* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Liu_Endocarditis Presentation
Remote ischemic conditioning wikipedia , lookup
Electrocardiography wikipedia , lookup
Coronary artery disease wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Heart failure wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Echocardiography wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
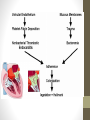
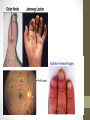
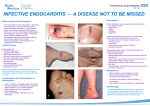
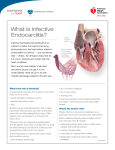
Endocarditis Wei Liu, BSN Penn State Nursing N 870 Introduction • Endocarditis is inflammation of the inside lining of the heart chambers (endocardium) and heart valves • It is commonly caused by bacteria infection, therefore we refer it to infective endocarditis (IE) • IE is an uncommon, but not rare, disease. The annual incidence ranging from 3 to 7 per 100,000 person-years in the most contemporary population surveys. • IE continues to be characterized by increased morbidity and mortality and is now the third or fourth most common lifethreatening infection syndrome, after sepsis, pneumonia, and intra-abdominal abscess. (AHA, 2015) Diagenosis • Infection of the endocardial surface of the heart, usually involving heart valves or an intracardiac device • Organisms: S. aureus, viridans streptococci, enterococci, and pseudomonas aeruginosa • Complications: • congestive heart failure, • arterial emboli, • myocardial infarction, • myocardial abscesses • death ( Sexton, 2015) Pathogenesis • Congenital or acquired heart condition • Alteration of the valvular endothelium leading to depositions of platelets and fibrin • Invasive procedures • Microorganisms in the circulating blood stream colonize on the damaged valvular surface or preexisting sterile vegetation • Microorganisms further propagate or enlarge the vegetation or cause systemic emboli • Further impeding blood flow and incite inflammation that involves the vegetation and adjacent endothelium ( Sexton, 2015) ROS • PMH: prior endocarditis, prosthetic valve or cardiac device, valvular or congenital heart disease, rheumatic fever, IV drug use, IV lines, immunosuppression, recent dental/surgical procedure • fever and chills • fatigue • nausea and vomiting • weight lost and anorexia • aching muscles and joints • night sweats • headaches • shortness of breath and cough • skin lesions • hematuria (NHLBI, 2010) Physical Exam • • • • • • • • General: chills, fatigue, and paleness vital signs: fever Eyes: Roth spots peripheral vascular: edema, clubbing, Splinter hemorrhages, Janeway lesions, and Osler's nodes Cardiovascular: onset/changed heart murmur, pleuritic pain Pulmonary: dyspnea, cough Gastrointestinal: splenomegaly, pain and fullness Neurological: confusion, sensory dysfunction Diagnostic Tests • blood cultures and echocardiography(TEE/TTE) • Sed rate, C-reactive-protein, urinalysis, WBC • modified Duke diagnosis criteria • definite endocarditis: 2 major criteria, 1 major criterion and 3 minor criteria, or 5 minor criteria • possible endocarditis: 1 major criterion and 1 minor criterion, or 3 minor criteria • The sensitivity of the Modified Duke Criteria is 98-100%, and the specificity is 93% • TEE has a substantially high sensitivity (76% to 100%) and specificity (94%), which is higher than TTE (Loeb et al, 2011 & Baddour, et al, 2015 ) Modified Duke Criteria Differential Diagnosis • • • • • Intravascular catheter infection Skin and soft tissue infection Cardiac device infection Prosthetic joint infection Sepsis And many more… This diagnosis of endocarditis (Red Flag) can be difficult to make, or the signs misleading, and there is a wide differential diagnosis to consider. (Sexton, 2015) Treatment • Antibiotic Therapy 4 to 6 weeks: based on the causative microorganism and its antibiotic susceptibility, and whether the involved valve is native or prosthetic. • Initial empiric therapy- Vancomycin or Ampicillin/Sulbactam (Unasyn) plus an Aminoglycoside (plus rifampin in patients with prosthetic valves) • Native Valve Endocarditis associates with staphylococci - Nafcillin and Gentamicin • Prosthetic Valve Endocarditi associate MRSA or coagulase-negative staphylococci - Vancomycin, Rifampin and Gentamicin • Vancomycin intolerance or resistant organisms Linezolid or Daptomycin (Baddour, et al, 2015 ) Treatment Con't • Surgical Therapy: patients with structural and functional damaged cardiac valves. • Anticoagulation: controversial • American Heart Association endocarditis treatment guidelines 2015: http://circ.ahajournals.org/content/early/2015/09/15/CIR.000 0000000000296.full.pdf+html Patient Education/Follow up • intravenous catheters should be removed promptly after antibiotic therapy • Monitor recurrent IE among intravenous drug abusers • echocardiography should be performed to establish a new baseline • monitored for complications such as valvular dysfunction, congestive heart failure, renal failure, and embolic phenomenon • provide information about daily dental hygiene; regular visits to the dentist; and the need for antibiotic prophylaxis for certain procedures (Pierce et, al, 2012) Outcomes • most of patients are able to recover with appropriate antimicrobial therapy. • The risk of embolization declines after institution of appropriate treatment. • in-hospital mortality rate is 18 to 23%; the six-month mortality rate is 22 to 27% • Complications: valvular dysfunction, congestive heart failure, renal failure, and embolic phenomenon (Spelman & Sexton, 2015) ) Reference: •Baddour, L. M., Wilson, W. R., Bayer A. S., Fowler, V. G., Tleyjeh, I. M., Rybak M.J., et al. (2015). Infective endocarditis in adults: diagnosis, antimicrobial therapy, and management of complications: a scientific statement for healthcare professionals from the American Heart Association. Circulation. 132(15), P1435-86 •Goroll, A. H., & Mulley, A. G. (2006). Primary care medicine: office evaluation and management of the adult patient. Philadelphia: Lippincott Williams & Wilkins. •Loeb, M., Smaill, F., & Smieja, M. (2011). Evidence based infectious diseases. 2nd ed. Chichester: Wiley-Blackwel. •National heart lung and blood institute (NHLBI). (2010). What is endocarditis. Retrieved from https://www.nhlbi.nih.gov/health/health-topics/topics/endo •Pierce, D., Calkins, B. C., & Thornton, K. (2012). Infectious endocarditis: diagnosis and treatment. American Family Physician, 85(10), p981-986 •Sexton, D. J. (2015) Pathogenesis of vegetation formation in infective endocarditis. UpToDate. Retrieved from http://www.uptodate.com/contents/pathogenesis-ofvegetation-formation-in-infective-endocarditis •Spelman, D., & Sexton, D. (2015). Complications and outcome of infective endocarditis. UpToDate. Retrieved from http://www.uptodate.com/contents/complications-and-outcome-of-infectiveendocarditis Questions?