* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Chapter 14 Heart: Cardiovascular Physiology
Electrocardiography wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Heart failure wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Coronary artery disease wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Artificial heart valve wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
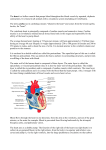
Chapter 14 Heart: Cardiovascular Physiology Exam 3 will be on Monday November 21 Will cover chapters 11, 12, 13, 14 May cover more, depends on how far we get Heart: Cardiovascular Physiology Cardiovascular system is a series of tubes (blood vessels) filled with fluid (blood) and connected to a pump (the heart) Pressure generated by the heart continuously moves blood through the system Blood picks up oxygen at the lungs and expels carbon dioxide Blood circulates to all the body cells, bringing oxygen and removing waste products Table 14-1 Copyright © 2010 Pearson Education, Inc. Arteries – Carry blood away from the heart – Usually carry oxygenated blood • Exception: pulmonary arteries carry deoxygenated blood to the lungs – Shown in red on the diagrams Veins – Carry deoxygenated blood to the heart • Exception: pulmonary veins carry re-oxygenated blood back to the heart – Shown in blue on the diagrams Systemic Circulation – Heart (left ventricle) to body tissues then back to the heart Pulmonary Circulation – Right ventricle to lungs then back to heart (left atrium) Hepatic Portal Circulation – Digestive tract to liver via the hepatic portal vein. This carries the digested nutrients directly to the liver for processing Portal Systems Definition: – Two capillary beds directly connected by a set of blood vessels Other body portal systems: – Kidney portal system – Hypothalamic-hypophyseal portal system Figure 14-1 Copyright © 2010 Pearson Education, Inc. Figure 14-7c Copyright © 2010 Pearson Education, Inc. Figure 14-7a Copyright © 2010 Pearson Education, Inc. Figure 14-7g Copyright © 2010 Pearson Education, Inc. Figure 14-7b Copyright © 2010 Pearson Education, Inc. Figure 14-7d Copyright © 2010 Pearson Education, Inc. Heart Structure Learn the following diagrams (if you don't already know them) Know, for the exam, pericardium, heart structures (including valves, atria, ventricles, septum), arteries and veins attached to the heart (including the coronary arteries—not shown on the diagrams), and the circulation of blood through the heart See Table 14-2 on page 478 for heart structures and major blood vessels Figure 14-7e Copyright © 2010 Pearson Education, Inc. Figure 14-7f Atria, ventricles, veins, arteries Copyright © 2010 Pearson Education, Inc. Table 14-2 Copyright © 2010 Pearson Education, Inc. Figure 14-7g Copyright © 2010 Pearson Education, Inc. Coronary Arteries and Veins Located in shallow grooves on the surface of the heart Supply blood to the heart muscle If any of these get blocked, can cause a myocardial infarction (heart attack) If the blood flow is blocked, then the heart cells that the artery supplies start to die Coronary Arteries and Veins Heart: Fibrous “Skeleton” (fig. 14-9a, p. 480) Four fibrous connective tissue rings surround the four heart valves Functions: 1. Separates atria from ventricles 2. Provides attachment for valve cusps and myocardium (all heart muscle originate and insert on it). This arrangement pulls the heart base and apex together when the ventricles contract Heart: Fibrous “Skeleton” (fig. 14-9a, p. 480) 3. Helps keep AV and semilunar valves open, but inhibits over distension of these valves 4. Forms an electrical insulator separating the electrical impulses of the atria and ventricles, so that they contract independently Heart Valves One-way flow through the heart, ensured by 2 sets of heart valves Atrioventricular (AV) valves – Located between the atria and ventricles – Tricuspid valve (has 3 flaps) • Between R. atrium and R. ventricle – Bicuspid valve (has 2 flaps) • Between L. atrium and L. ventricle • Also called mitral valve (looks like a bishop's hat) Figure 14-9a Copyright © 2010 Pearson Education, Inc. Figure 14-9c Copyright © 2010 Pearson Education, Inc. Chordae Tendinae – Collagenous tendons – Attached to the flaps of the AV valve on the ventricular side – At opposite end, they are attached to papillary muscles Papillary Muscles – Mound-like extensions of ventricular muscle – Provide stability for the chordae tendinae – These muscles do not actively pull on the valve flaps – The AV valves move passively, respond to flowing blood pressing on them Chordae Tendinae and Papillary Muscles When a ventricle contracts, blood pushes against the bottom side of its AV valve and forces it upward into a closed position Chordae tendinae prevent the valve from being pushed into the atrium during contraction Prolapse: – If the chordae tendinae fail and the valve is pushed into the atrium Figure 14-9d Copyright © 2010 Pearson Education, Inc. Figure 14-9b Copyright © 2010 Pearson Education, Inc. Heart Valves Semilunar valves – Separate the ventricles from the major arteries – Look like “half-moon” shapes – Each made of 3 “cuplike leaflets” that snap shut to prevent backflow of blood (back into the ventricles) – Don't need connective tendons like the AV valves – Aortic semilunar valve • Located between L. ventricle and aorta – Pulmonary semilunar valve • Located between R. ventricle and pulmonary trunk Figure 14-9c Copyright © 2010 Pearson Education, Inc. Figure 14-9a Copyright © 2010 Pearson Education, Inc. Blood Flow Through the Heart Right Atrium – Deoxygenated blood enterrs R. Atrium from the superior and inferior vena cavae – R. Atrium contracts, sends blood through the tricuspid valve and into the R. Ventricle Right Ventricle – R. Ventricle contracts, sends blood through the Pulmonary semilunar valve into the pulmonary artery – Pulmonary Artery takes blood to lungs Figure 14-7g Copyright © 2010 Pearson Education, Inc. Blood Flow Through the Heart Left Atrium – Pulmonary veins bring freshly oxygenated blood from the lungs back to the L. Atrium – L. Atrium contracts, sends blood through the mitral valve into the L. Ventricle Left Ventricle – Largest and most powerful of the four heart chambers – L. Ventricle contracts, sends blood through the aortic semilunar valve and into the aorta – Aorta distributes blood to the entire body Figure 14-7g Copyright © 2010 Pearson Education, Inc. Figure 14-9d Copyright © 2010 Pearson Education, Inc. Figure 14-9b Copyright © 2010 Pearson Education, Inc. Figure 14-7h Copyright © 2010 Pearson Education, Inc. Cardiac Muscle (Myocardium) Most of the heart is composed of cardiac muscle Most cardiac muscle is contractile Approximately 1% of cardiac muscle cells are specialized to spontaneously generate action potentials Heart muscle is myogenic: the contraction signal originates within the heart itself, doesn't need external input to keep beating Cardiac Muscle (Myocardium) Pacemaker or autorhythmic cells – Specialized myocarial cells – These set the rate of the heartbeat Pacemaker cells are anatomicall distinct from other myocardium – Smaller than the other cells – Contain few contractile fibers – Lack organized sarcomeres – Don't contribute much to heart contraction Figure 14-10 Cardiac muscle Copyright © 2010 Pearson Education, Inc. Figure 14-10a Spiral arrangement of ventricular cardiac muscle Allows ventricular contraction to squeeze blood upward from the heart apex Copyright © 2010 Pearson Education, Inc. Myocardium or Cardiac Muscle Differs in significant ways from skeletal muscle Shares some similarities with smooth muscle 1. Cardiac muscle fibers much smaller than skeletal muscle fibers and have a single nucleus per fiber 3. Individual cardiac muscle cells branch and join (end-to-end) with neighboring cells. Intercalated disks form the cell junctions Figure 14-10b Copyright © 2010 Pearson Education, Inc. Intercalated disks are interdigitated membranes consisting of desmosomes and gap junctions Desmosomes – Strong connections, tie adjacent cells together – Allow force created in one cell to be transferred to the adjacent cell Gap Junctions – Electrically connect cardiac muscle cells – Allow waves of depolarization to spread rapidly from cell to cell – Makes possible nearly simultaneous contraction of entire heart 4. T-tubules of myocardial cells are larger than those of skeletal muscle and they branch inside the myocardial cells 5. Myocardial sarcoplasmic reticulum is smaller than that of skeletal muscle This is because cardiac muscle depends more on on extracellular Ca++ to initiate contraction In this, it resembles smooth muscle more than skeletal muscle 6. Mitochondria occupy about one third of cell volume in a cardiac muscle fiber Cardiac muscle fibers have a very high energy demand Cardiac muscle consumes 70-80% of the oxygen delivered to it by the blood. This is twice the amount of oxygen extracted from blood by other body cells The only way to get more oxygen to an exercising heart is to increase blood flow This is why blocked arteries can be so dangerous! Cardiac Muscle Contraction Fig. 14-11, p. 482 In cardiac muscle, an action potential intitiates EC coupling (like in the previous chapter), but here, the AP originates spontaneously in the heart's pacemaker cells It then spreads throughout the heart via the gap junctions connecting the cardiac muscle cells Neurotransmitters can modulate the pacemaker rate Cardiac Muscle Contraction Fig. 14-11, p. 482