behind the stomach between the spleen and duodenum Has two major functions Digestive enzymes Releases two hormones: insulin and glucagon 19 29/11/2010 Pancreatic Hormones Insulin Glucagon—stimulates glycogenolysis and glyconeogenesis Somatostatin—decreases intestinal absorption of glucose 20 29/11/2010 Insulin Produced by the Beta cells in the islets of Langerhans Regulates blood glucose levels Mechanisms Eases the active transport of glucose into muscle and fat cells Facilitates fat formation Inhibits the breakdown and movement of stored fat Helps with protein synthesis 21 29/11/2010 Action of insulin and glucagon on blood glucose levels. (A) High blood glucose is lowered by insulin release. 22 29/11/2010 (continued) Action of insulin and glucagon on blood glucose levels. (B) Low blood glucose is raised by glucagon release. 23 29/11/2010 Glucagon Produced by the alpha cells in the islets of Langerhans Glucagon released when blood glucose falls below 70 mg/dL 24 29/11/2010 Glucagon Prevents blood glucose from decreasing below a certain level Functions: Makes new glucose Converts glycogen into glucose in the liver and muscles Prevents excess glucose breakdown Decreases glucose oxidation and increases blood glucose 25 29/11/2010 Kidney 1, 25 dihydroxyvitamin D—stimulates calcium absorption from the intestine Renin—activates the RAS Erythropoietin—Increases red blood cell production RAS: Renin-Angiotensin System 26 29/11/2010 Adrenal Glands Pyramid-shaped organs that sit on top of the kidneys Each has two parts: Outer Cortex Inner Medulla 27 29/11/2010 Adrenal Cortex Secretion of two hormones Glucocorticoids: cortisol Mineralocortocoids: aldosterone Involved with blood glucose level, anti- inflammatory response, blood volume, and electrolyte maintenance 28 29/11/2010 Adrenal Medulla Secretion of two hormones Epinephrine Norepinephrine Involved with the stress response 29 29/11/2010 Ovaries Estrogen Progesterone—inportant in menstrual cycle,*maintains pregnancy, 30 29/11/2010 Testes Androgens, testosterone—secondary sexual characteristics, sperm production 31 29/11/2010 Thymus Releases thymosin and thymopoietin Affects maturation of T lymphocetes 32 29/11/2010 Pineal Melatonin Affects sleep, fertility and aging 33 29/11/2010 Prostaglandins Work locally Released by plasma cells Affect fertility, blood clotting, body temperature 34 29/11/2010 Past Medical History Hormone replacement therapy Surgeries, chemotherapy, radiation Family history: diabetes mellitus, diabetes insipidus, goiter, obesity, Addison’s disease, infertility Sexual history: changes, characteristics, menstruation, menopause 35 29/11/2010 Physical Assessment General appearance Vital signs, height, weight Integumentary Skin color, temperature, texture, moisture Bruising, lesions, wound healing Hair and nail texture, hair growth 36 29/11/2010 Physical Assessment Face Shape, symmetry Eyes, visual acuity Neck 37 29/11/2010 Palpating the thyroid gland from behind the client. (Source: Lester V. Bergman/Corbis) 38 29/11/2010 Physical Assessment Extremities Hand and feet size Trunk Muscle strength, deep tendon reflexes Sensation to hot and cold, vibration Thorax Lung and heart sounds Extremity edema 39 29/11/2010 Older Adults and Endocrine Function Relationship unclear Aging causes fibrosis of thyroid gland Reduces metabolic rate Contributes to weight gain Cortisol level unchanged in aging 40 29/11/2010 Abnormal Findings Ask the client: Energy level Fatigue Maintenance of ADL Sensitivity to heat or cold Weight level Bowel habits Level of appetite Urination, thirst, salt craving 41 29/11/2010 Abnormal Findings (continued) Ask the client: Cardiovascular status: blood pressure, heart rate, palpitations, SOB Vision: changes, tearing, eye edema Neurologic: numbness/tingling lips or extremities, nervousness, hand tremors, mood changes, memory changes, sleep patterns Integumentary: hair changes, skin changes, nails, bruising, wound healing 42 29/11/2010 Most Common Endocrine Disorders Thyroid abnormalities Diabetes mellitus 43 29/11/2010 Diagnostic Tests GH: fasting, well rested, not physically stressed Water deprivation: fasting for 12 hours, no fluids/smoking after midnight T3/T4: no specific preparation Serum calcium/phosphate: fasting may or may not be required Collection that needs to be iced or refrigerated 44 29/11/2010 Diagnostic Tests Cortisol/aldosterone level: two blood samples, client to be up for at least 2 hours before test is drawn Urine 17-ketosteroids: 24-hour urine collection that needs to be iced or refrigerated 45 29/11/2010 Diagnostic Tests FBS: fast before the test HbA1c: No fasting required 2-hour OGTT: drink 75 g of glucose and do not eat anything until blood is drawn Urine glucose/ketones: fresh urine specimen Urine microalbumin: fresh urine specimen 46 29/11/2010 Imaging Studies MRI: metallic implants, lie motionless during test; remove all metal objects CT scan: assess for allergies to iodine and seafood; lie immobile during the test Thyroid scan: allergies to iodine and seafood; hold thyroid drugs containing iodine for weeks before the study 47 29/11/2010 Imaging Studies RAI: fast for 8 hours before; can eat 1 hour after radioiodine capsule/liquid taken; hold thyroid drugs with iodine for weeks before the study 48 29/11/2010 THYROID DISORDERS Dr Ibraheem Bashayreh, RN, PhD 49 29/11/2010 Thyroid Anatomy 1-The gland as seen from the front is more nearly the shape of a butterfly. 2-composed of 2 encapsulated lobes, one on either side of the trachea, connected by a thin isthmus. 3-The thyroid extending from the level of the fifth cervical vertebra down to the first thoracic. The gland varies from an H to a U shape, overlying the second to fourth tracheal rings. 4-The pyramidal lobe is a narrow projection of thyroid tissue extending upward from the isthmus and lying on the surface of the thyroid cartilage. 50 29/11/2010 Thyroid Anatomy 5-The thyroid is enveloped by a thin, fibrous, nonstripping capsule that sends septa into the gland substance to produce an irregular, incomplete lobulation. No true lobulation exists. 6-The weight of the thyroid of the normal nongoitrous adult is: 10-20 g depending on body size and iodine supply. 7-The width and length of the isthmus average; 20 mm, and its thickness is ;2-6 mm. 8-The lateral lobes from superior to inferior poles usually measure 4 cm. and their thickness is 20-39 mm. 51 29/11/2010 Relations of the Lobes 1-Anterolaterally: *The sternothyroid *The superior belly of the omohyoid *The sternohyoid *The anterior border of the sternocleidomastoid 2-Medially: *The larynx & the trachea. *The pharynx & the oesophagus. *Associated with these structures are the cricothyroid muscle & its nerve supply, the external laryngeal nerve. *In the groove between the esophagus and the trachea is the recurrent laryngeal nerve. 52 29/11/2010 Relations of the Lobes 3-Posterolaterally: The carotid sheath with: The common carotid artery, the internal jugular vein, and the vagus nerve. Relations of the Isthmus 1-Anteriorly: The sternothyroids The sternohyoids The anterior jugular veins Fascia & skin. 2-Posteriorly: The second, third, & fourth rings of the trachea. 53 29/11/2010 Venous Drainage 1-The superior thyroid vein: ascends along the superior thyroid artery and becomes a tributary of the internal jugular vein. 2- The middle thyroid vein: follows a direct course laterally to the internal jugular vein. 3- The inferior thyroid veins : 54 follow different paths on each side. The right passes anterior to the innominate artery to the right brachiocephalic vein or anterior to the trachea to the left brachiocephalic vein. On the left side, drainage is to the left brachiocephalic vein. Occasionally, both inferior veins form a common trunk called the thyroid ima vein, which empties into the left brachiocephalic vein. 29/11/2010 Physiology The thyroid follicles secretes tri-iodothyronine(T3)and thyroxin(T4)synthesis involves combination of iodine with tyrosine group to form mono and di-iodotyrosine which are coupled to form T3 andT4. The hormones are stored in follicles bound to thyrogobulin . When hormones released in the blood they are bound to plasma proteins and small amount remain free in the plasma . The metabolic effect of thyroid hormones are due to free (unbound)T3 and T4. 90%of secreted hormones is T4 but T3is the active hormone so, T4is converted to T3 peripherally. 55 29/11/2010 Physiological control of secretion Synthesis and libration of T3 and T4 is controlled by thyroid stimulating hormone(TSH)secreted by anterior pituitary gland. TSH release is in turn controlled by thyrotropin releasing hormone (TRH)from hypothalamus . Circulating T3and T4 exert –ve feedback mechanism on hypothalamus and anterior pituitary gland . So, in hyperthyroidism where hormone level in blood is high ,TSH production is suppressed and vice versa. 56 29/11/2010 Thyroid Hormones 57 Stimulated by Hormone Function T3/T4 h metabolic rate i metabolic rate h protein synthesis i T3/T4 h energy production h TSH Most important hormone in day today regulation of metabolic rate Calcitonin i blood calcium concentration i the reabsorption of Ca and Ph from bones to blood Calcitonin “tones” down serum Ca levels h blood Ca levels 29/11/2010 HYPOTHYRODISM Hypothyroidism is the disease state in humans and animals caused by insufficient production of thyroid hormone by the thyroid gland. INCEDENCE • 30-60 yrs of age • Mostly women Clinical Manifestations: 1. Goiter. 2. Fatigue. 3. Constipation. 4. Weight gain. 5. Memory and mental impairment and decreased concentration. 6. Depression. 7. Menstrual irregularities and loss of libido. 8. Coarseness or loss of hair. 9. Dry skin and cold intolerance. 58 29/11/2010 Clinical Manifestations: 10. Irregular or heavy menses. 11. Infertility. 12. Hoarseness. 13. Myalgias. 14. Hyperlipidemia. 15. Reflex delay. 16. Bradycardia, elevated diastolic BP. 17. Hypothermia. 18. Ataxia. 19. Decreased serum T4,T3 levels. 59 29/11/2010 LABORATORY ASSESSMENT T3 T4 TSH 60 29/11/2010 TREATMENT LIFELONG THYROID HORMONE REPLACEMENT levothyroxine sodium (Synthroid, T4, Eltroxin) IMPORTANT: start at low does, to avoid hypertension, heart failure and MI Teach about S&S of hyperthyroidism with replacement therapy 61 29/11/2010 MYXEDEMA DEVELOPS 62 Rare serious complication of untreated hypothyroidism Decreased metabolism causes the heart muscle to become flabby Leads to decreased cardiac output Leads to decreased perfusion to brain and other vital organs Leads to tissue and organ failure LIFE THREATENING EMERGENCY WITH HIGH MORTALITY RATE With low metabolism metabolites build up inside the cells which increases mucous and water leading to cellular edema Edema changes client’s appearance Nonpitting edema appears everywhere especially around the eyes, hands, feet, between shoulder blades Tongue thickens, edema forms in larynx, voice husky 29/11/2010 PROBLEMS SEEN WITH MYXEDEMA COMA Coma Respiratory failure Hypotension Hyponatremia Hypothermia hypoglycemia 63 29/11/2010 TREATMENT OF MYEXEDEMA COMA Patent airway Replace fluids with IV. Give levothyroxine sodium IV Give glucose IV Give corticosteroids Check temp, BP hourly Monitor changes LOC hourly Aspiration precautions, keep warm 64 29/11/2010 Hyperthyroidism Hyperthyroidism is a condition caused by the effects of too much thyroid hormone on tissues of the body. Although there are several different causes of hyperthyroidism, most of the symptoms that patients experience are the same regardless of the cause. Clinical Manifestations: 1. Heat intolerance. 2. Palpitations, elevated systolic BP. 3. Weight changes. 4. Menstrual irregularities and decreased libido. 5. Increased serum T4, T3. 6. Exophthalmos (bulging eyes) 7. Goiter. 8. Insomnia. 9. Muscle weakness. 10. Heat intolerance. 11. Diarrhea. 65 29/11/2010 Clinical presentation of specific condition THYROIDITIS: Thyroiditis is an inflammation (not an infection) of the thyroid gland. Several types of thyroiditis exist . 1-Hashimoto's Thyroiditis. Hashimoto's Thyroiditis (also called autoimmune or chronic lymphocytic thyroiditis) is the most common type of thyroiditis. Fatigue-Depression-Modest weight gain--Cold intolerance-Excessive sleepiness-Dry, coarse hair-Constipation-Dry skin-Muscle cramps-Increased cholesterol levels-Decreased concentration-Vague aches and pains-Swelling of the legs 2-De Quervain's Thyroiditis. (also called subacute or granulomatous thyroiditis). The thyroid gland generally swells rapidly and is very painful and tender.] Patients will experience a hyperthyroid period as the cellular lining of colloid spaces fails, allowing abundant colloid into the circulation, with neck pain and fever. Patients typically then become hypothyroid as the pituitary reduces TSH production and the inappropriately released colloid is depleted before resolving to euthyroid. The symptoms are those of hyperthyroidism and hypothyroidism. In addition, patients may suffer from painful dysphagia. There are multi-nucleated giant cells on histology.Thyroid antibodies can be present in some cases.There is decreased uptake on isotope scan. 66 29/11/2010 Clinical presentation of specific condition 3-Silent Thyroiditis. Silent Thyroiditis is the third and least common type of thyroiditis.. Silent thyroiditis features a small goiter without tenderness and, like the other types of resolving thyroiditis, tends to have a phase of hyperthyroidism followed by a phase of hypothyroidism then a return to euthyroidism. The time span of each phase is not concrete, but the hypo- phase usually lasts 2-3 months. 67 29/11/2010 Pressure effect: Dysphagia. breathlesness & orthopnoea. Hoarseness. Facial congestion. 68 29/11/2010 Goitre Enlargement of thyroid gland. Classification: Simple (non-toxic) goitre. Toxic goitre. Neoplastic goitre. Inflammatory goitre. 69 29/11/2010 Simple (non-toxic) goitre include: simple hyperplastic goitre (colloid goiter) Cause: -physiological in pregnancy, puberty -iodine definiecy. Appearance: Large, smooth firm, non-tendern goitre Effect: euythyroid & pressure effect. Multinodular goitre. Cause: presence of areas of hyperplasia & areas of hypoplasia in gland. Appearance: Large, irregular, nodular goiter Effect: euythyroid & pressure effect. 70 29/11/2010 Toxic goitre Grave’s disease Cause: Autoimmune disease characterizeby presence of antibodies stimulate TSH receptors in gland. Appearance: Diffuce, nodular, hyperemic gland. Effect: hyperthyroidism. Toxic Multinodular goiter (plummer’s disease) Cause: Toxic effect of MNG Appearance: Large, irregular, nodular goiter. Effect: hyperthyroidism 71 29/11/2010 Neoplastic goitre Include: -benign: adenoma -malignant: papillary, follicular, anaplastic, medullary and lymphoma Cause: -complication of MNG. -radiation Appearance: Enlarged goiter associated with lymphadenopathy Effect: -pressure effect. -euthyroid. -invasive effect 72 29/11/2010 Inflammatory goitre Rediel’s thyroditis Cause: Fibrosis of thyroid Appearance: Enlarged stony hard thyroid Effect: Pressure effect De quervain’s thyroiditis Cause: Viral infection Appearance: Diffuse, firm, tender swelling Effect: Mild hyperthyroidism Hashimoto’s thyroiditis Cause: Autoantibody against thyroid gland. Appearance: Diffuse, enlarged, non-tender goitre Effect: Hypothyroidism 73 29/11/2010 Investigation: Laboratory investigation: -serum T3, T4. -serum TSH. -serum LATS: (Long Acting Thyroid Stimulator) in grave’s disease -thyroid antibodies: in hashimoto’s disease. -serum cholesterol increase cholesterol level in hypothyroidism 74 29/11/2010 LABORATORY ASSESSMENT IN HYPERTHYROIDISM: T3 T4 TSH in Graves disease Radioactive Thyroid Scan Ultrasonography: used to determine goiter or nodules EKG: note tachycardia 75 29/11/2010 Radiological Investigation: -chest and neck x-ray: Show descend of thyroid gland to thorax and mediastanal shifting in retrosternal goitre. -iodine isotopes By i.v injection of I131. Then, use gama rays to show hot and cold nodules. -CT scan Show thyroid size and if there is compression to trachea 76 29/11/2010 Endoscopic investigation: -bronchoscopy: show compression and infiltration of trachea by tumer Biopsy: -fine needle aspiration biopsy. -true-cut biopsy. 77 29/11/2010 DRUG THERAPY Antithyroid drugs: Thioamides: blocks thyroid hormone production; takes time propylthiouracil (PTU) methimazole (Tapazole) carbimazole (Neo-Mercazole) Need to control cardiac manifestations (tachycardia, palpitations, diaphoresis, anxiety) until hormone production reduced: use Beta-adrenergic blocking drugs: propranolol (Inderal, Detensol) 78 29/11/2010 DRUG THERAPY Iodine preparations: Lugol’s Solution SSKI (saturated solution of potassium iodide) Potassium iodide tablets, solution, and syrup ACTION: decreases blood flow through the thyroid gland This reduces the production and release of thyroid hormone Takes about 2 wks for improvement Leads to hypothyroidism 79 29/11/2010 DRUG THERAPY Lithium Carbonate ACTION: inhibits thyroid hormone release NOT USED OFTEN BECAUSE OF SIDE EFFECTS: depressions, diabetes insipidus, tremors, N&V 80 29/11/2010 DRUG THERAPY RADIOACTIVE IODINE THERAPY: Receives RAI in form of oral iodine Takes 6-8 Weeks for symptomatic relief Additional drug therapy used during this type of treatment Not used on pregnant women 81 29/11/2010 SURGICAL MANAGEMENT Why use surgery? Used to remove large goiter causing tracheal or esophageal compression Used for pts who do not have good response to antithyroid drugs TWO TYPES OF SURGERIES: 1. Total thyroidectomy (must take lifelong thyroid hormone replacement) 2. Subtotal thyroidectomy 82 29/11/2010 PREOPERATIVE CARE Patient should become euthyroid before surgery to prevent thyroid crisis. Assessmment vocal cord condition Low weight: Hi protein, hi CHO diet for days/weeks before surgery 83 29/11/2010 PRE-OPERATIVE CARE 1. 2. 3. 84 Antithyroid drugs to suppress function of the thyroid Iodine prep (Lugols or K iodide solution) to decrease size and vascularity of gland to minimize risk of hemorrhage, reduces risk of thyroid storm during surgery Tachycardia, BP, dysrhythmias must be controlled preop 29/11/2010 PREOPERATIVE TEACHING Teach C&DB Teach support neck when C&DB Support neck when moving reduces strain on suture line Expect hoarseness for few days (endotracheal tube) C&DB: cough & deep breathing 85 29/11/2010 POST-OP THYROIDECTOMY NURSING CARE 1. 2. 3. 4. 5. 6. 7. 8. 9. 86 VS, I&O, IV Semifowlers Support head Avoid tension on sutures Pain meds, analgesic lozengers Humidified oxygen, suction First fluids: cold/ice, tolerated best, then soft diet Limited talking , hoarseness common Assess for voice changes: injury to the recurrent laryngeal nerve 29/11/2010 POSTOP THYROIDECTOMY NURSING CARE CHECK FOR 87 HEMORRHAGE 1st 24 hrs: Look behind neck and sides of neck Check for c/o pressure or fullness at incision site Check drain REPORT TO MD CHECK FOR RESPIRATORY DISTRESS Laryngeal stridor (harsh hi pitched resp sounds) Result of edema of glottis, hematoma,or tetany Trach set/airway/ O2, suction CALL MD for extreme hoarseness 29/11/2010 Complication of operation: Hemorrhage Recurrent laryngeal nerve damage. Superior laryngeal nerve damage Hypoparathyrodism Hypothyroidism Septesis Postoperative infection Hypertrofic scaring (keloid) 88 29/11/2010 Thank You !! 89 29/11/2010