* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Cardiac Pathophysiology
Cardiovascular disease wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Remote ischemic conditioning wikipedia , lookup
Heart failure wikipedia , lookup
Electrocardiography wikipedia , lookup
Aortic stenosis wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Rheumatic fever wikipedia , lookup
Artificial heart valve wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Jatene procedure wikipedia , lookup
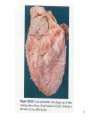
Management of acute coronary syndrome wikipedia , lookup
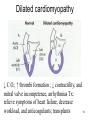
Mitral insufficiency wikipedia , lookup
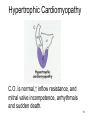
Coronary artery disease wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
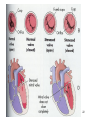
Cardiac Pathophysiology 1 Pericarditis • Often local manifestation of another disease • May present as: – Acute pericarditis – Pericardial effusion – Constrictive pericarditis 2 Acute Pericarditis • Acute inflammation of the pericardium • Cause often unknown, but commonly caused by infection, uremia, neoplasm, myocardial infarction, surgery or trauma. • Membranes become inflamed and roughened, and exudate may develop 3 Symptoms: • Sudden onset of severe chest pain that becomes worse with respiratory movements and with lying down. • Generally felt in the anterior chest, but pain may radiate to the back. • May be confused initially with acute myocardial infarction • Also report dysphagia, restlessness, irritability, anxiety, weakness and malaise 4 Signs • Often present with low grade fever and sinus tachycardia • Friction rub (sandpaper sound) may be heard at cardiac apex and left sternal border and is diagnostic for pericarditis (but may be intermittent) • ECG changes reflect inflammatory process through PR segment depression and ST segment elevation. 5 6 Treatment • Treat symptoms • Look for underlying cause • If pericardial effusion develops, aspirate excess fluid • Acute pericarditis is usually self-limiting, but can progress to chronic constrictive pericarditis 7 Pericardial effusion • Accumulation of fluid in the pericardial cavity – May be transudate – May be exudate – May be blood • Not clinically significant other than to indicate underlying disorder, unless: • Pressure becomes sufficient to cause cardiac compression – cardiac tamponade 8 Outcome depends on how fast fluid accumulates. • • • If development is slow, pericardium can stretch If develops quickly, even 50 -100 ml of fluid can cause problems When pressure in pericardium = diastolic pressure, get ↓ filling of right atrium, ↓ filling of ventricles, ↓ cardiac output → circulatory collapse. 9 Clinical manifestations • Pulsus paradoxus – B.P. higher during expiration than inspiration by 10 mm Hg • Distant or muffled heart sounds • Dyspnea on exertion • Dull chest pain • Observable by x-ray or ultrasound 10 Treatment • Pericardiocentesis • Treat pain • Surgery if cause is aneurysm or trauma 11 Constrictive (chronic) pericarditis • Years ago, synonymous with T.B. • Today, usually idiopathic, or associated with radiation exposures, rheumatoid arthritis, uremia, or coronary bypass graft 12 Pathophysiology: • Fibrous scarring with occasional calcification of pericardium • Causes parietal and visceral layers to adhere • Pericardium becomes rigid, compressing the heart →↓ C.O. • Stenosis of veins entering atria • Always develops gradually 13 Symptoms and Signs • • • • Exercise intolerance Dsypnea on exertion Fatigue Anorexia 14 Clinical manifestations • • • • • Weight loss Edema and ascites Distention of jugular vein (Kussmaul sign) Enlargement of the liver and/or spleen ECG shows inverted T wave and atrial fibrillation • Can be seen on imaging 15 Treatment • Drugs and diet – Digitalis – Diuretics – Sodium restriction • Surgery to remove restrictive pericardium 16 Cardiomyopathies • Disorders of the heart muscle • Most cases idiopathic • Many due to ischemic heart disease and hypertension. • Three categories: – Dilated ( formerly, congestive) – Hypertrophic – Restrictive • Heart loses effectiveness as a pump 17 Dilated cardiomyopathy ↓ C.O.; ↑ thrombi formation ; ↓ contractility, and mitral valve incompetence, arrhythmias Tx: relieve symptoms of heart failure, decrease 18 workload, and anticoagulants; transplants Hypertrophic Cardiomyopathy C.O. is normal,↑ inflow resistance, and mitral valve incompetence, arrhythmais and sudden death. 19 Restrictive cardiomyopathy Reduced diastolic compliance of the ventricle. C.O. is normal or↓; ↑ formation of thrombi, dilation of left atrium, and mitral valve 20 incompetence. Disorders of the Endocardium: Valvular dysfunction • Endocardial disorders damage heart valves • Changes can lead to : – Valvular Stenosis = too narrow – Valvular Regurgitation = too leaky (or insufficiency or incompetence) 21 22 • Valves that are most often affected are the mitral and aortic valves, but in I.V. drug users and in athletes that inject performance enhancing drugs, > 50 % involve only the tricuspid valve. • Heart Murmur – sound caused by turbulent blood flow through damaged valves. 23 Both types of valve disorders: • Cause increased cardiac work, and increased volumes and pressures in the chambers. • This leads to chamber dilation and hypertrophy. • Chamber dilation and myocardial hypertrophy are compensatory mechanisms to increase the pumping capability of the heart. • Eventually, the heart fails from overwork 24 Aortic Stenosis • Three common causes: – Rheumatic heart disease -Streptococcus infection – damage by bacteria and autoimmune response – Congenital malformation – Degeneration resulting from calcification 25 Aortic Stenosis • Blood flow obstructed from LV into aorta during systole Causes increased work of LV → LV dilation & hypertrophy as compensation → prolonged contractions as compensation Finally heart overwhelmed • → increased pressures in LA, then lungs, then right heart 26 Clinical manifestations • • • • • • • • Develops gradually Decreased stroke volume Reduced systolic blood pressure Narrowed pulse pressure Heart rate often slow and pulse faint Crescendo-decrescendo heart murmur Angina, dizziness, syncope, fatigue Can lead to dysrhythmias, myocardial infarction, and left heart failure 27 Mitral Stenosis • Most common of all valve disorders • Usually the result of rheumatic fever or bacterial endocarditis • During healing the orifice narrows, the valves become fibrous and fused, and chordae tendineae become shortened • Get decreased flow from LA to LV during filling • Results in hypertrophy of LA 28 • By causing LA to become pump: • Get increased pulmonary vascular pressures; pressures increase through LA into lung • →pulmonary congestion • →lung tissue changes to accommodate increased pressures • →increased pressure in pulmonary artery • →increased pressure in right heart • →right heart failure 29 Clinical Manifestations • Atrial enlargement can be seen on x-ray • Rumbling decrescendo diastolic murmur, and accentuated first heart sound • Dyspnea • Tachycardia and risk of atrial fibrillation • Other signs and symptoms are of pulmonary congestion and right heart failure 30 Aortic Regurgitation • Caused by acute or chronic lesion of rheumatic fever, bacterial endocarditits, syphilis, hypertension, connective tissue disorder (e.g.Marfan syndrome) or atherosclerosis 31 • Reflux of blood from aorta to LV during ventricular relaxation. • Causes LV to pump more blood w/ each contraction • → LV hypertrophy – LV takes on “globular shape” • → increased pressures in LA, lung, right heart 32 Clinical manifestations • Widened pulse pressure • Prominent carotid pulsations and throbbing peripheral pulses • Palpitations • Fatigue • Dyspnea • Angina • High-pitched or blowing heart sound during diastole 33 Mitral Regurgitation • Causes: mitral valve prolapse, rheumatic heart disease, infective endocarditis, connective tissue disorders, and cardiomyopathy • Permits backflow of blood from the LV into the LA during ventricular systole • Loud pansystolic murmur that radiates into the back and axilla 34 • Causes blood to flow simultaneously to aorta and back to LA. • Both LV and LA pump harder to move same blood twice – →LV hypertrophy and dilation as compensation – Compensation works awhile, then see ↓C.O. – → heart failure – Also →LA hypertrophy • → increased pressures through lungs → ↑ pressures in right heart →right heart failure • Can see edema, shock 35 Clinical Manifestations • Weakness and fatigue • Dyspnea • Palpitations 36 Mitral Valve Prolapse • Cusps of valve billow upward into the LA during ventricular systole • Mitral regurgitation can occur • Most common valve disorder in U.S. • Studies suggest an autosomal dominant inheritance pattern • Many cases completely asymptomatic • Regurgitant murmur or midsystolic click 37 Clinical manifestations • Palpitations • Tachycardia • Light-headedness, syncope, fatigue, weakness • Chest tightness, hyperventilation • Anxiety, depression, panic attacks • Atypical chest pain 38 • Once considered to be a psychiatric malady • May have an autonomic dysfunction in which large quantities of catecholamines are produced. • May be a normal variant • Can see: –chorda rupture –ventricular failure –systemic emboli and sudden death • actually associated with minimal morbidity and mortality 39 Management • • • • Echocardiography for diagnosis Related to degree of regurgitation Antibiotics before invasive procedures blockers to relieve syncope, severe chest pain, or palpitations • Avoid hypovolemia • Surgical repair 40 General Treatment for Valve disorders • Antibiotics for Strep • Anti-inflammatories for autoimmune disorder • Analgesics for pain • Restrict physical activity • Valve replacement surgery 41 Heart failure • Definition – When heart as a pump is insufficient to meet the metabolic requirements of tissues. • Acute heart failure – 65% survival rate • Chronic heart failure – Most common cause is ischemic heart disease 42 Ischemic Heart Disease • Coronary Artery Disease (CAD), myocardial ischemia and myocardial infarction are progression of conditions that impair the pumping ability of the heart by depriving it of oxygen and nutrients. 43 Coronary Artery Disease • Any vascular disorder that narrows or occludes the coronary arteries. • Most common cause is atherosclerosis 44 • The arteries that supply the heart are the first branches off the aorta • Coronary artery disease decreases the blood flow to the cardiac muscle. • Persistent ischemia or complete occlusion leads to hypoxia. • Hypoxia can cause tissue death or infarction, which is a “heart attack,” which accounts for about one third of all deaths in U.S. 45 Risk Factors • • • • • • • • • Hyperlipidemia Hypertension Diabetes mellitus Genetic predisposition Cigarette smoking Obesity Sedentary life-style Heavy alcohol consumption Higher risk for males than premenopausal women 46 Myocardial Ischemia • Myocardial cell metabolic demands not met • Time frame of coronary blockage: • 10 seconds following coronary block –Decreased strength of contractions –Abnormal hemodynamics • See a shift in metabolism, so within minutes: –Anaerobic metabolism takes over –Get build-up of lactic acid, which is toxic within the cell –Electrolyte imbalances –Loss of contractibility 47 • 20 minutes after blockage –Myocytes are still viable, so –If blood flow is restored, and increased aerobic metabolism, and cell repair, – →Increased contractility • About 30-45 minutes after blockage, if no relief –Cardiac infarct & cell death 48 Clinical Manifestations • May hear extra, rapid heart sounds • ECG changes: – T wave inversion – ST segment depression 49 Chest Pain • First symptom of those suffering myocardial ischemia. • Called angina pectoris (angina – “pain”) • Feeling of heaviness, pressure • Moderate to severe • In substernal area • Often mistaken for indigestion • May radiate to neck, jaw, left arm/ shoulder 50 • Due to : – Accumulation of lactic acid in myocytes or – Stretching of myocytes • Three types of angina pectoris: – Stable, unstable and Prinzmetal 51 Stable angina pectoris • Caused by chronic coronary obstruction • Recurrent predictable chest pain • Gradual narrowing and hardening of vessels so that they cannot dilate in response to increased demand of physical exertion or emotional stress • Lasts approx. 3-5 minutes • Relieved by rest and nitrates 52 Prinzmetal angia pectoris (Variant angina) • Caused by abnormal vasospasm of normal vessels (15%) or near atherosclerotic narrowing (85%) • Occurs unpredictably and almost exclusively at rest. • Often occurs at night during REM sleep • May result from hyperactivity of sympathetic nervous system, increased calcium flux in muscle or impaired production of prostaglandin 53 Unstable Angina pectoris • Lasts more than 20 minutes at rest, or rapid worsening of a pre-existing angina • May indicate a progression to M.I. 54 Silent Ischemia • Totally asymptomatic • May be due abnormality in innervation • Or due to lower level of inflammatory cytokines 55 Treatment • Pharmacologically manipulate blood pressure, heart rate, and contractility to decrease oxygen demands • Nitrates dilate peripheral blood vessels and • Decrease oxygen demand • Increase oxygen supply • Relieve coronary spasm 56 • blockers: – Block sympathetic input, so – Decrease heart rate, so – Decrease oxygen demand • Digitalis – Increases the force of contraction • Calcium channel blockers • Antiplatelet agents (aspirin, etc.) 57 Surgical treatment • Angioplasty – mechanical opening of vessels • Revascularization – bypass – Replace or shut around occluded vessels 58 Myocardial infarction • Necrosis of cardiac myocytes – Irreversible – Commonly affects left ventricle – Follows after more than 20 minutes of ischemia 59 Structural, functional changes • • • • • • Decreased contractility Decreased LV compliance Decreased stroke volume Dysrhythmias Inflammatory response is severe Scarring results – – Strong, but stiff; can’t contract like healthy cells 60 Clinical manifestations • Sudden, severe chest pain – Similar to pain with ischemia, but stronger – Not relieved by nitrates – Radiates to neck, jaw, shoulder, left arm • Indigestion, nausea, vomiting • Fatigue, weakness, anxiety, restlessness and feelings of impending doom. • Abnormal heart sounds possible (S3,S4) 61 • Blood test show several markers: – Leukocytosis – Increased blood sugar – Increased plasma enzymes • Creatine kinase • Lactic dehydrogenase • Aspartate aminotransferase (AST or SGOT) – Cardiac-specific troponin 62 ECG changes • Pronounced, persisting Q waves • ST elevation • T wave inversion 63 Treatment • • • • • • • First 24 hours crucial Hospitalization, bed rest ECG monitoring for arrhythmias Pain relief (morphine, nitroglycerin) Thrombolytics to break down clots Administer oxygen Revascularization interventions: by-pass grafts, stents or balloon angioplasty 64