* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download sinus node paces
Survey
Document related concepts
Heart failure wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Myocardial infarction wikipedia , lookup
Ventricular fibrillation wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Transcript
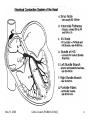
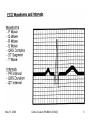
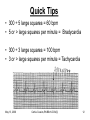
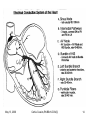
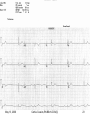
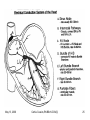
Advanced ECG’s for MLA’s Cathie Cousins, RN, BScN, CCN(C) Objectives 1. To review Basic Concepts for the 12-Lead ECG To discuss the following on the 12-Lead ECG 2. Bradycardia 3. Tachycardia 4. Ventricular Ectopy 5. ST and T wave changes 6. Pacemakers May 13, 2006 Cathie Cousins,RN BScN CCN(C) 2 1. Basic Concepts • The heart is a pump with an electrical conduction system • 2 basic types of cardiac cells in the heart • Myocardial cells or “muscle” cells • Specialized cells of the conduction system or “pacemaker” cells May 13, 2006 Cathie Cousins,RN BScN CCN(C) 3 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 4 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 5 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 6 Electrical Axes and Vectors • Each of the 12 leads on the ECG has a different pattern because each lead views the hearts electrical axis from a different position • Atrial and ventricular depolarization and repolarization generate an electric current known as an electrical axis or vector (different from the axis of a lead) May 13, 2006 Cathie Cousins,RN BScN CCN(C) 7 • Average of all the ventricular vectors points to the left and downward • Knowing the electrical axis of the heart enables us to determine the normal pattern of each lead and the cause for altered patterns in each lead May 13, 2006 Cathie Cousins,RN BScN CCN(C) 8 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 9 Rate • Both the atrial and ventricular rates should be measured May 13, 2006 Cathie Cousins,RN BScN CCN(C) 10 The Grid Method for Rate • Uses the distance between 2 sequential complexes on the ECG • Each small square represents 0.04 seconds - 1500 small squares in 1 minute - 300 large squares in 1 minute • Count the large squares between P waves for atrial rate and R waves for ventricular rate • 300 ÷ number of large squares = number of beats/min May 13, 2006 Cathie Cousins,RN BScN CCN(C) 11 Quick Tips • 300 ÷ 5 large squares = 60 bpm • 5 or > large squares per minute = Bradycardia • 300 ÷ 3 large squares = 100 bpm • 3 or > large squares per minute = Tachycardia May 13, 2006 Cathie Cousins,RN BScN CCN(C) 12 2. Bradycardia • Bradycardia is a heart rate < 60/min • Bradycardia can be due a slow sinus rate, the origin of the rhythm or an AV block: - Sinus Bradycardia - Junctional Rhythm - Idioventricular Rhythm - 2° AV Block Type I - 2° AV Block Type II - 3° AV Block May 13, 2006 Cathie Cousins,RN BScN CCN(C) 13 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 14 Sinus Bradycardia • Sinus node is pacing at a rate < 60/min • P wave, QRS normal May 13, 2006 Cathie Cousins,RN BScN CCN(C) 15 Junctional Rhythm • Sinus node and atria fail to pace the heart. AV junction paces at → 40-60/min • No P wave or PR interval < 0.12, QRS normal May 13, 2006 Cathie Cousins,RN BScN CCN(C) 16 Idioventricular Rhythm • Sinus node, atria, and AV junction fail to pace. Ectopic pacemaker in the ventricles paces at → 20-40/min • No P wave, QRS wide, ST & T waves often abnormal May 13, 2006 Cathie Cousins,RN BScN CCN(C) 17 AV Blocks • 2° Type I and 2°Type II AV Blocks, sinus node paces the heart • Not ever P wave results in QRS, QRS normal or wide May 13, 2006 Cathie Cousins,RN BScN CCN(C) 18 • 3° AV Block, sinus node paces the heart • P waves do not result in QRS AV junction paces, QRS normal Ventricles pace, QRS wide May 13, 2006 Cathie Cousins,RN BScN CCN(C) 19 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 20 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 21 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 22 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 23 3. Tachycardia • Tachycardia is a heart rate > 100/min • Tachycardia can be due to: - Sinus Tachycardia - Supraventricular Tachycardia - Ventricular Tachycardia May 13, 2006 Cathie Cousins,RN BScN CCN(C) 24 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 25 Sinus Tachycardia • Sinus node is pacing at a rate > 100/min • P wave, QRS normal May 13, 2006 Cathie Cousins,RN BScN CCN(C) 26 Superventricular Tachycardia • Ectopic focus in atria or AV junction paces the heart or Abnormal conduction thru AV node or Accessory pathway • P wave or no P wave, QRS narrow or wide, rate > 150/min May 13, 2006 Cathie Cousins,RN BScN CCN(C) 27 Ventricular Tachycardia • Ectopic pacemaker in ventricles paces the heart • No P wave, QRS wide and bizarre May 13, 2006 Cathie Cousins,RN BScN CCN(C) 28 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 29 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 30 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 31 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 32 4. Premature Ventricular Contractions QRS Duration • QRS duration - depolarization of right and left ventricles, from the endocardium to epicardium • Normal QRS duration - 0.06-0.10 sec • QRS duration > 0.10 sec, a conduction delay exists in the bundle branches, Purkinjie network or ventricular myocardium, or ventricular ectopic conduction exists May 13, 2006 Cathie Cousins,RN BScN CCN(C) 33 • PVC’s, premature ventricular complexes: the premature beat originates in an ectopic focus in one ventricle, it depolarizes that ventricle, then the other • No P wave, QRS wide & bizarre, ST often abnormal, T wave often opposite the rhythm • Multifocal PVC’s come from more than one ectopic focus, each foci has a different shape May 13, 2006 Cathie Cousins,RN BScN CCN(C) 34 • • • • 1 PVC 2 PVC’s 3 PVC’s 4 PVC’s = = = = a PVC couplet triplet ventricular tachycardia • Every 2nd PVC = bigeminy • Every 3rd PVC = trigeminy • Bigeminy or trigeminy can refer to any ectopic beat so clarify eg. bigeminal PVC’s or bigeminal PAC’s, etc. May 13, 2006 Cathie Cousins,RN BScN CCN(C) 35 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 36 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 37 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 38 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 39 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 40 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 41 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 42 5a. ST Segments • ST segment = end of ventricular repolarization + early part of ventricular repolarization • ST segment normally isoelectric • Ischemic + injured myocardial cells altered membrane potentials, this allows a current to flow as seen in ST elevation + depression May 13, 2006 Cathie Cousins,RN BScN CCN(C) 43 Measuring ST Segments • ST measurement = vertical difference between the isoelectric line + end of QRS complex, the “J” point” May 13, 2006 Cathie Cousins,RN BScN CCN(C) 44 ST Segment Elevation • ST segment elevation = >1 mm (>0.1 mV) above baseline after the J point • ST segment elevation due to severe injury temporary until ischemia resolved or injured heart tissue heals or dies • ST segments elevate in leads facing the injury • ST segments depress in leads opposite (reciprocal ) leads May 13, 2006 Cathie Cousins,RN BScN CCN(C) 45 Types of ST Elevation in AMI May 13, 2006 Cathie Cousins,RN BScN CCN(C) 46 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 47 Other Common Causes of ST Segment Elevation • • • • • Coronary artery vasospasm Acute pericarditis Ventricular aneursym Hyperkalemia Non-specific ST-T wave changes May 13, 2006 Cathie Cousins,RN BScN CCN(C) 48 ST Segment Depression • ST segment depression = > 1 mm below baseline after the J point • ST segment depression due to severe ischemia temporary until ischemia resolved or heart tissue heals • ST segments depress in leads facing the ischemia • ST segments elevate in opposite (reciprocal) leads May 13, 2006 Cathie Cousins,RN BScN CCN(C) 49 Types of ST Depression in AMI Different types of ST depression in AMI: - downsloping - horizontal - upsloping May 13, 2006 Cathie Cousins,RN BScN CCN(C) 50 Other Common Causes of ST Segment Depression • Left and right ventricular hypertrophy • Left and right bundle branch block • Digitalis in therapeutic and toxic doses May 13, 2006 Cathie Cousins,RN BScN CCN(C) 51 Acute MI Anterior Septal Anterior Lateral Inferior Facing Leads Opposite Leads V1-V2 V3-V4 I, aVL, & V5 or V6 II, III, & aVF None None II, III, & aVF I & aVL Posterior V7,V8, V9 on 18 lead V1-V4 Right Ventricle V4R, V5R, V6R on 18 lead None May 13, 2006 Cathie Cousins,RN BScN CCN(C) 52 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 53 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 54 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 55 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 56 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 57 5b. T waves • A T wave represents ventricular depolarization • T waves normally upright, rounded, and slightly asymmetrical. Normally negative in aVR. • Normally 1/8 to 2/3 the height of the QRS complex May 13, 2006 Cathie Cousins,RN BScN CCN(C) 58 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 59 Abnormal T Waves in AMI • Normal Heart positive T wave • Subendocardial Ischemia symmetrically positive tall, peaked T wave May 13, 2006 Cathie Cousins,RN BScN CCN(C) 60 • Subepicardial Ischemia symmetrically negative deep T wave • Late phases in AMI deeply inverted T waves with abnormal Q waves May 13, 2006 Cathie Cousins,RN BScN CCN(C) 61 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 62 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 63 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 64 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 65 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 66 6. Pacemakers May 13, 2006 Cathie Cousins,RN BScN CCN(C) 67 The 3 Functions of Pacing 1. Sensing – the ability of the pacemaker to recognize the patient’s intrinsic heartbeat 2. Pacing – the pacemaker produces a stimulus either when the sensing circuit does not detect an intrinsic heartbeat or at a predetermined time interval 3. Capturing – the depolarization of the myocardium in response to pacing May 13, 2006 Cathie Cousins,RN BScN CCN(C) 68 Pacemaker Codes • • • • • I II III IV V Chamber(s) paced Chamber(s) sensed Response to sensing Programmable function(s) Antitachyarrhythmia function(s) May 13, 2006 Cathie Cousins,RN BScN CCN(C) 69 Pacing Leads Sites - Permanent May 13, 2006 Cathie Cousins,RN BScN CCN(C) 70 Pacing Leads Sites - Temporary May 13, 2006 Cathie Cousins,RN BScN CCN(C) 71 Pacemaker Sites - Temporary Transcutaneous – External Pacing May 13, 2006 Cathie Cousins,RN BScN CCN(C) 72 Pacemaker Strip 1 1. Sensing 2. Pacing 3. Capturing May 13, 2006 Cathie Cousins,RN BScN CCN(C) 73 Pacemaker Strip 2 1. Sensing 2. Pacing 3. Capturing May 13, 2006 Cathie Cousins,RN BScN CCN(C) 74 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 75 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 76 May 13, 2006 Cathie Cousins,RN BScN CCN(C) 77 Thank You • Remember: It is the team that assists the patient in achieving wellness. • Thank you and enjoy the exciting world of 12 Lead ECG’s. May 13, 2006 Cathie Cousins,RN BScN CCN(C) 78