* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download 12/09 Tetralogy of Fallot - Anne
Survey
Document related concepts
Remote ischemic conditioning wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Heart failure wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Electrocardiography wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Coronary artery disease wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Aortic stenosis wikipedia , lookup
Myocardial infarction wikipedia , lookup
Echocardiography wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Transcript
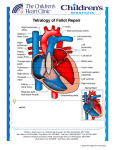
Anne-Marie Anagnostopoulos, MD Non-Invasive Conference December 9, 2009 TETRALOGY OF FALLOT FOR THE ADULT CARDIOLOGIST Outline History and Epidemiology Anatomy and Embryology Spectrum of TOF Surgical Repair Imaging The Adult with Repaired TOF Summary Special Thanks Special thanks to Dr. Anne Marie Valente who helped me enormously History of Tetralogy of Fallot 1671: Stenson first describes pathology of what would later be confirmed as TOF 1888: Etienne-Louis Fallot first recognizes a group of complex cardiac malformations that leads to cyanosis and identifies 4 abnormalities: pulmonary stenosis, VSD, dextroposition of the aorta, and RVH Fallot postulated that these abnormalities resulted from abnormal development of the subpulmonary infundibulum and pulmonary valve. 1924: Abbott and Dawson name the malformation “Tetralogy of Fallot” History From Wikipedia: E. L. A. Fallot. Contribution à l’anatomie pathologique de la maladie bleue (cyanose cardiaque). Marseille médical, 1888, 25: 77-93, 138-158, 207223, 341-354, 370-386, 403-420. Epidemiology Overall, congenital heart disease is rare However, of the cyanotic congenital heart abnormalities, TOF is the most common TOF has an incidence of approximately 32.6 per 100,000 live births The success of early surgical repair has led to a large population of adults with repaired TOF Anatomy and Embryology The fundamental embryologic malformation in TOF is abnormal development of the conotruncus (also known as: conal septum, subpulmonary infundibulum) There is hypoplasia of the conotruncus and anterior/superior displacement of the infundibular septum This results in failure of ventricular septation, subpulmonary and/or pulmonary valve stenosis and overriding aorta The Worlds Best Anatomical Charts. Anatomical Chart Company Skokie, IL. ISBN 0-9603730-5-5. Anatomy and Embryology in Tetralogy of Fallot Figures Emily Flynn, Echocardiography in Pediatric and Congenital Heart Disease Editors Lai, Mertens, Cohen, Geva 2009 Anatomy and Embryology – Simplified Diagram 2D Echo TOF Source: Feigenbaum’s 6th Ed. Spectrum of Tetralogy There is a spectrum of anatomy in TOF with an associated variation in clinical presentation Children with minimal pulmonary stenosis are at one end and can be “pink” At the other extreme is a form of TOF with pulmonary valve atresia and VSD (severely blue) In the latter case, life is sustained by PDA or aorto-pulmonary collateral vessels TOF:Pulmonary Atresia and VSD • Obliterated subpulmonary infundibulum • Marked anterior/left shift of conal septum •Figure Emily Flynn, Echocardiography in Pediatric and Congenital Heart Disease Editors Lai, Mertens, Cohen, Geva 2009 Anatomy and Embryology: Coronary Anomalies Because the aortic root is rotated in TOF, coronary artery anomalies can occur Most common (3%) is origin of LAD from RCA Double LAD occurs 1.8% of time Least common anomalies are single RCA or LCA (0.3% and 0.2% respectively) Surgical Repair Symptomatic infants are repaired early – can be palliated with a variety of shunts Asymptomatic children are usually electively repaired early as well Surgery involves repair of the VSD and enlargement of the RVOT with infundibular septum resection +/- use of a transannular patch This can usually be performed in one step as long as pulmonary artery and its main branches are of adequate size The surgery uniformally results in pulmonic regurgitation Palliative Shunts Glenn Shunt 2D Echo Glenn Shunt: SVC->PA Source: Feigenbaum’s 6th Ed. Surgical Repair – Transannular Patch Natural History Patients post-repair do well up to ~25 yrs postoperatively Modes of death: Sudden cardiac death Arrhythmias Congestive heart failure Nollert G. JACC 1997; 30:1374 The Adult with Repaired TOF Patients often remain asymptomatic Although decreased exercise capacity can often be elicited with objective testing Clinical Presentation: heart failure, dyspnea on exertion, atrial and ventricular arrhythmias, syncope, sudden death ECG findings include RAD, RVH/RAA and RBBB; QRS duration can be prolonged (>180ms is important to note) Sequelae of TOF Repair Residual lesions: Ventricular septal defect Branch pulmonary artery stenosis Tricuspid regurgitation Pulmonary regurgitation Progressive RV dilation and dysfunction Progressive LV dysfunction Aortic root dilation Exercise intolerance, heart failure, arrhythmias and sudden cardiac death Courtesy A. Valente MD Imaging in Repaired TOF Non-invasive imaging is the mainstay of longitudinal follow-up in previously repaired TOF Echocardiography is used to evaluate: residual VSD/PS, Ao Root size and associated AR, PR, and RV/LV function CMR is used to determine RV volumes and severity of PR Often these modalities are used in a complementary fashion Pulmonary Regurgitation Nearly universal Severity is dictated by: compliance of the RV capacitance of the pulmonary arteries Early: presence of RVH (↓ RV compliance) and small PAs (↓ capacitance) →↓ PR Late: dilation and thinning of the RV ( ↑ compliance) and dilation of the PAs (↑ capacitance) →↑ PR Courtesy A. Valente MD Pulmonary Regurgitation Courtesy A. Valente Effects of Chronic PR Adaptive mechanisms in chronic PR increased RV end-diastolic volume increased RV stroke volume These mechanisms compensate for the hemodynamic burden placed on the RV for many years Studies in the 1970’s – 1980’s on survivors of TOF repair were largely asymptomatic (based on self-reporting) Geva T. STCVS 2006; 9:11. Effects of Chronic PR Compensatory mechanisms exist up to a certain point, but ultimately these mechanisms fail Courtesy A. Valente MD Effects of Chronic PR Good RV Function Poor RV Function Courtesy A. Valente Severity of Pulmonary Regurgitation • Prospective study of 34 adults with repaired TOF • Echocardiogram & cardiac MRI within 3 months • Median age 33 yrs (12 yrs) • Mean time since initial surgical repair 25 8 yrs • 13 subjects had undergone transannular patch • 6 subjects had undergone bioprosthetic PVR Silversides C. JASE 2003; 16: 1057 Pulmonary Regurgitation % PR and volume are inversely related to the pressure half-time: r = -0.6, p <0.001 Mild PR Severe PR Silversides C. JASE 2003; 16: 1057 Pulmonary Regurgitation • In addition, PHT <100ms had highest sensitivity and specificity for detecting significant PR (RF >20%) Silversides C. JASE 2003; 16: 1057 Biventricular Interaction Median age from repair 21 years Unfavorable ventricularventricular interaction Confirmatory data that RV mechanics are only part of the problem Patients repaired at older age, more likely to have poor clinical status later Geva T. JACC 2004; 43(6): 1068 RV Function by Echocardiography Often adults with repaired TOF cannot undergo CMR due to devices Myocardial Performance Index (MPI) has been shown to correlate with MRI RVEF Retrospective study of 57 adults (repaired TOF) with a CMR and Echo within 6 months of each other RV MPI = (Doppler duration of TR-RV ejection time)/RV ejection time Schwerzmann, M. AJC 2007;99:1593 RV MPI Correlation With CMR RVEF MPI = (a-b)/b Schwerzmann, M. AJC 2007;99:1593 RV MPI Correlation With CMR RVEF Schwerzmann, M. AJC 2007;99:1593 Regional Wall Motion Abnormality • 85 subjects repaired TOF underwent MRI RVOT outflow aneurysm/akinesia present in 57% No significant difference in the type of repair Aneurysm/akinesia negative effect on RVEF Davlouros et al. JACC 2002; 40:2044 Pulmonary Valve Replacement Operative risk is small: mortality < 2% What criteria should we use in patient selection? Traditional indication: patient symptoms Is there a risk to waiting until patients develop symptoms? Patients may not detect subtle changes in exercise capacity By the time patients notice symptoms, problems may be severe and irreversible *Oosterhof T. Heart 2007; 93: 506 Predictors of Adverse Outcome 88 subjects with repaired TOF Surgical repair between 1966-1987 CMR between 1997-2001 Median follow-up from MRI 4.2 yrs 22 subjects had a major clinical event 4 deaths 8 sustained VT 10 change in NYHA class from good to poor Larger RVEDV, LVEF<50%, RVEF<45% by CMR predicted adverse events Knauth A. Heart 2008; 94: 211-16. Proposed Criteria for PVR Balance between patient’s clinical status (exercise capacity, heart failure symptoms, arrhythmia) and quantitative information Decision to do PVR is quite variable center to center Repaired TOF with moderate or severe PR (PR RF >25% by CMR) and > 2 criteria RVEDVi > 160 cc/m2 ( z > 5) RVESVi > 70 cc/m2 LVEDVi < 65cc/m2 RVEF < 45% RVOT aneurysm LVEF < 50% Geva T. STCVS 2006; 9:11. Aortic Root Dilation Aortic root dilation occurs in a subset of repaired TOF adults and can lead to significant AR May be a result of R L shunt prior to repair though not fully understood why it progresses after A small retrospective study identified risk factors for Ao root dilation (defined as Ao root size observed:expected >1.5) Therefore it is important to closely follow Ao root size with imaging longterm Aortic Root Dilation Niwa, K. Circulation 2002;106:1374 Predictors of Arrhythmia and SCD A study in England evaluated data from 793 repaired TOF patients QRS duration >180ms was found to be predictive of SCD and ventricular arrhythmias Older age at repair was associated with Afib/AFlutter and SCD QRS duration rate of change may also be significant predictor of SCD Gatzoulis, M. Lancet 2002; 356:95 Recommendations ECG (QRS duration): every 12 months Exercise Testing: every 24-36 months Echo: every 24 months CMR (RVEDVi, RV/LV EF): every 24 months EP testing: when clinically indicated Echo and CMR are used together Authors from CHB Geva T. STCVS 2006; 9:11. Summary Because of successful childhood repair, larger population of adults with repaired TOF exists and can present to adult cardiologists Pulmonary Regurgitation is predominant hemodynamic abnormality leading to RV dilation and dysfunction Timing of surgery for PR is an area of great interest as clinical symptoms do not always correlate with severity of PR and RV dysfunction. Echo and CMR are used together to follow repaired patients long term Aortic root dilation occurs in a subset of patients and must also be followed closely QRS duration >180 ms is an important predictor of ventricular arrhythmias and SCD References Feingenbaum’s Echo Textbook, 6th Ed. Echocardiography in Pediatric and Congenital Heart Disease Editors Lai, Mertens, Cohen, Geva 2009 Yale Congenital Heart Disease website: www.med.yale.edu/intmed/cardio/chd/ Braunwald’s Textbook Heart Disease