* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Chapter 4 MICROBIAL DISEASES OF THE SKIN
Human microbiota wikipedia , lookup
Staphylococcus aureus wikipedia , lookup
Virus quantification wikipedia , lookup
Urinary tract infection wikipedia , lookup
History of virology wikipedia , lookup
Social history of viruses wikipedia , lookup
Neglected tropical diseases wikipedia , lookup
Infection control wikipedia , lookup
Schistosomiasis wikipedia , lookup
Orthohantavirus wikipedia , lookup
West Nile fever wikipedia , lookup
Henipavirus wikipedia , lookup
Onchocerciasis wikipedia , lookup
Neonatal infection wikipedia , lookup
Eradication of infectious diseases wikipedia , lookup
Germ theory of disease wikipedia , lookup
Marburg virus disease wikipedia , lookup
Hepatitis B wikipedia , lookup
Transmission (medicine) wikipedia , lookup
Canine parvovirus wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
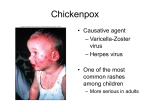
CHAPTER 4 MICROBIAL DISEASES OF THE SKIN Miss Rashidah Hj Iberahim Content Bacterial skin diseases* Viral skin diseases Fungal skin diseases Wound infection – gas-gangrene* Bacterial infections Gram positive infections Staphylococcus sp Folliculitis and other skin lesions Scalded skin syndrome Streptococcus sp Scarlet Fever Erysipelas Folliculitis(pimples / pustules) Pathogenesis • • • • S. aureus colonize skin and upper resp. tract of infants within 24 hrs after birth Invade thru hair follicleproducing folliculitis (form of pimples and pustules) Encapsulated of abcess- x shedding n antibiotic reach the area Treatment-surgery Transmission Spread thru hosp personnel, asympt carrier n hosp visitors/catheters and splinters for older patient /nasal droplets and fomites 100 m/org were enough to cause infection in suture on base of eye lashes – sty A larger and deeper form – abscess Exterior abscess – furuncle / boil Massive lesion - curbuncle Scalded Skin Syndrome Pathogenesis By certain exotoxin-producing strain of S.aureus (2 types exfoliatins) Common in infant; adult (toxic shock syndrome) Exotoxin move thru veins to the skin causing outer layer peeling off in leaflike sheets Can lead to septicemia and very antigenic Can cause reinfection – antibiotic very important Symptoms 1. 2. 3. 1st stage – redness of surrounding area 2nd stage – 1-2 days large, soft and easily ruptured vesicles around the body 3rd stage – the lesion getting dry and scale Peeling off skin Scarlet Fever Pathogenesis Also known as scarlatina By Streptococcus pyogenes Contain 3 types of erythrogenic toxin – reddening The strain was 1st infected by temperate phage – erythrogenic toxin that leads to rash Only infecting new exposure pt low- virulent strain – glomerulonephritis / rheumatic fever Reinfection that already defends by previous antibiotic – leads to strep throat (but carrier of scarlet fever) Might also caused by fomites Rash The best medicine is Penicillin – decrease mortality rate Erysipelas Pathogenesis Face- small, bright, raised, rubbery lesion. Beta hemolytic gp A Strept. Always occur after pt having surgery or wounds Producing hyaluronidase enzyme and toxin Minor abrasion— sup. Lymph vessels (causing septicemia, abscess,pneumonia, endocarditis, arthritis, death) Viral Diseases Rubella The disease Rashes appear on trunk after 16-21 days after infection Caused by togavirus 2ndary: arthritis and arthralgia Can caused congenital rubella syndrome Transmission Mainly through nasal secresion Direct contact among children age 5 – 14 Infected infants expose to hospital personnel Rubella Diagnosis Immunity assessment on pregnant woman Rubella – specific IgM antibody Other variety serology test Prevention Currently using rubella vaccine (MMR) Measles/ Rubeola Diagnosis and prevention Caused by Rubeola virus Koplik’s spots – bluish specks in upper lips and cheek mucosa Rubella – pink n flat rash Rubeola – red and raised Other complications : Measles encephalitis Subacute sclerosing panencephalitis (SSPE) Diagnose by its symptoms 2nd accompanied by bacterial infection Using the same vaccine as rubella and mumps (MMR) Chicken pox and Shingles The disease 1 virus – 2 diseases CP – varicella, S – zoster (varicella-zoster virus) 2nd inf by S. aureus In children Damages in blood and lymphatic drainage During latent period, stay in ganglia of nerve cells Symptoms CP = Causing blood clot and hemorrhage, Cause death S = pain, burning, prickling of the skin when it reactivate Disease progression 1. 2. 3. 4. 5. 6. Virus enter upper respiratory tract/ conjuctiva – replicates Carried by blood to various tissues – replicates Release of viruses causes fever and malaise After 14 – 16 days, present of small, irregular, rose-coloured skin lesions Fluid become cloudy, dry and crust over 2-4 days (virus cycle) Rashes start from scalp and trunk, face and limbs, to mouth/throat/ vagina, and may spread to resp tract and GIT Chicken pox and shingles Transmission CP – Infect between 59 yrs old V – age >45 yrs old Spread by respiratory secretion and fluid from moist lesion (not the dry lesion) Diagnosis and treatment Using rapid laboratory test Treatment – antiviral agent (valtrex and neurontin) Wound infection Gas gangrene Gas Gangrene Pathogenesis Caused by more than 1 bacteria = Clostridium sp. Spores of the bacteria expose during injuries and surgery The symptoms getting severe because of toxin and enzyme production Suddent onset = 12-48 hrs after exposure Symptoms Foul odour Ferment muscle carbohydrates “snap, crackle and pop” High fever, shock, massive tissue destruction, blackening of tissues Photograph before right leg amputation (hemipelvectomy) of a patient with gas gangrene. The right thigh is swollen, edematous and discoloured with necrotic bullae(large blisters). An impressive crepitation is already palpable. At this juncture, the patient is in shock. Others diseases 1. Wart Caused by Human Pappiloma Virus (DNA) Plane wart Face , back of hands Plantar wart sole Genital wart Condylomata accuminata Penile, vulvar skin, perianal area Sexual partner Child---sexual abuse Some: oncogenic:16, 18 2. Molluscum contagiosum Pox virus Child Face, neck Central punctum Hunderson-patterson bodies Fungal Superficial mycosis Deep mycosis Dermatophyte infection Skin Hair Nails Tinea pedis Adult (athlete’s) Toe webs , instep T.rubrum, T.mentagrophytes Tinea ungum T.rubrum, T.mentagrophytes Tinea corporis: Trunk Active edge T.rubrum T.cruris T.manun Tinea capitis Well circumscriped pruritic scaling area of hair loss Black dot (T.tonsurans) Gray patch (M.audouinii), Kerion (T.verrucosum) Favus (T.schoenleinii)