* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
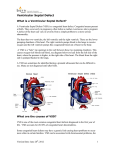
Download Atrial Septal defect (ASD) Device Closure in Detail
Remote ischemic conditioning wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Heart failure wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Coronary artery disease wikipedia , lookup
Electrocardiography wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Cardiothoracic surgery wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Congenital heart defect wikipedia , lookup
Atrial septal defect wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
HOME ABOUT CONTACT US RSS FEED Baby Heart 18 MAY Welcome to Baby Heart..!! By Admin Hi! We are excited to have you here, and happy to share with you some knowledge on baby heart diseases and related conditions. This site tries to give you some insight into baby heart diseases or congenital heart diseases, but it should never be used as a treatment guideline or reference. Please consult a registered medical practitioner or a hospital with pediatric facilities to treat or follow up with any baby heart diseases. Though the authors and staff of this site are highly qualified and experienced in pediatric cardiology we take no responsibility in the accuracy or the authenticity of the information contained with in and we do not claim the same. This site should not be used as an alternative to medical advice in any way be any one. Published by Admin 17 MAY Hole in the Heart: Quick Recap for Parents By Admin Every year 8-12 children per 1000 live deliveries are born with heart defects. These are also called Congenital Heart Defect (CHD) which simply means that the heart developed problems since when it was being formed inside the womb. The commonest problems are holes in the heart. Although sound innocuous, this short phrase in my experience created a lot of apprehension and fear among the family and also health care providers. This article is our attempt to put the facts straight. The Normal Heart: The heart is a pumping organ and has got four chambers. The two upper chambers are called the Right Atrium and Left Atrium (RA and LA) and the two lower chambers are called the Right Ventricle and Left Ventricle (RV and LV). The upper chambers are separated by a wall called inter-atrial septum and the lower chambers are separated by another wall called inter-ventricular septum. From the RV, one artery or pipe takes impure /deoxygenated blood to lungs for oxygenation. This is called the Pulmonary Artery (PA) and from the LV another artery called Aorta carries pure/oxygenrich blood to the whole body. Continue to common holes in the heart –> How to recognize that a child has hole in the heart? What to do if your child has a hole in the heart? Published by Admin in Hole in the Heart, Normal Structure of heart 16 MAY The Common Holes in The Heart By Admin The commonest holes are VSD (Ventricular Septal defect), ASD (Atrial Septal Defect) and PDA (Patent Ductus Arteriosus). VSD is a hole in the interventricular septum or wall between two lower chambers (RV and LV). ASD is the name of the hole in interatrial septum and PDA is actually an extra pipe connecting Aorta and Pulmonary Artery. Of these three, VSDs are the commonest lesion about 25-30% of all congenital heart defects whereas ASD and PDA are about 5-8% of them. Another point to remember is that all of us are born with small ASD and small PDA. However, VSD is never found in normal heart. Continue to How to recognize that a child has hole in the heart? –> Published by Admin in ASD, Atrial Septal Defect, Patent Ductus Arteriosus, PDA, Ventricular Septal defect, VSD 15 MAY How to recognize that a child has hole in the heart? By Admin Interestingly such babies often have Tell- tale signs which a conscious parent can easily pick up. STEP I: How to suspect that a child has heart disease? Frequent cough, cold and pneumonia Poor weight gain as compared to peers Bluish discolouration of lips and nails (Cyanosis) Gets tired easily Fast breathing or difficulty in breathing with flaring of nose, chest retractions Difficulty in feeding: unable to feed at a single attempt (suck-rest-suck cycle) Excessive sweating of forehead Delayed development (delay in sitting, standing, walking etc) Unexplained unconsciousness, chest pain and palpitations The pregnancy and delivery history is also important. If the mother catches infections like rubella in first three months of pregnancy or is addicted to alcohol, cigarette or is taking medicines for epilepsy (convulsions), diabetes, thyroid disorders, their offsprings have an increased risk. Family history is also crucial. Marriage between blood relations (consanguineous marriage), other family members having heart disease etc are high risk factors. STEP II: Now what to do? Visit your child specialist. The pediatrician hears your child’s chest with a stethoscope and can diagnose abnormal sounds called murmurs. He will also check the Blood pressure, pulses and measure the oxygen percentage in your child with an instrument called Pulse Oximeter. Sometimes he asks for an ECG (Electrocardiogram) or Xray of chest. If any of these are abnormal, he will refer your child to a pediatric cardiologist. A pediatric cardiologist is a cardiologist exclusively treating children with heart defects. Depending upon the problem, the pediatric cardiologist usually advises an Echocardiogram, ECG, and Chest X-ray and then decides. Echocardiogram: The most effective diagnostic test is an Echocardiogram. Echo is an ultrasound of heart where ultrasound waves are applied on the heart by a transducer and the reflected waves from heart and blood vessels are recaptured and reconstructed by the computer to form a structural image of the heart. It tells us about the heart chambers, holes in heart, valve problems, heart function, and fluid around heart. Continue to What to do if your child has a hole in the heart? Article by: Dr Maitri Chaudhuri MD(Pediatrics), Fellow National Board(Pediatric Cardiology) Consultant Pediatric Cardiologist Vikram Hospitals, Bangalore Published by Admin in closing of hole in the heart, recognize hole in the heart, treating heart disease 14 MAY What to do if your child has a hole in the heart? By Admin There is no simple and/or single answer to this. Your best guide is the pediatric cardiologist. As I have told that all of us are born with small ASD and PDA. Usually they close spontaneously by 1 st week of life. Premature babies often have large PDAs and they often close after medical therapy with oral Ibuprofen or Indomethacin. Rarely some preemies need surgery. The baby’s neonatologist will start these. Regarding ASD, small defects upto 3-5mm, often close spontaneously. However, larger defects like more than 5-8mm size do not close. They need closure by 3-4 years of age i.e. preschool age either by operation or non-operatively by a button called DEVICE. This is a nonsurgical technique, done under general anesthesia and takes about 40-45 minutes. The child is observed for 24 hours post procedure and then discharged. The advantage is this that there is no scar and unless someone does an Echo or Chest X-ray, it is impossible to identify that the child had an ASD. The usual hospital stay is 36 hours. Although VSDs are the commonest lesion, many of them close spontaneously especially if located in muscular part of the interventricular septum. However, the VSDs are also the trickiest lesion as some of them do not close, get bigger and cause poor growth, frequent chest infections and lung hypertension. It is only through an echocardiography that the correct stage is identified. Nowadays, VSDs are mainly closed by open heart surgery. It is a standard procedure and done in competent centers, the overall risk is <3%. We can expect a hospital stay for 7-10 days after surgery. Some VSDs can also be closed non surgically by DEVICE Closure. PDAs are routinely closed non-surgically by PDA device closure. The procedure time and recovery is like that after ASD device closure. The Financial Issues: Many Indian families delay surgery fearing the cost factor. The costs of cardiac surgery in corporate setups vary between 70,000 – 250,000 Rs as a package. Fortunately many social health schemes like Yasawsini, Arogya Bhagya, Chief Minister Relief Fund, Prime Minister Relief Fund, Needy Heart Foundation etc are regularly helping poor patients below poverty line. Take Home Message 1. Holes in Heart Are Quite Common 2. Be Aware of The Common Signs 3. Go to A Pediatric Cardiologist and Do Echocardiogram 4. Successful Treatment is Available For All Holes 5. Some Holes Can Be Closed Without Surgery 6. Financial Help Is Available If You Cannot Afford Article by Dr Maitri Chaudhuri MD (Pediatrics), Post Doctoral Fellow (Pediatric Cardiology) Consultant Pediatric Cardiologist Vikram Hospitals, Bangalore Email: [email protected] Contact No: 09731721968 Published by Admin in surgery for hole in heart, treating hole in heart 02 SEP FAQ : Ventricular Septal Defect By Admin Q: What is a VSD? Ans: VSD is a abbreviation for the Ventricular Septal Defect. This is a hole in the thick interventricular septum, a muscular wall dividing right and left sided pumping chambers. Q: What is the role of interventricular septum? Ans: Inter-ventricular septum allows the two pumping chamber to pump at the drastically different pressures. The heart is a four chamber structure. The upper two chambers are collecting chambers, known as atria. The right atrium collects oxygen deficient blood from the body and the left atrium collects oxygen rich blood from the lungs. Lower two thick muscular chambers are pumping chambers and known as ventricles. The right sided chamber is connected to lung artery and pumps impure or dark red blood to the lungs. This blood gets oxygen during the process of breathing and becomes bright red in colour. It reaches to left atrium and then to left ventricle. Left ventricle then pumps it out to the aorta. Aorta and its branches then carry this oxygen rich blood all over the body. Left ventricle has to work at 4-5 times higher pressure than the right ventricle. Qns: Why a VSD is harmful to the baby? Ans: A large VSD allows escape of blood into right ventricle and eventually to the lungs. Normally lungs and body accommodate almost equal amount of blood during each cardiac cycle. Lungs get extra blood and body gets less than required amount of blood and baby suffers due to this imbalance. The wet lungs are vulnerable for lung infections. Baby may get about the one episode of pneumonia in every one to two months, they can be life threatening. They also affect the growth of the baby which is maximum in the first 6 months of life. Qns: We have seen babies who become alright with drugs , then why my doctor advised operation? Ans: One must remember following points regarding the VSDs: 1. Every VSD has a natural history. All VSDs can not close spontaneously. 2. The location of VSD is very important in predicting their eventual outcome. A muscular VSD has the probability of spontaneous closure around 80% while a VSD in perimembranous area has 30-40 chance of closure. Even a smaller doubly committed VSD has to be closed as it can harm the aortic valve. 3. No medical management can lead to closure of VSD. Moreover, Medical management is done to support the system till VSD is closing either spontaneously or by interventions. 4. A VSD is a totally curable disease if intervention is done at the right time, with negligible residual effect. 5. A close follow-up and right monitoring with pediatrician, pediatric cardiologist is required. 6. One must not disobey the advice. Because once the flooded lung vessels are thickened , they can not reverse to normal even after the successful operation.. Qns: What are the optimum timing for VSD closure? Ans: A VSD is significant if baby is not growing well , not gaining weight, having perspiration, not able to suck on breast and having high rate of respiration and heart beats and an enlarged heart on X-ray chest. This baby if not improving on medical management must be operated around 3 months. If there are features of decrease in lung pressure one can further wait. A murmur getting louder may be a good sign. But a loud murmur can also be due to some complication which your pediatric cardiologist only can tell you. Qns: Can umbrella device can be used for VSD closures? Ans: VSDs in muscular region are usually closed by devices. However A significant VSD needs to be closed between 3-6 months. So at this as entry through thigh vessel is difficult. Hence still surgical closure is the treatment of choice for the VSDs Some times cardiac bypass can be avoided and VSD can be closed by a device by entering into a beating heart by right ventricular anterior wall. This hybrid procedure is done in operation theaters by pediatric cardiologists and pediatric cardiac surgeon. This shortens the hospital stay for the patients. Qns: My doctor says that a small hole need not to be treated and only SBE prophylaxis to be done. What is the SBE prophylaxis? Ans: A small hole which is not causing enlargement of heart or other symptoms is not a botheration as it can not affect the lungs. SBE prophylaxis is not a kind of medication but it is the set of advices given to the patient. In the presence of hole in heart, the smoothness of inner surface of heart is not maintained . The rough area inside the heart can provide a hiding space for bacteria inside the heart. This is a very serious complication for an otherwise benign condition. A simple way of getting bacteria in the blood is to keep a bad oro-dental hygiene . When we brush our teeth there may be bleeding and also the entrance of bacteria of oral cavity into the blood. Following are the common precautions to be taken: i) Brushing of teeth at morning and before going into bed. ii) Use of mouth-wash particularly after eating candies. iii) No regular antibiotics are recommended. iv) Any procedure which can lead to entry of bacteria in blood stream must be precede by appropriate antibiotic administration. v) No antibiotics must be consumed on self prescription. vi) done. Antibiotics preferably must be given after the sepsis screening and blood cultures are vii) Any fever persisting beyond 3-5 days without any obvious cause must be investigated with 3 blood cultures and echocardiography. Compiled By Dr. Smita Mishra Senior Consultant, Deptt. of PediatricCardiology Escorts Heart Institute, New Delhi. Published by Admin in Ventricular Septal defect, VSD closing without surgery, VSD Treatment in india 10 AUG Closure of Holes in the Heart Without Surgery – A Dream Turned Reality!! By Admin 8-10/1000 live born babies have congenital defects in the heart. The most common defects are “Holes in the Heart.” For last six- seven decades, the only treatment available was surgical closure. Though the ultimate outcome was good, these children had to inevitably suffer the pain, scar and long hospital stay. From 1970s onwards, a group of cardiologists started thinking differently. They experimented on animals by creating holes in their hearts and then tried closing them without surgery. Gradually they replicated the whole procedure on humans. For the last twenty years, nonsurgical closure or device closure has been the norm. The Common Holes: The commonest holes are VSD (Ventricular Septal defect), ASD (Atrial Septal Defect) and PDA (Patent Ductus Arteriosus). VSD is a hole in the interventricular septum or wall between two lower chambers (RV and LV). ASD is the name of the hole in interatrial septum and PDA is actually an extra pipe connecting Aorta and Pulmonary Artery. Read more about the holes ASD VSD Of these three, VSDs are the commonest lesion about 25-30% of all congenital heart defect whereas ASD and PDA are about 5-8% of them. Another point to remember is that all of us are born with small ASD and small PDA. However, VSD is never found in normal heart. Click here to Read more abut Nonsurgical Closure – the basic techniques Article by: Dr Maitri Chaudhuri MD(Pediatrics), Fellow National Board(Pediatric Cardiology) Consultant Pediatric Cardiologist Vikram Hospitals, Bangalore Published by Admin in ASD closure without surgery, close hole in heart without surgery, closing of hole in the heart, Device closure of hole in heart, VSD closing without surgery 10 AUG Nonsurgical Closure – The Basic Technique By Admin Device closures are usually tried after child has good weight like 6-7 Kg. We have large vessels in our groin called Femoral Artery and Femoral Vein. A needle is first introduced into these two vessels (something like starting a saline drip). Next cardiac catheters are passed through these vessels and they reach the heart. We take the intracardiac pressure and anatomic data from these catheters. Then we inject radicontrast to outline the hole. Simultaneous echocardiography and fluoroscopy is done to confirm the findings. Then a nitinol(nickel- titanium alloy) device or button is delivered to the site of the hole and finally it is released. Post procedure angiography and echocardiography is done to confirm everything is OK. Then all catheters are taken out and only the device stays inside the heart. All this is done under general anesthesia so that the baby does not feel anything. Post procedure , baby is taken to the pediatric ICU, slowly taken out of anesthesia and monitored for 24 hours. Next day, he/ she undergoes another echo and discharged home. Preparation of the child before Device Closure: The child is admitted the evening before. Some basic investigations like blood tests(hemogram, urea, creatinine, serology ), Chest X Ray and ECG are done. An anesthesist checks the baby for fitness and starts saline. The child has to fast for a minimum of four hours before the procedure. Post Device Closure: What to Expect? 1. Your child will be in pediatric ICU till he is conscious, breathing normally, blood pressure and heart rate stabilizes and he is able to take oral feeds. Usually this takes 4-6 hours but may vary from child to child. 2. There will be a bandage covering the groin. The baby should not walk or bend that leg for 24 hours. Next day he can walk. 3. Echocardiography and Xray next day. 4. The baby is started on medicines to prevent clot inside the heart. This is called Aspirin and given once daily for 3-6months. 5. The baby is advised not to carry any heavy load and avoid direct trauma to the chest for three months only. 6. This three months is the time taken for the heart to develop endothelium lining around the device so that the device becomes a part of the body. 7. Schedule of follow up in cardiology OPD: Ist visit : 1 month later 2nd visit: 3 months later 3rd visit: 6 months later Thereafter annual visits Device Closure in Detail Atrial Septal defect Device Closure Ventricular Septal Defect Device Closure Patent Ductus Arteriosus (PDA) Device Closure Article by: Dr Maitri Chaudhuri MD(Pediatrics), Fellow National Board(Pediatric Cardiology) Consultant Pediatric Cardiologist Vikram Hospitals, Bangalore Published by Admin in Avoid surgery i nvsd, avoid surgery in asd, Device closures of hear holes 10 AUG Atrial Septal defect (ASD) Device Closure in Detail By Admin Atrial Septal defect: When to Close an ASD? a.Size More than 5-8mm b. Right Heart Enlargement c. High Lung Pressures d. Recurrent Pneumonias, Poor Weight Gain ASD Device Closure is one of the earliest device closures. Only ASDs in central portion of interatrial septum (Secundum ASD or FOSSA OVALIS ASD) can be closed by device.ASDs in topmost or lowest portion of the interatrial septum can be closed only surgically.Success rate is 95%. Risks include device migration, erosion, cardiac tamponade. But usually all these complications are immediately picked up by echo and angiography-fluoroscopy and the device is taken out by surgery and simultaneously the ASD is closed surgically. Take Home Message!!: 1. Device Closures of Holes in Heart Is Effective, Safe and Time Tested Procedure. 2. It is painless and scar less and allows your child to resume normal life including school within 3 days. Published by Admin in ASD closure without surgery, ASD Treatment 10 AUG Ventricular Septal Defect (VSD) Device Closure in Detail By Admin VENTRICULAR SEPTAL DEFECT (VSD Device Closure) VSD is the commonest congenital heart disease. Percutaneous device closures of VSDs are still under evolution. Muscular VSDs or Holes in the muscular partition between right and left ventricles are easily closed by devices. However VSDs which are situated close to the cardiac valves (like aortic and tricuspid) are better closed surgically. Indications: 1. 2. 3. 4. Poor weight gain, repeated pneumonias VSD with left hear enlargement VSD with high lung pressures Left to right shunt ratio >2:1 Success rate is 95% and complications and their management are similar to ASD Devices. Take Home Message!!: 1. Device Closures of Holes in Heart Is Effective, Safe and Time Tested Procedure. 2. It is painless and scar less and allows your child to resume normal life including school within 3 days. Published by Admin in VSD closing without surgery, VSD Treatment in india 10 AUG Patent Ductus Arteriosus (PDA) Device Closure in Detail By Admin PATENT DUCTUS ARTERIOSUS(PDA DEVICE CLOSURE) PDAs are found in 6-8% of children with heart disease. Unlike ASD or VSD, all PDAs are now closed nonsurgically be device closure. Smaller PDAs like <2.5mm in size are closed by coils. The decision whether coil or device is taken inside the cath lab. Both have excellent results,reported success rates is 98-99%. Only premature newborns with very large PDAs causing heart failure are closed by surgery. Take Home Message!!: 1. Device Closures of Holes in Heart Is Effective, Safe and Time Tested Procedure. 2. It is painless and scar less and allows your child to resume normal life including school within 3 days. Published by Admin in Blue baby syndrome in india, Close PDA without surgery, PDA DEVICE CLOSURE, Treatment for Blue baby syndrome 14 JUL Ventricular Septal Defect – Hole between lower chambers of heart By Admin A ventricular septal defect (VSD) — sometimes referred to as a hole in the heart — is a type of congenital heart defect in which there is an abnormal opening in the dividing wall between the main pumping chambers of the heart (the ventricles). VSDs are the most common congenital heart defect, and in most cases they’re diagnosed and treated successfully with few or no complications. What Is a Ventricular Septal Defect? To understand this defect, it first helps to review some basics about the way a healthy heart typically works. The heart has four chambers: The two lower pumping chambers of the heart are called the ventricles, and the two upper filling chambers are the atria. In a typical healthy heart, blood that returns from the body to the right-sided filling chamber (right atrium) is low in oxygen. This blood passes to the right-sided pumping chamber (right ventricle), and then travels to the lungs to receive oxygen. The blood that has been enriched with oxygen returns to the left atrium, and then to the left ventricle. It’s then pumped out to the body through the aorta, a large blood vessel that carries the blood to the smaller blood vessels in the body. The right and left-sided pumping chambers (ventricles) are separated by shared wall, called the ventricular septum. Kids with a VSD have an opening in this wall. As a result, when the heart beats, some of the blood in the left ventricle (which has been enriched by oxygen from the lungs) is able to flow through the hole in the septum into the right ventricle. In the right ventricle, this oxygen-rich blood mixes with the oxygen-poor blood and goes back to the lungs. The blood flowing through the hole creates an extra noise, which is known as a heart murmur. The heart murmur, can be heard when a doctor listens to the heart beat with a stethoscope. VSDs can be located in different places on the ventricular septum, and they can be different sizes. The symptoms and medical treatment of the VSD will depend on those factors. In some rare cases, VSDs are part of more complex types of congenital heart disease. What Causes a VSD? Ventricular septal defects occur during fetal heart development and are present at birth. During the first weeks after conception, the heart develops from a large tube, dividing into sections that will eventually become the walls and chambers. If a problem occurs during this process, it can create a hole in the ventricular septum. In some cases, the tendency to develop a VSD may be genetic. There can be genetic syndromes that cause extra or missing pieces of chromosomes that can be associated with VSD. For the vast majority of children with a defect, however, there’s no clear cause of the VSD. Signs and Symptoms of a VSD VSDs are usually found in the first few weeks of life by a doctor during a routine checkup. The doctor will be able to detect a heart murmur, which is due to the sound of blood as it passes between the left and right ventricles. The murmur associated with a VSD has certain features that allow a doctor to distinguish it from heart murmurs due to other causes. The size of the hole and its location within the heart will determine whether VSD causes any symptoms. Small VSDs will not typically cause any symptoms, and may ultimately close on their own. Older kids or teens who have small VSDs that persist usually don’t experience any symptoms other than the heart murmur that doctors hear. They may need to see a doctor regularly to check on the heart defect and make sure it isn’t causing any problems. Moderate and large VSDs that haven’t been treated in childhood may cause noticeable symptoms. Babies may have faster breathing and get tired out during attempts to feed. They may start sweating or crying with feeding, and may gain weight at a slower rate. These signs generally indicate that the VSD will not close by itself, and cardiac surgery may be needed to close the hole. Surgery is typically done within the first 3 months of life to prevent it from causing other complications. A cardiologist can prescribe medication to lessen symptoms before surgery. People with VSD are at greater risk in their lifetime of developing endocarditis, an infection of the inner surface of the heart. This occurs when bacteria in the bloodstream infect the lining of the heart. Bacteria are always in our mouths, and small amounts are introduced into the bloodstream when we chew and brush our teeth. The best way to protect the heart from endocarditis is to to reduce oral bacteria by brushing and flossing daily, and visiting the dentist regularly. In general, it is not recommended that patients with simple VSDs take antibiotics before dental visits, except for the first 6 months after surgery. Diagnosing a VSD If your child is discovered to have a heart murmur that was not noticed earlier, a doctor may refer you to a pediatric cardiologist, a doctor who specializes in diagnosing and treating childhood heart conditions. In addition to doing a physical exam, the cardiologist take your child’s medical history. If a VSD is suspected, the cardiologist may order one or more of the following tests: a chest X-ray, which produces a picture of the heart and surrounding organs an electrocardiogram (ECG), which records the electrical activity of the heart an echocardiogram (echo), which uses sound waves to produce a picture of the heart and to visualize blood flow through the heart chambers. This is often the primary tool used to diagnose VSD. a cardiac catheterization, which provides information about the heart structures as well as blood pressure and blood oxygen levels within the heart chambers. This test is usually performed for VSD only when additional information is needed that other tests cannot provide. Treating a VSD Once an VSD is diagnosed, treatment will depend on the child’s age and the size, location, and severity of the defect. A child with a small defect that causes no symptoms may simply need to visit a cardiologist regularly to make sure that there are no other problems. In most children, a small defect will close on its own without surgery. Some may not close, but they do not get any larger. In cases where the VSD is small and has not closed, there are generally no restrictions to activities or to playing sports. For kids with medium to large VSDs, surgery may be necessary. In most cases, this takes place within the first few weeks to months of life. In this procedure, the surgeon makes an incision in the chest wall, and a heart-lung machine is used to do the work of the circulation while the surgeon closes the hole. The surgeon can stitch the hole closed directly or, more commonly, sew a patch of manmade surgical material over it. Eventually, the tissue of the heart heals over the patch or stitches, and by 6 months after the surgery, the hole will be completely covered with tissue. Certain types of VSDs may be closed during cardiac catheterization. A thin, flexible tube called a catheter is inserted into a blood vessel in the leg that leads to the heart. A cardiologist guides the tube into the heart to make measurements of blood flow, pressure, and oxygen levels in the heart chambers. A special implant, shaped into two disks formed of flexible wire mesh, can be positioned into the hole in the septum. The device is designed to flatten against the septum on both sides to close and permanently seal the VSD. After healing from surgery or catheterization, kids with VSDs are considered cured and should have no further symptoms or problems. Caring for a Child With a VSD Some kids with VSDs may take heart medication prior to surgery to help lessen the symptoms from the defect. Those who have surgery for larger VSDs usually leave the hospital within 4 to 5 days after surgery if there are no problems. In most cases, kids who have had VSD surgery recover quickly and without problems. But doctors will closely monitor the child for signs or symptoms of any problems. Your child may undergo another echocardiogram to make sure that the heart defect has closed completely. If your child is having trouble breathing, call your doctor or take your child to the emergency department immediately. Other symptoms that may indicate a problem include: a bluish tinge or color (cyanosis) to the skin around the mouth or on the lips and tongue poor appetite or difficulty feeding failure to gain weight or weight loss listlessness or decreased activity level prolonged or unexplained fever increasing pain, tenderness, or pus oozing from your child’s incision Call your doctor if you notice any of these signs in your child after closure of the VSD. Any time a child is diagnosed with a heart condition, it can be scary. But the good news is that your pediatric cardiologist will be very familiar with this condition and how to best manage it. Most kids who’ve had a VSD corrected have a normal life expectancy and go on to live healthy, active lives. Published by Admin in Hole in the Heart, Treatment for hole in the heart, VSD Treatment in india, what is ventricular septal defect? 01 JUN Atrial Septal Defect – Hole between Upper Chambers of Heart By Admin What is an Atrial Septal Defect? (ASD) An Atrial Septal Sefect (ASD) — sometimes referred to as a hole in the heart — is a type of Heart Defect Present from birth (Congenital Heart Defect) in which there is an abnormal opening in the dividing wall between the upper filling chambers of the heart (the atria). In most cases ASDs are diagnosed and treated successfully with few or no complications. To understand this defect, it first helps to review some basics about the way a healthy heart typically works. The heart has four chambers: The two lower pumping chambers are called the ventricles, and the two upper filling chambers are the atria. In a healthy heart, blood that returns from the body to the right-sided filling chamber (right atrium) is low in oxygen. This blood passes to the right-sided pumping chamber (right ventricle), and then to the lungs to receive oxygen. The blood that has been enriched with oxygen returns to the left atrium, and then to the left ventricle. It’s then pumped out to the body through the aorta, a large blood vessel that carries the blood to the smaller blood vessels in the body. The right and left filling chambers are separated by a thin shared wall, called the atrial septum. Kids with an atrial septal defect (ASD) have an opening in the wall (septum) between the atria. As a result, some oxygenated blood from the left atrium flows through the hole in the septum into the right atrium, where it mixes with oxygen-poor blood and increases the total amount of blood that flows toward the lungs. The increased blood flow to the lungs creates creates a swishing sound, known as a heart murmur. This heart murmur, along with other specific heart sounds that can be detected by a cardiologist, may be clues that a child has an ASD. ASDs can be located in different places on the atrial septum, and they can be different sizes. The symptoms and medical treatment of the defect will depend on those factors. In some rare cases, ASDs are part of more complex types of congenital heart disease. It’s not clear why, but ASDs are more common in girls than in boys Causes ASDs occur during fetal development of the heart and are present at birth. During the first weeks after conception, the heart develops. If a problem occurs during this process, a hole in the atrial septum may result. In some cases, the tendency to develop a ASD may be genetic. There can be genetic syndromes that cause extra or missing pieces of chromosomes that can be associated with ASD. For the vast majority of children with a defect, however, there’s no clear cause of the ASD. Signs and Symptoms The size of an ASD and its location in the heart will determine what kinds of symptoms a child experiences. Most children who have ASDs seem healthy and appear to have no symptoms. Generally, kids with an ASD feel well and grow and gain weight normally. Infants and children with larger, more severe ASDs, however, may possibly show some of the following signs or symptoms: poor appetite poor growth fatigue shortness of breath lung problems and infections, such as pneumonia If an ASD is not treated, health problems can develop later, including an abnormal heart rhythm (known as an atrial arrhythmia) and problems in how well the heart pumps blood. As kids with ASDs get older, they may also be at an increased risk for stroke, since a blood clot that develops can pass through the hole in the wall between the atria and travel to the brain. Pulmonary hypertension (high blood pressure in the lungs) may also develop over time in older patients with larger untreated ASDs. Fortunately, most kids with ASD are diagnosed and treated long before the heart defect causes physical symptoms. Because of the complications that ASDs can cause later in life, pediatric cardiologists often recommend closing ASDs early in childhood. Diagnosis Generally, a child’s doctor hears the heart murmur caused by ASD during a routine checkup or physical examination. ASDs are not always diagnosed as early in life as other types of heart problems, such as ventricular septal defect (a hole in the wall between the two ventricles). The murmur caused by an ASD is not as loud and may be more difficult to hear than other types of heart murmurs, so it may be diagnosed any time between infancy and adolescence (or even as late as adulthood). If a doctor hears a murmur and suspects a heart defect, the child may be referred to a pediatric cardiologist, a doctor who specializes in diagnosing and treating childhood heart conditions. If an ASD is suspected, the cardiologist may order one or more of the following tests: chest X-ray, which produces an image of the heart and surrounding organs electrocardiogram (ECG), which records the electrical activity of the heart and can indicate volume overload of the right side of the heart echocardiogram (echo), which uses sound waves to produce a picture of the heart and to visualize blood flow through the heart chambers. This is often the primary tool used to diagnose ASD. Treatment Once an ASD is diagnosed, treatment will depend on the child’s age and the size, location, and severity of the defect. In kids with very small ASDs, the defect may close on its own. Larger ASDs usually won’t close, and must be treated medically. Most of these can be closed in a cardiac catheterization lab, although some ASDs will require open-heart surgery. A child with a small defect that causes no symptoms may simply need to visit a pediatric cardiologist regularly to ensure that there are no problems; often, small defects will close spontaneously without any treatment during the first years of life. In general, a child with a small ASD won’t require restrictions on his or her physical activity. In most children with ASD, though, doctors must close the defect if it has not closed on its own by the time a child is old enough to start school. Depending on the position of the defect, many children with ASD can have it corrected with a cardiac catheterization. In this procedure, a thin, flexible tube called a catheter is inserted into a blood vessel in the leg that leads to the heart. A cardiologist guides the tube into the heart to make measurements of blood flow, pressure, and oxygen levels in the heart chambers. A special implant can be positioned into the hole in the septum. The device is designed to flatten against the septum on both sides to close and permanently seal the ASD. In the beginning, the natural pressure in the heart holds the device in place. Over time, the normal tissue of the heart grows over the device and covers it entirely. This non-surgical technique for closing an ASD eliminates the scar on the chest needed for the surgical approach, and has a shorter recovery time, usually just an overnight stay in the hospital. Because there is a small risk of blood clots forming on the closure device while new tissue heals over it, children who undergo device closure of an ASD may need to be on medications for several months after the procedure to prevent clots from forming. If surgical repair for ASD is necessary, a child will undergo open-heart surgery. In this procedure, a surgeon makes a cut in the chest and a heart-lung machine is used to do the work of the circulation while the heart surgeon closes the hole. The ASD may be closed directly with stitches or by sewing a patch of surgical material over the defect. Eventually, the tissue of the heart heals over the patch or stitches, and by 6 months after the surgery, the hole will be completely covered with tissue. For 6 months following catheterization or surgical closure of an ASD, antibiotics are recommended before routine dental work or surgical procedures to prevent infective endocarditis. Once the tissue of the heart has healed over the closed ASD most people who have had their ASDs corrected no longer need to worry about having a higher risk of infective endocarditis. Your doctor will discuss other possible risks and complications with you prior to the procedure. Typically, after repair and adequate time for healing, children with ASD rarely experience further symptoms or disease. Caring for Your Child Kids who undergo cardiac catheterization to close an ASD usually spend the night in the hospital after the procedure. Those who have had a catheterization procedure should also be kept out of gym class or sports practice for a week; after a week, they can usually return to their normal physical activities, with their doctor’s OK. Kids who undergo surgery for their ASDs usually go home after a few days in the hospital if there are no complications. After surgical ASD repair, the main medical concern is the healing of the chest incision. In general, the younger patients are when they have their surgical repairs, the less pain they will have during recovery. The child will be watched closely for signs or symptoms that may indicate a problem. If your child has trouble breathing, is not eating, has fever, or redness or pus oozing from the incision, get medical treatment right away. In most cases, kids who have had ASD surgery recover quickly and without problems. In the weeks following surgery or cardiac catheterization, your doctor will check on your child’s progress. Your child may undergo another echocardiogram to make sure that the heart defect has closed completely. Kids who have undergone ASD repair will continue to have follow-up visits with the cardiologist. Most children who undergo treatment for ASDs recover quickly — you may even notice that within a few weeks of treatment, your child is eating more and is more active than before surgery. However, some signs and symptoms may indicate a problem. If your child is having trouble breathing, call the doctor or take your child to the emergency department immediately. Other symptoms that may indicate a problem include: a bluish tinge or color (cyanosis) to the skin around the mouth or on the lips and tongue poor appetite or difficulty feeding failure to gain weight or weight loss listlessness or decreased activity level prolonged or unexplained fever increasing pain, tenderness, or pus oozing from the incision Call your doctor if you notice any of these signs in your child after closure of the ASD. Any time a child is diagnosed with a heart condition, it can be scary. But the good news is that your pediatric cardiologist will be very familiar with this condition and how to best manage it. Most kids who’ve had an ASD corrected have a normal life expectancy and go on to live healthy, active lives. Published by Admin in ASD Treatment, atral septal defect causes, baby heart disease symptoms, How do i know if my child has heart diease?, Treatment for hole in the heart Older posts » BABY HEART WEBLOG Send PAGE TOP © Baby Heart 2010 DESIGN: DISPLAY:INLINE Blog All the latest news about our products and services About Who's behind this blog RSS feed Keep in touch with us Home About Contact Us RSS