* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download The ABCs of Genetic Testing
Artificial gene synthesis wikipedia , lookup
DNA supercoil wikipedia , lookup
Deoxyribozyme wikipedia , lookup
Non-coding DNA wikipedia , lookup
Whole genome sequencing wikipedia , lookup
Microevolution wikipedia , lookup
Neocentromere wikipedia , lookup
Birth defect wikipedia , lookup
Genomic library wikipedia , lookup
Genome (book) wikipedia , lookup
History of genetic engineering wikipedia , lookup
Medical genetics wikipedia , lookup
DiGeorge syndrome wikipedia , lookup
Genealogical DNA test wikipedia , lookup
Public health genomics wikipedia , lookup
Nutriepigenomics wikipedia , lookup
DNA paternity testing wikipedia , lookup
Genetic testing wikipedia , lookup
Comparative genomic hybridization wikipedia , lookup
Down syndrome wikipedia , lookup
Newborn screening wikipedia , lookup
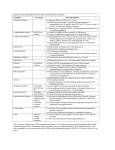
THE ABC’S OF GENETIC TESTING Garrett K. Lam, MD Professor and Chair, Dept of Ob/Gyn University of Tennessee COM Chattanooga Regional Obstetrical Consultants LEARNING OBJECTIVES 1. Compare the specificity and sensitivity of serum aneuploidy screening against NIPS 2. Explain the difference between NIPS vs true diagnostic testing 3. Assess the utility of cfDNA testing for detecting other chromosomal and genetic issues 4. Describe the utility of microarray in the workup of fetal demise Credits 1. Thanks to Dr. Owen Phillips (UT Memphis) and Janet Ulm (genetic counselor, ROC) for their direct contributions to this talk 2. Some of their slides have been incorporated into this talk with their express permission 3. Some of the slides are adapted from the Sequenom/LabCorp speaker’s slide deck. They are used for teaching purposes only, and do not mention their product and names are redacted. Survey says: What percentage of early pregnancy loss is attributable to aneuploidy? A. <5% B. 10% C. 25% D.50% Survey says: What is the proportion of pediatric inpatients with some type of genetic disorder? A. <5% B. 10% C. 25% D.50% Epidemiology of genetic disease Reproductive Approximately half of early pregnancy loss attributable to aneuploidy Average number of recessive traits each adult carries is 2-3 Incidence of microdeletion or duplication in structurally normal fetuses is about 1%; incidence is about 6% in structurally abnormal fetuses Epidemiology of genetic disease Childhood 3/1000 newborns have aneuploidy, and 9.2/1000 newborns have some type of structural rearrangement of chromosomes 7/1000 have autosomal dominant traits, 2.5/1000 have autosomal recessive traits, and 0.5/1000 have X-linked trait Among pediatric inpatients, more than 25% have a genetic disorder Over 1/3 pediatric deaths attributed to congenital anomalies – 17% of these due to chromosome abnormalities, and 12% due to some other recognized malformation syndrome Prenatal screening in US 10 years ago Define a woman’s risk for having a child with a chromosomal abnormality (age, previously affected) via risk factors With this information, offer serum screening or invasive testing (CVS or amniocentesis) Prenatal Screening in US NOW First Trimester (Combination) Screening Second Trimester Maternal Serum Screening NIPT CMA ???? Prenatal Trisomy 21 Screening Detection Rate & Testing Performance Screening Tests1 2nd Tri Triple Test 69 % 2nd Tri Quad Test 81% Screen Positive Rate NonDetection Rate 5% 5% 31% 19% 1st Tri Combined (+NT) 85% 5% 15% 1st & 2nd Full Integrated (+NT) 95% 5% 5% Diagnostic Confirmatory Tests2,3 Chorionic Villus Sampling (CVS) > 99.2% <0.8% Amniocentesis >99.7% <0.3% 1. Malone FD, Canick JA, Ball RH, Nyberg DA, et al. First-trimester or second-trimester screening, or both, for Down syndrome. First- and Second-Trimester Evaluation of Risk (FASTER) Research Consortium. N Engl J Med. 2005 Nov 10;353(19):2001-11. 2. Hsu LY, Perlis TE.United States survey on chromosome mosaicism and pseudomosaicism in prenatal diagnosis. Prenat Diagn. 1984 Spring;4 Spec No:97-130. 3. Ledbetter DH, Martin AO, Verlinsky Y, et al. Cytogenetic results of chorionic villus sampling: High success rate and diagnostic accuracy in the U.S. Collaborative Study. Am J Obstet Gynecol 1990;162:495. Newest Screening Test: NIPS (Non-Invasive Prenatal Screen) Done at 9-10 weeks or greater Screening test; not diagnostic Utilizes circulating cell free DNA (ccfDNA) in the mother’s blood “Fetal” DNA is actually of placental origin Screens for: Trisomy 21 Trisomy 18 Trisomy 13 X and Y chromosome abnormalities Microdeletions optional in some labs Detects sex of baby Detection rate 85-99%. False positive rate <1% Black- euploid fetus Red- Fetus with Trisomy 21 NIPS Tests Available MaterniT21Plus (Sequenom) Verifi (Progenity) Harmony (Ariosa) Panorama (Natera) InformaSeq (LabCorp) Qnatal Advanced (Quest) Informed Pregnancy Screen (Counsyl/PathGroup) Survey says: NIPS is such a highly sensitive test, that I feel comfortable ordering it to diagnose or rule out an aneuploidy with a positive serum screening test result 1. I agree 2. I disagree 3. I don’t know Procedure Blood sent to processing lab Determine fetal fraction (at least 4% to run specimen)-thus GA at time of testing is important Sequence all DNA in specimen (shot gun sequencing) or use of site specific probes Analyze for 13, 18, 21, presence of Y Report ‘positive’ if excess 13, 18 or 21 is present DATA ON DETECTION RATE OF TRISOMY 21, 18 AND 13 BY CCFF DNA Trisomy 21 Number of cases Detected Performance 210/212 Sensitivity 99.1% Specificity 99.9% Trisomy 18 59/59 Sensitivity 99.9% Specificity 99.6% Trisomy 13 11/12 Sensitivity 91.7% Specificity 99.7% Palomaki GE, et al.. DNA sequencing of maternal plasma reliably identifies trisomy 18 and trisomy 13, as well as Down syndrome: An international collaborative study. Genet Med. 2012 Jan 26. doi: 10.1038/gim.2011.73. NIPS: Accuracy= Detection rates and FPR: Not 100% NIPT result N (%) True positive for T21 119/126 (94.4%) False positive for T21 7/126 (5.6%) True positive for T18 25/42 (59.5%) False positive for T18 17/42 (40.5%) True positive for T13 12/27 (44.4%) False positive for T13 15/27 (55.6%) True positive for SCA 11/29 (37.9%) False positive for SCA 18/29 (62.1%) Wang et al, Genet Med 2015 Why NIPS can be wrong False positives Confined placnetal mosaicism vanishing twins Microdeletion/duplication Maternal conditions False negatives Obesity ‘no calls’ from low fetal fraction trisomies other than T21 chromosome rearrangements (translocations, microdeletions/duplications) ACOG Opinion “Given the performance of conventional screening methods, the limitations of cell free DNA screening performance, and the limited data on cost-effectiveness in the low-risk obstetric population, conventional screening methods remain the most appropriate choice for first-line screening for most women in the general obstetric population.” -Committee Opinion Number 640, September 2015 Microdeletions: The “Seek” tests Microdeletion syndromes-covers five clinically relevant microdeletions. References 3. Data on file, Illumina, Inc. Microdeletion detection by NIPT The “Seek tests”) ACMG and ACOG recommend against screening Played on fears “Test for everything” Serious conditions, but exceedingly rare (PPV issues) Most common (1/2000): del 22q11.2 Rare disorders: PPV an issue 5.3% Kids may have heart defect Kids may have just a psychiatric disorder How do you counsel for that? ACOG Opinion Routine cell free DNA screening for microdeletion syndromes should not be performed. The PPV for microdeletions is much lower than for the Trisomies because the prevalence is lower. Cell free DNA screening is not recommended for women with multiple gestations. -Committee Opinion Number 640, September 2015 Professional Recommendations for NIPS • • • • • • Advanced Maternal Age Previous Pregnancy with a Trisomy Family History (i.e. balanced translocation) Positive Multiple Marker Screening Abnormal Ultrasound Findings Soft Markers for Aneuploidy Why just high risk groups? Why not all patients? 1. Understanding PPV 2. Issue of rarer trisomies and other chromosome abnormalities in younger patients 3. Large studies yet to be published Detection rate/Sensitivity vs PPV The # true positives/total number of cases x 100 How many affected cases did the test pick up EX: 212 cases in a population. Test detected 209 and missed 3. DR= 209/212 (X 100)= 98.6% PPV=What are the odds that a positive result means the fetus is truly affected. Since there are false positives, the PPV depends on the prevalence of the disease in the population. If there is low prevalence, the positive result is most likely a false positive as the disease is so rare. For trisomies, PPV differs based on age Sensitivity Specificity Age 25 PPV (%) Age 40 PPV (%) Trisomy 21 99.3 99.8 33 87 Trisomy 18 97.4 99.8 13 68 Trisomy 13 99.9 9 57 91.6 -In younger women, a positive result is more likely to be a false positive than in older women because fewer cases are seen. -Since not 100% accurate-should report out an adjusted risk -Regardless, positive predictive value means all positive tests need diagnostic confirmation AJMG: 2010; Grati et al In women > 35 y/o NIPT detected 65.1% of all clinically significant chromosome abnormalities Why?– AMA=More trisomies, specifically 21, 18 and 13 In women < 35 y/o NIPT detected 45.8% of all clinically significant chromosome abnormalities. Fewer abnormalities present were trisomies Traditional serum screening in low risk population Norton et al, Obstet Gynecol, 2014 Traditional screening (first trimester and quad screening) in low risk population followed by amniocentesis Found 17% of clinically significant chromosomal abnormalities that would not have been by NIPT ccfDNA does outperform traditional screening for T21, but that is about all we can say, so ACOG recommends in low risk population: “Traditional” serum screening should be performed “Invasive” (Diagnostic) Testing: is it dangerous? Danish Fetal Medicine Study Group 147,987 women who underwent FTS for Down syndrome 5072 CVS (transabdominal, 18/20 g double needle technique) 1809 amniocentesis (20 g needle) 141,106 women had no procedure CVS loss difference ranged from -0.08% at 3 days to -0.21% at 21 days after screening Amniocentesis loss difference ranged from 0.56% at 28 days to 0.52% at 42 days after screening Conclusion: No statistically significant differences between those women having a procedure and those not having one Wulff CB et al; Ultrasound Obstet Gynecol 2016;47:38-44. ‘Prenatal Diagnosis’ Advantages Chromosomal abnormalities will be missed by ccfDNA, but detected with testing. Some women who receive a screen positive result from MSS may ask about cell free technology rather than definitive PD May delay definitive diagnosis and management plan as well risk missing some pregnancies with aneuploidy Risks of invasive nature are negligible compared to benefit in high risk patients Obstet Gynecol: 2015; Benachi et al Compared effectiveness of NIPT in 2 groups: Group 1: indications like AMA, screen positive on serum screening Group 2: Ultrasound abnormalities NIPT DR (Confirmed by amnio): both groups T21 100% T18 88% T13 100% BUT: Group 1 (n=510): 2.5% cases were NIPT negative but had other significant findings on Invasive testing Group 2 (n= 376) 7.7% cases were NIPT negative but had other significant findings on Invasive testing Reasonable approach Offer low risk patients: MSS or PD (amnio or CVS) Offer high risk patients (AMA, +MSS, previously affected child) ccfDNA or PD (amnio or CVS) (ACOG) cfDNA really for 21, 18 Evidence: PD Safe and detects 99.7% of all chromosome abnormalities 2nd screen delays PD by 7-10 days Offer patients with fetal ultrasound anomalies: PD (amnio or CVS) ACOG: cfDNA really for 21, 18. Go to amnio Evidence: PD Safe and detects 99.7% of all chromosome abnormalities and can follow up with microarray Positive ccfDNA Recommendations: Do not use ultrasound for risk reduction. Go to CVS or amnio Evidence: US has lower sensitivity than ccfDNA. PD Safe and detects 99.7% of all chromosome abnormalities. All women should be offered the option of aneuploidy screening or diagnostic testing….choice of screening test is affected by many factors NIPS not recommended for women with multiple gestations. All positive NIPS results should have a diagnostic test before considering pregnancy termination NIPS should not be used as a substitute for diagnostic testing Cell-free DNA for microdeletions has not been validated clinically and should not be offered at this time Women whose NIPS results are inconclusive or not resulted because of low fetal DNA content should be offered testing Survey Says: 38 y/o (AMA) G3P1011 presents with IUFD at 20.5 wk found at anatomy US. CVS = 46,XX MSAFP only elevated at 3.5MoM US with abnormal fetal body positioning (hyperextension) and clefting of face Your next step is: 1. Fetal autopsy 2. Send fascia lata/achilles for FISH & karyotype 3. Send placenta for chromosomal microarray Diagnostic Technology: Microarray Aka Comparative Genomic Hybridization (CGH), Chromosomal microarray (CMA), SNP array Helps further characterize abnormalities seen by karyotyping (e.g. unbalanced translocations, marker chroms) and detects chromosome imbalances such as deletions or duplications that are too small to be seen by the microscope and may cause multiple congenital abnormalities and/or known genetic syndromes. Gains or losses are called copy number variants (CNVs) Will not detect balanced translocations. Google Scavenger Hunt What tissue sample needs to be sent for a CMA? -use your smartphone to find the answer • Chromosomal microarray analysis have been found to detect a pathogenic (or likely) copy number variant in approximately 1.7% of patients with a normal ultrasound exam and a normal karyotype • CMA detected all aneuploidies that routine karyotyping detected • It is recommended that microarray be made available to any patient choosing diagnostic testing, and may eventually replace conventional karyotype for patients undergoing prenatal diagnosis ACOG Opinion “In patients with a fetus with one or more major structural abnormalities identified on ultrasonographic examination and who are undergoing invasive prenatal diagnosis, chromosomal microarray analysis is recommended.” -Committee Opinion , Number 581, December 2013 Microarray Statistics In samples from fetuses with growth or structural anomalies, 6% had clinically relevant findings on microarray that were not found on karyotyping. With indication of AMA or abnormal screening for Tri 21, 1.7% had clinically relevant finding on microarray not detected on routine karyotyping. Wapner, et al. NEJM, December 6, 2012 Issues with Microarray Variants of unclear significance Coincidental findings Cost Conclusions ACOG Committee Opinion: no. 640; September 2015 NIPT(S) does not replace CVS or amniocentesis - should remain options (the gold standard for diagnosis) NIPS, though powerful, is a screening, not diagnostic tool Sensitivity does not equal positive predictive value the performance of the test is affected by disease prevalence Similarly, microdeletion testing by ccfDNA is of limited use CMA is valuable at detecting specific genetic mutations that are below the karyotypic (subchromosomal) level, at a scope beyond what microdeletion testing can offer Good for IUFD and searching for answers when karyotype does not offer any help Extra slides for discussion Terminology: Basics of traits Germline (versus somatic) mutation Heterozygous/Homozygous/X-linked Microsatellite (as in microsatellite instability) – normally occurring repetitive sequence of DNA within the genome that can be used as a genetic “marker”, but also may predispose to mutation and gene disruption Terminology: Diagnostic studies Genome-wide association studies – examination of genetic “markers” among many individuals to find common genetic variations associated with disease states Hybridization (as in comparative genomic hybridization) – annealing of a single-strand of nucleic acid (usually DNA that carries some type of chemical identification, such as fluorescence) to its complementary strand Terminology: Diagnostics Next-gen sequencing – new technologies that allow for more rapid and less costly DNA sequencing Whole genome sequencing Whole exon sequencing Oncogene (and proto-oncogene) Tumor suppressor gene Microdeletion syndromes (examples) Cri-du-Chat…5p minus (46,XX,del(5p) ) Wolf-Hirschhorn…4p minus (46,XY,del(4p) ) DiGeorge…22q11.2 deletion, aka Velo-Cardio-Facial syndrome, Sphrintzen syndrome 46,XX,ish del(22)(q11.2q11.2) (D22S75-) OR arr cgh 22q11.2 (D22S75)X1 Case Example Abnormality noted on U/S: micrognathia Amnio FISH: Normal male Microarray: “Normal result with the exception of a recessive disease risk” A 56.10 kb heterozygous deletion …was detected. Individuals with this gene deletion are generally asymptomatic carriers for glycogen storage disease IXb. Newer Diagnostic Technology: Whole Exome Sequencing Sequencing of the protein coding regions of the genome (exons) (approximately 1% of the genome) Useful in prenatal when chromosomal analysis and microarray have been normal and particularly when there has been a recurrence of the same abnormalities Modes of Inheritance Mitochondrial inheritance e.g. Leber hereditary optic neuropathy, MERRF (Myoclonic Epilepsy with Ragged-Red Fibers) Mitochondrial DNA only transmitted by the mother. NO transmission by the male. Thus affected males do not have affected offspring. Affected females MAY have a very high chance of having affected offspring Mitochondrial Inheritance Uniparental Disomy (UPD) Both chromosomes or portions of chromosomes inherited from the SAME parent. Examples: Prader-Willi syndrome -mat UPD15 Angelman syndrome -pat UPD 15 Beckwith-Wiedemann syndrome -pat UPD 11 Web resources ACOG.org Genome.gov OMIM.org Genereviews.org (www.ncbi.nlm.nih.gov/books/NBK1116/) ACMG.net NSGC.org Genetests.org What about multiples? An issue with serum screening Fetal DNA into maternal circulation detected Canick et al 25 twins: 17 were euploid 5 discordant for trisomy 21 (100% DR) 2 concordant for trisomy 21 (100% DR) 1 discordant for trisomy 13 (100% DR) No cases of trisomy 18 in this set Results of prenatal testing Traditionally Cell Culture (10 days to 3 weeks) Karyotype (computer-assisted) +/- Fluorescent In situ hybridization (rapid 1-2 days) Karyotype FISH Interphase cells No culture needed Cells are 3 dimensional View can distort count of signals First Trimester Screening Biochemistry Free beta hCG PAPP-A Ultrasound Nuchal Translucency Nasal Bone First Trimester Screening Biochemistry: Can be drawn as early as 9 weeks gestation until 13+6. Ultrasound measurements: CRL must be 45-84 mm Advantages of First Trimester Screening Higher detection rate (85-95% for Trisomy 21 and 18) Earlier detection Separate risk estimates for twins Will take into account previous pregnancy with Trisomy 21 or 18. Disadvantages to First Trimester Screening Sonographer must be specially certified for NT and NB measurements Some patients do not present for care early enough for screening. Does not detect open neural tube defects (can draw AFP ONLY in 2nd trimester) Maternal Serum Screening in Second Trimester Quad screen Penta screen AFP hCG Estriol Inhibin Hyperglycosylated hCG (Penta only) Maternal Serum Screening Done at 15-20 weeks gestation Screens for: Open NTDs (AFP only) 85% detection rate Trisomy 21 80% detection rate Trisomy 18 60% detection rate False positive rate 5% Advantages of Prenatal Diagnostic Testing If you go from MSS (5% positive rate) to PD with a karyotype will detect additional 17% chromosomal abnormalities (not T21, 13, 18) If microarray is used, an additional 2% (over karyotype) chromosomal abnormalities (deletion or duplication syndromes) will be detected