* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download glycogen, calcification
Survey
Document related concepts
Transcript
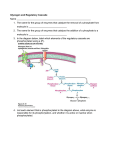
General Pathology Cellular and Organ Pathology Disorders of Glycogen Degradation. Pathology of Calcification. Jaroslava Dušková Inst. Pathol. ,1st Med. Faculty, Charles Univ. Prague Disorders of Glycogen Degradation. Pathology of Calcification. Table of contents Glycogen – morphology, function, regulation – pathology states inborn - glycogenoses acquired – – – – hyperglycemia – DM I, DM II, MODY hypoglycemia – insulinoma hyperglycemia – glucagonoma glycogen storage in the neoplasms (clear cell kidney ca, seminoma, Ewing sarcoma… Calcification – dystrophic – metastatic clinical manifestations complications Glycogen linear and branched polymer cca 60 000 - D-glucose molecules – monoparticles (beta) - muscle – complex particles (alpha) - hepatocyte Main Hormones in Glycogen Metabolism insulin glucagon Insulin The Actions of Insulin on Cells glycogen synthesis –in liver (and muscle) cells. Reducing high blood glucose levels in diabetes. Forces adipose tissue to make fats; lack of insulin causes the reverse. Decreased proteolysis Decreased lipolysis Decreased gluconeogenesis Increased amino acid uptake Increased potassium uptake Arterial muscle tone – forces arterial wall muscle to relax, increasing blood flow, especially in micro arteries; lack of insulin reduces flow by allowing these muscles to contract Increased Glucagon -physiologic effects increase in blood concentration of glucose. Neurons can not utilize alternative energy sources like fatty acids Glucagon stimulates breakdown of glycogen stored in the liver. Glucagon activates hepatic gluconeogenesis. Non-hexose substrates such as amino acids are converted to glucose. Glucagon also appears to have a minor effect of enhancing lipolysis of triglyceride in adipose tissue. Control of Glucagon Secretion Secreted in response to hypoglycemia Two other conditions : – Elevated blood levels of amino acids, after consumption of a protein-rich meal . Since high blood levels of amino acids also stimulate insulin release both insulin and glucagon are active. – Exercise: not clear whether the actual stimulus is exercise per se, or the accompanying exercise-induced depletion of glucose. Negative control - glucagon secretion is inhibited by – high levels of blood glucose – insulin – somatostatin Glucagon – 29AA α-cells in islets opposite effect of insulin insulin glucagon Clear Intracellular Vacuoles & adjunct techniques accumulations of water neg. lipides SUDAN, OIL RED polysaccharides PAS, A-PAS Glycogen Metabolism Diseases diabetes mellitus type I (& LADA – late autoimmune diabetes of adults) - polygenic HLA-DR 3, 4 diabetes mellitus type II - polygenic MODY - more than 10 types described – monogenic insulinoma glucagonoma insulin resistance in : – metabolic syndrome (=obesity, glucose intolerance, hypertension, hyperlipemia… ) – insulin receptor mutations – polycystic ovary syndrome – hypercortisolism……. Enzymes Involved in Glycogen Metabolism glucokinase, hexokinase isomerases g.-synthase - brancher phophorylase kinase - debrancher g-6-phosphatase -glucosidase… Glucokinase Role in Maintenance of Glucose Homeostasis coded on 7th chromosome inactivating and activating mutations - GLUCOKINASE DISEASES inactivating mutation – MODY 2 – autosomal dominant - heterozygots – mild hyperglycemia – homozygots - severe newborn diabetes activating mutation - heterozygots – severe hypoglycemia Glucokinase role in maintenance of glucose homeostasis M glucose – G6P GLUT2 ATP/ADP pancreas – B cell K+ GKB Ca2+ insulin glucose GLUT2 GKA GKh glucose IR G6P glycogen hepatocyte Storage Diseases Def.: inborn errors of metabolism (mostly single gene abnormality) leading to an enzyme defect with subsequent accumulation of the substrate (& lack of the product) in tissues or organs „thesaurismoses“ Gr. thesaurus = treasure, storage Causes of Glycogenoses I-VIII & Fructose Intolerance lysosomal breakdown Glycogenoses - complications glycogen glucose liver other organs liver types blood glucose hepatomegaly glucose glycogen other types hypoglycemia muscle types in muscle effort cardiomegaly, cramps, weeknes resp. muscles palsy myoglobinuria cardiorespiratory insufficiency kidney failure E defect - gl-6 - phosphatase Organ damage - liver, kidney Glycogenosis I – von Gierke E-defect-alpha1, 4 - glucosidase Organ damage - heart Glycogenosis II – Pompe Glycogen Storage Diseases -1. Disease E- def Severity of Tissues Disease Involved von Gierke Glucose-6 Severe phosphatase Liver,kidney, gut Pompe 1,4 Lethal glucosidase Heart (+systemic) Cori Amylo-1,6 Lethal Glucosidase (debrancher) Liver (+systemic) Glycogen Storage Diseases -2. Disease E- def Andersen Amylo-1,4-1,6 Mc Ardle Hers transglucosidase (brancher) Muscle phosphorylase Liver phosphorylase Severity of Disease Lethal Tissues Involved Mild Skeletal muscle Mild Liver Liver (+systemic) Andersen dis. /glycogenosis type IV - liver PAS Armani´cells Best´carmine Complications of Diabetes Glucotoxicity due to: formation of Advanced Glycation E products release of pro-inflammatory cytokines and growth factors generation of ROS (free radicals) in endothelia accelerated developmeent of atherosclerosis Complications of Diabetes macroangiopathy microangiopathy – retinopathy – nephropathy neuropathy infections….. diabetic gangrene Nesidioma capitis pancreatis GAF HE Glycogen water soluble easily lost in long lasting water based fixative solutions Clear cell kidney ca Clear cell kidney ca Metastases in cervical lymph nodes TGB Calcification Def.: depositions of Ca (mostly phosphate salts) in tissues or organs Ca Salts in the Calcified Foci Ca phophate Ca3(PO4)2 Ca diphosphate Ca2P2O7 Hydroxyapatite Ca5 (PO4)3.OH Ca salts in the body bones, teeth dissolved in body fluids (bound to proteins) blood Ca levels 2,1-2,6 mmol/l Calcification - physiology Osteoblasts - collagen I synthesis - matrix vesicles (phragments of osteoblast cytoplasm- storage of hydroxyapatite) Alkalic phosphatase – bone formation Osteoblasts - receptors for PTH on the membrane osteoclasts activation Vitamin D - bone formation PTH - bone resorption Calcitonine – inhibition of osteoclasts Insulin, GH, thyroid hormones, steroids …. Pathology Conditions with Calcium Deposits Calcification dystrophic metastatic Calcinosis localized generalized Chondrocalcinosis - pseudogout Calcification - Microscopy common microtoms tissues – chelates, HCl, non-decalcified – decalcified acetic acid tissues embedding, special microtoms – resin Calcification - Microscopy Basophilic Von Kossa - Ag impregnation (ass. phosphates) Alizarine red + + Tetracyclin fluorescence Polarized light birefringence Calcification Def.: depositions of Ca (mostly phosphate salts) in tissues or organs Classification: dystrophic metastatic Calcification Dystrophic Metastatic Serum Ca level: normal Serum Ca level: Tissues/Organs status Tissues/Organs status dystrophic changes normal, local alcalisation (necrosis, scar…, low metab. turnover) (acid secretion - urine, stomach juice, sweat…) Dystrophic Calcification Frequent necrotic tissue connective tissue vessels calcospherites intracellular calcification of lysosomes Less frequent tendon, cartilage, elastics, bas. membranes Huether S., Mc Cance K.L. eds.: Understanding Huether SE, Mc Cance KL:Pathophysiology. Understanding Pathophysiology 3rd ed., Mosby, 2004, 1235 pages, p.70 clinic reversible ireversible Ca in mitochondria and GER in cytoplasm bound to proteins Released after cell damage Activaton of protein kinases Activaton of phospholipid degradation and loss Phosphorylation of protein and chromatin phragmentation Membrane damage Calcium disturbances leading to cell death Activaton of proteases Cytoskeletal disassembly Dystrophic Calcification Necrosis or degeneration of tissue Release of enzymes Breakdown of organic Alteration of pH phophates Increased deposition of calcium Schaumann´s inclusions Mediocalcinosis Mediocalcinosis Phlebolith H y a li n o s i s Calcificatio anuli fibrosi valvae mitralis Calcificatio valvae aortalis Atherosclerosis aortae gr. I, II, III Aneurysma aortae abdominalis Atherosclerosis calcificata aa. coronariae stenosans Cor petrosum P Ribeiro, R Sapsford, T Evans, G Parcharidis and C Oakley Constrictive pericarditis as a complication of coronary artery bypass surgery. Heart 1984;51;205-210 Cholelithiasis. Empyema vesicae felleae chronicum. Metastatic calcification - causes PTH secretion adenoma, carcinoma destruction of bone – leukemia, myeloma, metastases, Paget (polyostotic) vitamin D intoxication renal failure – phophate retention - secondary hyperparathyreosis - PTH Vitamin D3 (1,25(OH)2D3) is a Hormone Vitamin D3 is responsible for regulating the calcium and phosphorus levels in the blood by their absorption from food and re-absorption of calcium in the kidney. It promotes bone formation It also inhibits parathyroid hormone secretion from the parathyroid gland. Vitamin D affects the immune system by promoting immunosuppression and anti-tumor activity. Vitamin D3 (1,25(OH)2D3) is a Hormone Vitamin D3 is not politically correct. – It discriminates depending where you live, the further you live from the equator the less sun exposure consequently the lower your Vitamin D3 level. – It discriminates against the elderly, as you age your skin loses up to 75% of its ability to make Vitamin D3. – It discriminates against the obese. They have lower levels of Vitamin D3, due to the fact it is oil soluble, that it builds up in the fat tissue. – It discriminates against skin color a dark complected person needs more sun exposure to produce their Vitamin D3 than a fair skinned person. – It also discriminates against a person who does as they are told. It has been reported the incident of breast cancers have increased 40% in Australia due to Vitamin D3 deficiency caused by sunscreen use. alcalic substances inactivity neoplastic cells renal retention vit.D3 intake excess hypercalcemia Disorders of Calcium metabolism fall out tight junctions impermeable lack of vit.D3 hypocalcemia (hypercalcemia, hypocalcemia) decreased bowel resorption insufficient mobilisation Ca2+ renal loss of and retention of PO42- formation of complexes Recklingausen´s disease adenoma gl. para thyreoideae Osteodystrophia fibrosa (Recklinghauseni) Calcificatio metastatica ventriculi et pulmonum „Pumice“ lung osteoid Morphometry of the non-ossified bone tissue PACIENT Starec Bohumil BIOPSIE 57 KOST RODNÉ ČÍSLO KLINIKA III.int. NumberObjects AreaFraction Perimeter MeanChordClass 3 0,25389 7,79E+03 249,713 2 0,294111 7108,63 316,82 RO KT ( % ) 481029/073 1 1 RO O S ( % ) 27% MORFOMETRIE OSTEOID NumberObjects AreaFraction Perimeter MeanChord 2 0,003747 1,34E+03 21,4015 0 0 1,62E-01 0 FO O S ( % ) 100 % Průměr 2,50 LEGENDA ROKT ROOS FOOS RPOS STKT STOS RPO S ( % ) 1% 0% 73% Dun 5% 99% 27,40% 7447,10 283,27 1,00 27,40% 72,60% Relativní objem kostního trámce (vztaženo k měřenému poli) Relativní objem osteoidu (vztaženo k měřenému poli) Frakční objem osteoidu (vztaženo k objemu kostního trámce) Relativní povrch trámce krytý osteoidem Střední tloušťka kostního trámce Střední tloušťka osteoidu 95% 1,00 27,40% 0,19% 0,68% 4,50% 293,97 10,70 0,19% 670,50 99,81% 0,0450173 0,68% 0,95 99,32% Střední šířky kostních komponent 1 0,00 50,00 100,00 150,00 200,00 mikrome try 250,00 300,00 350,00 TRÁMEC OSTEOID 10,70 Pathology Conditions with Calcium Deposits Calcification dystrophic metastatic Calcinosis localized generalized Chondrocalcinosis – pseudogout Calciphylaxix – extensive microvascular calcification and occlusion / thrombosis Calcinosis – the result of either dystrophic or metastatic calcification described first in the skin by Virchow 1855 Forms - localised generalised Localisation – connective tissue, cartilage, skin, muscles Chondrocalcinosis crystal deposit disease (pseudogout) Ca-pyrophosphate and Ca- hydroxyapatite deposits localisation – synovial membrane, cartilage, bone Calcium pyrophosphate deposition disease (Chondrocalcinosis, pseudogout) Clinic: may simulate different diseases Arthroscopy - chalky white deposits Tophaceus deposits with crystalline aggregates Crystals stain with von Kossa technique Foreign body type multinucleated giant cell reaction Deposits are in synovium, cartilage, bone Almafragi A, Vandorpe J, Dujardin K. Calciphylaxis in a cardiac patient without renal disease. Acta Cardiol. 2009 Feb;64(1):91-3. Calciphylaxis is a rare complication that occurs in 1% of patients with end-stage renal disease (ESRD) each year. Extensive microvascular calcification and occlusion/thrombosis lead to violaceous skin lesions, which progress to nonhealing ulcers with secondary infection, often leading to sepsis and death. The lower extremities are predominantly involved (roughly 90% of patients). A case of histologically proven calciphylaxis in a 54-year-old woman with normal renal function and normal calcium-parathyroid homeostasis. She had a history of alcoholic cardiomyopathy, and was treated with warfarin anticoagulation. She has been successfully treated with antibiotics, i.v. biophosphonates and intensive local wound care. We recorded a complete wound healing in contrast to what is reported in other series. Calciphylaxis was reported in: hypoalbuminemia malignant neoplasm systemic corticosteroid use anticoagulation with warfarin chemotherapy systemic inflammation hepatic cirrhosis obesity rapid weight loss, and infection….