* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Burns Pulm Lect 1 Physiol 2017
Cushing reflex wikipedia , lookup
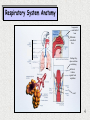
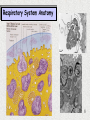
Pre-Bötzinger complex wikipedia , lookup
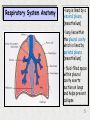
Haemodynamic response wikipedia , lookup
Circulatory system wikipedia , lookup
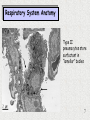
Biofluid dynamics wikipedia , lookup
Homeostasis wikipedia , lookup
Intracranial pressure wikipedia , lookup
Cardiac output wikipedia , lookup
Hemodynamics wikipedia , lookup
Common raven physiology wikipedia , lookup
Physiology of decompression wikipedia , lookup
Acute respiratory distress syndrome wikipedia , lookup
OPTO 5331 General Pathology and Medicine Respiratory Physiology Dr. Alan Burns Room 2168 [email protected] Spring 2017 1 Reading Chapters 27-31 in Principles of Physiology (4th ed.) by Berne & Levy 2 Respiratory System Anatomy 3 Respiratory System Anatomy Long narrow curled shelf of bone Turbinates – smooth air flow Cartilage flap depressed when swallowing Protects trachea against food aspiration cord 4 Respiratory System Anatomy • lung is lined by a visceral pleura (mesothelium) • lung lies within the pleural cavity which is lined by parietal pleura (mesothelium) • fluid-filled space within pleural cavity exerts suction on lungs and helps prevent collapse 5 Respiratory System Anatomy Alveolar cell types • Type I pneumocytes are squamous epithelial cells through which gas exchanges – 95% surface area •Type II pneumocytes are cuboidal epithelial cells that secrete surfactant – 5% surface area • Other cells: macrophages, capillary endothelial cells, fibroblasts and blood 6 elements Respiratory System Anatomy Type II pneumocytes store surfactant in “lamellar” bodies 7 Respiratory System Anatomy 8 Respiratory System Anatomy Surfactant • Mix of phospholipid, protein, carbohydrate • Major component is dipalmitoylphosphatidyl choline • Reduces surface tension so prevents collapse of alveoli • Lack of surfactant causes respiratory distress syndrome in premature infants (surfactant production begins at 32 weeks) 9 Functions of Respiratory System Primary Function Secondary Functions • Gas exchange • • • • • – entry of O2 – elimination of CO2 Acid-base balance in blood Speech Defense against microbes Circulatory filter Blood Reservoir Acid - Base Balance Carbonic Acid (H2CO3) and Bicarbonate (HCO3-) Buffer System In blood: CO2 + H2O ↔ H2CO3 ↔ H+ + HCO3- Response to change in pH is INSTANTANEOUS and constitutes the body’s first line of defense against acid-base imbalance 11 Acid - Base Balance CO2 + H2O ↔ H2CO3 ↔ H+ + HCO3- •Henderson-Hasselbalch equation: pH=6.1 + log([HCO3-]/PCO2) Substitute normal blood values and multiply mm Hg PCO2 by 0.03 to convert to mEq/L PCO2: 7.4=6.1+ log(24 mEq/L/(0.03 x 40 mm Hg))= 6.1 + log 20/1 mEq = molar equivalent = amount of substance that reacts with or supplies one mole of H+ ions *As long as the ratio of bicarbonate (HCO3-) to CO2 is 20:1, pH will be 7.4 12 Acid - Base Balance - Lungs: regulate blood CO2 level by eliminating or retaining CO2 pH regulated by altering rate and depth of respiration Allows for RAPID pH response Normal CO2 level (35-45 mm Hg) Kidneys: - Long-term regulators of acid-base balance - Maintain balance by excreting or conserving blood bicarbonate (HCO3-) and hydrogen ions (H+) - SLOW pH response (hours or days to correct pH) - Normal bicarbonate level (22-26 mEq/L) 13 Acid - Base Balance CO2 + H2O ↔ H2CO3 ↔ H+ + HCO3Arterial [H+] can change for many reasons: - If the change does not involve the lungs: Metabolic acidosis – pH decreases Metabolic alkalosis – pH increases - If the lungs are the cause: Respiratory acidosis/alkalosis 14 Acid - Base Balance CO2 + H2O ↔ H2CO3 ↔ H+ + HCO3• Because the CO2-bicarbonate buffer system plays a significant role in regulating pH, the lungs can alter arterial pH by changing PCO2 • Ventilation is increased in response to metabolic acidosis (arterial↑H+ / acidemia) • Ventilation is decreased in response to metabolic alkalosis (arterial↓H+ / alkalemia) 15 Acid - Base Balance CO2 + H2O ↔ H2CO3 ↔ H+ + HCO3Inability of lungs to remove CO2 → elevated arterial PCO2 → respiratory acidemia • elevated PCO2 increases acid (H+ + HCO3-) production Inappropriate removal of CO2→ lowered arterial PCO2 → respiratory alkalemia • because lowered PCO2→ decreases acid production 16 Functions of Respiratory System • • • • • • Entry of O2 - elimination of CO2 Acid-base balance Speech Defense against microbes Circulatory filter Blood reservoir 17 Speech • air passing over larynx causes it to vibrate and produce sound. Sound is modified by tongue, lips, etc. to make speech Defense against microbes • alveolar macrophages, antibacterial peptides (epithelial) & BALT (lymphocytes, dendritic cells, macrophages….immune response) 18 Circulatory filter • filters small blood clots & destroys them • endothelial-derived tissue plasminogen activator (TPA) converts circulating plasminogen to plasmin which dissolves fibrin in clots Blood reservoir • lung blood volume (500 ml) = 10% of total blood volume • stabilizes left ventricle stroke volume when going from supine to standing 19 Overview of Respiration • • • • Ventilation (breathing) Gas exchange Transport of gases in blood Control of breathing 20 Ventilation • • • • Mechanics Pressure Changes Lung Volumes and Capacities Dead Space 21 Mechanics • Conducting zone - nose, mouth, pharynx, larynx, trachea, bronchi, bronchioles & terminal bronchioles - Warms, humidifies and filters air “muco-ciliary escalator” - No gas exchange, volume is known as anatomical dead space 22 Mechanics • Conducting zone - nose, mouth, pharynx, larynx, trachea, bronchi, bronchioles & terminal bronchioles - No gas exchange • Respiratory Zone - respiratory bronchioles, alveolar ducts and alveolar sacs - Site of gas exchange Generations (n) (0) (1-3) (4-16) (17-19) (20-22) (23) 23 Mechanics • Lungs are held against the chest wall by pleural fluid surface tension • Natural elastic forces – chest wants to expand and lung wants to contract • Opposing forces between lung and chest wall generate a subatmospheric (negative) pressure within the pleural cavity (intrapleural pressure) 24 Mechanics Inspiration (thoracic volume increases- active process) • Diaphragm, main muscle of inspiration, contracts, flattens and descends • Rib cage moves up and outwards facilitating lung expansion • External intercostal (between ribs) & neck accessory muscles are important during forced inspiration 25 Mechanics Expiration (thoracic volume decreases - passive process) • Diaphragm relaxes and becomes more rounded • Natural recoil lung, chest and abdominal structures help compress lungs • Internal intercostal & abdominal muscles important during forced expiration 26 Mechanics Respiratory or Breathing Cycle • One inspiration + one expiration constitute one breathing cycle • Average 12-15 breaths/minute 27 Pressure Changes in Ventilation • Pressure gradient is required to move air into and out of the lungs • Gases move from areas of higher to lower pressure • Behavior of gases during ventilation conform to Boyle’s Law : “volume is inversely related to pressure” 28 Boyle’s Law 29 Pressure Changes in Ventilation • Inspiration - Lung expansion increases alveolar volume, alveolar pressure falls. Now alveolar pressure is lower than the pressure at the airway opening (atmospheric) so air flows into the lungs - Air continues to flow in until pressure gradient dissipates • Expiration - Lung contraction decreases alveolar volume, alveolar pressure increases. Now alveolar pressure is greater than the pressure at the airway opening, so air flows out of the lungs - Air continues to flow out until pressure gradient dissipates 30 Pressure Changes in Ventilation • Under physiologic conditions, transpulmonary pressure (Ptp) = alveolar pressure (Palv) minus pleural pressure (Ppl). Hence, Ptp is always positive; pleural pressure is negative and large and alveolar pressure moves from slightly negative to slightly positive during breathing • When Ptp = 0 (i.e., Palv = Ppl), such as when the lungs are removed from the chest or air enters the pleural space (pneumothorax), the lungs collapse due to inherent elastic recoil (modulates Ptp) • For a given lung volume, Ptp is equal and opposite to the elastic recoil pressure of the lung 31 Pressure Changes in Ventilation Compliance • Change in lung volume/unit change in pressure across the lung • Normal is 0.2L/1cm of water • Measure of expansibility • Increased compliance (emphysema) lungs expand more • Decreased compliance (fibrosis) lungs expand less 32 Lung Volumes • Four terms describe specific lung volumes: • VT (Tidal volume) - volume inspired or expired with each breath • IRV (Inspiratory Reserve Volume) - additional volume inspired above VT • ERV (Expiratory Reserve Volume) - additional volume expired above VT • RV (Residual Volume) - volume remaining in lungs after maximal forced expiration 33 Lung Volumes → Capacities Four terms describe lung capacities: IC Inspiratory Capacity (VT + IRV) FRC Functional Residual Capacity (ERV + RV) VC Vital Capacity (IC+ERV) TLC Total lung capacity (VT + IRV + ERV + RV) 34 Lung Volumes and Capacities Volumes: IRV VT ERV RV Capacities: IC = VT + IRV = 3.5 liters FRC = ERV + RV = 2.4 liters VC = IC + ERV = 4.7 liters TLC = VT + IRV + ERV + RV = 5.9 liters 35 Lung Volumes and Capacities Changes RV/TLC ratio are early indicators of lung disease • Normal - 0.2-0.35 • Obstructive lung disease - airway obstruction (asthma, bronchitis,COPD) - >0.35 when RV increased because of increased gas trapping out of proportion to any increase in TLC • Restrictive lung disease - reduced lung volume due to parenchymal disease or disease of pleura, chest wall or neuromuscular apparatus - >0.35 because TLC decreased out of proportion to any 36 decrease in RV Dead Space - Areas not participating in gas exchange • Anatomic = conducting zone • Alveolar = alveoli receiving inadequate blood flow • Physiologic = anatomic + alveolar (i.e. alveoli not exchanging gas) 37 Dead Space • Ventilation rate Minute ventilation (VT x breaths/min) – normal value 7.5 L/min (500ml x 15bpm) Alveolar ventilation (VA) (VT - physiologic dead space) x breaths/min - (500ml – 150ml) x 15bpm = 5.25 L/min (normal) - VA is the actual amount of air available for gas exchange 38 Dead Space •Various combinations of tidal volume and breathing frequency can produce the same minute ventilation but not the same alveolar ventilation •At the extreme, if tidal volume is < dead space volume, alveolar ventilation will be zero and no gas exchange is possible. Animals take advantage of this and pant (shallow rapid breaths) to enable heat radiated by conducting airways to be removed while not altering gas composition of blood 39 Gas Exchange Gas exchange (i.e., diffusion of O2 from air into capillaries and diffusion of CO2 in opposite direction) occurs across the “respiratory membrane” Fick’s law of diffusion Gas movement across a sheet of tissue is: • directly proportional to surface area, diffusion constant and the partial pressure gradient Surface area x Diffusion constant x Partial Pressure Gradient Thickness • inversely proportional to surface thickness 40 Gas Exchange The respiratory membrane 41 Gas Exchange The lung generates a large surface area by dividing the “respiratory membrane” into many units (alveoli or alveolar sacs) 42 Gas Exchange •300 x 106 alveoli in the human lung •Each alveolus is 1/3mm in diameter •Alveolar surface area (~160 m2) – nearly the size of a tennis court •Alveolar capillaries unwound and laid end-end extend for 620 miles •The alveolar blood-gas barrier (wall) is also very, very thin (0.3-0.5 µm) 43 Gas Exchange • Occurs across “respiratory membrane” • Oxygen and carbon dioxide move between air (gas) and blood (liquid) by simple diffusion • Driving force is partial pressure difference • Dalton’s Law: “Total pressure exerted by a mixture of gases equals the sum of individual partial pressures” * • Net diffusion of gas is from higher to lower partial pressure *Dry air has 21% Oxygen. Its partial pressure (PO2) at sea level is 21/100 x 760 = 160 mm Hg. 44 Partial Pressure (Dalton’s Law) “Total pressure exerted by a mixture of gases equals the sum of the individual partial pressures” Po2 in dry air = 760 mmHg x 0.21 = 160 mmHg Po2 in humid* air = (760 mmHg - 47 mmHg) x 0.21 = 150 mmHg * Inhaled air is warmed and moistened and the water 45 vapor pressure is 47 mmHg Partial Pressure Net diffusion of a gas from area of higher partial pressure to one of lower partial pressure. 78% N2 21% O2 0.3% CO2 Alveolar gas exchange results in decreased alveolar O2 (PAO2) and increased CO2 (PACO2) 46 Gas Exchange Oxygen • Partial pressure in alveolar air (PAo2) is greater than in capillaries so O2 diffuses across respiratory membrane from alveoli to capillaries • At tissues, Pao2 is greater in capillaries than tissue so O2 diffuses from capillaries into tissue 47 Gas Exchange Carbon Dioxide • Partial pressure (PAco2) in alveolar air is lower than in capillaries so CO2 diffuses across respiratory membrane from capillaries to alveoli • At tissues, Paco2 is lower in capillaries than tissue so CO2 diffuses from tissue into capillaries 48 Factors affecting gas exchange • Rate of gas diffusion (Fick’s law) decreases if: Increase in thickness of respiratory membrane Decrease in surface area of respiratory membrane • Alveolar ventilation rate Alveolar ventilation inversely related to PAco2: Increase rate (hyperventilate) lowers PAco2, so increases partial pressure difference, facilitates exchange Decreased rate (hypoventilate) raises PAco2, so decreases partial pressure difference, inadequate exchange 49 Factors affecting gas exchange • Amount of gas dissolved in blood can be limited by pulmonary blood flow (perfusion limited) • It takes 0.75 seconds for blood to flow through a pulmonary capillary, and only 0.25 seconds for alveolar O2 to equilibrate with blood O2; for the remaining 0.5 seconds, the blood will not take on more O2 • The amount of oxygen and carbon dioxide in the blood is limited by perfusion (i.e., the only way to transfer more dissolved gas would be to add more blood (increase flow) 50 Ventilation (V)/ Perfusion (Q) Ratio • V and Q not evenly matched in normal lung (V/Q mismatch) due to gravity • Normal lung V/Q ratio is 0.8 • Regional ratios : Apex 3 Base 0.6 • Where ventilation is insufficient (low V/Q), blood not oxygenated (shunted blood) • 2.5% of cardiac output is shunted • Pathologic changes Low V/Q blood not oxygenated - more shunted blood High V/Q excess of oxygen - wasted ventilation 51 Ventilation (V)/ Perfusion (Q) Ratio 52 O2 Transport in Blood • 2% dissolved in plasma • 98% bound to iron in heme groups of hemoglobin (Hgb) - O2 carrying capacity of blood increased 65 times by binding to Hgb…..compared to O2 dissolved in plasma • 1 molecule of Hgb binds 4 molecules of O2 • O2 binding capacity (maximum amount of O2 that can be carried) = 20.1ml/100ml blood 53 O2-Hemoglobin (Hgb) Dissociation Curve Percent saturation of Hgb reflects how many O2 molecules are bound and this is dependent upon the Po2. The relationship is described by the oxygen-Hgb dissociation curve Flat part of curve (60-100 mm Hg) shows a drop in Po2 over a wide range has minimal effect on Hgb saturation Steep part of curve (<60 mm Hg) shows a large amount of O2 released with only a small change in Po2, which facilitates diffusion of O2 to the tissue 54 Factors affecting O2-Hgb Dissociation Curve Right shift: blood Pco2 leads to H+ and enhances O2 release from Hgb to tissue. Right shift is due to the pH and a direct effect of CO2 on Hgb. (Bohr effect) Left shift: Opposite of right shift. For example, as blood passes through lungs, CO2 is exhaled ( blood Pco2 , H+) and an pH, which enhances O2 binding to Hgb in the lung 55 Bohr effect (simply stated) • hemoglobin's oxygen binding affinity is inversely related both to acidity and to the concentration of carbon dioxide 56 CO2 Transport in Blood • Dissolved gas (7%) in plasma • Bound to carbamino (terminal lys or arg) protein complexes - Hgb (22%) - plasma proteins (1%) • Bicarbonate (HCO3-) formed within RBC - HCO3- released into plasma (70%) 57 CO2 Transport in Blood HALDANE EFFECT: Deoxygenation of blood increases the tendency of hemoglobin to bind carbon dioxide (and vice versa) 58 Control of Breathing • Rate and depth of breathing tightly controlled to ensure Po2 and Pco2 are appropriately maintained over conditions ranging from rest to vigorous excerise • Involuntary (usually) • Basic rhythm is set and controlled by respiratory centers in brain stem (medula and pons) which control the muscles involved in respiration 59 Control of Breathing Pneumotaxic center (upper pons) - inhibits dorsal respiratory neurons and apneustic center and this helps regulate breathing depth and rate Apneustic center (lower pons) - activates dorsal respiratory neurons of medulla Medullary respiratory center Dorsal respiratory neurons - set inspiration frequency - spontaneously active - phrenic nerve goes to diaphragm Ventral respiratory neurons - for forced expiration 60 Fine tuning: • Chemoreceptors Control of Breathing - Present in medulla, common carotid arteries, aortic arch - Sensitive to Po2, Pco2, arterial pH - Signal back to respiratory centers in medulla and pons • Mechanoreceptors - Stretch receptors present in airway smooth muscle - Hering-Breuer reflex originates outside the brain respiratory centers and prevents over-stretching of lung (action potentials transmitted through vagus nerves inhibit medulla inspiratory area and pons apneustic center; allows expiration to occur) • Irritant receptors - Present beween epithelial cells lining airways - Detect noxious chemicals, etc. (nociceptors) and cause 61 airway constriction and increase ventilation rate Control of Breathing Voluntary control: - Commands from cerebral cortex can temporarily over-ride respiratory centers so it is possible to increase rate and depth of breathing (hyperventilate) or “hold breath” (hypoventilate)……for a short time 62