* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Amino acid pool
Survey
Document related concepts
Transcript
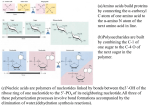
Dr. Walaa AL- Jedda – 2016/2017 Amino acid pool Amino acids, on absorption from intestine are carried to liver through portal blood. They are taken up by liver cells to some extent and remainder enters the systemic circulation and diffuse throughout the body fluid and taken up by tissue cells. At the same time, most of the tissue proteins both "structural" proteins and functional proteins,(including plasma proteins) are continually undergoing disintegration to release amino acids which likewise enter the circulation. There is also a continuous synthesis of amino acids (except the "essential" amino acids). Amino acids from all these sources get mixed up to constitute what is known as "general amino acid pool" of the body."Amino acid pool" has no anatomical reality but represents an availability of amino acid building units. No functional distinction can be drawn between the fate of the amino acids derived from dietary source and those derived from the tissue breakdown. - Amino acids that released by hydrolysis of dietary or tissue protein, or synthesized de novo, mix with other free amino acids distributed through the body, collectively, they constitute the amino acid pool. - The amino acid pool, containing about (100 g) of amino acid, is small in comparison with the amount of protein the body (about 12 Kg in a 70Kg man) - Only about 75% of the amino acids obtained through hydrolysis of body protein are recaptured through the biosynthesis of tissue protein. - The remainder are metabolized or serve as precursor for the nitrogen containing compounds, in addition to the synthesis of carbohydrates and lipids. -The amino acids not used in biosynthesis reactions are burned as a fuel. - The metabolic loss of amino acids is compensated for by dietary protein which contributed to the amino acid pool. Protein turnover -The total amount of protein in the body remains constant, because the rate of protein synthesis is just sufficient to replace the protein that is degraded. -Protein turnover lead to the hydrolysis and resynthesis of (80-100g) of tissue protein or resynthesis of (300-400 g) of body protein each day, about 1/2 of it occurring in the liver. -On an average, plasma proteins are completely replaced every 15 days. -Rate of turnover: The rate of protein turnover varies for individual proteins. - Short-lived protein (many regulatory proteins and misfolded proteins) are rapidly degraded, having half-lives measured in minutes or hours. - Long –lived proteins, with half-lives of days to weeks, constitute the majority of proteins in the cells. - Structural proteins, such as collagen, are metabolically stable, and have half-lives measured in months or years. Nitrogen balance -In an adult healthy individual maintaining constant weight, the amount of intake of N in food( mainly as dietary proteins) will be balanced by an excretion of an equal amount of N in urine ( in form of urea mainly, uric acid, creatinine / and creatine, and amino acids contribute to a minor extent) and in feces ( mainly said to be in " nitrogen balance " or as unabsorbed N). The individual is then " nitrogenous equilibrium". -Nitrogen balance occurs when the amount of nitrogen consumed equal that of the nitrogen excreted in the urine, sweat and feces. -Most healthy adults are normally in nitrogen balance. 1-Positive nitrogen balance: - occurs when nitrogen intake exceeds nitrogen excretion. -it is observed in situations in which tissue growth occurs, for example, in children, pregnancy, or during recovery from an emaciating illness or when anabolic hormones (insulin, GH, and testosterone) are given. 2-Negative nitrogen balance: - occurs when nitrogen loss is greater than nitrogen intake (e.g. in losing weight) -it is associated with inadequate dietary protein, lack of an essential amino acid, or during physiologic stresses such as trauma, burns, illness, or surgery. Essential amino acids: its defined as one which cannot be synthesized by the organism but must be supplied in the diet usually combined in proteins. Exclusion of any one of these essential amino acids leads to( –ve) N-balance manifesting as loss of weight, fatigue, loss of appetite and Nervous irritability. When missing essential amino acid is supplemented in the diet, perfect health is promptly restored. The eight essential amino acids are: valine, leucine, iso-leucine, threonine, methionine, phenylalanine, tryptophan and lysine. Removal of Nitrogen from amino acid - The presence of the α- amino group keeps amino acids safety locked away from oxidative breakdown -Removing the α- amino group is essential for producing energy from any amino acid, and is an obligatory step in the catabolism of all amino acids. -Once removed the α- amino group, the nitrogen can be converted first to NH3 and then to urea and excreted in the urine. - The formation of NH3 and urea can be discussed under the following heads: transamination, deamination, transdeamination, NH3 transport and formation of urea. A. Transamination reactions: Transamination is a reversible reaction involve the transfer of an amino group from one amino acid (which is converted to its corresponding α- keto acid) to an αketo acid (which is converted to its corresponding α- amino acid). Thus, the nitrogen from one amino acid appears in another amino acid, it is a process of combined deamination and amination. 1-The enzymes that catalyze transamination reactions are known as transaminases or aminotransferases. 2-Glutamate and α-ketoglutarate are often involved in transamination reaction, serving as one of the amino acid /α- keto acid pairs. 3- Transamination reaction s is readily reversible and can be used in the synthesis or the degradation of amino acids. 4- Most amino acids participate in transamination reactions. Lysine, Threonine, the cyclic iminoacids and proline are an exception; they are not transaminated. 5- Pyridoxal phosphate (PLP) or( B6P) as the cofactor for transamination reactions. PLP is derived from vitamin B6. 6-Transaminases take place principally in liver, kidney, heart and brain. Enzymes are normally intracellular enzymes found in almost all tissues, with the low levels found in the plasma representing the release of cellular contents during normal cell turnover. 7-The presence of elevated plasma levels of transaminases indicates damage to cells rich in these enzymes. B- Deamination: (Removal of amino acid nitrogen as ammonia) In contrast to transamination, a number of amino acids undergo oxidative deamination in which their nitrogen is released as ammonia or ammonium ion (NH4+). It can be in two types: oxidative deamination and non-oxidative deamination -Glutamate dehydrogenase catalyzes the oxidative deamination of glutamate. Ammonium ion is released, and α- ketoglutarate is formed. The glutamate dehydrogenase reaction, which is readily reversible, requires NAD or NADP. These reactions occur primarily in the liver and kidney. C- Transdeamination (deamination of L-Glutamic acid) The involvement of transamination and coupled with oxidative deamination, the process is called transdeamination. This mechanism seems to be the major pathway for removal of NH2 group from an L-amino acid and formation of NH3. The enzyme L-glutamate dehydrogenase catalyzes the deamination of L-glutamate to form α- iminoglutaric acid, which on addition of a molecule of water forms NH3 and α-keto glutarate. D- NH3 Transport: in addition to NH3 formation in the tissues, a considerable quantity of NH3 is produced in the gut by intestinal bacterial flora, both -from dietary proteins, and -from urea present in fluids secreted into GI tract. Other sources of NH3 are: 1-From amino acid: Many tissues, but particularly the liver, form ammonia from amino acids by series of transamination and deamination reactions. 2- From glutamine: a. The kidneys form ammonia from glutamine by the action of renal glutaminase. - Most of this ammonia is excreted into the urine as NH4+, which provides an important mechanism for maintaining the body acid-base balance. b. Ammonia is also obtained from the hydrolysis of glutamine by intestinal glutaminase. -The intestinal mucosal cells obtained glutamine either from the blood or from digestion of dietary protein. 3- From bacteria action in the intestine. - Ammonia is formed from urea by the action of bacterial urease in the lumen of the intestine. - This ammonia is absorbed partly from intestine by the way of the portal vein and removed by the liver via conversion to urea, and partly lost in the feces. - The intestinal action of urease on the urea becomes a clinically important source of ammonia contributing to the hyperammonemia especially in those patients with renal or hepatic failure. Oral administration of Neomycine reduces the number of intestinal bacteria responsible for this NH3 production. 4- From amines Amines obtained from the diet, and monoamines that serves as hormones or neurotransmitters, give rise to ammonia by the action of amine oxidase. 5- From purines and pyrimidines In the catabolism of purines and pyrimidines, amino groups attached to the rings are released as ammonia. -This NH3 is absorbed from the intestine into portal venous blood which contains relatively high concentration of NH3 as compared to systemic blood. - Under normal conditions of health, liver promptly removes the NH3 from the portal blood, so that blood leaving the liver is virtually NH3- free. This is essential since even small quantities of NH3 are toxic to CNS. Why NH3 is toxic? The cause of NH3 toxicity is not definitely known. Following associated biochemical changes are important. -Increased NH3 concentration enhances amination of α-ketoglutarate, an intermediate in TCA cycle to form glutamate in brain. This reduces mitochondrial pool of α-ketoglutarate consequently depressing the TCA cycle, affecting the cellular respiration. - Increased NH3 concentration enhances "glutamine" formation from glutamate and thus reduces" brain-cell" pool of Glutamic acid. Hence there is decreased formation of inhibitory neurotransmitter "GABA"( γ- amino butyric acid) . - Rise in brain glutamine level enhances the outflow of glutamine from brain cells. Glutamine is carried "out" by the same "transporter" which allows the entry of "tryptophan" into brain cells. Hence "tryptophan" concentration in brain cells increases which leads to abnormal increases in synthesis of " serotonin", a neurotransmitter. Metabolic fate of NH3 in the body: Three main fates: 1-mainly NH3 is converted to urea (urea cycle) 2-formation of glutamine. 3-amination of α-keto acid to form α-amino acid. Clinical Aspect : Hyperammonemia -The capacity of the hepatic urea cycle exceeds the normal rates of ammonia generation. -Serum ammonia levels are normally low (40-70µg / 100 ml), free NH4+conc. is less than( 20 µg / 100 ml). -Hyperammonemia is associated with comatose states such as may occur in hepatic failure. -Hyperammonemia may be of 2 types: a. Acquired Hyperammonemia: liver disease is the common cause in adults, it may be due to : 1-Acute process (viral hepatitis, ischemia, hepatotoxins) 2- Chronic process (cirrhosis due to alcoholism, hepatitis, billiary obstruction). -The detoxification of ammonia (conversion to urea), is severely impaired leading to elevated levels of circulating ammonia. b. Hereditary Hyperammonemia: - Genetic deficiencies of each of the five enzymes of the urea cycle. - In each case, the failure to synthesize urea leads to hyperammonemia during the first weeks following birth. - All inherited deficiencies result in mental retardation. - Treatment includes limiting protein in diet, and administrating compounds that bind covalently to amino acid producing nitrogen- containing molecules that excreted in the urine. -Phenyl butyrate given orally is converted to phenyl acetate which condenses with glutamine to form phenylacetylgutamine which is excreted. Features of NH3 intoxication: The symptoms of NH3 intoxication include: - a peculiar flapping tremor - slurring of speech - blurring of vision - and in severe cases follows to coma and death. These resemble those of syndrome of hepatic coma, where blood and brain NH3 levels are elevated. Urea Cycle Urea is formed in the urea cycle from NH4+ , CO2 , and the nitrogen of aspartate. The cycle occurs mainly in the liver. Ammonia, which is very toxic in humans,( particularly to the central nervous system), is converted to urea , which is nontoxic, very soluble, and readily excreted by kidneys. -The concentration of ammonia and ammonium ions in the blood is normally very low. (NH3 + H+ NH4+) - This is due to the rapid removal of blood ammonia by the liver, and the fact that many tissues particularly, muscles, release amino acid nitrogen in the form of glutamine or alanine rather than ammonia. A- Reactions of the urea cycle NH4+and aspartate provide the nitrogen that is used to produce urea and CO2 provides the carbon. Ornithine serves as a carrier that is regenerated by the cycle. The reactions of urea cycle can be studied in five enzymatic reactions: - Reaction 1: Synthesis of carbamoyl- phosphate - Reaction 2: Synthesis of citrulline - Reaction 3: Synthesis of argininosuccinate - Reaction 4: Cleavage of argininosuccinate - Reaction 5: Cleavage of arginine to form ornithine *Only the liver can cleave arginine and, thereby, synthesize urea. - Urea passes into the blood and is excreted by the kidneys. -The urea excreted each day by a healthy adult (about 30 g ) accounts for about 90% of the nitrogenous excretory products. The overall process in each turn of cycle requires 3 moles of ATP. -The overall reaction of the urea cycle: Aspartate + NH3 + CO2 +3 ATP Urea + Fumarate + 2 ADP + 2Pi + PPi +3 H2O B- Significance of urea cycle: 1- Detoxification of NH3 : Toxic ammonia is converted into a nontoxic substance urea and excreted in urine. 2- Biosynthesis of Arginine :the arginine is used for protein synthesis. Clinical significance of urea: 1-Normal level: the normal concentration of blood plasma in healthy adult ranges from 20-40 mg/dl 2- Increase levels(uremia): may occurs in a number of diseases, the causes can be classified as: a- Pre-renal: most important are conditions in which plasma vol / body-fluid are reduced: -salt and water depletion, -sever and protracted vomiting as in pyloric and intestinal obstruction, -sever and prolonged diarrhea, -hemorrhage and shock; due to severe burns,.. b- Renal: The blood urea can be increased in all forms of kidney diseases like: - in acute glomerulonephritis, - in early stages of type II nephritis(nephrosis), malignant nephrosclerosis, mercurial poisoning, renal tuberculosis,.. c-Post-renal diseases: these lead to increase in blood urea, when there is obstruction to urine flow. The causes are: enlargement of prostate, stones in urinary tract, stricture of the urethra, tumors of the bladder affecting urinary flow. 3- Decreased levels: are rare, but may be seen in: - some cases of severe liver damage. -physiological condition: blood urea is lower in pregnancy than in normal non pregnant women.