* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download 5 Paediatric cardiology
Cardiac contractility modulation wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Cardiovascular disease wikipedia , lookup
Electrocardiography wikipedia , lookup
Aortic stenosis wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Heart failure wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Coronary artery disease wikipedia , lookup
Cardiothoracic surgery wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Myocardial infarction wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Atrial septal defect wikipedia , lookup
Congenital heart defect wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
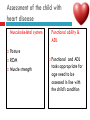
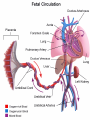
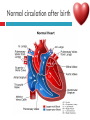
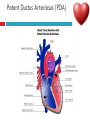
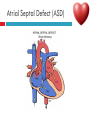
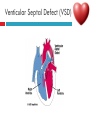
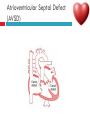
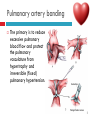
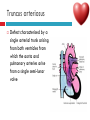
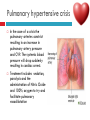
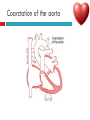
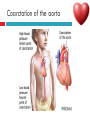
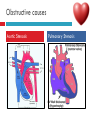
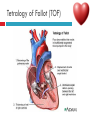
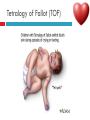
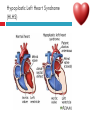
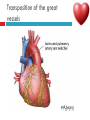
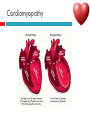
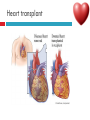
PAEDIATRIC CARDIAC DISORDERS Robyn Smith Department of Physiotherapy, UFS, 2011 Dealing with a child with cardiac dysfunction is often disconcerting and we are often unsure of how to proceed this lecture aims to provide an overview of common heart pathology in children and the physiotherapy management thereof Background Congenital heart defects (CHD) occur in 1% of the live births (6 of every 1 000) Most common congenital abnormality seen Approximately 1/3 of these children will require surgery, whilst the rest of the cases resolve spontaneously or are deemed haemodynamically insignificant Early surgical intervention is recommended to limit CVS and neurodevelopmental complications. Most children are operated on before 1 year of age Background Mortality for children with CHD has decreased significantly ( ≤ 5 %) as a result of medical and surgical advances, and many of these children are surviving well into adulthood. The decreasing mortality rates has resulted in the shift in focus to the neurodevelopmental status of these children and ways of addressing the associated developmental delays Background As PT’s we will encounter children with CHD in all clinical settings we work in Acute care setting – pre/postoperatively Sub-acute care setting in the ward Out patient department As PT’s we need to know: What CHD is Types of cardiac disorders How the child’s CVS system is affected during exercise Prevalent complications associated CHD Aetiology In most cases of CHD the aetiology is multi-factorial and include genetic inheritance (patterns not yet clear) Maternal conditions Environmental factors Above factors interact during the first 8-10 weeks of gestation a critical development phase of the heart Cardiac Physiology in the infant Normal foetal circulation Foetal heart in not dependant on the lungs for respiration. Instead the placenta is used for gaseous exchange. The R and L ventricles exist in a parallel circuit Blood travels through the umbilical vein through the ductus venosus to the foetal heart via the IVC to the RA and through the foramen ovale to the LA The SVC leads to the RA to the RV to the pulmonary artery to the lungs or ductus arteriosus bypassing the lungs into the descending aorta to perfuse the lower extremities and the body, travelling back to the placenta via the umbilical arteries. Normal foetal circulation The blood travelling through the left ventricle to the aorta perfuses the upper extremities and the brain. All of the blood flowing through the chambers of the heart, arteries and veins is rich in Oxygen The vessels for pulmonary circulation in the foetus are vasoconstricted. All blood travelling in the arteries to the lungs is oxygen rich and contributes to the nourishment of the lung tissue Changes in the circulatory system at birth As the baby takes its first breath the lungs expand, causing the lung P to fall. This allows the blood to move more easily into the lung. After reaching the lungs and being oxygenated the blood is moved to the LA. The P on the L side of the atrial septum becomes higher than on the R causing the foramen ovale to gradually close (closed by 3/12) Once the lungs are filled with air and the oxygen level in the child’s blood rises the muscle wall of the ductus arteriosus contracts no longer allowing blood to flow through the ductus. The ductus arteriosus closes 10-15 hours after birth. Now child has separate oxygenated and de-oxygenated blood and relies fully on the lungs for gaseous exchange Normal circulation after birth Common heart disease in children Congenital heart defects At any point in the development of the cardiac system problems can arise leading to congenital heart disease. CHD can be classified into two main groups: lesions ( ↓O2 saturation in the blood) Acyanotic lesions (O2 saturation unaltered, but can result in pressure or volume related issued) Cyanotic Common cardiac conditions seen in children Acyanotic Congenital Heart Defects Classification of Acyanotic heart lesions Coarctation of aorta Pulmonary stenosis Aortic stenosis Patent ductus arteriousus Atrial septal defects Ventral septal defects increased pulmonary bloodflow Atrioventricular septal defects with shunting O2 rich blood from obstructive in nature left to right “PINK BABY” Patent Ductus Arteriosus (PDA) The ductus arteriousus is the foetal vascular connection between the main pulmonary trunk and the aorta which under normal circumstances closes soon after birth (usually within the first week of life). If it stays open excessive blood shunts from the aorta ton the lungs Causing pulmonary oedema and in the long run pulmonary vascular disease Symptoms may vary from mild to severe depending on the magnitude of the shunt Very common in premature infants and may further complicate weaning from the ventilator and result in CHF Patent Ductus Arteriosus (PDA) clinical signs and symptoms of significant PDA Poor feeding Failure to thrive (below weight for and height for age) Sweating with crying or play Persistent tachypnoea or breathlessness (dyspnoea) Easy tiring Tachycardia Frequent lung infections A bluish or dusky skin tone Developmental delay Patent Ductus Arteriosus (PDA) Patent Ductus Arteriosus (PDA) Management Closing of PDA can be induced using medication (indomethacin) Surgically Surgical correction is done via a thoracotomy Atrial Septal Defect (ASD) An ASD is an opening or whole in the wall separating the atria This permits free communication of blood between the two atria. Seen in 10% of all congenital heart disease Rarely presents with signs of congestive heart failure or other cardiovascular symptom Most are asymptomatic but may have easy fatigability or mild growth failure. The right atrium and ventricle may enlarge over time Cyanosis does not occur unless pulmonary hypertension is present. Atrial Septal Defect (ASD) Atrial Septal Defect (ASD) Management: Surgical or catheterization closure is usually indicated Closure is performed electively between ages 2 & 5 yrs if the whole has not closed in order to avoid late complications. Children may be on anticoagulant therapy for 6 months to prevent clotting Surgical correction is done earlier in children with congestive heart failure or significant pulmonary hypertension Venticular Septal Defect (VSD) A VSD is an abnormal opening in the ventricular septum, which allows free communication between the right and left ventricles ventricles. Oxygen rich blood in the left ventricle is then pumped into the right ventricle through the opening instead of to the body. In a large VSD excessive blood is pumped to the lungs resulting in congestion and shortness of breath. In return excessive amounts of blood are pumped back from the lungs to the left heart overburdening and enlarging it resulting in CHF Venticular Septal Defect (VSD) In case of a small VSD most children are asymptomatic and 50% will close spontaneously by age 2yrs In the case of a moderate or large VSD the child will be symptomatic. This may include dyspnoea, feeding difficulties, failure to thrive recurrent respiratory infections and profuse sweating Venticular Septal Defect (VSD) Venticular Septal Defect (VSD) Management In case of a small VSD 50% will close spontaneously by age 2yrs Large VSD’s are usually closed surgically Atrioventricular Septal Defect (AVSD) AVSD results from the incomplete fusion of the tendocardial cushions, which help to form the lower portion of the atrial septum, the membranous portion of the ventricular septum and the septal leaflets of the triscupid and mitral valves. They account for 4% of all CHD Commonly associated with chromosomal disorders Down Syndrome Clinical findings include CHF in infancy, recurrent respiratory infections, failure to thrive, exercise intolerance and easy fatigability. Atrioventricular Septal Defect (AVSD) Atrioventricular Septal Defect (AVSD) Treatment Surgery is always required. Prior to surgery congestive symptoms are treated. Pulmonary banding maybe required in premature infants or infants < 5 kg. Correction is done during infancy to avoid irreversible pulmonary vascular disease. Pulmonary artery banding The primary is to reduce excessive pulmonary blood flow and protect the pulmonary vasculature from hypertrophy and irreversible (fixed) pulmonary hypertension. Truncus arteriosus Defect characterised by a single arterial trunk arising from both ventricles from which the aorta and pulmonary arteries arise from a single semi-lunar valve Pulmonary hypertensive crisis Can be a severe complication post operatively Children at risk of pulmonary hypertension are those with excessive shunting of blood from left to right e.g. VSD, AVSD This results in excessive bloodflow to the lungs resulting in distension and damage to the pulmonary artery wall which becomes muscularised Unable to dilate and vulnerable to reactive vasoconstriction Hypoxaemia, hypercapnea, metabolic acidosis as well as relentless handling (including by the physiotherapist) and tracheal suctioning may predispose the child to a hypertensive crisis. In children at risk physiotherapy should be indicated, treatment must be quick and effective and vitals need to be monitored. Effective sedation, paralysis and additional oxygen may be required to avoid a crisis. Pulmonary hypertensive crisis In the case of a crisis the pulmonary arteries constrict resulting in an increase in pulmonary artery pressure and CVP. The systemic blood pressure will drop suddenly resulting in cardiac arrest. Treatment includes sedation, paralysis and the administration of Nitric Oxide and 100% oxygen to try and facilitate pulmonary vasodilatation Obstructive causes of CHD Coarctation of the aorta Congenital narrowing of the aorta as it leaves the heart anywhere from the transverse arch to the iliac bifurcation. Resulting in increased pressures in the arteries nearest the heart, head and arms and decreased circulation in lower extremities. 7 % of all CHD Male: Female ratio 3:1 Coarctation of the aorta This is often not evident in the newborn until the ductus arterious closes causing a constriction. The blood in the left ventricle has then to be pumped out against the constriction. Child presents with symptoms of left ventricular hypertrophy and left ventricular failure, with congestive heart failure. Changing a healthy baby into a baby that has hard breathing, is sweaty and wheezing. Coarctation of the aorta Coarctation of the aorta Coarctation of the aorta Management: With severe coarctation maintaining the ductus with prostaglandin E is essential Early surgical repair and resection of the stenosis is imperative Simple coarctation repair have a extremely low mortality but in complex cases mortality might be higher A rare complication of surgical repair is paraplegia (longer cross clamping times during surgery) In 18% of children undergoing surgery re-coarctation occurs Obstructive causes Aortic Stenosis Is an obstruction to the outflow from the left ventricle at or near the aortic valve. Resulting in left ventricular overload and hypertrophy Pulmonary Stenosis Is obstruction in the region of either the pulmonary valve or the sub-pulmonary ventricular outflow tract. Pulmonary circulation decreased Work of the RV increased RV hypertrophy ↓ cardiac output Accounts for 7% of CHD. Accounts for 7-10% of all CHD. Obstructive causes Aortic Stenosis Asymptomatic in mild cases, in more severe cases fatigue, syncope and dyspnoea Treatment is surgical repair Pulmonary Stenosis Symptoms include dyspnoea, exercise intolerance, fatigue CHF and hypoxaemia Treatment is surgical repair Obstructive causes Aortic Stenosis Pulmonary Stenosis Cyanotic Congenital Heart Defects Classification of cyanotic heart lesions Cyanotic heart lesions include: Tetralogy of Fallot Hypoplastic left heart Trasposition of the great vessels Tetralogy of Fallot (TOF) Most common cyanotic heart lesion Has 4 components: A high VSD Pulmonary stenosis Anomalous position aorta RV hypertrophy Results in a right to left shuntting of blood with low oxygen levels in the artieires and in the body tissues Resulting in cyanosis, easy fatigability, fainting and shock. Clubbing may be observed Tetralogy of Fallot (TOF) Tetralogy of Fallot (TOF) Tetralogy of Fallot (TOF) Early surgical intervention (TOF repair) is usually required Palliative care by means of anestomosis and pulmonary valvotomy can be done Hypoplastic Left Heart Syndrome (HLHS) Most serious congenital heart malformation with the poorest of prognosis Means that the left ventricle is extremely small and the mitral valve and aortic valves may be missing Symptoms usually minimal until the ductus arteriosus closes causing shock and multi-organ failure Hypoplastic Left Heart Syndrome (HLHS) Treatment prpstaglandin E1 until surgery Initial palliative surgeries Heart transplant is often the suggested option Hypoplastic Left Heart Syndrome (HLHS) Other Congenital Heart Defects Transposition of the great vessels Aorta arises from the RV and the pulmonary arteries arise from the LV The 2 circulations namely the systemic and pulmonary are in parallel instead of in series Venous blood circulates around the body and oxygenated blood around the lungs May be dyspnoea, cyanosis and syncope Transposition of the great vessels Transposition of the great vessels Treatment Palliative surgeries including pulmonary banding or atrial septum excision Corrective surgery Non Congenital Heart Disease Cardiomyopathy Primary heart muscle disease Cardiomyopathy is a chronic and sometimes progressive disease in which the heart muscle is abnormally enlarged, thickened and/or stiffened. The condition typically begins in the walls of the ventricles and in more severe cases also affects the walls of atria) The actual muscle cells as well as the surrounding tissues of the heart become damaged. Hallmark is depressed cardiac functioning. Eventually, the weakened heart loses the ability to pump blood effectively and heart failure or irregular heartbeats (arrhythmias or dysrhythmia) may occur. Cardiomyopathy Cardiomyopathy "primary cardiomyopathy" where the heart is predominately affected and the cause may be due to infectious agents or genetic disorders "secondary cardiomyopathy" where the heart is affected due to complications from another disease affecting the body e.g. HIV, cancer, muscular dystrophy or cystic fibrosis Cardiomyopathy Cardiomyopathy can affect a child at any stage of their life. It is not gender, geographic, race or age specific. Rare disease in infants and young children. Cardiomyopathy continues to be the leading reason for heart transplants in children. Complications may include arrythmias, heart block, blood clots, congestive heart faiulure, endocarditis and sudden death Organ Transplantation Heart transplant Heart transplantation is used only as an option in end stage heart failure in children with heart defects or cardiomyopathies that are unresponsive to surgery or medication Heart failure may occur in children with CHD postoperatively due to the nature of their artificial circulations Individual units have their own transplant protocols A heart transplant presents a ling risk of organ rejection and infection The transplant half life of children is estimated at 18 years Heart transplant Physiotherapy Assessment Assessment of the child with CHD History Will need to conduct an interview with the family: Children often have a very long and complicated medical and often surgical history that has to be well document Medications that the child is taking e.g. blood thinners, and immunosuppressant drugs Social, economic and family circumstsances need to be determined (CHF highly stressful to the family unithigh divorce rate) Developmental history –these children often present with developmental delays Is child receiving any early intervention services e.g. physio/OT Child’s general health Sleeping patterns’ Current and previous level of functioning ADL – if child of schoolgoing age is he attending school. What is their chief complaint with the child: Most common complaint from parent with children awaiting surgery is failure to thrive and poor feeding. I In older children it is often lethargy, fatigue Assessment of the child with CHD Interview with paediatric cardiologist Nature of the CHD Intervention and treatment planning Precautions Need for physiotherapeutic intervention Assessment of the child with heart disease Oxygenation –laboratory results Vital sign parameters Arterial blood gas values and saturation monitor reading are incredibly important when assessing a patient with cardiac dysfunction Cyanotic lesions the ABG may be reduced due to the mixing of arterial and venous blood The following reading need to be taken manually or read off the monitor HR, RR, BP prior to your assessment to serve as baseline values Important to retake vital signs during assessment and after as well Assessment of the child with heart disease PaO2 60-80 mmHg PaO2 40-60 mmHg PaO2 ≤ 40 mmHg = SaO2 ≤ 60% = SaO2 60-90% = SaO2 90-95% Mild hypoxaemia Severe hypoxaemia Assessment of the child with heart disease General observations Child’s LOC – is he sedated, on a neuromuscluar blocker (paralysis) in children where any movement or position changing has a negative impact on the CVS function) Equipment and indwelling devices Pain Integrity of the skin Surgical sites and wounds e.g. sternotomy/ thoracotomy Clubbing Oedema Capillary refill Cyanosis central and peripheral Assessment of the child with heart disease Respiratory system Chest shape Chest deformities Chest expansion Thoracic mobility; flexion, extension, lateral flexion, rotation Breathing pattern Shoulder girdle tightness and mobility Shortness of breath (tachypnoea) Dyspnoea and grade Cough Sputum Auscultation If ventilated –ventilator settings Assessment of the child with heart disease Musculoskeletal system Posture ROM Muscle strength Functional ability & ADL Functional and ADL tasks appropriate for age need to be assessed in line with the child’s condition Assessment of the child with heart disease Aerobic capacity, endurance and exercise tolerance In younger children observe during activity and play- monitor HR In older child can do the 6 min. walk test Shortness of breath can objectively be monitored through the ventilatory index in older children Can also use the dyspnoea index or Borg scale but it is often subjective and difficult in children Ventilatory index child must inhale deeply and count to 15 (8 seconds) 0 1 2 3 4 • Count aloud to 15 without taking a breath • Count aloud to 15 taking 1 breath • Count aloud to 15 taking 2 breaths • Count aloud to 15 taking 3 breaths • Count aloud to 15 taking 4 breaths Dyspnoea Index 1 2 3 4 • Breathlessness barely noticeable • Breathlessness moderately bothersome • Breathlessness severe and very uncomfortable • Most severe breathlessness ever experienced Borg scale of perceived exertion 6-8 8-10 • Very, very light • Very light 10-12 • Fairly light 12-14 • Somewhat hard 14-16 • Hard 16-18 • Very hard 18-20 • Very, very hard Preoperative physiotherapy Seeing the child prior to surgery affords the physiotherapist the opportunity to get to know the child and their family, makes the post-operative period far easier. Provides an opportunity to do a quick respiratory, developmental and functional assessment In other cases it might be a child you know well from previous inpatient/out patient visits to adress recurrent respiratory tract infections and neurodevelopmental delays Explain the operation in simple terms and tell him/her and the parents about the post operative stay in PICU (lines, ventilator ,ET tubes etc.). Also indicate the post-operative role of the physiotherapist. Preoperative physiotherapy aims Maintain joint ROM, circulation and function preoperatively Correct posture and positioning in bed CPT if indicated to clear secretions and breathing exercises Teach older child how to cough with wound/chest support Maintain functional abilities as cardiovascular status allows Postoperative physiotherapeutic problems Pain –see child has adequate sedation Decreased air entry Retained secretions Ineffective cough –must cough with wound support Reduced UL movements Decreased mobility Family and caregiver education Postoperative physiotherapy Avoid physiotherapy in the first few hours after surgery as they are aiming to stabilise the child and achieve haemodynamic stability The exception to the rule here may be in the case of a lobar collapse on the post-operative CXR or poor ABG. In this case careful physiotherapy is to be done avoiding any deterioration in haemodynamic status Postoperative physiotherapy When not to treat Confidence in treating cardiothoracic patient only comes with experience, but accurate assessment will reveal the needs of the child: Treatment should be avoided in the following cases: Haemodynamic instability Tachycardia or bradycardia Hyper/hyptensive Child in a pulmonary hypetensive crisis Postoperative physiotherapeutic intervention Intubated in the ICU Localised breathing exercises if child awake and of age or tactile neurophysiological stimulation Modified postural drainage positions are used as the head down position may compromise cardiac output and diaphragm functioning Mechanical vibrations, gentle percussions (ensure adequate analgesia) and suctioning to remove secretions Must give chest support when coughing Bilateral UL mobility above 90 degrees Correct positioning for ventilation and posture Postoperative physiotherapeutic intervention Extubated in the ICU Children are usually extubated quickly unless underlying lung pathology or secondary infection. Teach huffing & coughing with chest support Localised and lateral basal breathing exercises or can use blowing pin-wheel, bubbles, incentive spirometry Manual CPT techniques if indicated Functional activities e.g. teaching log rolling, coming up into sitting Active bed exercise programme Older child can sit out in a chair in the unit Postoperative physiotherapeutic intervention Ward Exercise rehabilitation in paediatric patients Mobilisation can be start once inotropic drugs stopped and some of drains removed Studies in children show an improvement in work capacity & VO2 max following a 6-8 week rehabilitation exercise programme Not much research has been done on rehabilitation exercise programmes in children Postoperative physiotherapeutic intervention Ward Exercise rehabilitation in paediatric patients An at risk group for exercise..... There is a small population of children who are at risk of sudden death ( hypertrophic cardiomyopathy, coronary artery anomalies, Marfan Syndrome, Aortic valve stenosis and long QT syndrome)with physical activity and sport participation. These children need to be identified and restriction placed on competitive sport and high intensity physical activity Postoperative physiotherapeutic intervention Ward Start with activity and endurance training Allow older child to walk, cycle and stair climb (can be taught to monitor own HR) Smaller children uses play and functional activities Pay attention to the following principles mode : walking, cycling Duration (sick children shorter intensity e.g. 3-5 minutes Frequency (3-5/wk) Intensity: monitor exhaustion, dyspnoea and HR (not a rise of ≥ 20 beats) In older children where stress ECG can be done, the child can exercise at 60 -65% of maximal HR Postoperative physiotherapeutic intervention Ward and out patient basis Aerobic and endurance training Not all patients e.g. Left to right shunt have impaired exercise tolerance where in some cases children with cyanotic heart lesions and severe abnormalities may have impaired exercise tolerance due to the hypoxemia Exercise tolerance is also often affected by recurrent hospitalisations, inactivity and periods of bed rest Therefore post operatively there must be a progressive exercise plan aiming to improve the child’s cardiovascular fitness and endurance Postoperative physiotherapeutic intervention Ward and out patient basis Aerobic and endurance training Over time children that have had a complete defect repair at an early age should have normal cardiovascular functioning-with normal age expected exercise tolerance and endurance In cases where complete repair was not possible and cardiac functioning still impaired the child have to monitor HR and signs of fatigue can aim at improving endurance and at least maintaining it where possible Sporting activity in cases of impaired cardiac function needs to be reviewed by the interdisciplinary team Postoperative physiotherapeutic intervention Ward and out patient basis Strength training General strength training may be undertaken preand postoperatively although there is a 6-8 week postoperative restriction on lifting activities for children Important that children breathe correctly during resistance training in order not to increase the blood pressure Postoperative physiotherapeutic intervention Ward and out patient basis Neurodevelopmental outcomes in children with heart disease: CHD often has a significant impact on a child’s development Cause of delays are often multifactorial Child with CHD may have brain insults prior to surgery due to prolonged hypoxaemia Studies have found that children with CHD show delays in all main areas of development as well as tonal abnormalities (hypotonia), abnormal posture emotional and behavioural difficulties Following open heart surgery children may suffer from mild hypotonia, motor problems and CMD may occur in 5% of cases. Postoperative physiotherapeutic intervention Ward and out patient basis Neurodevelopmental outcomes in children with heart disease: language development also delayed in many cases. Even at one year after surgery most children were still behind for age. Delayed gross and fine motor development also impacted negatively on perceptual skills. Children often exhibited behavioural problems and greater caregiver dependency Postoperative physiotherapeutic intervention Ward and out patient basis Neurodevelopmental therapy Age appropriate play is an important activity that can be used in order to get a child to move In cardiac patient it is often important to then try and get the child accustomed to prone over towel enven on a caregivers lap during awake, play time. Prone is an important developmental position. Nerodevelopmental assessment and therapy to aid the child in catching up on his age appropriate milestones is often essential post operatively especially in younger children who were acutely ill and failed to thrive. Regular developmental monitoring would also be recommended Family and caregiver support A family suffers huge amounts of anxiety and stress in the case of having a child with CHD The distress, frustration and reaction shown by the mother may affect the relationship with the child Often over-restriction and over-observation of children with CHD by parents The child’s reaction and adjustment to their illness is largely related to the emotional and behavioural reaction of the family Physiotherapist can play an important role by providing support and encouraging more positive interactions within the family References Ammani Prasad, S. & Main, E. Paediatrics in Physiotherapy for respiratory and cardiac Problems. Adults and children 4th ed. Pryor, J.A. & Ammani Prasad, S. (eds.)358-363 E-medicine. 2010. pulmonary artery banding. Available online at: http://emedicine.medscape.com/article/905353-overview Hendon. K.L. Not dated. Congenital Heart Disease (slideshow) Children’s Cardiomyopathy Foundation. 2010. About the disease. Available online at: http://www.childrenscardiomyopathy.org/site/description.php References Pepper, J.R.; Anderson, J.M. & Innocenti, D.M. 1992. Cardiac surgery in Cash’s Textbook of chest, Heart and Vascular disorders for Physiotherapists. 4th ed. Downie, P.A. (ed). Mosby, london pp 407429 Bar-Or, O. & Rowland, T.W. 2004. Cardiovascular disease in Paediatric exercise medicine. From physiological principles to healthcare application. Human Kinetics, USA Pp177-217 Brossman, H. 2008. Cardiac disorders in Pediatric Physical Therapy. 4th ed. Telin, J.S. (ed.). Lippincott williams Wilkins, Baltimore pp 589609 References Main, E. 1998. Paediatric Cardiothoracic Surgery in Paediatric Management in Cardiovascular/Respiratory Physiotherapy.Smith, M. & Ball,V. (eds.).Mosby, London pp291-298 Image courstey of GOOGLE images (2010)