* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Hypersensitivities, Infection and Immune Deficiencies
Survey
Document related concepts
Adaptive immune system wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
Immune system wikipedia , lookup
Monoclonal antibody wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Autoimmunity wikipedia , lookup
Hepatitis B wikipedia , lookup
DNA vaccination wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Innate immune system wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Molecular mimicry wikipedia , lookup
Psychoneuroimmunology wikipedia , lookup
Transcript
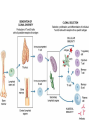
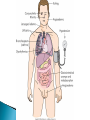
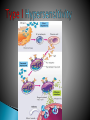
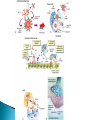
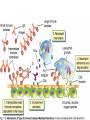
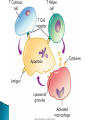
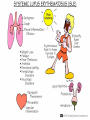
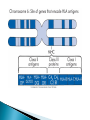
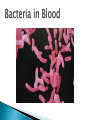
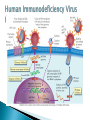
Chapter 7 Immune System “protects against foreign antigens” Inappropriate ◦ Exaggerated – allergy ◦ Misdirected – autoimmunity ◦ Against beneficial foreign tissue – alloimmunity ◦ Insufficient – immune deficiency Hypersensitivity Allergy: exaggerated ◦ Deleterious effects of hypersensitivity to environmental (exogenous) antigens Autoimmunity: misdirected ◦ Disturbance in the immunologic tolerance of self-antigens (autoantibodies) Alloimmunity: beneficial tissue ◦ Immune reaction to tissue of another individual Hypersensitivity Characterized by the immune mechanism ◦ Type ◦ Type ◦ Type ◦ Type I II III IV IgE mediated Tissue-specific reaction Immune-complex mediate Cell mediated ◦ Tables:7-1, 7-2, 7-3 Mechanisms of Hypersensitivity “require sensitization against Ag from a 1° immune response” “disease symptoms after 2° immune response” Immediate – minutes to hours ◦ Anaphylaxis – rapid & severe Delayed – hours to days Type I Hypersensitivity IgE mediated Environmental antigens (allergens) IgE binds to Fc receptor on a mast cell Histamine release ◦ H1 receptors ◦ antihistamines Type I Genetic predisposition Tests ◦ Food ◦ Skin ◦ Lab (IqE) Desensitization ◦ IgG – blocking antibodies Type II Hypersensitivity autoimmune Tissue specific ◦ Cells or tissue (tissue-specific Ag) – target of an immune response Type II Five mechanisms ◦ Cellular destruction – Ab + Complement ◦ Phagocytosis ◦ Neutrophil-mediated damage to tissue ◦ Antibody dependent cell mediated cytotoxicity (NK cells) ◦ Target cell malfunction Type III Hypersensitivity Immune complexes (Ag – Ab cplx) ◦ Formed in the circulation → vessel walls or extravascular tissue → C3b + neutrophils → tissue damage ◦ SLE, serum sickness, Raynaud phenomenon Type IV Hypersensitivity Cytotic T-lymphocytes – lymphokine ◦ Direct killing or phagocytosis Examples ◦ Acute graft rejection TB skin test, contact allergic reactions (poison ivy) ◦ Type II collagen → rheumatoid arthritis thyroid cell surface → Hashimoto disease ◦ Pancreas → diabetes Type I Allergy Environmental antigens that cause atypical immunologic response – genetically predisposed individuals ◦ Pollens, molds, fungi, foods, animals, dust Allergen is contained within a particle too large to be phagocytosed or is protected by a nonallagenic coat Autoimmunity Loss of Tolerance ◦ Views self as foreign Examples ◦ Acute rheumatic fever – group A streptococcal sore throat – M protein – capsule mimics normal heart Ag → antibodies to valve (Type II) ◦ Glomerulonephritis – bacterial Ag into blood: immune cplx → kidney (Type III) Autoimmunity :Example Systemic lupus erythematosus (SLE) ◦ “Chronic multisystem disease” ◦ Autoantibodies against Nucleic acids, erythrocytes, coagulation proteins, phospholipids, lymphocytes, platelets, etc. ◦ Deposition of immune complexes Kidneys, brain, heart, spleen, lung, GI tract, peritoneum and skin Alloimmunity Immune system reacts with antigens on the tissue of other genetically dissimilar members of the same species ◦ ABO blood group ◦ Rh antigen Alloimmune Disease Major histocompatibility complex (HLA) ◦ Antigen – presenting molecules ◦ Chromosome #6 (A, B, C, DR, DQ & DP) 6 genetic loci Class ICD8 on Tc cells Class II CD4 on Th cells Class III Complement ◦ More than 300 different HLA-A antigens ◦ Closer match with sibling Graft Rejection Classified according to time ◦ Hyperacute Immediate and rare → white graft Preexisting antibody to the graft Ag (Type II reaction) ◦ Acute Cell-mediated against unmatched HLA antigens (days to months → Type IV reaction) ◦ Chronic Months to years, slow organ failure Weak cell mediated (Type IV reaction) – endothelial cells of organ’s vessels Infection • Number 1 cause of death world wide – 26% 2005 – Africa – 62% deaths • Developing countries – population & poor sanitation – Plague, cholera, malaria, tuberculosis, leprosy & schistosomiasis • New disease – West Nile virus, severe acute respiratory syndrome (SARS), Lyme disease, Hantavirus and drug resistant tuberculosis Exotoxin: protrin released during bacterial growth ◦ Specific effects :cytotoxins, neurotoxins, hemolysins… ◦ Immunogenic : antibodies(antitoxins) Tetanus, diphtheria, pertussis Endotoxin: contained within the cell walls of gram negative bacteria lysis/destruction ◦ LPS: pyrogenic bacteria DIC, shock inflammation + fever, Microorganisms and Human Relationships • Mutual relationships – Normal flora – Table 7-1 • Provided – nutrients • Produce –Enzymes to facilitate digestion –Produce antibacterial factors # colonization by pathogenic microorganisms –Useable metabolites (Vitamin K, B) • Opportunistic organisms – immune Table 7-1 Pathogenic Defense Mechanisms • Surface coats –Inhibit phagocytosis • Toxins –Kill neutrophils & pyrogenic effect • Proliferation –Rapid > immune response • Antigenic variation –Mutation – antigenic drift –Recombination – antigenic shift –Gene switching Bacteremia – Septicemia Presence of bacteria in the blood Usually gram-negative bacteria Septic shock caused by endotoxins Evaluation – blood culture “bugs in da blood” Institution: Zedek Medical Center, Jerusalem Participants: 75 nurses, 60 physicians Evaluation: Cultures of 3 spots on uniforms Findings: Potential pathogens on 63% of uniforms. Antibiotic resistant strains on 14% nurses & 6% physicians. Eight cultures grew MRSA Suggestion: “infrequent hand washing” Viral Disease “most common affliction humans” - colds → # cancers → AIDS Obligate intracellular parasites ◦ Dependent on the host cell ◦ No metabolism – incapable of independent reproduction ◦ Permissive host cell ◦ Usually a self-limiting infection Spreads cell to cell Viral Replication DNA or RNA Single or double stranded Protein receptor – binding site Virus uncoats Most RNA viruses directly produce mRNA DNA “provirus” enters nucleus and is transcribed into mRNA Viral Replication Translation of mRNA results in the production of viral proteins New viruses are released through budding Viral DNA, integrated into host cell DNA is transmitted to daughter cells by mitosis. Cellular Effects of Viruses Inhibition of host cell DNA, RNA or protein synthesis Disruption of lysosomal membranes Promotion of apoptosis Fusion of infected, adjacent host cells Alteration of antigenic properties Cellular Effects of Viruses Transformation of host cell into cancerous cells Promotion of secondary bacterial infections Clinical Manifestations of Infection Variable depending on the pathogen Direct cause → pathogen Indirect cause → products Fever – “reset hypothalamus” ◦ Exogenous – cell walls - “LPS” → inflammation ◦ Endogenous IL-1, IL -6, interferon, TNF-a Countermeasures • Vaccines – “Induction of long-lasting protective immune response – no disease in a healthy recipient → memory cells (T or B):” – Attenuated viruses (MMR, varicella) – Killed organisms (hepatitis A) – Recombinant viral protein (hepatitis B) – Bacterial antigens – capsular polysaccharides 10 strains S. pneumoniae – Toxins – diphtheria, cholera, tetanus → toxoid (IgG) “chemical detoxified” Countermeasures Antimicrobials: ◦ Inhibit synthesis of cell walls ◦ Damage cytoplasmic membranes ◦ Alter metabolism of nucleic acids ◦ Inhibit protein synthesis ◦ Modify energy metabolism Pathogenic Adaptations Immune system suppression ◦ HIV Multiple drug resistance ◦ Streptococcal pneumonia, tuberculosis, MRSA, VRE, E. coli, Klebsiella ◦ Genetic mutation → selection ◦ “Overuse and compliance” Immune Deficiencies :Lab Evaluation Table 7-12 Hallmark ◦ Unusual or recurrent, severe infections Primary (congenital) immunodeficiency ◦ Genetic anomaly – single gene Secondary (acquired) immunodeficiency ◦ 2° to another illness ◦ More common Secondary (Acquired) Deficiencies Causes ◦ ◦ ◦ ◦ ◦ ◦ ◦ ◦ Normal physiologic condition Psychological stress Dietary insufficiencies Malignancy Physical trauma Medical treatment Infection AIDS Where did the AIDS Virus arise? Evolved from a simian immunodeficiency virus…chimpanzees Southern and western Africa… 1931 ◦ “Jumped species” Spread slowly until mid-to-late 1950s …when it spread exponentially Acquired Immunodeficiency Syndrome (AIDS) RNA virus ◦ Depletes body’s Th cells (MHC II, CD4) ◦ Incidence 40 million 50,000 new/year USA (Denver Post: 8/11)-steady* 18,000 RIP/year ◦ Chronic disease – HAART therapy Epidemiology ◦ Blood-borne pathogen ◦ *Gay & bisexual men=2/3;heterosexual=1/4;IV drug=1/10 AIDS Pathogenesis ◦ RNA virus ◦ Reverse transcriptase → RNA → double stranded DNA ◦ Integrase – insertion of new DNA into host DNA AIDS Pathogenesis Th cells – “helpers”-CD4s non-infected – 600 to 1200 mm3 infected - < 200 mm3 → AIDS Antibodies Blood product: 4-7 weeks Intercourse: 6-12 months Diagnosis: + serology + clinical symptoms AIDS Treatment ◦ HAART – highly active antiretroviral therapy Inhibitor Reverse transcriptase Protease inhibitor Vaccine ◦ Antigenically variable ◦ Ab – lack of protection