* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download CHD
Public health genomics wikipedia , lookup
Transgenerational epigenetic inheritance wikipedia , lookup
Genome (book) wikipedia , lookup
Microevolution wikipedia , lookup
Epigenetics of neurodegenerative diseases wikipedia , lookup
Quantitative trait locus wikipedia , lookup
Fetal origins hypothesis wikipedia , lookup
Down syndrome wikipedia , lookup
Medical genetics wikipedia , lookup
Nutriepigenomics wikipedia , lookup
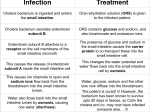
Genetics of Congenital Heart Disease 张咸宁 [email protected] Tel:13105819271; 88208367 Office: A705, Research Building 2013/03 Required Reading Thompson &Thompson Genetics in Medicine, 7th Ed (双语版,2009) ● Pages 91-92、168-169、356 Learning Objectives • To recognize familial patterns of CHD • To understand developmental mechanisms of CHD • To see CHDs as examples of the larger group of common disorders with common complex inheritance involving – Single genes – Multiple genes – Environmental influences Overview • Introduction to Congenital Heart Disease (CHD) • Developmental Mechanisms – – – – – Flow Lesions Problems in Cell Migration Problems in Cell Death Abnormalities in Extracellular Matrix Abnormalities in Targeted Growth • Summary Introduction to CHD • Relatively common birth defect – Liveborn infants • 4-8/1 000 – Stillborns • 10× higher or 8% – Miscarriages • 15% in abortuses <24 weeks gestation Introduction to CHD • Variety of causes – Single gene – Chromosomal – Teratogen exposures • Maternal rubella infection • Gestational diabetes mellitus Environmental Component • Maternal Infections – Rubella: 35% affected • Maternal Diseases – Diabetes Mellitus: 3-5% – Maternal PKU: 10% • Teratogenic Substances – Alcohol: 25-35% – Dilantin(苯妥英): 2-3% Genetic Component • Gross Chromosomal Defects – 5-8% of Defects – Examples • Trisomy 21: 35-50% • Trisomy 18: 99% • Turner syndrome: 20% • Single-Gene Defects – 3% of Defects Familial Patterns of Recurrence • CHD recurrence in a family – Affected individuals may not have identical anatomical heart abnormality – Will have lesions representing similarity in the developmental mechanism • Should look for abnormalities outside of the cardiovascular system – May indicate a syndromic association with CHD Developmental Mechanisms Flow Lesions Problems in Cell Migration Problems in Cell Death Abnormalities in Extracellular Matrix Abnormalities in Targeted Growth Is Isolated CHD a Multifactorial Trait? • • • • Table 8-12: Population Incidence and Recurrence Risks for Various Flow Lesions VSD = Ventricular Septal Defect PDA = Patent Ductus Arteriosus ASD = Atrial Septal Defect AS = Aortic Stenosis Defect Pop Freq Incid in Sibs (%) (%) λsib VSD 0.17 4.3 25 PDA 0.083 3.2 38 ASD 0.066 3.2 48 AS 0.044 2.6 59 Is Isolated CHD a Multifactorial Trait? • For these flow lesions – Sib relative risk ratio (λsib) • Support familial aggregation – Where genetic mutation not known • Use empiric risk factors to counsel first degree relatives • Rapid decrease in risk for second and third degree relatives to not much higher than population risks • For families with CHD other than flow lesions – Reassure that recurrence risk is no greater than population risk • Prenatal ultrasound can be used as part of counseling and often reassurance before birth Flow Lesions • Large category of CHDs – Approximately 50% of all CHDs • Up to 25% of flow lesion CHDs, particularly tetralogy of Fallot, have del22q11.2 – DiGeorge syndrome – Velocardiofacial syndrome – Conotruncal anomaly face syndrome del22q11.2 Syndromes • Autosomal dominant • Variable expressivity • Deletion of approximately 3 Mb – Caused by homologous recombination of low copy repeat sequences • One of the most common cytogenetic deletions with a significant phenotype – 1 per 2 000 – 4 000 live births 22q11.2 Rearrangements Fig 6-9 del22q11.2 Syndromes • Phenotypes may include – – – – – – CHD Craniofacial abnormalities Mental retardation/developmental delay Reduced circulating lymphocytes Hypocalcemia Schizophrenia del22q11.2 and CHD • Responsible for between 5% and 12.5% of CHDs • Particularly common in certain CHDs – >40% of patients with tetralogy of Fallot (TOF) and pulmonary atresia (PA) – >60% of patients with TOF and absent pulmonary valve DGS TDR (Typically Deleted Region) • 3 Mb deletion – Loss of approximately 30 genes • Smaller 1.5 Mb deletion – Seen in approximately 10% of patients • TBX1 maps in DGS TDR – Encodes transcription factor involved in pharyngeal arch development – Haploinsufficiency implicated in DGS – Mutated in patients with similar phenotype who do not have del22q11.2 Apoptosis and CHD • TBX1 may be involved in apoptosis, a mechanism known to be involved in normal cardiac and lymphocyte development – Foxp1 in mice • Required for remodeling of endocardial cushions (portions of ventricular septum and cardiac outflow tract) • To position aortic and pulmonary vessels normally by eliminating certain cells to shift the cushions’ positions – Apoptosis occurs during immune system development • To eliminate lymphocytic lineages that react to self • Required for protection against autoimmune disease Apoptosis and CHD • If TBX1 causes the conotruncal defects (e.g. TOF) associated with del22q11.2, and if the mechanism is apoptosis, then what does that do to our “developmental mechanisms” outlined at the beginning – del22q11.2 causes the largest proportion of flow lesions, but may be a problem in cell death Case #1 4-m.o. Female Infant – CHF from a Large VSD – Dysmorphic Appearance Truncus TOF Arteriosus – Family History: Sib and Half-Sib with CHD – Mother with Multiple Psychiatric Admissions VSD DiGeorge Syndrome • DiGeorge (not DiGeorge’s) Syndrome • Features Include: – Cardiac: Conotruncal Defects – Immunologic: Thymic Aplasia or Hypoplasia – Hypocalcemia: Parathyroid Absence or Hypoplasia – Dysmorphism: Hypertelorism, Short Philtrum, Cupid’s Bow Mouth, Ear Anomalies VeloCardioFacial (VCF) Syndrome • Features Include: – Cardiac: VSD, Tetralogy of Fallot, Rt. Aortic Arch – Cleft Palate: Overt or Submucosal – Development Delay: Mild-to-Moderate, esp. Speech – Dysmorphisms: Prominent Nose, Abnormal Ears, Abundant Hair, Tapered Fingers VCF/DG SYNDROMES Clinical Overlap Cleft Palate Dev. Delay DGS Cleft Palate Dev. Delay VCF Facies CHD Dev. Delay VCF Facies Problems in Cell Migration: Patent Ductus Arteriosus (PDA) • 1 in 2 000 Fullterm Infants • 10% of CHD • 2:1 Female to Male Ratio • Multifactorial Etiology: Genes and Environment Familial PDA • 2-y.o. Palestinian Boy – Patent Ductus Arteriosus – Positive Family History PDA PDA Neural Crest Cell Migration and Cardiac Development Cardiac Genetics Population Perspective • Developing Innovative Therapies – Postnatal Interventions • Marfan Syndrome: Anti-TGF – Prenatal Interventions • Folate • Improving Clinical Trials Research – Cardiology Emulating Heme/Onc – Primary Endpoints - Function, Not Survival – Better Statistical Power • First, exome-centered and whole-genome next-generation sequencing • Second, epigenetics and transcriptomics • Third, systems biology GWAS: the genetic variants identified often explain 10% of the variation in a trait or disease! Epigenetics and Transcriptomics • Research is increasingly acknowledging that static DNA sequence variation explains only a fraction of the inherited phenotype. Therefore, we expect that multiple epigenetic and gene expression signatures will be related to CVD in experimental and clinical settings. Complex relationships between the genome, epigenetic and transcriptional regulations, the proteome, and the metabolome that produce CVD phenotypes. Summary: CHD • Relatively common birth defect – 4-8/1 000 live births • Familial CHD – May not have identical anatomic abnormality • Variety of developmental mechanisms – Undergoing revision as we understand molecular pathogenesis CHD • Recurrence risk – If familial, identify inheritance pattern – If not familial, use empiric risk data • del22q11.2 is a common cause of CHD – Up to 25% of flow lesions – Flow lesions represent 50% of all CHD – Therefore, 12.5% of all CHD