* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download RCP 112 Basic Concepts
Survey
Document related concepts
Transcript
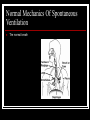
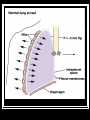
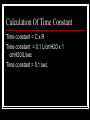
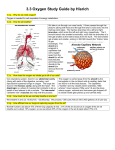
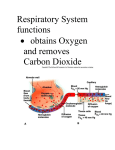
RCP-112 PATIENT MANAGEMENT Basic Terms And Concepts Of Mechanical Ventilation Normal Mechanics Of Spontaneous Ventilation Respiration – movement of gas molecules across a membrane. External respiration – 02 moves from the lung into the bloodstream, C02 moves from the blood stream into the alveoli. Normal Mechanics Of Spontaneous Ventilation Internal respiration – cellular level, C02 moves from the cells into the blood and 02 moves from the blood into the cells. Normal Mechanics Of Spontaneous Ventilation Here’s how we breathe: 1. 2. 3. 4. 5. Muscles of inspiration contract. The diaphragm descends and enlarges the vertical size of the thoracic cavity. The external intercostals contract – and slightly raise the ribs, increasing the circumference of the thorax. The activity of these muscles represent the work needed to inhale. Exhalation is passive – muscles relax and the volume of the thoracic cavity decreases and air is forced out. Normal Mechanics Of Spontaneous Ventilation The normal breath Gas Flow And Pressure Gradients During Ventilation You Need To Understand The Basic Concept Of Airflow! 1. For air to flow through the airways – pressure at one end must be higher than pressure at the other end. 2. Pressure gradient – air flows from the high-pressure point to the low pressure point. Gas Flow And Pressure Gradients During Ventilation Lung volumes change as a result of gas flow caused by changes in pressure. The conductive airway starts at the mouth and nose and ends at the small airways near the alveoli. Gas Flow And Pressure Gradients During Ventilation Gas flows into the lung when the pressure in the alveoli is < than the pressure at the mouth and nose. Gas flows out of the lungs when the pressure in the alveoli is > than the pressure at the mouth and nose. Gas Flow And Pressure Gradients During Ventilation A pressure gradient doesn’t exists – when the pressure in the mouth and alveoli are the same. This occurs at the end of inspiration or the end of expiration – gas flow doesn’t occur because the pressure across the conductive airways are =. Units Of Pressure Ventilating pressure are measured in cm H20. These pressures are referenced to atmospheric pressure and given a baseline value of zero. Definition Of Pressures And Gradients In The Lungs Airway opening pressure (Pawo) or mouth pressure (Pm) is called airway pressure (Paw). Mouth pressure and airway pressure are the terms most commonly used. But this pressure may be called upper airway pressure, mask pressure or proximal airway pressure. Pressures And Gradients In The Lungs Pbs – pressure at the body surface area: 1. Equal to 0 (atmospheric) unless the person is using a hyperbaric chamber or a iron lung. Pressure And Gradients In The Lungs Intrapleural pressure (Ppl) – measurement of pressure in the potential space between the parietal and visceral pleural: 1. Normal is -5 cmH20 at the end of exhalation during a spontaneous breath. 2. -10 cmH20 at the end of inspiration. 3. Since intrapleural pressure is hard to measure, they will look at esophageal pressure (Pes) – balloon is placed in the esophagus and changes in balloon pressure are used to estimate pressure and pressure changes in the pleural space. Pressure And Gradients In The Lungs Alveolar Pressure (Palv/PA) – also called intrapulmonary or lung pressure: 1. It normally changes as intrapleural pressure changes. 2. During inspiration alveolar pressure is about -1 cmH20 and during exhalation it is about +1 cmH20. Pressures And Gradients In The Lung 4 basic pressure gradients used to describe normal ventilation: 1. 2. 3. 4. Transairway pressure Transthoracic pressure Transpulmonary pressure Transrespiratory pressure Pressures And Gradients In The Lungs Transairway pressure – (PTA) the pressure gradient between the airway opening and the alveolus: 1. PTA = Pawo – PA. 2. Pawo is often called the airway pressure (Paw). 3. It produces airway movement in the conductive airways. 4. It also represents the pressure caused by resistance to gas flow in the airways (airflow resistance). Pressure and Gradients In The Lungs Transthoracic pressure (Pw) – the pressure difference between the alveolar space (PA) or lung and the body’s surface (Pbs): 1. Pw = PA-Pbs. 2. It represents the pressure needed to expand or contract the lungs and the chest wall at the same time. Pressures And Gradients In The Lungs Transpulmonary pressure – (PL) or transalveolar pressure, is the pressure difference between the alveolus PA and the pleural space (Ppl): PL=PA-Ppl: 1. PL maintains alveolar inflation and is sometimes called the alveolar distending pressure. 2. All modes increase PL, either by decreasing Ppl (- pressure ventilators) or increasing PA by increasing pressure at the upper airway ( + pressure ventilators). 3. Transalveolar pressure is used synonymously with transpulmonary pressure Pressures And Gradients In The Lung Transrespiratory pressure (PTR) – the pressure gradient between the airway opening and the body surface: 1. PTR = Pawo-Pbs. 2. This pressure is required to inflate the lungs and airways during positive pressure ventilation. 3. In this situation the body surface pressure is atmospheric and given the value 0. 4. Thus – Pawo becomes the pressure reading on the ventilator. Pressures And Gradients In The Lungs Transrespiratory pressure continued: 5. It has 2 components – transthoracic pressure (pressure required to overcome elastance) and transairway pressure (pressure required to overcome airway flow resistance) Pressures And Gradients In The Lungs Let’s look at the normal spontaneous breath: 1. Remember Boyle’s Law? 2. With spontaneous inspiration – the volume of the thoracic space increases and the pressure in the pressure in the pleural space is more negative in relation to atmospheric pressure. 3. Negative intrapleural pressure goes from -5 cmH20 at end-inspiration to about -10 cmH20 at endinspiration. Pressure And Gradients In The Lung Spontaneous breath continued: 4. - pleural pressure is transmitted to the alveolar space. 5. PA pressure becomes more negative relative to atmospheric pressure. 6. PL widens – thus the alveoli have a negative pressure during spontaneous inspiration. Pressure and Gradients In The Lungs The spontaneous breath continued: 7. Pressure at the mouth is still atmospheric. 8. There is a pressure gradient between the mouth and alveolus – thus air flow from the mouth to the alveolus and they expand. 9. When the volume of gas builds up in the alveoli and pressure returns to 0, airflow stops. 10. This is the end of inspiration – pressure at the mouth and in the alveoli is 0. Pressures And Gradients In The Lungs Spontaneous breath continued: 11. During the expiratory phase the muscles relax. 12. Thoracic volume decreases to resting and the intrapleural pressure returns to around -5 cmH20. 13. The pressure inside the alveolus during exhalation increases and becomes slightly positive. 14. Pressure is lower at the mouth than inside the alveoli – transairway pressure gradient causes air to move out of the lungs. 15. Pressure in the alveoli and the mouth are =, exhalation ends. Changes In Transpulmoanry Pressure Under Varying Conditions Passive Spontaneous Ventilation Pressure End-Expiration End-Inspiration Intraalveolar 0 cmH20 0 cmH20 Intrapleural -5 cmH20 -10 cmH20 +5 cmH20 +10 cmH20 Transpulmonary Changes In Transpulmonary Pressure Under Varying Conditions Positive Pressure Ventilation Pressure End-Expiration End-Inspiration Intraalveolar 0 cmH20 9-12 cmH20 Intrapleural -5 cmH20 2-5 cmH20 Transpulmonary +5 cmH20 8 cmH20 Lung Characteristics 2 primary characteristics of the lungs: 1. Compliance 2. Resistance These 2 parameters are evaluated for patients receiving mechanical ventilation. Lung Characteristics 2 types of force that oppose the inflation of the lung: 1. Elastic force – arise from the elastic properties of the lungs and thorax that oppose inspiration. 2. Frictional forces – which is the result of 2 factors, the resistance of the tissues and organs as they move and become displaced during breathing and resistance to gas flow through the airways. Lung Characteristics Compliance: 1. The ease with which the structure distends. 2. A balloon that’s easy to inflate is very compliant. 3. Elastance is the tendency of a structure to return to its original form after being stretched or acted on by an outside force Lung Characteristics Pulmonary physiology and compliance: 1. Describes the elastic forces that oppose lung inflation. 2. Defined as change of volume that corresponds to the change in pressure. 3. C = cV/cP. Lung Characteristics Pulmonary physiology and compliance continued: 4. Volume is measured in liters or milliliters and pressure in centimeters of water pressure. 5. Compliance of the respiratory system is the sum of the compliances of both the lung tissue and the surrounding thoracic structures. Lung Characteristics Pulmonary physiology and compliance continued: 6. The value for compliance varies based on a person’s posture, position and active breathing. 7. It can range from .05 L/cmH20 to 0.17 L/cmH20 (50 to 170 ml/cm H20). 8. For intubated and mechanically ventilated patients with normal lungs and chest wall – males 40-50 ml/cmH20, up to 100 ml/cmH20 and females 35 - 45 ml/cmH20, up to 100 ml/cmH20. Lung Characteristics Pulmonary physiology and compliance continued: 9. Monitoring changes in compliance is an excellent way of assessing changes in the patient’s condition. 10. Compliance is usually measured under conditions of no gas flow – called static compliance. Lung Characteristics Pulmonary physiology and compliance: 11. Changes in condition of the lungs and/or chest wall affect total respiratory system compliance and the pressure needed to inflate the lungs. 12. Examples ARDS and COPD. Excercise Calculate Pressure If compliance is normal at 0.1 L/cmH20, calculate the amount of pressure needed to attain a tidal volume of .5 L (500ml). Answer C = cV/cP – so cP = cV/C .5L/0.1L/cmH20 = 5 cmH20 So a Palv. change of 5 cmH20 would be needed to achieve a .5 L Vt in a person with normal compliance. Lung Characteristics Pulmonary physiology and compliance: 13. When patients are mechanically ventilated, compliance calculations use the plateau pressure measured at static or no flow conditions and the pressure at the end-exhalation. 14. Tidal volume exhaled from the patient’s lungs is determined by measuring the volume near the patient connector. Equation For Calculating Static Compliance CL = Exhaled Tidal Volume/(Plateau pressure-EEP) C = VT/Plateau – EEP Compliance value includes both lung and thorax If a patient actively inhales or exhales during the measurement of a plateau pressure, the value will be inaccurate. L Lung Characteristics Resistance: 1. Frictional forces seen with ventilation are due to the anatomical structure of the conductive airways and the tissue viscous resistance of the lungs and adjacent tissues and organs. 2. When the lungs and thorax move during ventilation, the movement and displacement of the lungs, abdominal organs , rib cage and diaphragm create resistance to breathing. Lung Characteristics Resistance continued: 3. During MV, resistance of the airways is the factor most often evaluated. 4. Ability of air to flow through the conductive airways depends on the gas viscosity and density, length and diameter of the E.T. tube and the flow rate of the gas through the tube. Lung Characteristics Resistance continued: 5. Clinically diameter of the airway lumen and flow rate of the gas are factors that can change. 6. Tube size, secretions, bronchospasm, edema or kinks in the ET tube. 7. The flow rate can be controlled in most modes of ventilation. Lung Characteristics The equation Raw = (PIP-Pplateau) Flow Raw = (40-25) 1(L/sec) = 15 cmH20/(L/sec) Lung Characteristics Normal Resistance Values Unintubated Patient 0.6 to 2.4 cmH20/(L/sec) at 0.5 L/sec flow Intubated Patient 6 cmH20/(L/sec) or higher (airway resistance increases as ET tube size decreases. Lung Characteristics Factors that can affect Raw: 1. 2. 3. 4. Smaller internal diameter of the ET tube. Diseases processes like asthma Secretions, bronchospasm , kinks in the ET tube Flow patterns Lung Characteristics Disadvantage of higher Raw: 1. More of the pressure for breathing goes to the airways and not the alveoli (some molecules are slowed as they collide with the tube and the bronchial walls – this causes them to exert pressure against the passages – airways expand and some of the molecules stay in the airway and don’t reach the alveoli). 2. Less pressure in the alveolus, smaller volume of gas is available for gas exchange. Lung Characteristics Disadvantages continued: 3. With higher resistance, more force needs to be exerted to try to get the gas flow through the obstructed airways. 4. For this to happen a spontaneously breathing patient will use their accessory muscles – this generates more negative intrapleural pressure and a greater pressure gradient between the upper airway and the pleural space to achieve gas flow. 5. The same thing happens on a mechanical ventilator. Lung Characteristics More on measuring Raw: 1. Ex. PIP during a mechanical breath is 25 cmH20 and the plateau pressure is 20 cmH20 – the pressure lost to the airways because of Raw is 5 cmH20. 2. This is normal with a proper size ET tube. 3. Key – the calculation assumes that the flow is constant and the flow is converted from liters/min. to liters/sec. Calculation Time An intubated, 36-year-old woman is being ventilated with a volume of .5L (500ml). The PIP is 24cmH20, Pplateau is 19 cmH20 and baseline pressure is 0. The inspiratory gas flow is constant at 60 L/min ( 1 L/sec). What are the static compliance and Raw? Are these values normal? Time Constants Differences in compliance and resistance occur throughout the lung. So the characteristics of the lung are heterogenous – some units may be normal, others affected by increased resistance, decreased compliance or both. This is based on the pathophysiology of the lung. Time Constants Differences in C and Raw affect how quickly the lung units fill and empty. If a lung unit is stiff (hypocompliant) it fills rapidly. If pressure is applied to a stiff lung unit for the same time as to a normal unit, a smaller volume results --- C = V/P. For the same amount of pressure applied, if compliance is low, the resulting volume is lower than normal. Time Constants If the lung unit is normal, but the airway is very narrow (increase Raw) the lung unit fills very slowly. The gas takes longer to move through the narrow passage and reach the alveoli. If the gas flow is applied for the same length of time as in a normal situation, the resulting volume is smaller. Time Constants Length of time lung units require to fill and empty can be calculated. The product of compliance and resistance is called a time constant. Calculation Of Time Constant Time constant = C x R Time constant = 0.1 L/cmH20 x 1 cmH20/L/sec Time constant = 0.1 sec. Time Constant It expresses the time required for the lung to fill or empty by a certain amount. Ex. A patient with a time constant of 0.1 sec. 63% of exhalation (inhalation) occurs in 0.1 sec – that’s 1 time constant. Time Constant 2 time constants allow for about 86% of the volume to be exhaled (inhaled). 3 time constants allow for about 95% to be exhaled (inhaled). 4 time constants allow 98% of the volume to be exhaled or inhaled. Time Constants 5 time constants – the lung is considered to have exhaled (inhaled) 100% of tidal volume. In our previous calculation, 5 time constants would = 5 x 0.1 sec. or .5 sec. So in half a second a normal lung unit would empty. Time Constant Why is this important: 1. It’s important in setting up a ventilator’s inspiratory time and expiratory time. 2. An inspiratory time < than 3 time constants can lead to incomplete delivery of the tidal volume. 3. Increasing the inspiratory time allows even distribution of ventilation and adequate delivery of tidal volume. Time Constants Why is this important continued: 4. 5 time constants should be used for the IT in PCV to ensure an adequate volume delivery. 5. ET < than 3 time constants can lead to incomplete emptying of the lungs – this increases the FRC and leads to gas trapping in the lungs. 6. The belief is using the 95% to 98% volume emptying is adequate for exhalation. 7. The key though is careful observation of the patient and measurement of end-expiratory pressure to decide which time is better tolerated. Time Constant Lung units can be described as fast or slow. Fast units have short time constants. Short time constants are a result of normal or low Raw and decreased compliance – ex. interstitial fibrosis. Time Constant Fast lung units take < time to fill and empty, but require more pressure to achieve a normal volume. Slow lung units have long time constants, this is a product of increased resistance or increased compliance or both – ex. Emphysema. This units require more time to fill and empty. Time Constant Key fact ---- the lung is rarely an even mixture of ventilating units – some units empty and fill quickly, others do so more slowly. The RT determines how most of the lung is functioning and base treatment decisions on his/her findings and on patient’s response to therapy Types of Mechanical Ventilation 3 basic methods: 1. Negative pressure ventilation – please read in your book. 2. Positive pressure ventilation 3. High-frequency ventilation – will cover fall. Positive Pressure Ventilation This happens when an mechanical ventilator moves air into the patient’s lungs by way of an E.T. tube or mask. At any point during inspiration – the inflating pressure at the proximal airway = the sum of the pressure required to overcome the compliance of the lung and chest wall and the resistance of the airways. Positive Pressure Ventilation During the inspiratory phase, the pressure in the alveoli builds and becomes more positive --- this is transmitted across the visceral pleura. Thus the intrapleural space may become positive at the end of inspiration. Positive Pressure Ventilation At end inspiration, the ventilator stops delivering the positive pressure. Mouth pressure returns to ambient. Alveolar pressure is still positive – this creates a gradient between the alveolus and the mouth and air flows out. Definition Of Pressures In Positive Pressure Ventilation Baseline pressure: 1. There read from baseline values. 2. Look at figure 2-9 p. 27 – there the baseline pressure is 0 (atmospheric) – this indicates that no additional pressure is applied at the airway opening during expiration and before inspiration. 3. There are times the baseline pressure is > than 0 – ex. when the RT picks a higher pressure to be present during exhalation -- this is PEEP. Definition Of Pressures In Positive Pressure Ventilation When PEEP is set – the ventilator prevents the patient from exhaling to 0 (atmospheric). It increases the volume of gas left in the lungs at the end of a normal exhalation. It increases FRC Definition Of Pressures In Positive Pressure Ventilation PEEP applied by the RT is called extrinsic PEEP. Auto-PEEP (Intrinsic PEEP) is a complication of positive pressure ventilation. Here gas is accidently trapped in the lungs. This happens when a patient doesn’t have enough time to exhale before the ventilator gives another breath Definition Of Pressures In Positive Pressure Ventilation During positive pressure ventilation, you will see a rise to a peak pressure (Ppeak or PIP or peak airway pressure. It is the highest pressure recorded at the end of inspiration. This is the sum of 2 pressures – the pressure needed to force the gas through the resistance of the airways (PTA) and the pressure of the gas volume as it fills the alveoli. Definition Of Pressures In Positive Pressure Ventilation Plateau pressure is measured after a breath has been delivered to the patient and before exhalation begins. An inspiratory pause (.5-1.5 sec) to get this measurement. With the pause, the pressure inside the mouth and alveoli are equal (no gas flow). Definition Of Pressures In Positive Pressure Ventilation Relaxation of the respiratory muscles and the elastic recoil of the lung tissues are exerting force on the inflated lungs. This creates a + pressure and reads as a + pressure on the ventilator. Definition Of Pressures In Positive Pressure Ventilation Plateau pressure is a good estimate of alveolar pressure (PA). It reflects the effect of the elastic recoil on the gas volume inside the alveoli and any pressure exerted by the volume in the ventilator circuit that is acted upon by the recoil of the circuit.