* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Cardiovascular Physiology
Survey
Document related concepts
Management of acute coronary syndrome wikipedia , lookup
Heart failure wikipedia , lookup
Coronary artery disease wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Electrocardiography wikipedia , lookup
Artificial heart valve wikipedia , lookup
Jatene procedure wikipedia , lookup
Cardiac surgery wikipedia , lookup
Myocardial infarction wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Transcript
Cardiovascular
Physiology
Dr. Khalid Alregaiey
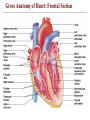
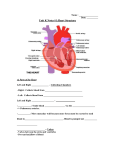
Gross Anatomy of Heart: Frontal Section
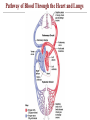
Pathway of Blood Through the Heart and Lungs
• Right atrium tricuspid valve right ventricle
• Right ventricle pulmonary semilunar valve
pulmonary arteries lungs
• Lungs pulmonary veins left atrium
• Left atrium bicuspid valve left ventricle
• Left ventricle aortic semilunar valve aorta
• Aorta systemic circulation
Pathway of Blood Through the Heart and Lungs
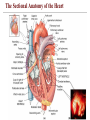
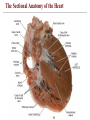
The Sectional Anatomy of the Heart
The Sectional Anatomy of the Heart
Heart chambers and valves
• Structural Differences in heart chambers
• The left side of the heart is more muscular than
the right side
• Functions of valves
• AV valves prevent backflow of blood from the
ventricles to the atria
• Semilunar valves prevent backflow into the
ventricles from the pulmonary trunk and aorta
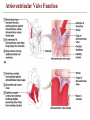
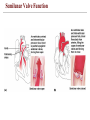
Atrioventricular Valve Function
Semilunar Valve Function
Cardiac Physiology
• Two classes of cardiac muscle cells
• Specialized muscle cells of the conducting
system
• Contractile cells
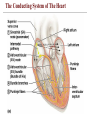
The Conducting System of The Heart
• The conducting system includes:
• Sinoatrial (SA) node (pacemaker)
• Atrioventricular (AV) node
• atrioventricular bundle (bundle of His)
• Purkinje fibers
The Conducting System of The Heart
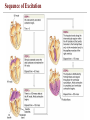
Impulse Conduction through the heart
• SA node generates impulses about 75
times/minute (pacemaker)
• Stimulus spreads to the AV node
• Impulse is delayed at AV node
• Impulse passes from atria to ventricles via
the atrioventricular bundle (bundle of His)
• Then distributed by Purkinje fibers
Sequence of Excitation
The electrocardiogram (ECG)
• A recording of the electrical events occurring
during the cardiac cycle
• The P wave corresponds to the
depolarization of SA node
• The QRS complex corresponds to
ventricular depolarization
• The T wave corresponds to ventricular
repolarization
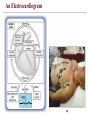
An Electrocardiogram
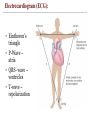
Electrocardiogram (ECG):
• Einthoven's
triangle
• P-Wave –
atria
• QRS- wave –
ventricles
• T-wave –
repolarization
An Electrocardiogram
ECG Information Gained
• (Non-invasive)
• Heart Rate
• Signal conduction
• Heart tissue
• Conditions
Figure 14-24: Normal and abnormal electrocardiograms
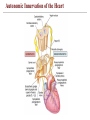
Autonomic Innervation of the Heart
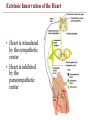
Extrinsic Innervation of the Heart
• Heart is stimulated
by the sympathetic
center
• Heart is inhibited
by the
parasympathetic
center
Sympathetic and Parasympathetic
• Sympathetic – speeds heart rate by Ca++ & I-f
channel flow
• Parasympathetic – slows rate by K+ efflux &
Ca++ influx
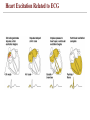
Heart Excitation Related to ECG
Heart Sounds
• Auscultation – listening to heart sound via
stethoscope
• Four heart sounds
• S1 – “lubb” caused by the closing of the AV
valves
• S2 – “dupp” caused by the closing of the
semilunar valves
• S3 – a faint sound associated with blood
flowing into the ventricles
• S4 – another faint sound associated with atrial
contraction
Cardiac Cycle
• Cardiac cycle refers to all events
associated with blood flow through the
heart
• Systole – contraction of heart muscle
• Diastole – relaxation of heart muscle
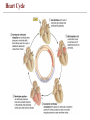
Heart Cycle:
1. Late diastole: all chambers relax, filling
with blood
2. Atrial systole: atria contract, add 20%
more blood to ventricles
3. Isovolumic ventricular contraction:
closes AV valves ("lub"), builds pressure
Heart Cycle: Finish and Around To the Start
4. Ventricular ejection: pushes open semi
lunar valves, blood forced out
5. Ventricular relaxation: Backflow of blood
in aorta and pulmonary trunk closes
semilunar valves ("dup")
AV valves open refilling starts – back to
start of cycle
Heart Cycle
Phases of the Cardiac Cycle
Cardiac Output (CO) and Reserve
• CO is the amount of blood pumped by
each ventricle in one minute
• CO = heart rate (HR) X stroke
volume (SV)
• HR is the number of heart beats per
minute
• SV is the amount of blood pumped out by
a ventricle with each beat
• Cardiac reserve is the difference between
resting and maximal CO
Cardiac Output: Example
• CO (ml/min) = HR (75 beats/min) x SV (70
ml/beat)
• CO = 5250 ml/min (5.25 L/min)
Regulation of Stroke Volume
• SV = end diastolic volume (EDV) minus
end systolic volume (ESV)
• EDV = amount of blood collected in a
ventricle during diastole
• ESV = amount of blood remaining in a
ventricle after contraction
Factors Influencing Stroke Volume
• Force of contraction
• Venous return:
• Skeletal pumping
• Respiratory pumping
Regulation of Heart Rate: Autonomic Nervous System
• Heart rate range: about 50 – near 200
• Typical resting: near 70 (60-100).
• Hormones like epinephrine, norepinephrine,
thyroid hormone (T3) increase heart rate.
• Sympathetic stimulation
• Releases norepinephrine (NE)
• Increases heart rate
• Parasympathetic stimulation
• Releases acetylcholine (Ach)
• Decreases heart rate
Regulators of the Heart Rate
Figure 14-28: Reflex control of heart rate
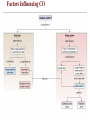
Factors Influencing CO
Blood Flow, Blood Pressure, and Resistance
• Blood flow (F) is directly proportional to the
difference in blood pressure (P) between two
points in the circulation
• If P increases, blood flow speeds up; if P
decreases, blood flow declines
• Blood flow is inversely proportional to resistance
(R)
• If R increases, blood flow decreases
• R is more important than P in influencing local
blood pressure
Systemic Blood Pressure
• The pumping action of the heart generates blood
flow through the vessels along a pressure
gradient, always moving from higher- to lowerpressure areas
• Pressure results when flow is opposed by
resistance
• Systemic pressure:
• Is highest in the aorta
• Declines throughout the length of the pathway
• Is 0 mm Hg in the right atrium
• The steepest change in blood pressure occurs in
the arterioles
Systemic Blood Pressure
Maintaining Blood Pressure
• The main factors influencing blood pressure are:
• Cardiac output (CO)
• Peripheral resistance (PR)
• Blood volume
• Blood pressure = CO x PR
• Blood pressure varies directly with CO, PR, and
blood volume
Chemicals that Increase Blood Pressure
• Adrenal medulla hormones: norepinephrine and
epinephrine increase blood pressure
• Antidiuretic hormone (ADH) – causes intense
vasoconstriction in cases of extremely low BP
• Angiotensin II – kidney release of renin generates
angiotensin II, which causes intense
vasoconstriction
• Endothelium-derived factors – endothelin and
prostaglandin-derived growth factor (PDGF) are
both vasoconstrictors
Chemicals that Decrease Blood Pressure
• Atrial natriuretic peptide (ANP): causes blood
volume and pressure to decline
• Nitric oxide (NO): has brief but potent vasodilator
effects
• Inflammatory chemicals: histamine, prostacyclin,
and kinins are potent vasodilators
• Alcohol: causes BP to drop by inhibiting ADH
Alterations in Blood Pressure
• Hypotension: low BP in which systolic pressure is
below 100 mm Hg
• Hypertension: condition of sustained elevated
arterial pressure of 140/90 or higher
• Transient elevations are normal and can be
caused by fever, physical exertion, and
emotional upset
• Chronic elevation is a major cause of heart
failure, vascular disease, renal failure, and
stroke
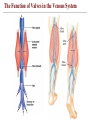
Factors Aiding Venous Return
• Venous BP alone is too low to promote adequate
blood return and is aided by the:
• Respiratory “pump” – pressure changes
created during breathing suck blood toward the
heart by squeezing local veins
• Muscular “pump” – contraction of skeletal
muscles “milk” blood toward the heart
• Valves prevent backflow during venous return
The Function of Valves in the Venous System
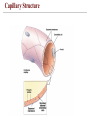
Capillaries
• Narrowest of vessels; wide enough to allow only
for single file passage of RBCs
• Causes slowest flow rate of any vessels in
system
• Thinnest of vessels; walls composed of a single
cell layer
• No smooth muscle
• No elastic
• More capillaries than all other types of vessels
• Greatest cross-sectional area of all vessels in
system
Capillary Structure
Capillaries (continued)
•
•
•
•
Slowest flow rate
Thinnest walls
Narrowest Diameters
Greatest total cross-sectional area
Optimal conditions for
maximum diffusion of
gases, nutrients and
wastes in capillary beds
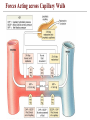
Processes that move fluids across capillary walls
• Diffusion
• Filtration
• Hydrostatic pressure (CHP)
• Reabsorption
Forces Acting across Capillary Walls