* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download PERI – ARREST ARRHYTHMIAS
Survey
Document related concepts
Management of acute coronary syndrome wikipedia , lookup
Coronary artery disease wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Heart failure wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Cardiac surgery wikipedia , lookup
Jatene procedure wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Myocardial infarction wikipedia , lookup
Electrocardiography wikipedia , lookup
Atrial fibrillation wikipedia , lookup
Ventricular fibrillation wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Transcript
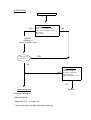
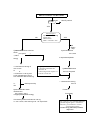
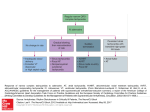
PERI – ARREST ARRHYTHMIAS Anu Roy BACKGROUND The term ‘peri – arrest arrhythmias’ are used to describe cardiac rhythm disorders that may precede cardiac arrest or follow initial resuscitation from a cardiac arrest. Effective treatment of such arrhythmias may prevent cardiac arrest. A clear trace showing ‘P’ waves and ‘QRS’ complexes is mandatory for diagnosis. A 12 - lead ECG is essential for the management of tachycardias associated with a broad QRS complex. When the mechanism of a Broad Complex Tachycardia cannot be determined regard it as VT (ventricular tachycardia ), especially in the clinical context of ischaemic heart disease. PRINCIPLES OF TREATMENT It is important to treat the patient and not the ECG. The two basic questions are : 1. How is the patient? 2. What is the arrhythmia? Adverse signs or symptoms dictate the appropriate treatment for most arrhythmias. They are - • • • Clinical evidence of low cardiac output pallor, sweating, cold extremities, impaired consciousness, hypotension. Excessive tachycardia or bradycardia Heart failure CLASSIFICATION OF THE PERIARREST ARRTHTHMIAS 1. BRADYCARDIA A bradycardia is defined as a ventricular rate below 60 beats / min. It is also important to classify a bradycardia as absolute (< 40 beats / min) or relative, when the heart rate is inappropriately slow for his or her haemodynamic state. 2. BROAD COMPLEX TACHYCARDIA In the context of resuscitation, a broad complex tachycardia will almost invariably be ventricular in origin. If there is no palpable pulse, the patient should be treated as for ventricular fibrillation 3. NARROW COMPLEX TACHYCARDIA Supraventricular in origin. Can be a trigger for ventricular fibrillation in vulnerable patients. Atrial fibrillation, on the other hand, occurs commonly in the early period after resuscitation. ALGORITHMS. BRADYCARDIA YES Adverse signs ? *Systolic BP < 90 mmHg *Heart rate < 40 beats / min *Ventricular arrhythmias requiring suppression *Heart failure NO Atropine 500mcg i.v. initially to maxm 3 mg Satisfactory Response ? YES NO NO YES Risk of asystole ? *Recent asystole *Mobitz II AV block *Complete heart block with broad QRS *Ventricular pause > 3 secs NO Interim measures: *Atropine 500mcg IV *External pacing *Adrenaline IV 2 – 10 mcg / min * Seek expert help (arrange transvenous pacing) Observe BROAD COMPLEX TACHYCARDIA Pulse ? NO Use VF protocol YES NO Adverse signs ? *Systolic BP < 90mmHg *Chest pain *Heart failure *Rate > 150 beats / min YES Seek Expert Help Synchronised DC If potassium known to be low shock ( see panel ) J; 360 J 100 J; 200 or equivalent biphasic energy >> Amiodarone 150 mg IV over 10 min to or >>Lidocaine i.v. 50 mg over 2 min repeated every 5 min to a maximum dose of 200 mg i.v. min **give potassium chloride up to 60 mmol, maximum rate 30 mmol / hr **Give magnesium sulphate i.v. 5 ml 50 % in 30 min. Seek expert help Synchronised DC shock cardioversion 100 J; 200 J; 360 J or appropriate biphasic energy If necessary, further amiodarone 150 mg i.v. over 10 min, then 300 mg over 1 hr & rpt shock If potassium known be low, see panel > >Amiodarone 150 mg over 10 Further if necessary For refractory cases consider additional pharmacological agents : amiodarone, lidocaine, procainamide or sotalol; **Or overdrive pacing Caution: drug induced myocardial depression THE ALGORITHMS (continued ) Narrow complex tachycardia ( Presumed supraventricular tachycardia ) NARROW COMPLEX TACHYCARDIA Pulseless ( heart rate usually > 250 beats / min) Atrial fibrillation Synchronised DC shock 100 J; 200 J; 360 J below* or appropriate biphasic energy see Vagal manoeuvres ( caution if possible digitalis toxicity, acute ischaemia, or presence of carotid bruit for carotid sinus massage ) Adenosine 6 mg by rapid bolus injection; if unsuccessful, follow, if necessary, with up to 3 doses each of 12 mg every 1 – 2 min Caution with adenosine in known WPW syndrome Seek expert help • • • No• Adverse signs ? Systolic BP < 90 mHg Chest pain Heart failure Heart rate > 200 beats / min Choose from : Esmolol – 40 mg over 1 min + infusion 4 mg / min ( i.v. injection can be repeated and infusion increased incrementaly to 12 mg / min ), OR *Verapamil 5 – 10 mg i.v. OR *Amiodarone – 300mg i.v. over 1 hr, may be repeated once if necessary * Digoxin – maximum dose 500 mcg i.v. over 30 min x 2 Yes Synchronised DC shock 100 J; 200 J; 360 J or equivalent biphasic energy 150 mg iv over 10min, the 300 mg over 1hr & rpt shock * Atrial Fibrillation ( AF ) AF is a chaotic, irregular atrial rhythm at 300 – 600 beats / min. It is common in the elderly. ECG shows absent ‘P’ waves, irregular ventricular rate. The appropriate treatment for AF is determined from the patient’s relative risk. It is helpful if time of onset of AF is known. Management of AF : seek help of a senior colleague if necessary In acute situations, assess the haemodynamic stability of the patient. If patient unstable ( heart rate >150 beats/min; ongoing chest pain; critical perfusion ) – urgent DC cardioversion ( 100J; 200J; 360J ). If cardioversion fails : Amiodarone 300mg i.v. over 1 hr and if necessary, may be repeated once. Or Flecainide 100 – 150 mg i.v. over 30 mins. Rate control medications include – verapamil / digoxin / diltiazem / betablockers. Treat complications (e.g. heart failure). Consider anticoagulation: heparin / warfarin. NOTES DC shock is always given under sedation / general anaesthesia. Verapamil is not to be used in patients receiving Betablockers. The algorithms include doses based on adult of average body weight and may need adjustment For paroxysms of torsades de pointes, use magnesium (as used in algorithm above) or overdrive pacing (seek expert help). Little harm results if SVT is treated as a ventricular arrhythmia but the converse error may have serious consequences. Pre-excited AF. This is a chaotic, broad complex tachydysrhythmia that occurs in the context of WPW and related conditions. It may be confused with V, VF or torsades. It may be treated with Flecainide or DC cardioversion. It may degenerate into VF if treated with Adenosine, Lignocaine, Gigoxin or Verapamil . Pre-excited atrial fibrillation