* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Cholinoceptor blocking drugs
Specialty drugs in the United States wikipedia , lookup
Pharmacokinetics wikipedia , lookup
Environmental impact of pharmaceuticals and personal care products wikipedia , lookup
Discovery and development of tubulin inhibitors wikipedia , lookup
Discovery and development of proton pump inhibitors wikipedia , lookup
Polysubstance dependence wikipedia , lookup
Discovery and development of non-nucleoside reverse-transcriptase inhibitors wikipedia , lookup
Orphan drug wikipedia , lookup
Psychedelic therapy wikipedia , lookup
Nicotinic agonist wikipedia , lookup
Pharmacogenomics wikipedia , lookup
Pharmaceutical industry wikipedia , lookup
Prescription costs wikipedia , lookup
Prescription drug prices in the United States wikipedia , lookup
Drug discovery wikipedia , lookup
Drug interaction wikipedia , lookup
Neuropharmacology wikipedia , lookup
Pharmacognosy wikipedia , lookup
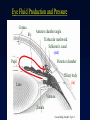
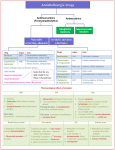
Clinical importance of anticholinesterases Ophthalmologic applications Diagnosis and treatment of myasthenia gravis Treatment of atropine and curare type poisoning Some chemicals (from agricultural or military sources) are themselves significant sources of poisoning. Physostigmine (Eserine, Antilirium) Non-quaternary, well absorbed and distributed to CNS and other tissues. Pharmacological effects result from the increase in concentration of acetylcholine at muscarinic and nicotinic sites following inhibition of cholinesterases. Physostigmine CNS: eye: bronchioles: glands: GIT: bladder: CV: NMJ: restlessness, convulsions miosis, accommodation constriction, increased secretions increased lacrimation, salivation, sweating increased tone and motility increased tone, effect variable, low doses decrease HR; higher could increase HR and BP. fasciculations and tremor; paralysis Physostigmine Clinical uses reserved for reversal of serious atropine or scopolamine type poisoning where CNS is involved. Not routinely used for overdose of drugs with anticholinergic side effects (e.g., may exacerbate arrhythmia in tricyclic antidepressant overdose) Toxicity is predictable based upon ANS effects. CNS stimulation and coma often result. Edrophonium (Tensilon, Reversol) Brief duration of action, rapid onset Uses – – – – Diagnostic aid for myasthenia gravis (not primary diagnostic, but useful for distinguishing MG from other neurological disorders) Differentiation of myasthenia crisis from cholinergic crisis during therapy for MG Antidote for non-depolarizing neuromuscular blockers Treatment for paroxysmal atrial tachycardia (PAT) Toxicities limited because of brief action Irreversible Cholinesterase Inhibitors Highly lipid soluble (except echothiopate) Bind covalently to and inhibit cholinesterases Have muscarinic and nicotinic actions Readily penetrate the CNS Absorbed by all routes Hydrolyzed slowly in the body by phosphorylphosphatases Organophosphates: Clinical relevance Treatment of open angle glaucoma – Insecticides (malathion; parathion) – – Echothiopate and isoflurophate (DFP) are used but not preferred because of potential for development of cataracts and other side-effects. In insects, parathion is converted to paraoxon; malathion to malaoxon. Mammals can preferentially oxidize these chemicals to less toxic compounds. Parathion and malathion are only preferentially toxic to insects. Nerve gas (soman, tabun, sarin) – Developed for volatility, rapid absorption and “aging” Organophosphates: Toxicity Muscarinic, nicotinic and CNS manifestations: Muscarinic Nicotinic CNS Bronchoconstriction Muscular fasciculation Restlessness Bronchial secretion Sweating Salivation Lacrimation Bradycardia Hypotension Tachycardia Hypertension Insomnia Tremors Confusion Ataxia Convulsions respiratory depression circulatory collapse Miosis Blurring of vision Urinary incontinence Organophosphates: Toxicity Limited reversibility if treated rapidly Enzyme/drug bond becomes increasingly irreversible with time. “Aging” is related to loss of alkoxy groups which result in more stable bonds. Aging rate varies with compounds Treatment [Atropine; pralidoxime (2-PAM)]: – – – support respiration large doses of atropine cholinesterase reactivator pralidoxime Cholinergic Receptor Antagonists Cholinoceptor blocking drugs: Overview Definition and classification Alkaloids – Quaternary and non-quaternary synthetics – Sites of action Prototypes: atropine; scopolamine Therapeutic uses Toxicity Contraindications Cholinergic Receptor Antagonists Cholinoceptor blocking drugs DEFINITION: Drugs which occupy muscarinic receptors and prevent the muscarinic actions of endogenous acetylcholine or other muscarinic agonists. Often referred to as anticholinergics or antimuscarinics Anticholinergic drugs Antimuscarinic M 1- selective Nonselective Antinicotinic Ganglion blockers Neuromuscular blockers Naturally occurring compounds (Belladonna alkaloids) plant Atropa belladonna Dautura stramonium Hyosacyamus niger drug atropine scopolamine atropine scopolamine Synthetic/semisynthetic compounds Quaternary compounds: Ipratropium (Atrovent) Propantheline (Pro-Banthine) Synthetic/semisynthetic compounds Non-quaternary compounds Dicyclomine (generic, Bentyl) Homatropine (Isopto Homatropine) Tropicamide (Nydriacyl) Prototypes: Atropine & scopolamine The actions of these drugs upon peripheral tissue/organ activity are similar to that which would occur following reduction of activity in postganglionic, parasympathetic and postganglionic cholinergic sympathetic nerves. Both drugs also block CNS muscarinic receptors Pharmacokinetics of atropine and other tertiary amines Atropine is relatively lipid soluble and readily crosses membrane barriers. The drug is well distributed into the CNS and other organs and is eliminated partially by metabolism in the liver and partially by renal excretion. The elimination half-life is approximately 2 hours, and the duration of action of normal doses is 4-8 hours except in the eye, where effects last for 72 hours or longer. Other tertiary amines are able to enter the eye after conjunctival administration. Similar ability to cross lipid bariers is important for the agents used in parkinsonism. Cardiovascular system effects Heart: low dose high dose bradycardia tachycardia Vascular – no (direct) effect – except, dilate cutaneous vessels (red as a beet) – block hypotensive effect of muscarinic agonists Extravascular smooth muscle Eye: – – mydriasis cycloplegia Bronchial: GIT: Urinary: Glands (dilation of iris sphincter) (relaxation of ciliary muscle) dilation decreased tone, motility (antispasmodic effect) relaxation of detrusor, ureter; constriction of sphincter decrease in all secretions Eye Fluid Production and Pressure Cornea Iris Anterior chamber angle Trabecular meshwork Schlemm’s canal (out) Pupil Posterior chamber Ciliary body (in) Lens Vitreous Zonule Cassel, Billig, Randall Fig 8-2 Types of Glaucoma Open-Angle Glaucoma Blocked drainage of aqueous Blocked drainage of aqueous Anterior chamber open Blockage at trabecular meshwork Cassel, Billig, Randall Closed-Angle Glaucoma Fig 8-4 Anterior Chamber angle closure Cassel, Billig, Randall Fig 8-3 Central nervous system Slowing of heart after therapeutic doses (??) Action at respiratory center therapeutic dose: – larger doses: – Cerebral centers: low doses: – high doses: – higher doses: – Note: faster deeper breathing depression of respiration sedation restlessness, amnesia, delirium stupor; coma with therapeutic doses, atropine generally has less CNS sedative effects Tissue organ specificity of antimuscarinics Order of appearance of physiological effects with increasing dosage: Salivary, bronchial, sweat secretions Micturition Tachycardia, mydriasis, cycloplegia Intestinal motility Gastric secretion Quaternary vs Non-quaternary antimuscarinics Absorption. Quaternary compounds are less well absorbed and lack CNS actions Nicotinic actions. Quaternary compounds can block nicotinic receptors and may have ganglion or neuromuscular blocking action Therapeutic uses of antimuscarinics Anesthesiology – Prevention (partly historical) of bronchial and salivary secretions – Prevent bronchospasm – Reversal of reflex bradycardia or hypotension during surgery – Drugs: Belladonna alkaloids, some synthetics Therapeutic uses of antimuscarinics Respiratory – Ipratropium disorders: (Atrovent). Inhalational drug to reverse bronchial constriction and secretion – Asthma, emphysema, chronic bronchitis ( Therapeutic uses of antimuscarinics Ophthalmology – production of mydriasis and cycloplegia of long or short duration – choice of agent depends upon requirements. – routine examination: short duration; minimal cycloplegia. – many appear in combinations with alpha adrenergic drugs Mydriatic antimuscarinics Drug Duration of Action Cycloplegia Atropine 6-12 days +++ Cyclopentolate 12-24 h ++ Homatropine 12-48 h + Scopolamine 3-7 days +++ Tropicamide 1-2 h ++ Therapeutic uses of antimuscarinics Gastroenterology: Peptic ulcer treatment. Can reduce basal and nocturnal acid secretion (other drugs are better, e.g., H2 antagonists) – Inhibit gastrointestinal motility – Reduce pain and prolong actions of antacids – Drugs: atropine, dicyclomine, propantheline – Therapeutic uses of antimuscarinics Gastroenterology: Irritable bowel syndrome – Reduce motility for reduction of pain, constipation, or diarrhea – Drugs: atropine, dicyclomine, propantheline Therapeutic uses of antimuscarinics Urologic disorders – Detrusor hyperreflexia, enuresis – Increase bladder capacity – Decrease bladder pressure – Drugs: dicyclomine, oxybutynin Therapeutic uses of antimuscarinics Motion – sickness Scopolamine is useful in prophylactic treatment via CNS action in vestibular nuclei and reticular formation Muscarine poisoning poisoning with muscarinic mushrooms (Inocybe) or cholinesterase inhibitors – Drugs: Belladonna alkaloids or synthetics (propantheline) – Sources of Belladonna Poisoning: Nonprescription Plants drugs of the Solanaceae family Antiparkinsonian drugs Classic symptoms of belladonna poisoning: Hot as a hare Dry as a bone Red as a beet Blind Mad as a bat as a hatter Bloated as a toad Contraindications for Antimuscarinics Glaucoma Prostatic hypertrophy Toxicity more severe in children Toxicity constipation Urinary retention Mydriasis Blurred vision Flushing, dry skin Heart palpitation hyperthermia headache Dizziness Excitement Mental confusion, memory loss, hallucinations Drugs with anticholinergic side-effects Antihistamines Monoamine oxidase inhibitors Antipsychotics Lithium Tricyclic Antidepressants Antiparkinsonian drugs