* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Human Papillomavirus and Cervical Cancer
Survey
Document related concepts
Trichinosis wikipedia , lookup
Dirofilaria immitis wikipedia , lookup
Henipavirus wikipedia , lookup
Herpes simplex virus wikipedia , lookup
Schistosomiasis wikipedia , lookup
Sarcocystis wikipedia , lookup
Human cytomegalovirus wikipedia , lookup
Neonatal infection wikipedia , lookup
Microbicides for sexually transmitted diseases wikipedia , lookup
Hepatitis C wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Hepatitis B wikipedia , lookup
Sexually transmitted infection wikipedia , lookup
Oesophagostomum wikipedia , lookup
Transcript
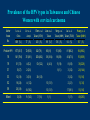
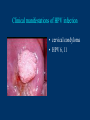
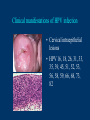
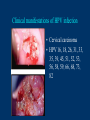
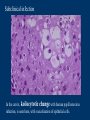
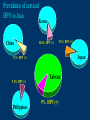
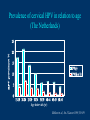
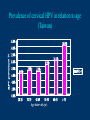
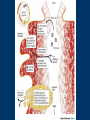
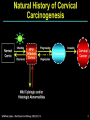
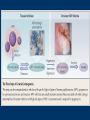
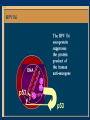
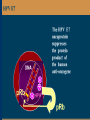
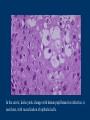
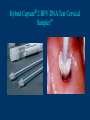
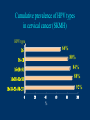
Human Papillomavirus Infection and Cervical Cancer 輔仁大學 實習醫學生 核心課程 新光 吳火獅紀念醫院 婦產科 黃莉文 Human Papillomavirus (HPV) • HPV: species-specific, infect human only. • HPV virion is 55 nm, nonencapsulated, and has an icosahedral capsid. • The genome is a circular double-stranded DNA molecule consisting of 7900 base pairs. HPV infection as the main etiologic factor of cervical cancer • There is now compelling evidence both from biologic and from epidemiologic standpoints to consider HPV infection as the cause of cervical cancer. zur Hausen H, J Natl Cancer Inst 2000;92:690 Viruses linked to Human Tumors Virus types Malignant tumors EBV Burkitt’s lymphoma, NPC HBV Hepatocellular carcinoma HPV 5, 8, 14, 17, 20 Skin carcinoma HPV 16, 18, 31, 33, 35, Cervical cancer, Vulvar cancer, 39, 45, 51, 52, 56, 58, Penile cancer, Anal cancer 59, 61 HTLV-1 Adult T cell leukemia Zur Hausen H, Sciences 1991;254:1167-73 Human diseases associated with HPV infection Sites Skin diseases Deep plantar warts, common warts Anogenital tract Anogenital warts, Bowenoid-papulosis, Cervical, vulvar, and perianal intraepithelial neoplasia, Carcinomas of the cervix, vulva, penis, and anus Juvenile laryngeal papillomatosis, squamous cell carcinoma of the larynx, sinuses, and lung Respiratory tract Other Conjunctival papillomatosis, carcinoma of periungual areas Beutner et al., Am J Med 1997;102:9-15 Human Papillomavirus (HPV) • The more than 200 different HPV genotypes – Less than 90% homology in the L1 ORF with any of the known types • More than 40 HPV types infect the anogenital mucosa – Type 6, 11, 16, 18, 26, 31, 33, 35, 39, 42, 43, 44, 45, 51, 52, 53, 54, 55, 56, 58, 59, 66, 68 (23 types) infect cervical epithelia • HPV 16 is the most prevalent type and found in at least 50% of the cervical cancer Bosch et al., 1995; Walboomers et al., 1999 Human Papillomavirus • • • • • • • Clinical manifestations of HPV Epidemiology of HPV Natural history of HPV Molecular biology and oncogenesis of HPV HPV and CIN HPV and cervical cancer Diagnosis of HPV infection Clinical manifestations of genital HPV infection 1) Clinical infection: condyloma, dysplasia, and cancer 2) Subclinical infection: colposcopic and microscopic identification 3) Latent infection: detectable HPV DNA only Clinical manifestations of HPV infection • • cervical condyloma • HPV 6, 11 Clinical manifestations of HPV infection • Cervical intraepithelial lesions • HPV 16, 18, 26, 31, 33, 35, 39, 45, 51, 52, 53, 56, 58, 59, 66, 68, 73, 82 Clinical manifestations of HPV infection • Cervical carcinoma • HPV 16, 18, 26, 31, 33, 35, 39, 45, 51, 52, 53, 56, 58, 59, 66, 68, 73, 82 Subclinical infection In the cervix, koilocytotic change with human papillomavirus infection, is seen here, with vacuolization of epithelial cells. Prevalence of clinical manifestations of human papillomavirus infection among men and women 15 to 49 years of age in the United States in 1994. 考題 • The infectious agent that is involved in the development of cervical cancer is 1. 2. 3. 4. Herpes virus Chlamydia Syphilis Human papillomavirus (HPV) 考題 • By some estimates, up to what percent of the population is infected with HPV at some point during their lifetime? 1. 10% 2. 25% 3. 50% 4. 75% Prevalence of HPV infection in Taiwan • Prevalence - 9% (N=1624) in normal and abnormal pap smear • HPV 52 > HPV 16 > type 58 91% HPV (-) • May 2000, Taiwan 9% HPV (+) Prevalence of cervical HPV in Asia Korea China 10.4% HPV (+) 9.3% HPV (+) Japan 7.3% HPV (+) 9.2% HPV (+) Philippines Taiwan 9% HPV (+) Prevalence of cervical HPV in relation to age (The Netherlands) 25 20 15 HPV(+) HPV16 or 18 10 5 0 15-19 20-24 25-29 30-34 35-39 40-44 45-49 50-54 Age intervals (yr) Melkert et al., Int J Cancer 1993;53:919 Prevalence of cervical HPV in relation to age (Taiwan) 16.0% 14.8% 14.0% 12.0% 10.0% 8.0% 6.0% 9.2% 6.6% 7.5% 7.3% 30-39 40-49 10.3% HPV(+) 4.0% 2.0% 0.0% 20-29 50-59 Age intervals (yr) 60-69 > 70 Transmission of HPV infection • Sexual – HPV is primarily transmitted through genital-to-genital sexual contact. – Risk increases with the numbers of sexual partners, e.g. from 17% to 83% in women with one and five partners – The number of sexual partners as one of the most significant risk factors for genital HPV infections – The most common time from exposure to HPV to development of genital warts is 4 weeks to 8 months Transmission of HPV infection • Non-sexual – There is no evidence that contaminated toilet seats, doorknobs, towels, soaps, swimming pools or hot tubs, contaminated instruments and underwear can transmit HPV. – Autoinoculation: HPV lesions in one area of the lower genital tract probably already have HPV in other genital tract areas – Vertical transmission from infected mother to her newborn baby. Transmission to the baby of HPV 6 or 11 is known to occur during the birth process but is not common. Transmission of HPV infection • HPV status of partners – 1/3 to 1/2 of couples have been shown to harbor the same HPV type Schneider A et al, Obstet Gynecol 1987;69:554 – The number of extramarital sexual partners a man had was associated with an increased risk of cervical cancer in his wife. Bosch FX et al, J Natl Cancer Inst 1996;88:1060 – In a study of 25 male partners of women with SIL or high-risk HPV, 18 (72%) of the men had detectable HPV DNA. Strand A et al, Acta Derm Venereol 1995;75:312 Natural history of HPV infection -Ho GYL et al., N Engl J Med 1998;338:423 • • • • • • 608 college women, at 6 month intervals for three years The cumulative 36 month incidence of HPV: 43%. The mean duration of new infection was 8 months. By 12 months, 70% of were no longer infected. By 24 months only 9 % continued to be infected. The risk factor for persistent infection of > 6 months were older age, high-risk types, and multiple types of HPV. Will I always have HPV? • The answer to this question is not clear. • Most people (up to 90%) who test positive for HPV with very sensitive tests for HPV (polymerase chain reaction [PCR] and Hybrid Capture 2) will become HPV negative on the same tests within 6 to 24 months from first testing positive. • What is not known is whether this means that the virus is actually eliminated from the body or just suppressed to such a low number of HPVs (as in latency) that even these sensitive tests cannot detect it. Why do most people get very little from being infected with HPV, while others get warts, and a few get cancer? • For most individuals immunity appears to dominate and lesions never develop, or they develop and are suppressed by an immune response before the person ever realizes the presence of the lesions. • Long-term persistence of HPV is not the norm, but is required for the complex interplay of HPV, host immunity, various co-factors, and perhaps, spontaneous mutations in the host cell that may eventually result in the development of cancer of the cervix, vagina, vulva, anus, or penis. Human Papillomavirus and CIN • • • • • • 129 cervix biopsy specimens 85% of low-grade CIN contained HPV DNA 92% of high-grade CIN contained HPV DNA HPV 16: 21% in low-grade, and 57% in high-grade CIN HPV 18: only 3% of CIN HPV 30, 39, 45, 51, 52, 56, 58, and 61 were detected in 44% of low-grade but only 8% of high-grade CIN Bergeron C et al., Am J Surg Pathol 1992;16:641 HPV and Cervical Neoplasms -A case-control study in Taiwan• 88 cases- 40 CIN I, 9 CIN II, 36 CIN III, 3 CC • PCR-bases test: MY09/MY11 • HPV DNA positive – 92% of high-grade (CIN II, III and CC) – 54% of low-grade (CIN I) – 9% of control • HPV-positive high-grade: type 52 and/or 58 (48%) • HPV-positive low-grade: type 52 and/or 58 (25%) Laiw et al, Int J Cancer 1995;62:565 HPV and Cervical Intraepithelial Neoplasia Schiffman, 1993, PCR 51 (28.0-94.0) Olsen, 1995, PCR 67.2 (28.6-157.5) Kjaer, 1996, PCR 18.4 (12.3-27.4) Liaw, 1995, PCR (Taiwan) Wang, 1996, PCR (Taiwan) 122.3 (38.5-388.9) 5.02 (2.54-8.01) 0 1 10 OR and 95% CI 100 HPV and Cervical Carcinoma Munoz, 1992, (Spain, Colombia) 28.8 (15.7-52.6) Eluf-Neto, 1994, (Brazil) 69.7 (28.6-169.9) Chichareon, 1998, (Thailand) 119 (64-222) Ngelangel, 1998, (Philippines) 156 (87-280) Rolon, 2000, (Paraguay) 114 (36-361) 0 1 10 OR and 95% CI 100 Prevalence of HPV in cervical cancer: a worldwide perspective -Bosch FX et al., J Natl Cancer Inst, 1995,87:796• Over 1000 cases with cervical cancer from 32 hospitals in 22 countries – International Biological Study on Cervical Cancer (IBSCC) • HPV DNA was detected in 93% of the tumors • HPV 16 was present in 50% of the Squamous cell tumors – HPV 18 in 14%, HPV 45 in 8%, and HPV 31 in 5% • HPV 18 predominated in adenocarcinomas (56%), and adenosquamous tumors (39%) HPV is a necessary cause of invasive cervical cancer worldwide -Walboomers JMM et al., J Pathol 1999;189:12• The formerly HPV-negative cases from IBSCC– 66 cases • Three PCR-based HPV assays – Type-specific E7, E1 and /or L1 consensus PCR • The world HPV prevalence in cervical carcinomas is 99.7%. Press Release WHO/47 3 July 1996 CERVICAL CANCER: EXPERTS CONFIRMED VIRUS A MAJOR CAUSE, NEW DETECTION TECHNOLOGIES AVAILABLE Experts have formally labelled the human papilloma virus (HPV) types 16 and 18 as "carcinogenic to humans", HPV types 31 and 33 as "probably carcinogenic", and suggested that some other HPV types were "possibly carcinogenic". Epidemiologic classification of HPV types associated with cervical cancer High risk Low risk Lorincz AT 1992 16, 18, 45, 56 31, 33, 35, 51, 52, 58 6, 11, 42, 43, 44 Munoz N IARC 2003 16, 18, 31, 33, 35, 39, 45, 51, 52, 56, 58, 59, 68, 73, 82 (26, 53, 66) 6, 11, 40, 42, 43, 44, 54, 61, 70, 72, 81 (CP8304), CP6180 Participation of oncogenic human papillomavirus E6 in cell cycle regulation. Participation of oncogenic human papillomavirus E7 in cell cycle regulation. For definitions, please refer to the list of abbreviations Do HPV-negative cervical carcinomas exist? • HPV DNA is present but has not been identified (false negative). – Insensitivity of the detection system – DNA integrity – Validity of tumor samples • HPV DNA is not present (true negative). – Hit-and-run mechanism – HPV-independent pathway Diagnostic technique of HPV infection • Pap smear – koilocytosis • Colposcopy • Histopathology – Condyloma, flat, giant, inverted condyloma, papulosis • Hybridization • PCR • serology Screening for Pre-malignant Lesions • PAP smear test is the gold standard –but has limitations*. In the cervix, koilocytotic change with human papillomavirus infection, is seen here, with vacuolization of epithelial cells. Bosch et al., J Clin Pathol 2002;55:244-265 Hybrid Capture® 2 HPV DNA Test Cervical Sampler™ FDA Approves Expanded Use of HPV Test • The HPV DNA test is not intended to substitute for regular Pap screening. • Nor is it intended to screen women under 30 who have normal Pap tests. – Although the rate of HPV infection in this group is high, most infections are short-lived and not associated with cervical cancer. HPV 檢驗晶片 • • • • 子宮頸癌是台灣地區婦女癌症發生率的首位 99%以上的子宮頸癌組織切片可發現人類乳突瘤病毒 目前醫界認為子宮頸癌是『會傳染的癌症』 PCR - DNA Sequencing 並無法鑑別多重病毒感染,市 售HPV檢測產品 無法鑑別 HPV 的基因型 HPV genotypes in cervical cancer worldwide Proper characterization of the distribution of the various HPV types in cervical cancer from different geographic areas is essential to the development of vaccination strategies Type-specific prevalence of HPV in 10058 worldwide cases of invasive cervical cancer Clifford et al., Br J Cancer 2003; 88, 63-73 Type-specific prevalence of HPV in 10058 worldwide cases of invasive cervical cancer Prevalence of HPV Genotypes in Cervical Cancers (SKMH) % 65.9 70 60 50 40 22.8 30 14.4 20 10 0 16 18 31 HPV 9 33 9 58 Prevalence of the HPV types in Taiwanese and Chinese Women with cervical carcinoma Author Lo et al. Lin et al. Chen et al. Areas No. China Jianqxi Taiwan (NTUH) 809 (%) 77 (%) 433 (%) 99 (%)* 136 (%) 94 (%) 167 (%) Positive HPV 677 (83.7) 72 (93.5) 342 (79) 80 (81) 113 (83) 81 (86.2) 164 (98.2) 16 541 (79.6) 37 (48.1) 200 (46.2) 38 (38.4) 86 (58) 45 (47.5) 110 (65.9) 18 51 (7.5) 4 (5.2) 53 (12.2) 4 ( 4.0) 11 (16) 8 ( 8.5) 38 (22.8) 31 5 (0.7) 2 (2.6) 8(5) 3 ( 3.2) 24 (14.4) 33 12 (1.8) 3 (3.9) 3 ( 3.2) 15 ( 9.0) 52 18 (2.6) 4 ( 5.2) 13 (13.1) 2 ( 2.1) 5 ( 3.0) 58 26 (3.8) 14 (18.2) 13 (13.1) 17 (18.1) 15 ( 9.0) Mixed 3 (0.8) 11 (14.3) 1(1) 1 ( 1.1) 49 (29.3) Liaw et al. Taiwan 28 ( 6.5) 7 (1.6) Yang et al. Lai et al. Taiwan (MMH) Taiwan (TSGH) Huang et al. Taiwan (SKMH) Cumulative prevalence of HPV types in cervical cancer the IARC multi-centric case-control study Boschet al., J Clin Pathol, 2002;55(4):244-265 Cumulative prevalence of HPV types in cervical cancer the IARC multi-centric case-control study • Types 16, 18, 45, 31, 33, 52, 58, and 35 accounted for 95 percent of the squamous-cell carcinomas positive for HPV DNA. • They imply that an effective vaccine against the five most common HPV types (types 16, 18, 45, 31, 33) could prevent about 90 percent of the cases of cervical cancer worldwide. Munoz et al., N Engl J Med 2003;348:518 Cumulative prevalence of HPV types in cervical cancer (SKMH) HPV type 66% 16 80% 16+18 84% 16+18+31 88% 16+18+31+58 92% 16+18+31+58+33 0 20 40 % 60 80 100 HPV types 16, 18, 31, 33, and 58 accounted for 90% of the cervical carcinomas in Taiwan From basic studies to clinical applications • Cancer therapy – Therapeutic vaccine – Molecular and chemotherapy • Cancer screening – HPV-based cervical cancer screening program • Cancer prevention – Immunization against type-specific HPV (prophylactic vaccine) HPV-16 L1 VLP vaccine (Merck, 2002) HPV-16 and HPV-18 L1 VLP vaccine (GSK, 2004) HPV-6, 11, 16, 18 L1 VLP vaccine (Merck, 2005) 默克大藥廠表示,臨床試驗結果顯示,一種名為Gardasil的實驗性 疫苗預防子宮頸癌的短期效果可達百分之百。 Gardasil是一種基因 工程合成疫苗,可預防感染兩種人類乳突病毒HPV16、18。這兩 種病毒主要經由性行為傳染,是大約七成子宮頸癌的元凶。 FDA Licenses New Vaccine for Prevention of Cervical Cancer Proper name: Quadrivalent Human Papillomavirus (Types 6, 11, 16, 18) Recombinant Vaccine Tradename: GARDASIL Manufacturer: Merck & Co., Inc., West Point, PA, License #0002 Indication for Use: Vaccination in females 9 to 26 years of age for prevention of the following diseases caused by Human Papillomavirus (HPV) Types 6, 11, 16, and 18: 1. Cervical cancer 2. Genital warts (condyloma acuminata) 3. following precancerous or dysplastic lesions: Cervical adenocarcinoma in situ (AIS) Cervical intraepithelial neoplasia (CIN) grade 2 and grade 3 Vulvar intraepithelial neoplasia (VIN) grade 2 and grade 3 Vaginal intraepithelial neoplasia (VaIN) grade 2 and grade 3 Cervical intraepithelial neoplasia (CIN) grade 1 Approval Date: 6/8/2006