* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Heart Diseases
Saturated fat and cardiovascular disease wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Cardiovascular disease wikipedia , lookup
Electrocardiography wikipedia , lookup
Remote ischemic conditioning wikipedia , lookup
Drug-eluting stent wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Heart failure wikipedia , lookup
History of invasive and interventional cardiology wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Cardiac surgery wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
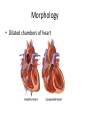
Heart Diseases Heart Failure • Decreased contractility power of the heart • Decreased cardiac output • Can affect right or left sides of heart Left-sided heart failure Causes: a. Ischemic heart disease (IHD), b. Systemic hypertension, c. Mitral or aortic valve disease. d. Diseases of myocardium e. Severe anemia Clinical symptoms • • • • • Fatigue Exretional Dyspnea (shortness of breathe) Orthopnea (recumbent position) Cough Impairment of renal and cerebral functions Right sided heart failure • • • • • Causes: Late consequence of left sided heart failure Pulmonary hypertension (cor pulmonale) Pulmonary or tricupid valve stenosis Left-right shunt Symptoms • • • • • • Systemic venous congestion Lower limb edema Hepatomegaly Splenomegaly Pericardial effusion Ascites Morphology • Dilated chambers of heart Ischemic Heart Disease (IHD) • Also known as Coronary Artery Disease(CAD) • Decreased oxygen demand to cardiac muscles • >90% of cases, due to reduced coronary blood flow secondary to obstructive atherosclerosis • Other causes: vasospasm, embolus, shock Clinical Presentation 1) Angina Pectoris ذبحة صدرية 2) Myocardial infarction احتشاء عضلة القلب 3) Chronic ischemic heart disease 4) Sudden cardiac death Angina pectoris • Most patients have “stable, or typical Angina”, characterized by: • Squeezing, retrosternal pain • Intermittent • Reversible (rest, drugs) • Short duration (<10 min) • Preceded by stress • Atherosclerosis in 70% of coronary arteries Unstable angina • • • • Appears at rest Longer duration Atherosclerosis occlusion 90% Commonly precedes myocardial infarction Prinzmetal Angina • Also known as variant angina • Caused by vasospasm Myocardial Infarction (MI) • Also known as heart attack • Can occur at any age but the frequency rises progressively with increasing age • Approximately 10% of MIs occur before age 40 • Men are at significantly greater risk than women, and women tend to be protected against MI during their reproductive years • However, menopause women with declining estrogen is associated with exacerbation of coronary artery disease and IHD is the most common cause of death in elderly women Pathogenesis • Complete arterial obstruction • Disease begin with atherosclerotic plaque in arteries, causing narrowing of the lumen • External factors, such as hypertension, vasospasm, adrenergic stress, causes disruption of plaque • Thrombus forms on the complicated plaque, causing complete lumen obstruction • Ischemic necrosis follows to the cardiac territory supplied by that vessel • Surge in adrenergic stimulation associated with awakening and rising may underlie that the incidence of acute MI is highest in early morning • 10% of cases results from vasospasm & no atherosclerosis Cardiac Cathetarization • Immediate medical intervention (angiography) can demonstrate the thrombus • If late (>12 hours), thrombus is demonstrated in only 60% of cases, due to fibrinolysis • Early administration of thrombolytics limit the degree of cardiac infarction Complications 1. Loss of contractility occurs within a minute of onset of ischemia and may be reversible 2. Myocyte coagulative necrosis, in severe ischemia lasting 20 to 40 minutes (if no intervention), can be fatal if massive (cardiogenic shock) 3. Heart failure 4. Arrhythmia: ventricular fibrillation is responsible for 90% of mortalities 5. Papillary muscle rupture: results in valve prolapse 6. Cardiac rupture: results in hemopericardium 7. Mural thrombus Morphology The extent of infarction depends on: 1.The size and distribution of the involved vessel 2. The rate of development and the duration of the occlusion 3. Extent of collateral supply MI is a white infarction 1) 2) Transmural infarctions: Involve > 50% of the myocardial wall thickness Subendocardial infarctions : limited to the inner third of the myocardium Collateral circulation • If an atherosclerotic lesion progressively occludes a coronary artery at slow rate over years, this causes remodelling of other coronary vessels which may provide a second compensatory blood flow • Such collateral perfusion can protect against MI even if the vessel eventually becomes completely occluded (alternative way for flow) • These collaterals normally are closed, gradual narrowing of one artery allows blood to flow from high to low pressure areas through the collaterals, therefore; gradual collateral dilation can provide adequate perfusion to myocardium • With acute coronary blockage, there is no time for collateral flow to develop and infarction results Clinical Symptoms 1) 2) 3) 4) 5) Severe crushing retrosternal chest pain that can radiate to the neck, epigastria, jaw or left arm In 10% to 15%, MIs may even be "silent" infarcts (particularly common in patients with diabetes mellitus) Rapid and weak pulse Nausea and sweating Dyspnea attributable to resultant acute pulmonary edema Diagnosis • Based on measuring blood levels of macro molecules that leak out of injured myocardial cells: Cardiac troponins and CK-MB(creatine kinase) have high specificity and sensitivity for MI • Electrocardiogram: specific changes occur in MI