* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Identifying Central Hypothyroidism in Persons with
Hormone replacement therapy (menopause) wikipedia , lookup
Hormone replacement therapy (male-to-female) wikipedia , lookup
Sexually dimorphic nucleus wikipedia , lookup
Signs and symptoms of Graves' disease wikipedia , lookup
Growth hormone therapy wikipedia , lookup
Hypothalamus wikipedia , lookup
Hyperthyroidism wikipedia , lookup
Pituitary apoplexy wikipedia , lookup
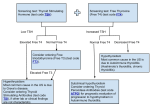
Identifying Central Hypothyroidism in Persons with Traumatic Brain Injury Elizabeth Reusche BSN, RN & Mary Anne Saveoz BSN, RN, CRRN Introduction Individuals who have sustained Traumatic Brain Injury (TBI) frequently develop pituitary and/or hypothalamic dysfunction. This is a contributing factor to central hypothyroidism whose onset is not related to injury severity and can, in fact, develop several to many years post injury. This poster will define central hypothyroidism, indications for ongoing evaluation of pituitary hormone secretion, current diagnostic tools and treatment with adequate hormonal therapy. The rehabilitation nurse’s involvement is critical in advocating for these individuals for proper diagnosis and treatment. Pituitary Gland- Referred to as the “master gland”. Anterior pituitary has many functions. A critical hormone it produces is TSH which stimulates the thyroid gland to produce Thyroxine. Hypothalamus – A midbrain structure that produces hormones which direct the pituitary gland to stimulate the thyroid gland. Thyroid Gland- Secretes Thyroxine (T4) which is needed for growth and development. Located in the lower throat region. Primary Hypothyroidism is a dysfunction occurring at the level of the thyroid gland. Causes • Autoimmune disease (Hashimoto disease) • Thyroid surgery • Radiation therapy • Medication Comprehensive medical history, physical exam, and extensive lab work. Low serum TSH concentration in the presence of subnormal T4 and T3 concentration is characteristic of central hypothyroidism. Signs and Symptoms of Hypothyroidism • • • • • • • • • • • • Weakness, fatigue • Dry skin Cool extremities • Puffy face, hands • Difficulty hearing Alopecia • Paresthesia • Bradycardia Menorrhagia • Poor concentration • Peripheral edema Poor memory Delayed tendon reflex relaxation Constipation Carpal tunnel syndrome Weight gain Serous cavity effusions Dyspnea Hoarse voice Male: Date of Injury- 2008 (age 30) Diagnosed with Hypothyroidism in February 2013 (age 35, 5 yrs post injury) Managed by PCP No T3/T4 levels were monitored Date 2/2013 6/2013 12/2014 5/2015 TSH 5.02 0.85 4.83 4.93 Levothyroxine 50 mcg 50 mcg 50 mcg 75 mcg Female: Date of Injury- 1989 (age 17) Secondary or Tertiary Hypothyroidism (central hypothyroidism) is a defect at the pituitary, hypothalamus, or hypothalamic portal circulation level Causes • Certain drugs such as opiates, glucocorticoids, dobutamine, and dopamine • Space occupying lesions of the brain or pituitary • Radiation • Traumatic brain injury • Growth hormone therapy • Genetic mutations • Idiopathic causes Case Studies Diagnosis Definitions & Causes Diagnosed with Hypothyroidism in March 2009 (age 37, 20 yrs post injury) Managed by PCP No T3/T4 levels were monitored Treatment A majority of people are treated with Levothyroxine. The principle of this treatment includes replacement of thyroid hormone. Labs are monitored for serum TSH T3 and T4 levels with the goal of maintaining these levels in the higher range of normal. Client Review • • • • • • • • Total of 29 clients Females n=11, Males n=18 Age range: 40 – 60 years Hypothyroidism diagnosis: 7 clients (5 females, 2 males) This is 24% of reviewed population Levothyroxine doses: Female 25mcg – 112mcg Male 50mcg-75mcg One female diagnosed with Grave’s Disease in 2000 (two years prior to injury) and was treated with I-131. Date 3/2009 3/2010 2/2011 7/2011 12/2012 2/2013 4/2013 6/2013 3/2015 TSH 7.32 5.36 3.95 2.28 3.95 3.28 2.45 1.67 3.40 T4 -----0.9 --1.2 Levothyroxine 25 mcg 50 mcg 50 mcg 50 mcg 50 mcg 75 mcg 100 mcg 100 mcg 112 mcg Conclusions Individuals who have sustained TBI frequently develop pituitaryhypothalamic dysfunction which is a contributing factor to central hypothyroidism. The onset of central hypothyroidism is not related to the severity of the injury. Central hypothyroidism, most importantly, can arrive several to many years after injury. Ongoing evaluation of pituitary hormone secretion should be included in long term follow up of all TBI patients so proper diagnosis can be made and adequate hormonal therapy administered.