* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Equalization of diastolic pressures
Heart failure wikipedia , lookup
Coronary artery disease wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Cardiac surgery wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
History of invasive and interventional cardiology wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Myocardial infarction wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
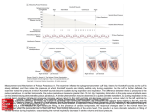
Hemodynamics for the Interventional Cardiologist Gregory J. Dehmer, MD Professor of Medicine, Texas A&M College of Medicine Director, Cardiology Division Scott & White Clinic Hemodynamics: What invasive cardiologists did before stents were invented 2007 SCAI Interventional Cardiology Fellows Course Gregory J. Dehmer, MD, FSCAI I have no relevant financial disclosures to make. Must Know Hemodynamics for PCI • How to measure pressures • Catheter behaviors • Hypotension during PCI • Tamponade Rules for Proper Pressure Recording • Use the same routine and (almost) never take a short cut • Critically assess the fidelity of the waveforms and exclude artifact Statham transducer • Time the events with the ECG • Always know the transducer level and zero position Disposable transducer Balancing and Zeroing • The “zero” position is: – Mid-chest level – Uppermost blood level in the chamber being measured* For the LV -5 cm below the LSB at the 4th LICS Error for other chambers – ± 0.8 mmHg for other chambers • The transducer should be placed at the “zero” position – Above zero = falsely low pressure – Below zero = falsely high pressure * Courtois M, et al. Circulation 1995;92:1994-2000. Common Errors and Artifacts • Over-damped waveform Over-damped Air bubble, clot or contrast in the line Soft compliant tubing Loose catheter connection Properly damped Common Errors and Artifacts • Underdamped waveform (“ring artifact”) Tubing too stiff or too long Hyperdynamic state Catheter tip in turbulent jet Common Errors and Artifacts • Catheter whip or fling “Fling” caused by extra loop of Swan Ganz in RV. Same patient after removal of extra loop Common Errors and Artifacts • Catheter malposition What’s the problem? • Loose connections, catheter kinks, faulty transducers RA catheter is near the TV and is periodically being “hit” by the valve creating high frequency noise Catheter Behaviors • Damping: loss of systolic and diastolic components Damping – Occlusion of the catheter tip Clot, vessel wall • – Kink in body of catheter – Balloon inflation within tip Ventricularization: loss of diastolic component “Ventricularization” – Occlusion of the coronary by the catheter – Transmural myocardial pressure – Guide too large, proximal spasm or proximal stenosis Hybrid: FLP Hypotension During PCI More Common • Bleeding • Vagal reaction • • Overmedication Technical considerations • • • Arrhythmia Shock Transient ischemic dysfunction – Low filling pressures 81 y/o man with prior CABG and LVEF 24% Investigational percutaneous-implanted LA pressure monitoring system Ritzema-Carter JLT. Circ 2006;113:e705 - e706 – Bezold Jarisch reflex – Pressure miscalibration / display – Loose connections Baseline Hemodynamic Changes During PCI Baseline After 3 min. With balloon inflation V waves to 80 mmHg During PCI Ritzema-Carter JLT. Circ 2006;113:e705 - e706 Hypotension During PCI • More Common Bleeding – Low filling pressures • Vagal reaction • • Overmedication Technical considerations • • • Arrhythmia Shock Transient ischemic dysfunction – Bezold Jarisch reflex – Pressure miscalibration / display – Loose connections Less Common • • • Tamponade Anaphylactoid rxn New or unsuspected valvular lesion – Acute MR – AS Hemodynamics of Tamponade • Incidence 0.12 – 0.6 % • Increased with newer devices • – Atherectomy – Hydrophilic wires GP IIb/IIIa inhibitors – Influence outcome (death) – Delayed presentation • May be delayed in 50% – Dx outside of the lab – 2 – 36 hrs post PCI Fejka M, et al. Am J Cardiol 2002;90:1183-86 Fasseas P, et al. Am Heart J 2004;147:140-45. Delayed Onset Tamponade • Symptoms – Chest discomfort – Tachypnea, dyspnea but clear lungs – Restlessness, agitation or drowsiness – Generalized weakness – Postural weakness/syncope • Signs – heart rate – Hypotension or relative hypotension – urine output – ± pericardial rub – Inspiratory JVP prominent x descent attenuated y descent – Electrical alternans – Pulsus paradoxus Hemodynamics of Pulsus Paradoxus Inspiration: pericardial pressure, augment right heart filling, shifting the septum to left further compressing the LV and systolic BP falls Expiration: augments left heart filling, shifting septum to the right, compressing the RV, but with an increase in BP. Pulsus Paradoxus • Nonpericardial Causes – COPD – Acute asthma – – – – – Diastolic and systolic fall with inspiration Hemorrhagic shock Tension pneumothorax Tracheal compression RV infarction Massive pulmonary embolism – Restrictive cardiomyopathy – Mediastinal and cardiac compression by tumors • Tamponade without pulsus paradoxus – Marked LVH – Severe left-sided CHF – Severe aortic regurgitation – Atrial septal defect – Extreme hypotension – Acute, large LV infarction – Local cardiac compression – Pericardial adhesions over the right heart Spodick DH. The Pericardium - A Comprehensive Textbook 1997 Equalization of Diastolic Pressures All diastolic pressures within 5 mmHg • Absent y descent in RA pressure – Pressure wave reflects blood flow – Total heart volume is fixed, thus blood can only enter when blood is leaving – y descent normally from a pressure drop at the opening of the TV during diastole. Blunted as no blood is leaving the heart in diastole – X descent from atrial relaxation during systole is preserved, as blood is leaving the RV during systole Differential of Impaired Diastolic Filling Constrictive pericarditis RV infarct Tamponade Restrictive cardiac disease < 1/3 Occasional Frequent Rare Prominent y descent “M “ or “W” Insp. Prominent y descent Prominent x descent Variable y descent Equalization of diastolic pressures Frequent Frequent Frequent Rare “Square root” sign Frequent Frequent Absent Variable Pulses paradoxus RA waveforms Insp. Diagnostic Criteria for Constriction Dynamic respiratory factors Traditional Criteria Sensitivity Specificity PPV NPV LVEDP vs. RVEDP < 5 mmHg 60 38 4 57 RVEDP vs. RVSP > 1/3 93 38 52 89 PASP < 55 mmHg 93 24 47 25 RV free wall > 7 mm 93 57 61 92 Respiratory change in RA , 3 mmHg 93 48 58 92 PCWP vs. LV > 5 mmHg 93 81 78 94 100 95 94 100 LV/RV Interdependence From: Kern MJ. Editor SCAI Interventional Cardiology Board Review Book Ventricular Interdependence Concordant pressures Restrictive Discordant pressures Constrictive