* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download P - AATS
Survey
Document related concepts
Transcript
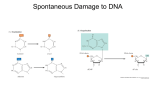
Ultra long term outcomes in adult survivors of tetralogy of Fallot and the effect of pulmonary valve replacement Dobson R1,2, Danton M2, Walker N2, Tzemos, N1,Walker H2 1Institute of Cardiovascular and Medical Sciences, University of Glasgow 2Scottish Adult Congenital Cardiac Service, Golden Jubilee National Hospital Part 1 INTRODUCTION The problem • Survival to adulthood of infants with tetralogy of Fallot (ToF) now exceeds 90% in modern cohorts1,2 • Form a significant proportion of the workload of adult CHD services • The ability of post-ToF repair interventions to modify the long term prognosis for these patients has not been fully defined 1Ide et al 2009, 2Park et al 2010 Objective • To define the long term outcomes of adult survivors of ToF with respect to – Survival, functional capacity and adverse events – The effect of pulmonary valve replacement on clinical and functional outcome Part 2 METHODOLOGY Data collection • National centralized model for ACHD care in Scotland • Computerised database • Electronic records were where possible corroborated with op notes and medical certificate of cause of death Methods • Overall survival analysis; KM curve compared to age and gender matched controls • Morbidity outcomes – – – – Ventricular arrhythmia Atrial arrhythmia Device (pacemaker or ICD) Reintervention and PVR • Current functional status (clinical / CPET / CMR data) Part 3 RESULTS Baseline characteristics • 376 patients (male:female 59:41) post ToF repair who survived to at least age 16 • Mean age at repair 5.2 years (SD 7.3); median 3 years • Mean follow-up from repair 28.3 years (SD 9.4) Era of repair Temporal trends in median age at repair* *Excluded 1950s and 2000s as too few patients in each category ToF subtypes and repair details Variable % Subtype Classical ToF-PA, ToF absent pulmonary valve, ToF-AVSD Unknown 93.6 4.1 1.3 Palliative shunt 0 1 >1 65.4 29.0 5.6 Repair Infundibular resection Transannular patch VSD closure and pulmonary homograft Unknown 19.1 30.1 5.9 45.0 Overall survival lower than general population Log rank test p <0.001 Tetralogy cohort Control group Deaths • 15 patients died at a mean age of 49 +/- SD 13.7 years • Cause of death – – – – – – Heart failure (5) Postoperative – PVR (3)* Sepsis (3) Sudden (2) Stroke (1) Malignancy (1) *From 166 PVR procedures Multivariate analysis for death Variable HR 95% CI P-value Older age at repair 1.11 1.04 – 1.19 0.003 Male gender 5.64 1.08 – 29.49 0.041 Nonclassical ToF 13.43 2.51 – 71.92 0.002 QRS duration* 1.07 1.02 – 1.11 0.003 *Univariate mode only Quality of life • NYHA class – I: 87.5%, – II: 5.3% – III: 0.5% • Median peak VO2 69.5% predicted • Social deprivation score = 4.1 – Scottish population mean 4; p=0.51 • Total Fertility Rate 0.18 (1.61 for national data 2013) MRI n=181 RV volumes RV ejection fraction CPET n=169 % predicted VO2max VE/VCO2 slope RVEF versus peak VO2 Spearman’s rho 0.226 p = 0.013 Reintervention Procedure N PVR 166 Surgical 147 1 2 3 110 14 3 Percutaneous 19 1 2 17 1 Early revision 24 AVR/root replacement 2 Tricuspid valve 8 Balloon pulmonary angioplasties 24 Historical trends in repeat intervention Freedom from repeat intervention Total reintervention PVR Multivariate analysis for reintervention Variable HR 95% CI P-value Transannular patch 1.72 1.23 – 2.39 0.001 Nonclassical ToF 2.95 1.57 – 5.54 0.001 Older age at repair 0.96 0.92 – 1.00 0.008 Transannular patch 1.79 1.26 – 2.56 0.001 Nonclassical ToF 4.22 2.16 – 8.25 <0.001 Older age at repair 0.92 0.87 – 0.96 <0.001 Any reintervention PVR only PVR and survival Log rank test p = 0.539 PVR group Severe PR group The effect of PVR on RV size and function Indexed RVEDV ml/m2 P < 0.001 N=17 RV ejection fraction % P = 0.154 The effect of PVR on exercise performance Peak VO2 as % predicted P = 0.623 N=16 VE/VCO2 slope P = 0.050 Prevalence of arrhythmia • Atrial arrhythmia in 13.3%, ventricular arrhythmia in 3.4% • Therapy – 12.8% on regular antiarrhythmics – 5.1% ICD – 2.1% had radiofrequency ablation Freedom from arrhythmia Multivariate analysis for arrhythmia • Atrial arrhythmia – Older age at repair conferred hazard ratio of 1.10 (95% CI 1.07 – 1.13) p = <0.001 • No significant variables identified for ventricular arrhythmia Device insertion (pacemaker or ICD) • 9% of patients overall • Device type – Pacemaker in 4% (VVI 0.8% and DDD in 3.2%) – ICD in 4.8% – CRT-D in 0.3% Freedom from device insertion Part 4 SUMMARY Mortality • Long term (>30 years) survival remains excellent – For patients who survive to age >16 • Heart failure is the main cause of death • Older age at repair, non-classical forms of ToF, and male gender confer increased risk Morbidity • Arrhythmia is common • High rates of repeat intervention, mainly PVR, performed with low mortality • PVR reduces RV volumes but does not improve exercise capacity Limitations and future directions • Single center retrospective cohort • Functional data is cross-sectional for a heterogenous group • Historical loss of follow-up – patients geographically remote from surgical center may still be under the radar • Creation of an international registry will enable far more powerful and robust analysis of prognosis and intervention Part 4 QUESTIONS