* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Congenital Heart Defects
Heart failure wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Aortic stenosis wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Coronary artery disease wikipedia , lookup
Infective endocarditis wikipedia , lookup
Myocardial infarction wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Cardiac surgery wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Congenital heart defect wikipedia , lookup
Atrial septal defect wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
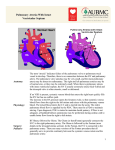
Congenital Heart Defects Kirsten H. Ohler, PharmD, BCPS Clinical Assistant Professor Neonatal / Pediatric Clinical Pharmacist University of Illinois at Chicago Objectives • Review normal fetal and pediatric cardiac anatomy • Describe the diagnosis of congenital heart disease • Discuss select congenital heart defects and their surgical repairs • Describe the pharmacist’s role in the care of a neonate or child with congenital heart disease Background • ~35,000 babies born per year w/ a cardiac defect • Cause of more deaths in 1st year of life than any other birth defect • Risk factors: diabetes, illicit drugs, hereditary (?), maternal viral infection (ex. rubella) ♦ association with genetic abnormalities like Trisomy 21 (i.e. Downs syndrome) and DiGeorge syndrome Fetal Circulation • Oxygenated blood enters right atrium via inferior vena cava • Pulmonary pressure greater than systemic • Right to Left shunt across foramen ovale and PDA Normal Cardiac Anatomy • Right side = deoxygenated blood • Left side = oxygenated blood • Systemic pressure greater than pulmonary • Foramen ovale and PDA closed Congenital Heart Defects: Diagnosis • Clinical Presentation ♦ murmur ♦ cyanosis ♦ blood pressure • hypotension • four extremity variation - CoA ♦ widened pulse pressure • PDA ♦ failure to thrive ♦ respiratory distress/ tachypnea / exercise intolerance ♦ congestive heart failure • Echocardiogram findings Congenital Heart Defects • Acyanotic defects ♦ atrial septal defect (ASD) • 1 in 1500 live births • ~6 – 10% of CHD frequently asymptomatic diagnosed in later childhood ♦ ventricular septal defect (VSD) • 1.5-3.5 in 1000 live births • 20 – 25% of CHD symptoms depend on size endocarditis prophylaxis ♦ endocardial cushion defects (AV canal / AVSD) • 0.19 in 1000 live births • ~4 – 5% of CHD symptoms similar to large VSD endocarditis prophylaxis ♦ patent ductus arteriosus (PDA) ♦ coarctation of the aorta (CoA) Patent Ductus Arteriosus • 1 in 2500 live births • incidence in preterms • ~9 – 12% of CHD • connects pulmonary artery to aorta ♦ usually closes by 3 -7 days • closure by PGE inhibition or surgical ligation ♦ endocarditis prophylaxis until closed PDA: Pharmacological Closure • Indomethacin vs. Ibuprofen ♦ MOA: prostaglandin inhibition ♦ similar closure rate (60-80%) • ~40% with second course ♦ IV administration • INDO: q 12 hours x 3 doses – Infuse over 20 – 30 minutes • IBU: q 24 hours x 3 doses ♦ Oral administration • 64 VLBW randomized to oral or IV IBU • No difference in closure rates or side effects PDA: Pharmacological Closure • Indomethacin vs. Ibuprofen ♦ Prophylactic indomethacin • Reduces PDA, need for surgical ligation, severe IVH • No effect on renal function, NEC, bleeding • Long-term benefits unknown ♦ Side effects • Nephrotoxicity: IBU < INDO (7% vs 19%) – reversible • NEC: IBU < INDO • CLD/BPD and hemorrhage: PDA: Surgical Closure • Success of drug therapy decreases significantly after ~ 10 - 14 days of life • May be indicated if pharmacological closure fails or is contraindicated Coarctation of the Aorta • ~ 5 – 8 % of CHD • Degree of aortic narrowing varies • Upper extremities’ blood pressure higher than lower extremities’ • PGE1 may improve systemic blood flow CoA: Repair • Resection with end-to-end anastomosis • Restenosis at the site of repair may occur • Post-procedure rebound hypertension may occur ♦ β-blockers, ACEI CoA: Repair • Other options: ♦ graft bypass ♦ subclavian flap repair ♦ patch aortoplasty Congenital Heart Defects • Cyanotic defects ♦ ♦ ♦ ♦ ♦ ♦ hypoplastic left heart syndrome (HLHS) tetralogy of Fallot (TOF) transposition of the great arteries (TGA) truncus arteriosus (TA) total anomalous pulmonary venous return (TAPVR) tricuspid valve atresia Hypoplastic Left Heart Syndrome • Hypoplastic left ventricle is unable to support systemic circulation • Often, aortic and mitral valves are atretic or nearly atretic • Patent foramen ovale and ASD allow mixing of blood • Systemic blood flow is dependent on PDA • Right ventricle acts as single ventricle Hypoplastic Left Heart Syndrome • Ductus Arteriosus: allows R L shunting of mixed blood from pulmonary artery to aorta • Patency is dependent on prostaglandin concentration and oxygen tension • Prostaglandin E1 (PGE1,alprostadil, Prostin VR®) ♦ continuous IV administration maintains patency of DA ♦ administer via large vein or umbilical artery catheter ♦ side effects: apnea, flushing, hypotension, fever HLHS: Stage I Repair • Norwood Procedure ♦ usually w/in 1st few weeks of life ♦ ligation of PDA ♦ “neoaorta”: attaches RV to aortic arch using pulmonary artery ♦ Blalock-Taussig (BT) shunt: provides pulmonary blood flow from aortic arch to branch pulmonary artery HLHS: Stage II Repair • Bidirectional Glenn Shunt (Hemi-Fontan procedure) ♦ usually at 4 – 6 months of age ♦ volume load of single RV ♦ removes BT shunt ♦ connects SVC to branch pulmonary artery HLHS: Stage III Repair • Fontan Procedure ♦ usually at ~ 2 years old ♦ completes the separation of systemic and pulmonary blood flow ♦ connects IVC to branch pulmonary artery ♦ fenestration allows run-off if PVR acutely increases Tetralogy of Fallot • 10% of CHD • 4 defects ♦ VSD ♦ overriding aorta ♦ pulmonary stenosis / atresia ♦ RV hypertrophy • Pulmonary blood flow may be ductal dependent ♦ PGE1 • “Tet” spells ♦ hyperpnea, cyanosis, syncope ♦ Propranolol TOF: Repair • Palliative repair with modified BT shunt may occur first • Patch closure of VSD • Patch to enlarge PA • Removal of subpulmonary obstructive tissue Transposition of the Great Arteries • 5% of CHD • Parallel blood flow circuits ♦ Aorta originates from RV ♦ Pulmonary artery originates from LV • Oxygenation of systemic blood is ductal dependent ♦ PGE1 TGA: Temporary Repair • Balloon atrial septostomy ♦ cardiac cath via PFO • Removes atrial septum to allow mixing of oxygenated and deoxygenated blood • PGE1 no longer required TGA: Repair • Arterial switch ♦ usually w/in the 1st few weeks of life • Stenosis at the reanastomosis sites may occur Truncus Arteriosus • 1 – 3% of CHD • One great vessel gives rise to coronary arteries, branch pulmonary arteries, and aortic arch • Large VSD with RV hypertrophy • Not generally ductal dependent unless interrupted aortic arch is present TA: Repair • Initial management is symptomatic ♦ diuretics, digoxin, ACEI • Definitive repair usually occurs at 6-8 weeks of life ♦ Patch closure of VSD ♦ Valved homograft from RV to pulmonary artery • Homograft does not grow must be replaced at ~ 3-6 yrs and again in adolescence Bacterial Endocarditis Prophylaxis Circulation 2007;116:1736-54. Bacterial Endocarditis Prophylaxis Dental Procedures Prophylaxis is Reasonable • All dental procedures involving manipulation of gingival tissue or perforation of oral mucosa Prophylaxis is NOT Warranted • Placement / adjustment of orthodontic appliances • Shedding of deciduous teeth • Bleeding from lips or oral mucosa Circulation 2007;116:1736-54. Bacterial Endocarditis Prophylaxis Other Procedures Prophylaxis is Reasonable • Incision or biopsy of respiratory mucosa • Tonsillectomy or adenoidectomy Prophylaxis is NOT Warranted • Cardiac catheterization, implanted pacemaker • Respiratory Tract ♦ intubation, bronchoscopy, tympanostomy tube insertion • GI / GU Tract ♦ transesophageal echo, endoscopy ♦ urethral catheterization, circumcision Circulation 2007;116:1736-54. Circulation 2007;116:1736-54. Role of the Pharmacist • Identify patients requiring endocarditis prophylaxis • Identify patients at risk for altered pharmacokinetic parameters Conclusions