* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Dear Colleagues - Centre for Rare Cardiovascular Diseases
Survey
Document related concepts
Heart failure wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Coronary artery disease wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Cardiothoracic surgery wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Cardiac surgery wikipedia , lookup
Atrial septal defect wikipedia , lookup
Ventricular fibrillation wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Transcript
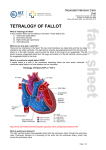
Article* "Development of the European Network in Orphan Cardiovascular Diseases" „Rozszerzenie Europejskiej Sieci Współpracy ds Sierocych Chorób Kardiologicznych” Title: Patient after operation of Tetralogy of Fallot with pulmonary hypertension RCD code: Please fill in the code Author: Lidia Tomkiewicz-Pajak Affiliation: Department of Cardiac and Vascular Diseases, John Paul II Hospital, Krakow, Poland. Date: 28.12. 2014 * The article should be written in English] John Paul II Hospital in Kraków Jagiellonian University, Institute of Cardiology 80 Prądnicka Str., 31-202 Kraków; tel. +48 (12) 614 33 99; 614 34 88; fax. +48 (12) 614 34 88 e-mail: [email protected] www.crcd.eu Background, Tetralogy of Fallot is the most common cyanotic congenital heart disease after one year of age. Less than 5% of all patients with uncorrected ToF survive beyond their 40s. Prognosis after surgical correction is good with a 32-year survival of 86% [1]. Surgery is carried out to close ventricular septal defect (VSD) and relieve right ventricular outflow tract (RVOT) obstruction. Patients who have reached adulthood after earlier repair of Tetralogy of Fallot frequently present complications. They include severe pulmonary regurgitation (PR), right ventricular outflow tract obstruction, right ventricular dilation and dysfunction, residual VSD, aortic root dilation with aortic regurgitation, left ventricular dysfunction, endocarditis, atrial and ventricular tachycardia, and sudden cardiac death. Case presentation, A 40-year-old woman after correction of Tetralogy of Fallot was admitted to hospital due to deterioration in exercise tolerance (NYHA functional class III). Surgical correction was performed in 1974. Surgical closure of residual VSD was performed in 2003. A dual chamber pacemaker was implanted due to sick sinus syndrome associated with paroxysmal atrial fibrillation in 2005. Current treatment included warfarin and metoprolol CR. Physical examination revealed holosystolic murmur with a thrill at fourth left intercostal space. Routine laboratory tests were within normal limits, except of elevated natriuretic peptide level - 1300 pg/ml. Resting electrocardiogram showed sequential atrial and ventricular pacing. Holter monitoring didn’t reveal cardiac arrhythmias and pacing disturbances. The cardiopulmonary exercise testing showed reduced exercise tolerance (workload of 8,4METs) and a reduction in maximal oxygen consumption - 15,2 ml/kg/min. The observed values were significantly lower compared previous examinations, February 2011 - 22 ml/kg/min and October 2010 23 ml/kg/min. The transthoracic echocardiography revealed numerous abnormalities: enlargement of all heart chambers, impaired RV systolic function, residua perimembraneous VSD with left to right shunting, severe PR, dilated pulmonary trunk and branches of pulmonary artery, mild aortic regurgitation, moderate to severe tricuspid regurgitation,dilated tricuspid annulus, elevated RV systolic pressure (60 mmHg). Coronary angiography revealed no critical lesions in coronary arteries. Right heart John Paul II Hospital in Kraków Jagiellonian University, Institute of Cardiology 80 Prądnicka Str., 31-202 Kraków; tel. +48 (12) 614 33 99; 614 34 88; fax. +48 (12) 614 34 88 e-mail: [email protected] www.crcd.eu catheterization confirmed presence of residual VSD with left- to- right shunt (ratio of pulmonary to systemic flow was 2:1). Other findings included mild pulmonary hypertension (mean pulmonary artery pressure, 29 mmHg) increased pulmonary vascular resistance - 203,9 ARU and increased pulmonary capillary wedge pressure - 16 mmHg. Discussion, Patients with transannular patch repair of right ventricular outflow tract obstruction have higher degree of PR compared to patients with subvalvular resection or repair without a patch [2]. PR may be well tolerated for decades before any symptoms develop but in some patients can lead to progressive right ventricular dilatation, onset of tricuspid regurgitation and the need for surgery. It is also known as risk factor for ventricular arrhythmias and sudden cardiac death [3]. Long-term consequences of PR are augmented by co-existing distal pulmonary stenosis and pulmonary arterial hypertension. Residual VSD requiring reintervention after primary surgical repair of Teralogy of Fallot is not rare [4]. Significant left to right shunt through VSD leads to LV volume overload, pulmonary hypertension should be qualify for surgery. Moreover residual VSD closure, is recommended if the patient is undergoing pulmonary valve surgery. Reference. [1] Murphy JG, Gersh BJ, Mair DD, et al. Long-term outcome in patients undergoing surgical repair of tetralogy of Fallot. N Engl J Med 1993;329:593–599. [2] Frigiola A, Redington AN, Cullen S, Vogel M. Pulmonary regurgitation is an important determinant of right ventricular contractile dysfunction in patients with surgically repaired tetralogy of Fallot. Circulation. 2004 Sep 14;110(11 Suppl 1):II153-7. [3] Gatzoulis MA, Balaji S, Webber SA, et al. Risk factors for arrhythmia and sudden cardiac death late after repair of tetralogy of Fallot: a multicentre study. Lancet 2000;356:975–981. [4] Hanna BM, El-Hewala AA, Gruber PJ, et al. Predictive value of intraoperative diagnosis of residual ventricular septal defects by transesophageal echocardiography. Ann Thorac Surg. 2010 Apr;89(4):1233-7. ……………………………………….. Author’s signature** John Paul II Hospital in Kraków Jagiellonian University, Institute of Cardiology 80 Prądnicka Str., 31-202 Kraków; tel. +48 (12) 614 33 99; 614 34 88; fax. +48 (12) 614 34 88 e-mail: [email protected] www.crcd.eu [** Signing the article will mean an agreement for its publication] John Paul II Hospital in Kraków Jagiellonian University, Institute of Cardiology 80 Prądnicka Str., 31-202 Kraków; tel. +48 (12) 614 33 99; 614 34 88; fax. +48 (12) 614 34 88 e-mail: [email protected] www.crcd.eu