* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download David Duncan, M.D. Chief of Cardiothoracic surgery :36 Walking
Survey
Document related concepts
Cardiac contractility modulation wikipedia , lookup
Heart failure wikipedia , lookup
Electrocardiography wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Coronary artery disease wikipedia , lookup
Rheumatic fever wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Myocardial infarction wikipedia , lookup
Pericardial heart valves wikipedia , lookup
Cardiothoracic surgery wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Aortic stenosis wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Transcript
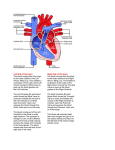
David Duncan, M.D. Chief of Cardiothoracic surgery :36 Walking through the procedure [you know] it starts in the office first and :40 the first thing that we’re going to be doing is assessing the aortic valve, looking to see if the patient has critical aortic stenosis, that it corresponds to their symptoms, that things make sense :50 there’s specific criteria that we look for in the cardiac echo as well as the cardiac catheterization and we take that information and make sure that that all lines up with critical aortic stenosis 1:01 at that point then we start trying to go through the education component of things 1:07 giving the options to the patients on what we can do, how we go about treating that 1:12 typically I’ll explain to the patient that basically the heart is a pump, its purpose in life is just to circulate the blood and nutrients around to the rest of the body, and that the heart is composed of four chambers 1:21 there’s two on the right hand side, two on the left hand side and there are a series of valves, or doorways, that direct that blood through in an efficient manner 1:30 occasionally one of those doors or one of those valves doesn’t work right, occasionally one of those blood vessels might have a blockage and that’s where I get involved as a plumber to either fix that door or to bypass one of those blood vessels 1:45 so for aortic stenosis, typically what’s going on there is the front door on the left ventricle, the valve coming off the left ventricle leading into the aorta [where all the blood flows that goes to the body other than the lungs], 1:58 that doorway is tonetic or doesn’t open the way that it’s supposed to 2:02 and that’s something that we can manage some of the symptoms from with medications but there is no treatment outside of surgical or mechanical repair [of that valve] replacing that valve 2:16 so historically what we’ve done is we’ve gone in surgically, put the patient on the heart and lung machine which does exactly what it sounds like 2:24 – takes over the function of the heart and lungs and would put the heart to sleep and stop the heart 2:29 – and then make an incision in the aorta, which is the big pipe coming off the heart, go down to the aortic valve, excise it, [take it out] and then we would put in another valve 2:39, a man-made valve – either a tissue valve or a mechanical valve 2:43– and once we’ve got the valve in perfectly the way we want it, then we close things up, tidy up, come off the heart and lung machine then we’re done. 2:52 2:53 For patients who are maybe older, have some co-morbid issues, that are not candidates for doing surgery 3:02 – and if you look at the STS data based for 20112012, there was a little less than 100,000 aortic valves done in the United States 3:09 and it turns out that there’s about another 30,000-40,000 folks who’ve not had their aortic valve treated appropriately or by recommendations because of their age or these co-morbid issues 3:27* such as, maybe somebody who’s had previous bypass surgery and had radiation to their chest or maybe they have severe lung disease and they can’t be on the heart and lung machine or maybe they’re just very frail and they’re not able to walk and get around 3:40 And those patients [um, you know] it’s very important for recovering from open heart surgery to be able to ambulate and to help rehabilitate your lungs from that perspective. 3:51 3:52 So these patients that have these co-morbid issues that would not be candidates for having surgery then are referred to me to talk to them about TAVR 4:02 and we start assessing their valve size – there’s two particular areas that I’m going to be looking at 4:12– one of them are the characteristics of the aortic valve itself, the size, what size valve we would replace it with, the calcification that’s in the valve, the height of the coronary ostium, where the blood vessels that come off the heart are located 4:27 because we have a very precise landing zone that we have to put this catheter based valve in 4:32 so we need to know [the very…] have specifics about the valve and the sizing to do that 4:39 4:40 The second thing that [sort of] where I become a bigger part of the team is in the access 4:45 and the access for this typically is going to be through the groin – the transfemoral approach – or occasionally we’ll go just below the breast on the left side and go through the apex of the heart 4:58 where we put a PER string in the heart and and put the catheters directly through that PER string up into the aorta 5:05 [aortic valve…] and occasionally taking off on some of the minimally invasive procedures that we do, we can make a very small sternonomy 5:15 instead of making a full sternonomy the length of the chest we can make a stenonomy that’s a couple of inches in length and you can access the aorta and put the valve in directly through that 5:26 5:27 So the assessment of the vascular access is very important 5:32 and the catheters that we use for placing this valve, the delivery system, are extremely large they’re [in order?] the size of your thumb 5:42 so a lot of folks, particularly if you’re in your 80s or 90s, those vessels may be very calcified and smaller and you’d have to be very careful on how you handle those blood vessels so that you don’t injure or rupture those blood vessels and create additional problems 5:56 5:57 So we’ve gone through the process then of assessing the valve, the character of the valve, the access to get into it and then we’ve talked to the patients about the risks and benefits associated with the procedure 6:08 [prior to getting to the operating room] 6:12 6:39 So once we get to the operating room, we use a different type of operating room. It’s not the typical operating room that we usually do heart surgery in, 6:48 it’s a hybrid room that combines some of the special characteristics of the cath lab along with the ability to do an open procedure with the heart and lung machine in there 6:59 And we also take advantage of a lot of people’s different skill sets 7:03 So there’s interventional cardiologists, such as bob preli and there’s cardiac surgeons such as myself and Dr. [Roshel??] and Dr. Morgan, there’s a perfusionist that’s here, there’s a excellent operating room team that does open heart surgery on a routine basis, the cath lab team is here, 7:24 we have a heart failure specialist who also does a lot of the imaging – Dr. David Small – 7:29 We have cardiac anesthesiologists who specialize in doing cardiac anesthesia and TB(?) echos 7:38 7:39 So we have a group of people who have special skill sets that we use and we combine them in this hybrid procedure 7:46 So once we get into the operating room we prep and drape them just like we would do in an open heart procedure – we are