* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download A case of 75-year-old survivor of unrepaired tetralogy of Fallot and
Survey
Document related concepts
Heart failure wikipedia , lookup
Coronary artery disease wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Marfan syndrome wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Pericardial heart valves wikipedia , lookup
Turner syndrome wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Artificial heart valve wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Cardiac surgery wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Aortic stenosis wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Transcript
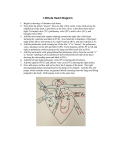
European Journal of Echocardiography (2008) 9, 167–170 doi:10.1016/j.euje.2007.06.009 A case of 75-year-old survivor of unrepaired tetralogy of Fallot and quadricuspid aortic valve Cristina Maria Stanescu† and Kyriaki Branidou*† Colentina University Hospital Bucharest, Romania Received 12 March 2007; accepted after revision 20 June 2007; online publish-ahead-of-print 24 August 2007 KEYWORDS Tetralogy of Fallot; Quadricuspid aortic valve In tetralogy of Fallot (TOF), the most common form of cyanotic congenital heart disease, only a few patients reach adulthood without surgical correction. We present the case of a man with TOF who survived until the age of 75 years without surgical intervention and had a very unusual combination of TOF and quadricuspid aortic valve (QAV). QAV, complicated by aortic regurgitation, is an uncommon finding in TOF patients. The hemodynamic consequences for both the right and left ventricles are significant. This case provides a rare insight into the late outcome of an elderly patient with uncorrected TOF. Introduction Tetralogy of Fallot (TOF), the most common cyanotic congenital heart disease, could be accompanied by right-sided aortic arch, patent ductus arteriosus (PDA) and major aortopulmonary collateral arteries, pulmonary atresia, hypoplasia or stenosis of pulmonary artery, aortic regurgitation (AR) and anomalies of the coronary arteries.1,2 The association with quadricuspid aortic valve (QAV), a rare congenital cause of AR, readily diagnosed by echocardiography, was seldom reported. We present the case of a man with TOF and QAV, who survived until the age of 75 years without surgical intervention. Case report A 75-year-old patient was admitted to our hospital with cyanosis, clubbing of the fingers and exertional dyspnea. A diagnosis of a congenital heart disease was made at birth, but diagnosis of TOF was not made until adolescence. He had a nearly asymptomatic childhood, describing dyspnea and cyanosis only at big effort, without cyanotic spells. He became symptomatic in his 50s, with progressive dyspnea on effort and cyanosis. He was first assessed in our hospital at 70 years, when he was admitted for aggravated chronic heart failure due to new onset atrial fibrillation. * Corresponding author. Maior Alexandru Campeanu nr 66, Bloc 37, sc. A, ap.12, Bucharest, Romania. Tel: þ40 722885908. E-mail address: [email protected] † C. M. Stanescu and K. Branidou contributed equally to this article and thus share first authorship. At presentation, he was alert but appeared fatigued and cachectic. He had mild kyphosis, pectus carinatum, central cyanosis and clubbing of the fingers and toes. The pulse was irregular at 77 beats per minute, and the respiratory rate was 22 breaths per minute, with increased respiratory effort. The blood pressure was 100/60 mm Hg. The oxygen saturation was 88% while the patient was breathing 2 L of oxygen with the use of a nasal cannula. The partial pressure of oxygen in arterial blood (PaO2) level was 53 mmHg and the partial pressure of carbon dioxide in arterial blood (PaCO2) level was 30 mmHg. A right ventricular (RV) impulse and systolic thrill were palpable at the left sternal border. An early systolic ejection sound was heard on the same region. The first and second heart sounds were soft. He had an ejection systolic murmur in the pulmonary area and a diastolic regurgitant murmur on the left sternal border. An electrocardiogram showed atrial fibrillation, right axis deviation, biventricular hypertrophy and incomplete right bundle branch block with QRS duration of 100 ms. The chest radiography showed a prominent RV with concavity in the main pulmonary artery area and a lifted apex, (so-called boot-shaped heart) with diminished pulmonary vascular markings. (Figure 1) An echocardiography revealed a large malaligned ventricular septal defect (VSD) of 2.2 cm, which extended from the membranous septum, beneath the tricuspid valve into the outlet septum, with about 50% ascending aorta overriding the interventricular septum. There was an infundibular obstruction with an RV outflow tract gradient of 70 mmHg, RV hypertrophy (12 mm) and dilation (50 mm) with impaired Published on behalf of the European Society of Cardiology. All rights reserved. & The Author 2007. For permissions please email: [email protected]. 168 C.M. Stanescu and K. Branidou Figure 3 Parasternal short-axis echocardiographic view, showing the four aortic cusps. Figure 1 Chest radiograph showing a prominent RV, concavity in the main pulmonary artery area and a lifted apex with diminished pulmonary vascular markings. MPA, main pulmonary artery; RV, right ventricle. Figure 4 Parasternal long-axis echocardiogram with color flow Doppler imaging, showing severe aortic regurgitation, with the regurgitant jet directed into the right ventricle. IVS, interventricular septum; RV, right ventricle; AO, ascending aorta; AR, aortic regurgitation. be discharged from the hospital one week after his admission. He refused any surgical treatment and any invasive procedure because of religious beliefs. Figure 2 Parasternal long-axis echocardiographic view, showing ascending aorta overriding the interventricular septum. LV, left ventricle; LA, left atrium; IVS, interventricular septum; RV, right ventricle; AO, ascending aorta. systolic function. (Figure 2). The right atrium was dilated (65 mm) and a moderate–severe tricuspid regurgitation was present. The ascending aorta was dilated (48 mm). The aortic valve was quadricuspid, with a cross shape in diastole, with one large, one small and two intermediate cusps, and severe AR with the regurgitant jet directed into the RV was present. (Figure 3 and 4). The left atrium was dilated (50 mm) and the left ventricle (LV) was of normal dimensions, but with mildly impaired systolic function with an estimated ejection fraction of 45%. The shunt through the VSD had a low velocity and it was bidirectional. The magnetic resonance imaging (MRI) revealed significant RV outflow stenosis with a diameter of 0.6 cm, dilated ascending aorta and confirmed the presence of severe AR with the jet directed toward the RV. The patient was treated with furosemide, digoxin, spironolactone, and acenocoumarol and he was well enough to Discussion The adult patients with uncorrected TOF have nowadays become a rarity, with only a few patients with TOF surviving into adulthood without operation. In the literature, several conditions are related to longevity in these patients: hypoplastic pulmonary artery with moderately slow development of subpulmonary obstruction,3,4 LV hypertrophy5,6 and extracardiac shunts, including PDA4,7 or systemic to pulmonary artery shunting via internal mammaries.8 The patient under discussion had a relatively mild stenosis of the RV outflow tract, with a predominantly left to right shunt through the VSD at rest, explaining why cyanosis in his childhood appeared only during effort. The echocardiography and the MRI examination failed to demonstrate the presence of PDA. The presence of collaterals, initially suspected because of the increased amplitude R wave in left precordial derivations,9 was not demonstrated at MRI. AR was reported in several series in 2–6 % of TOF patients.2,10 Prolapse of the right coronary cusp was the main cause of AR in one of the studies.2 This mechanism is less often encountered in TOF than in high isolated VSD, A 75-year old survivor of unrepaired TOF and QAV due to different hemodynamics; in high VSD, the left to right shunt may damage the aortic cusps, whilst in TOF the output of both ventricles is ejected directly into the aorta, with no alteration of aortic valve function.10 Other reported causes of AR were a deformed aortic valve secondary to endocarditis and severe dilation of the aortic annulus.2 Aortic root dilation was frequently reported in TOF, especially in patients with pulmonary atresia and was attributed to increased blood flow from both ventricles to the overriding aorta.11 More recently, intrinsic histological abnormalities of the ascending aorta are thought to contribute to progressive aortic root dilation and AR.12 Additionally, malformations of the aortic valve can also lead to AR, but their association with TOF is rarely encountered. A few cases of bicuspid aortic valve in TOF patients were reported.10,13 Our case is a very unusual combination of TOF and quadricuspid aortic valve QAV. QAV is a rare congenital malformation often associated with other cardiac disorders, such as PDA, VSD, pulmonary stenosis, mitral valve malformation, hypertrophic cardiomyopathy, coronary abnormalities and congenital complete heart block.14,15 In a review performed in 2004, a total of 186 published cases of QAV were found.16 To the best of our knowledge, there are, so far, only two reported cases of QAV associated with TOF.17,18 Quadricuspid semilunar valves have been classified by Hurwitz and Roberts into seven types, according to the relative size of the four cusps.19 It was shown that the QAV is often incompetent; normally functioning valves have been found in only 16 % of cases.16 The findings reported in the literature suggest that fibrous thickening of valves, due to the unequal mechanical stress distribution on the valve, may lead to progressive AR.20,21 QAV can be easily diagnosed by two-dimensional echocardiography, because of the typical aspect of the four cusps in both diastole and systole. Our patient has a type four QAV, according to Hurwitz’s classification, represented by one large, one small and two intermediate cusps, leading, owing to their unequal size, to severe AR. The incompetent aortic valve constituted a hemodynamic burden for the RV, contributing to its dilation due to longstanding volume overload, as the regurgitant jet was directed into the RV through the nonrestrictive VSD. Substantial tricuspid regurgitation occurred because of RV dilation, leading to further dilation of the right chambers. AR, if acute, may have devastating effects on a compromised RV, from longstanding pressure overload, resulting in acute heart failure.22 In this particular patient, the AR caused by congenital QAV was well tolerated, as the RV had time to compensate for the chronic volume load in a context of mildly infundibular stenosis that did not markedly increase the afterload. Additionally, there is a strong possibility that the presence of chronic AR was somehow beneficial, raising the proportion of oxygenated blood in the RV. As a consequence, the right to left shunt provided the LV with partly oxygenated blood, resulting in a lower than expected degree of arterial hypoxemia and cyanosis. It has been demonstrated that hypoxemia per se may contribute to the worsening of heart failure. Low systemic oxygen saturation, increased coronary vascular resistance and increased blood viscosity secondary to polycythemia, have been considered as contributing factors to abnormal LV function, by means of repeated episodes of myocardial hypoxia and subsequent fibrosis.23 169 In our patient, the presumptive lower degree of hypoxemia contributed to the delayed occurrence of myocardial dysfunction, that appeared late in his 50s and it was worsened subsequently by the atrial fibrillation and probably by coronary artery disease. Conclusion In this particular case there are multivariable factors that affected the patient’s hemodynamics and therefore contributed to our patient’s prolonged survival; pulmonary blood flow was neither severely decreased, as the RV outflow tract obstruction was only moderate, nor raised enough to significantly increase pulmonary vascular resistance, in spite of the RV volume overload caused by the AR. Such a fine hemodynamic balance is clearly rare. Additionally, the raised proportion of oxygenated blood in the RV, due to the AR, had contributed to reducing cyanosis and hypoxic damage to the myocardium, which enabled prolonged survival. References 1. Shinebourne EA, Anderson RH. Fallot’s tetralogy: in Anderson RH, Baker EJ, Mac Courtney FJ et al. editors. Pediatric cardiology. 2nd ed. London: Churchill Livingstone 2002;1213–50. 2. Abraham KA, Cherian G, Rao VD, Sukumar IP, Krishnaswami S, John S. Tetralogy of Fallot in adults. A report on 147 patients. Am J Med 1979; 66: 811–6. 3. Meindok H. Longevity in the tetralogy of Fallot. Thorax 1964;19:12–5. 4. Thomas SHL, Bass P, Pambakian H, Marigold JH. Cyanotic tetralogy of Fallot in a 77 year old man. Postgrad Med J 1987;63:361–2. 5. Bowie EA. Longevity in tetralogy and triology of Fallot. Discussion of cases in patients surviving 40 years and presentation of two further cases. Am Heart J 1961;62:125–32. 6. Chin J, Bashour T, Kabbani S. Tetralogy of Fallot in the elderly. Clin Cardiol 1984;7:453–6. 7. Nottestad SY, Slife DM, Rubal BJ, Moody JM. Tetralogy of Fallot in a 71 year old patient with new onset hypoxemia. Cathet Cardiovasc Diagn 1993;28:335–8. 8. Liberthson RR, Miller SW, Drew F, Drew F, Palacios I, Singh J, Drew F. Congenital extracardiac shunts with tetralogy of Fallot. Cardiovasc Intervent Radiol 1981;4:131–5. 9. Reeta V, Deepak K. A review of electrocardiographic features in tetralogy of Fallot in Indian patients. Ind H Jour 2005;57:289–301. 10. Vernant P, Casasoprana A, Magnier S. Tetralogy of Fallot and aortic insufficiency. Arch Mal Coeur Vaiss 1981;74:609–14. 11. Marelli AJ, Perloff JK, Child JS, Laks H. Pulmonary atresia with ventricular septal defect in adults. Circulation 1994;89:243–51. 12. Tan JL, Davlouros PA, McCarthy KP et al. Intrinsic histological abnormalities of aortic root and ascending aorta in tetralogy of Fallot. Circulation 2005;112:961–8. 13. Ermis K, Gupta-Malhotra M, Titus JL. An obstructive bicuspid aortic valve in the setting of tetralogy of Fallot with pulmonary atresia: a rare combination. Cardiol Young 2004;14:99–101. 14. Brouwer MH, De Graaf JJ, Ebels T. Congenital quadricuspid aortic valve. Int J Cardiol 1993;38:196–8. 15. Moreno R, Zamorano J, De Marco E et al. Congenital qudricuspid aortic valve associated with congenital complete heart block. Eur J Echocardiography 2002;3:236–7. 16. Tutarel O. The quadriscuspid aortic valve: a comprehensive review. J Heart Valve Dis 2004;13:534–7. 17. Suzuki Y, Daitoku K, Minakawa M, Fukui K, Fukuda I. Congenital quadricuspid aortic valve with tetralogy of Fallot and pulmonary atresia. Jpn J Thorac Cardiovasc Surg 2006;54:44. 18. Sokol I, Vincelj J, Kirin M. Echocardiographic features of adult tetralogy of Fallot with natural palliative correction by patent ductus arteriosus. Croat Med J 2003;44:234–8. 19. Hurwitz LE, Roberts WC. Quadricuspid semilunar valve. Am J Cardiol 1973;31:623–6. 170 20. Feldman BJ, Khandheria BK, Warres CA, Seward JB, Taylor CL, Tajik AJ. Incidence, description and functional assessment of isolated quadricuspid aortic valves. Am J Cardiol 1990;65:937–8. 21. Bortolotti U, Scioti G, Levantino M, Milano A, Nardi C, Tartarini G. Aortic valve replacement for quadricuspid aortic valve incompetence. J Heart Valve Dis 1998;7:515–7. C.M. Stanescu and K. Branidou 22. Knobloch K, Lichtenberg A, Haverich A. Untreated tetralogy of Fallot in an adult patient complicated by acute aortic valve endocarditis. Interact Cardiovasc Thorac Surg 2004;3:326–7. 23. Chowdhury Ujjwal K, Ganapathy Subramaniam K, Kothari Shyam S, Airan B, Venugopal P. Congestive heart failure in unoperated tetralogy of Fallot: can hypoxia be a cause? Indian Heart J 2005;57:65–67.