* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download cardiac cycle - The department of cardiology, Calicut medical college
Management of acute coronary syndrome wikipedia , lookup
Coronary artery disease wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Heart failure wikipedia , lookup
Cardiac surgery wikipedia , lookup
Myocardial infarction wikipedia , lookup
Aortic stenosis wikipedia , lookup
Artificial heart valve wikipedia , lookup
Electrocardiography wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Atrial septal defect wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Atrial fibrillation wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
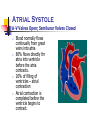
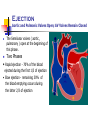
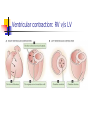
CARDIAC CYCLE DR RAKESH JAIN SR Cardiology Govt. Medical College, Calicut. Cardiac Cycle Def: The cardiac events that occur from beginning of one heart beat to the beginning of the next. first assembled by Lewis in 1920 but first conceived by Wiggers in 1915 Atria act as PRIMER PUMPS for ventricles & ventricles provide major source of power for moving the blood through the vascular system. Initiated by spontaneous generation of AP in SA node (located in the superior lateral wall of the right atrium near the opening of the superior vena cava) Electrical System: Brief Action potentials originating in the sinus node travel to AV node (1m/s) in 0.03 sec. 1. AV nodal delay of 0.09 sec before the impulse enters the penetrating portion of the A-V bundle 2. A final delay of another 0.04 sec occurs mainly in this penetrating A-V bundle total delay in the A-V nodal and A-V bundle system is about 0.13 sec A total delay of 0.16 sec occurs before the excitatory signal finally reaches the contracting muscle of the ventricles from its origin in sinus node. Delay in AV node (0.13sec) Why delay? Diminished numbers of gap junctions Between successive cells in the conducting pathways. Significance? Delay allows time for the atria to empty their blood into the ventricles before ventricular contraction begins Rapid Transmission in the Purkinje System (1.5 to 4.0 m/sec) i.e. • About 6x that in ventricular muscle • About 150x that in A-V nodal fibers allowing almost instantaneous transmission of the cardiac impulse throughout the ventricular muscle (B/c of very high level of permeability of the gap junctions) Summary of Cardiac Impulse Transmission Mechanical Phase Cardiac cycle – basically describes… 1. 2. 3. Pressure Volume, and Flow phenomenon in ventricles as a function of time Basics 1 Beat = 0.8 sec (800 msec) Systole = 0.3 sec Diastole = 0.5 sec In tachycardia, Diastolic phase decreases more than systolic phase Phases of cardiac cycle LV Contraction Isovolumic contraction (b) Maximal ejection (c) LV Relaxation Start of relaxation and reduced ejection (d) Isovolumic relaxation (e) LV Filling Rapid phase (f) Slow filling (diastasis) (g) Atrial systole or booster (a) Time Intervals Total ventricular systole 0.3 sec Isovolumic contraction (b) 0.05 sec (0.015sec for RV) Maximal ejection (c) 0.1 sec Reduced ejection (d) 0.15 sec Total ventricular diastole 0.5 sec Isovolumic relaxation (e) 0.1 sec Rapid filling phase (f) 0.1 sec Slow filling (diastasis) (g) 0.2 sec Atrial systole or booster (a) 0.1 sec GRAND TOTAL (Syst+Diast) = 0.8 sec Physiologic Versus Cardiologic Systole and Diastole PHYSIOLOGIC SYSTOLE Isovolumic contraction Maximal ejection PHYSIOLOGIC DIASTOLE Reduced ejection Isovolumic relaxation Filling phases CARDIOLOGIC SYSTOLE From M1 to A2, including: Major part of isovolumic contraction Maximal ejection Reduced ejection CARDIOLOGIC DIASTOLE 20msec A2-M1 interval (filling phases included) Physiological systole cardiologic systole, demarcated by heart sounds rather than by physiologic events, starts fractionally later than physiologic systole and ends significantly later. Cardiologic systole> physiologic systole Description of Cardiac cycle phases 1. 2. 3. 4. Pressure & Volume events ECG correlation Heart sounds Clinical significance Atrial Systole A-V Valves Open; Semilunar Valves Closed Blood normally flows continually from great veins into atria 80% flows directly thr atria into ventricle before the atria contracts. 20% of filling of ventricles – atrial contraction Atrial contraction is completed before the ventricle begins to contract. Atrial contraction normally accounts for about 10%-15% of LV filling at rest, however, At higher heart rates, atrial contraction may account for up to 40% of LV filling referred to as the "atrial kick” The atrial contribution to ventricular filling varies inversely with duration of ventricular diastole and directly with atrial contractility Atrial Systole Pressures & Volumes ‘ a ‘ wave – atrial contraction, when atrial pressure rises. Atrial pressure drops when the atria stop contracting. After atrial contraction is complete LVEDV typically about 120 ml (preload) End-diastolic pressures of LV = 8-12 mmHg and RV = 3-6 mmHg AV valves floats upward (pre-position) Abnormalities of “a” wave Elevated a wave Tricuspid stenosis Decreased ventricular compliance (ventricular failure, pulmonic valve stenosis, or pulmonary hypertension) Cannon a wave Atrial-ventricular asynchrony (atria contract against a closed tricuspid valve) complete heart block, following premature ventricular contraction, during ventricular tachycardia, with ventricular pacemaker Absent a wave Atrial fibrillation or atrial standstill Atrial flutter Why blood does not flow back in to SVC/PV while atria contracting, even though no valve in between? Wave of contraction through the atria moves toward the AV valve thereby having a "milking effect." Inertial effects of the venous return. Atrial Systole ECG p wave – atrial depolarization impulse from SA node results in depolarization & contraction of atria ( Rt before Lt ) PR segment – isoelectric line as depolarization proceeds to AV node. This brief pause before contraction allows the ventricles to fill completely with blood. Atrial Systole Heart Sounds S4 (atrial or presystolic gallop) - atrial emptying after forcible atrial contraction. appears at 0.04 s after the P wave (late diastolic) lasts 0.04-0.10 s Caused by vibration of ventricular wall during rapid atrium emptying into non compliant ventricle Causes of S4 Physiological; >60yrs (Recordable, not audible) Pathological; All causes of concentric LV/RV hypertrophy Coronary artery disease Acute regurgitant lesions An easily audible S4 at any age is generally abnormal. Clinical Facts about S4 In contrast to S3, which may mean ventricular failure, the presence of S4 does not indicates heart failure. It only signify “hardworking ventricle”. The presence of S4 correlate with a gradient of at least 50mmHg across LVOT in suspected LVOT obstruction. (This correlation is not applicable in HCM) In setting of MI, an audible S4 indicates that at least 10% of myocardium is at jeopardy. In presence of Shock, S4 indicates that hypovolemia is unlikely as PCWP will be >18mmHg. S4 can be heard when RVEDP >12mmHg on Rt or LVEDP > 15mmHg on Lt side. If EDP is very high i.e. >25 mmHg, S4 may be absent b/c of insufficient atrial functions. JVP: x descent Prominent x descent 1 2 3 Cardiac tamponade Constrictive pericarditis Right ventricular ischemia with preservation of atrial contractility Blunted x descent 1 2 Atrial fibrillation Right atrial ischemia Beginning of Ven.Systole Isovolumetric Contraction All Valves Closed Isovolumetric Contraction Pressure & Volume Changes The AV valves close when the pressure in the ventricles (red) exceeds the pressure in the atria (yellow). As the ventricles contract isovolumetrically -- their volume does not change (white) -- the pressure inside increases, approaching the pressure in the aorta and pulmonary arteries (green). JVP: c wave- d/t Right ventricular contraction pushes the tricuspid valve into the atrium and increases atrial pressure, creating a small wave into the jugular vein. It is normally simultaneous with the carotid pulse. Ventricular chamber geometry changes considerably as the heart becomes more spheroid in shape; circumference increases and atrial base-to-apex length decreases. Early in this phase, the rate of pressure development becomes maximal. This is referred to as maximal dP/dt. Ventricular pressure increases rapidly LV ~10mmHg to ~ 80mmHg (~Aortic pressure) RV ~4 mmHg to ~15mmHg (~Pulmonary A pressure) At this point, semilunar (aortic and pulmonary) valves open against the pressures in the aorta and pulmonary artery LV Torsion left-handed helix in subepicardium right-handed helix in subendocardium Figure: Schematic Drawing of LV Torsion The image on the left shows the myofiber directions. Solid lines epicardial region; dashed lines endocardial region. The image on the right shows untwisting. ED end-diastole; ES end-systole; LV left ventricle. (J Am Coll Cardiol Img 2009;2:648–55) Isovolumetric Contraction ECG The QRS complex is due to ventricular depolarization, and it marks the beginning of ventricular systole. Isovolumetric Contraction Heart Sounds S1 is d/t closure and after vibrations of AV Valves. (M1 occurs with a definite albeit 20 msec delay after the LV-LA pressure crossover.) S1 is normally split (~0.04 sec) because mitral valve closure precedes tricuspid closure. (Heard in only 40% of normal individuals) S1 heart sound low pitch and relatively long-lasting lasts ~ 0.12-0.15 sec frequency ~ 30-100 Hz appears 0.02 – 0.04 sec after the beginning of the QRS complex Some Clinical facts about S1 S1 is a relatively prolonged, low frequency sound, best heard at apex. Normally split of S1 (~40%)is heard only at tricuspid area.(As tricuspid component is heard only here.) If S1 is equal to or higher in intensity than S2 at base, S1 is considered accentuated. Variable intensity of S1 and jugular venous pulse are highly specific and sensitive in the diagnosis of ventriculoatrial dissociation during VT, and is helpful in distinguishing it from supraventricular tachycardia with aberration. Value of physical signs in the diagnosis of ventricular tachycardia. C J Garratt, M J Griffith, G Young, N Curzen, S Brecker, A F Rickards and A J Camm, Circulation. 1994;90:3103-3107 Causes of Loud S1 1. 2. 3. 4. 5. 6. 7. Exercise Emotinal excitibility Mitral stenosis Hyperkinetic circulation Atrial septal defect Sinus tachycardia Short P-R interval Soft S1 1. 2. 3. 4. 5. 6. 7. 8. 9. Sinus tachycardia Mitral regurgitation Severe AR Ventricular aneurysm Acute MI Myocarditis Cardiomyopathy Prolonged P-R interval Calcific MS Ejection Aortic and Pulmonic Valves Open; AV Valves Remain Closed The Semilunar valves ( aortic , pulmonary ) open at the beginning of this phase. Two Phases • Rapid ejection - 70% of the blood ejected during the first 1/3 of ejection • Slow ejection - remaining 30% of the blood emptying occurs during the latter 2/3 of ejection Rapid Ejection Pressure & Volume Changes When ventricles continue to contract , pressure in ventricles exceed that of in aorta & pul arteries & then semilunar valves open, blood is pumped out of ventricles & Ventricular vol decreases rapidly. Ventricular contraction: RV v/s LV Rapid Ejection ECG & Heart Sounds In rapid ejection part of the ejection phase there no specific ECG changes / heart sounds heard. Slow Ejection Aortic and Pulmonic Valves Open; AV Valves Remain Closed Blood flow from the left ventricle to the aorta rapidly diminishes but is maintained by aortic recoil, the “Windkessel effect “ At the end of ejection, the semilunar valves close. This marks the end of ventricular systole mechanically. Slow Ejection ECG & Heart Sounds T wave – slightly before the end of ventricular contraction it is d/t ventricular repolarization heart sounds : none Beginning of Diastole Isovolumetric relaxation All Valves Closed At the end of systole, ventricular relaxation begins, allowing intraventricular pressures to decrease rapidly (LV from 100mmHg to 20mmHg & RV from 15mmHg to 0mmHg), aortic and pulmonic valves abruptly close (aortic precedes pulmonic) causing the second heart sound (S2) Valve closure is associated with a small backflow of blood into the ventricles and a characteristic notch (incisura or dicrotic notch) in the aortic and pulmonary artery pressure tracings After valve closure, the aortic and pulmonary artery pressures rise slightly (dicrotic wave) following by a slow decline in pressure Isovolumetric relaxation Volumes remain constant because all valves are closed volume of blood that remains in a ventricle is called the end-systolic volume (LV ~50ml). pressure & volume of ventricle are low in this phase . Isovolumetric relaxation Throughout this and the previous two phases, the atrium in diastole has been filling with blood on top of the closed AV valve, causing atrial pressure to rise gradually JVP - "v" wave occurs toward end of ventricular contraction – results from slow flow of blood into atria from veins while AV valves are closed . Isovolumetric relaxation ECG & Heart Sounds ECG : no deflections Heart Sounds : S2 is heard when the semilunar vlaves close. A2 is heard prior to P2 as Aortic valve closes prior to pulmonary valve. Why A2 occurs prior to P2 ? “Hangout interval” is longer for pulmonary side (~80msec),compared to aortic side (~30msec). Hangout interval is the time interval from crossover of pressures (ventricle with their respective vessel) to the actual occurrence of sound. Due to lower pressure and higher distensibility, pulmonary artery having longer hangout interval causing delayed PV closure and P2. S2 heart sound Appears in the terminal period of the T wave lasts 0.08 – 0.12s Some clinical facts about S2 Normal split: Two components heard during inspiration and is single sound during expiration. (A2-P2 ~20- 50 msec in inspiration) Clinically split is defined as wide, if it is heard well in standing position, in expiration (normally not heard as the split is 15 msec, which can not be heard by human ears) Single S2: absence of audible split in either phase of respiration. Fixed split: two components fails to move with respiration. Reverse split: Inaudible split during inspiration and audible split during expiration. (recognized by wider split in expiration) Common causes of wide split S2 RBBB Sev PAH ASD Idiopathic dilatation of pul artery Sev right heart failure Moderate to severe PS Severe MR Normal variant Common causes of wide fixed split S2 ASD All causes of wide split with associated severe right ventricular failure. Common causes of single S2 Truncus arteriosus Pulmonary atresia Aortic atresia TGA AS, PS Single loud P2 in extreme PAH Causes of reverse split S2 LBBB RV pacing RV ectopy Severe AS Acute MI WPW type B Severe TR Aneurysm of ascending aorta Severe systemic hypertension JVP: V wave Elevated v wave 1 2 3 Tricuspid regurgitation Right ventricular heart failure Reduced atrial compliance (restrictive myopathy) a wave equal to v wave 1 2 3 Tamponade Constrictive pericardial disease Hypervolemia Rapid Inflow ( Rapid Ven. Filling) A-V Valves Open Once AV valves are open the blood that has accumulated in atria flows into the ventricle. Rapid Inflow Volume changes Despite the inflow of blood from the atria, intraventricular pressure continues to briefly fall because the ventricles are still undergoing relaxation JVP: Seen as y-descent. Rapid Inflow ( Rapid Ven. Filling) ECG & Heart Sounds ECG : no deflections Heart sounds : S3 is heard, lasts 0.02-0.04 sec (represent tensing of chordae tendineae and AV ring during ventricular relaxation and filling) Whatever the mechanism, a sudden inherent limitation in the long axis filling movement of the LV is consistently observed. Clinical facts about S3 In presence of HF, S3 correlates well with ventricular end diastolic pressure and is usually >25mmHg on left side. Right sided S3 correlate well with rapid y descend in neck veins. Normal A2-S3 interval is between 120-160 msec. Correlates of S3 Anatomical Dilated ventricle Functional Systolic dysfunction (EF<40%) Hemodynamics LVEDP Cardiac index Symptoms Doppler flow across AV valve >25 mmHg <2 L/min/m2 Dyspnea, PND, Orthopnea Tall E wave compare to A wave Gallop rhythm A gallop rhythm is a grouping of three heart sounds that together sound like hoofs of a galloping horse. Protodiastolic gallop or ventricular gallop or S3 gallop addition of an S3 to the physiological S1 and S2 creates a three-sound sequence, S1-S2-S3. Presystolic gallop rhythm or atrial gallop addition of an S4 to the physiological S1 and S2 creates a three-sound sequence, S4-S1-S2. (during tachycardia S4-S1 can fuse, producing a summation gallop ) Causes of S3 Physiological: Childrens & young adults <40 yrs (nearly 25%) (Not heard in normal infants & adult >40 yrs.) Pathological: Ventricular failure Hyperkinetic state (anemia, thyrotoxicosis, beri-beri) MR, TR AR, PR Systemic AV fistula JVP: y descent Prominent y descent 1 2 3 Constrictive pericarditis Restrictive myopathies Tricuspid regurgitation Blunted y descent 1 2 3 Tamponade Right ventricular ischemia Tricuspid stenosis Diastasis A-V Valves Open remaining blood which has accumulated in atria slowly flows into the ventricle. Diastasis Volume changes Ventricular volume increases more slowly now. The ventricles continue to fill with blood until they are nearly full. Diastasis ECG & Heart Sounds ECG : no deflections Heart Sounds : none The Lewis or wiggers cycle, Guyton & Hall. Textbook of Medical Physiology, 11th Edition Volumes End diastolic vol : During diastole, filling of ventricle increases vol of each ventricle to ~ 110 -120 ml Stroke Vol : amount of blood pumped out of ventricle during systole. ~ 70 ml End systolic vol : the remaining amount of blood in ventricle after the systole. ~40 -50 ml Pressure-Volume Loop Pressure-volume loop of RV is same as that of LV, however the area is only 1/5th of LV because pressures are so much lower on right RV v/s LV Rt • • • Ventricular Pressure wave 1/5th dp/dt is less Isovolumic contraction & relaxation phases are short. Timing of Cardiac EVENTS 1. RA start contracting before LA 2. LV start contracting before RV 3. TV open before MV, so RV filling start before LV. 4. RV peak pressure 1/5th of LV. 5. RV outflow velocity smooth rise & fall, while Lt side initial peak followed by quick fall. The First cardiac catheterization Cardiac catheterization was first attempted by Dr Werner Forssmann in 1929, at the age of 25 yrs only, when he was a resident in a hospital at Eberswalde, near Berlin. He was his own subject. A fellow resident who agreed to pass the catheter, got scared and abandoned the effort by the time the catheter reached the axilla. Forssmann completed the task himself with radiographer holding the mirror infront of screen. Forssmann catheterize his heart safely nine times till he had no more peripheral veins left to try. But this was not enough to convince the medical world about the safety of the procedure. After being banished from academics, frustrated Forssmann settled for medical practice in a small town. It was extensive studies with catheterization by Dr Andre Cournand & Dr Dickinson Richard Jr. and eventually the novel prize for physiology & medicine was awarded jointly to Forssmann, Cournand & Richard in 1956. The history of cardiac catheterization illustrates what reckless idealism of youth can achieve and the long time (here 27 yrs) might take the world to realize the value of even something of great significance. References 1. 2. 3. 4. 5. 6. Guyton and Hall Textbook of Medical Physiology, 11th Ed. Arthur C. Guyton, John E. Hall. Cardiovascular Physiology Concepts Second Edition, Lippincott Williams & Wilkins, 2011 Clinical Methods in Cardiology By Soma Raju, Second Edition, orient longman Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine, ninth edition Harrison's Principles of Internal Medicine, 19th edition, McGraw-Hill Book Co Understanding Medical Physiology: A Textbook for Medical Students: By R.L. Bijlani, M.D., RL Bijlani MD SM DSc (Hon Causa) FAMS, S. Manjunatha,4th edition 7. Medical Physiology E-Book: By Walter F. Boron, Emile L.Boulpaep, Second Edition 8. Value of physical signs in the diagnosis of ventricular tachycardia. C J Garratt, M J Griffith, G Young, N Curzen, S Brecker, A F Rickards and A J Camm, Circulation. 1994;90:3103-3107 9. Color Atlas of Physiology. Stefan Silbernagel, Agamemnon Despopoulos. 6th Edition. 10. Jacc: cardiovascular imaging, Vol.2 No. 5, 2009. May 2009: 648-55. QUIZ 1. Which letter indicates the point in the cardiac cycle that the mitral valve opens? A. A B. B C. C D. D 2. In a normal cardiac cycle , true is A. RA ejection precedes LA ejection B. RV contraction starts before LV contraction C. LV ejection starts before RV ejection D. Pulmonary valve closes before aortic valve 3. Which letter in the image represents the isovolumic 2.contraction of the left ventricle in the heart? A. F B. B C. H D. D 4. Which of the following pairs is INCORRECT? A. P wave: atrial depolarization B. QRS complex: ventricular depolarization C. T wave: ventricular repolarization D. QT interval: Measure of duration of atrial action potential 5. Isovolumic contraction phase correspond to A. AV opening to AV Closure B. MV closure to MV opening C. MV closure to AV opening D. AV opening to MV opening 6. Left ventricular end-diastolic volume is: A. 30-50 mls B. 50-70 mls C. 70-120 mls D. 120-150 mls 7. Prominent y descent in JVP seen in all except A. Constrictive pericarditis B. Restrictive cardiomyopathies C. Tricuspid regurgitation D. Cardiac temponade 8. All are true about S3 except A. Right sided S3 correlate well with rapid y descend in neck veins. B. S3 normally heard in normal infants C. S3 usually indicates systolic dysfunction D. S3 correlates well with ventricular end diastolic pressure usually >25mmHg on left side 9. Cardiac apex is palpable during which phase of cardiac cycle A. Isovolumic contraction phase B. Isovolumic relaxation phase C. Rapid ejection phase D. Atrial systole phase 10. Sensitive & specific sign of ventricularterial dissociation in VT are A. Variable intensity of S1 B. Variable jugular venous pulse C. Both A & B D. None of the above Answers 1. Which letter indicates the point in the cardiac cycle that the mitral valve opens? A. A B. B C. C D. D 2. In a normal cardiac cycle , true is A. RA ejection precedes LA ejection B. RV contraction starts before LV contraction C. LV ejection starts before RV ejection D. Pulmonary valve closes before aortic valve 3. Which letter in the image represents the isovolumic 2.contraction of the left ventricle in the heart? A. F B. B C. H D. D 4. Which of the following pairs is INCORRECT? A. P wave: atrial depolarization B. QRS complex: ventricular depolarization C. T wave: ventricular repolarization D. QT interval: Measure of duration of atrial action potential 5. Isovolumic contraction phase correspond to A. AV opening to AV Closure B. MV closure to MV opening C. MV closure to AV opening D. AV opening to MV opening 6. Left ventricular end-diastolic volume is: A. 30-50 mls B. 50-70 mls C. 70-120 mls D. 120-150 mls 7. Prominent y descent in JVP seen in all except A. Constrictive pericarditis B. Restrictive cardiomyopathies C. Tricuspid regurgitation D. Cardiac temponade 8. All are true about S3 except A. Right sided S3 correlate well with rapid y descend in neck veins. B. S3 normally heard in normal infants C. S3 usually indicates systolic dysfunction D. S3 correlates well with ventricular end diastolic pressure usually >25mmHg on left side 9. Cardiac apex is palpable during which phase of cardiac cycle A. Isovolumic contraction phase B. Isovolumic relaxation phase C. Rapid ejection phase D. Atrial systole phase 10. Sensitive & specific sign of ventricularterial dissociation in VT are A. Variable intensity of S1 B. Variable jugular venous pulse C. Both A & B D. None of the above THANK YOU